Table of Contents
Introduction
The body’s microbiome is a host of trillions of microorganisms that help form an ecosystem that interacts with the entire body system. Each of the systems inside the body like the musculoskeletal system, the gut system, the central nervous system, and the endocrine system each play a role in order for the body to function properly. When there are unwanted pathogens that start attacking each system, it can cause lots of problems to the body and over time can develop into chronic illnesses. In this 2 part series, we will be taking a look at how different organisms are associated with cardiovascular diseases and how to improve the gut’s microbiome health. Part 1 took a look at the body’s microbiome and how it plays a role in cardiovascular disease. By referring patients to qualified and skilled providers who specialized in cardiovascular services. To that end, and when appropriate, we advise our patients to refer to our associated medical providers based on their examination. We find that education is the key to asking valuable questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, in case you are uncertain here is the link to all the insurance providers we cover. If you have any questions, please call Dr. Jimenez at 915-850-0900.
The Gut Microbiome & Cardiovascular Disease
Since the gut is known to create a symbiotic relationship with its host, chronic illnesses can affect it and cause unwanted problems to not only the gut but also the entire body. Studies have found that when the gut goes through deleterious changes that cause an imbalance to the gut microbiota, it can impair the homeostatic mechanisms and activate multiple pathways that can trigger cardiovascular disease risk factors. Another study also found that when the gut microbiome is affected it can also cause bacterial translocation to be associated with the development of cardiac disorders that makes them potential triggers to the gut microbiome.
Organisms Associated With Cardiovascular Disease
Some of the organisms that are in the body can be associated with cardiovascular disease. Studies show that when these organisms are associated with cardiovascular diseases, they can cause impaired intestinal barrier function and the presence of bacterial products that they carry can be in the systemic circulation and heightened inflammatory state in the gut while also affecting the cardiovascular system. Some of the organisms include:
- Lipopolysaccharide (LPS)
- Occludin
- Zonulin
- Leaky Gut
- Metabolic Endotoxemia
Lipopolysaccharide
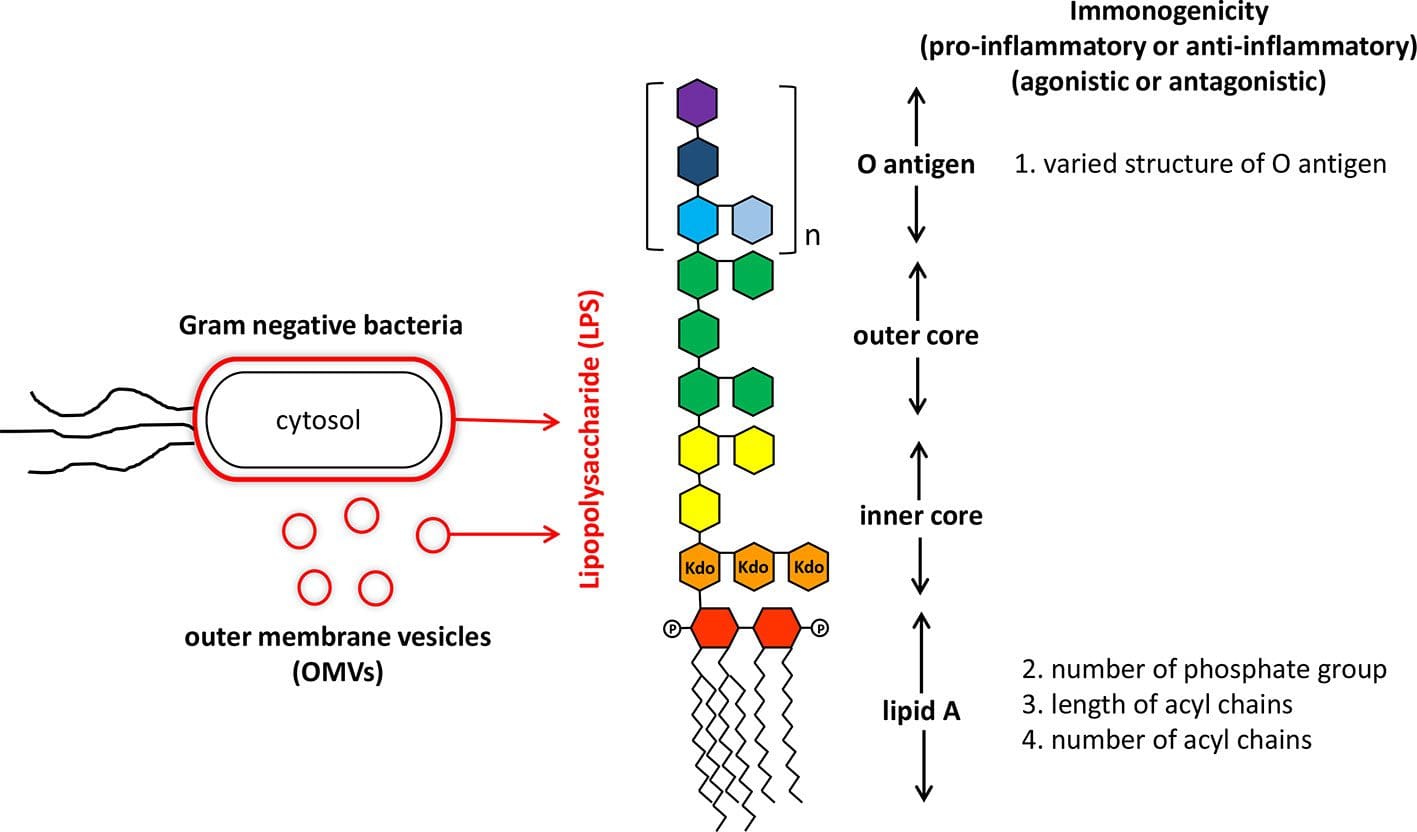
Lipopolysaccharides (LPS) are large molecules found in gram‐negative bacteria. They are endotoxins, and if absorbed can elicit a strong immune response. The detection of antibodies against LPS reveals macromolecule‐sized endotoxin infiltration through the intestinal barrier into the systemic circulation.
Intestinal permeability can cause systemic inflammation through translocation of LPS. Studies have found that lipopolysaccharides may be involved in the process of atherothrombosis process since it is an interesting molecule that once it crosses the gut microbiota and enters the systemic circulation it will cause chronic inflammation and atherosclerosis, which is a cardiovascular disease.
Occludin
Occludin is part of the main component of proteins holding together the tight junctions. Research shows that intercellular tight junctions help regulate the counter interactions of occludin and provide highly polarized barriers for homeostatic maintenance. The detection of antibodies to occludin indicates that the tight junctions are breaking down. Studies have found that occludin can help the tight junction with regulated maintenance but when chronic symptoms like oxidative stress are causing problems to occludin, it can cause damage to the gut and the intestinal barrier membrane.
Zonulin
Zonulin is a protein that regulates the permeability of the intestine and the detection of antibodies against zonulin indicates that the normal regulation of tight junctions is compromised. Research has found that zonulin expression is augmented in autoimmune conditions that are associated with tight junction dysfunction including celiac disease and cardiovascular disease. There are clues to the presence of an ongoing mechanism involved in damaging the intestinal barrier. Studies have also found that zonulin can possibly cause low-grade inflammation and degenerative disorders like coronary heart disease, stroke, and diabetes.
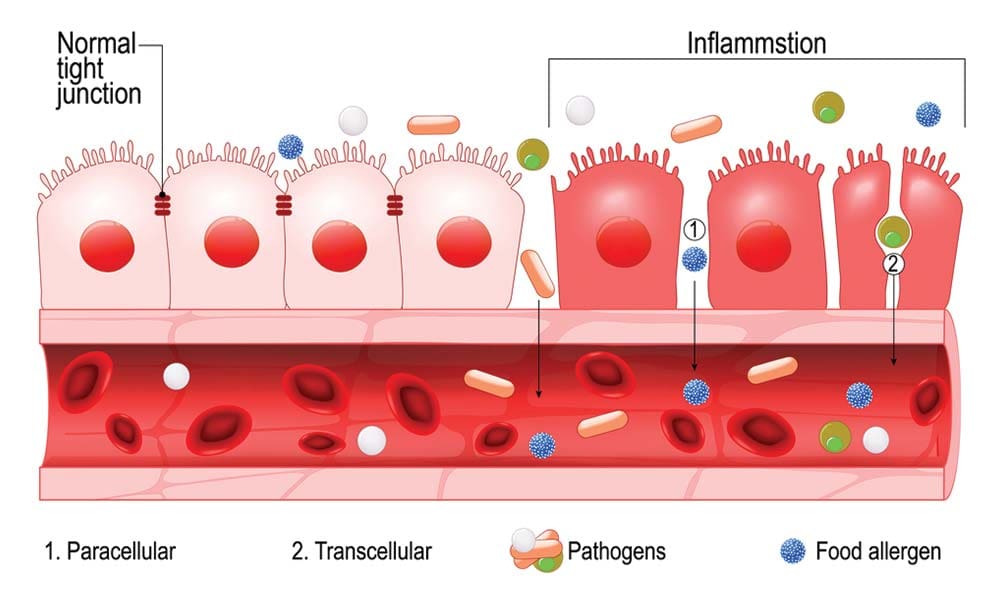
Leaky Gut
When the intestinal permeability is compromised with chronic illnesses that make holes in the intestinal walls, that is known as leaky gut. Research states that a leaky gut is caused when bad bacteria begin to cut holes and food particles and toxins start to leak out into the bloodstream. When that happens, the immune system will see these as pathogens and start to attack them causing irritation and inflammation. Leaky gut can even cause many chronic symptoms to the body that the bad bacteria outweighs the good bacteria and other symptoms that leaky gut can cause include:
- Inflammatory Bowel disease
- Small Intestinal Bacterial Overgrowth (SIBO)
- Celiac disease
- Protozoal infections
- Toxic Exposure
- Food allergy
- Chronic Alcoholism
- Diarrhea
- Strenuous exercise
- Increasing age
- Nutritional Depletions
Metabolic Endotoxemia
Metabolic endotoxemia is considered an important factor that is in developing many chronic illnesses that a person is dealing with. Research shows that when there are structural changes in the intestinal epithelium it can allow LPS into the bloodstream. LPS is common to trigger insulin resistance, obesity, diabetes, and endotoxemia increased during the fed and decreased during fasted state. This means that LPS concentration 2‐3X threshold defines metabolic endotoxemia which can dysregulate the inflammatory tone and trigger the body. Other factors that metabolic endotoxemia can do to the body are:
- Increased weight gain
- Increased markers of inflammation
- Increased triglyceride production by the liver
- Increase insulin resistance
By lowering plasma LPS concentration, it could be a potent strategy for the control of metabolic diseases and the body can start to feel better.
How To Improve Gut Microbiome Health
There are many ways to help improve gut microbiome health. One of the ways that an individual can help improve their gut is by eating soluble fibers. Soluble fibers are found in oats, beans, apples, and citrus fruits that are digested by enzymes into short-chain fatty acids (SCFAs). SCFAs are the main metabolites that are produced by the large intestine microbiota and constitute approximately 5–10% of the energy source in healthy people. By increasing dietary fibers and prebiotics in the body can help the large intestine microbiota increase production of SCFAs. Other ways to help the gut is by:
- Increase low‐mercury fish consumption
- Increase in whole plant food
- Avoid sugar and processed foods
- Eat foods like onion, leek, garlic, and dandelion greens (prebiotics are the non-digestible oligofructose, inulin, galactooligosaccharides within these plants).
- Fiber‐enriched diets improve insulin sensitivity in lean and obese diabetic subjects
HCTP Research

HCTP therapy is a form of regenerative treatment that both international and national affiliated clinics and distribution organizations use for individuals that are dealing with chronic pain. HCTP therapy helps the body’s natural healing process by regenerating damaged cells, tissues, and organs back to their original state.
Conclusion
All in all, the heat and gut microbiomes are connected to make sure that the body is functioning properly. When there are unwanted pathogens that are attacking one or the other, it can cause chronic illnesses that can cause inflammation and heart diseases to rise up. By incorporating a healthy diet that is rich in fiber, can help lower inflammation and repair the gut microbiota. With a healthy gut, the body can begin to heal and repair itself with the necessary nutrients that it needs in order to function normally.
References
Camilleri, Michael. “Leaky Gut: Mechanisms, Measurement and Clinical Implications in Humans.” Gut, U.S. National Library of Medicine, Aug. 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6790068/.
Carrera-Bastos, Pedro, et al. “Serum Zonulin and Endotoxin Levels in Exceptional Longevity versus Precocious Myocardial Infarction.” Aging and Disease, JKL International LLC, 1 Apr. 2018, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5963352/.
Cummins, Philip M. “Occludin: One Protein, Many Forms.” Molecular and Cellular Biology, American Society for Microbiology, Jan. 2012, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3255790/.
Fasano, Alessio. “Zonulin, Regulation of Tight Junctions, and Autoimmune Diseases.” Annals of the New York Academy of Sciences, U.S. National Library of Medicine, July 2012, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3384703/.
Forkosh, Esther, and Yaron Ilan. “The Heart-Gut Axis: New Target for Atherosclerosis and Congestive Heart Failure Therapy.” Open Heart, BMJ Publishing Group, 23 Apr. 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6519415/.
Mohammad, Shireen, and Christoph Thiemermann. “Role of Metabolic Endotoxemia in Systemic Inflammation and Potential Interventions.” Frontiers, Frontiers, 1 Jan. 2021, https://www.frontiersin.org/articles/10.3389/fimmu.2020.594150/full.
Novakovic, Marko, et al. “Role of Gut Microbiota in Cardiovascular Diseases.” World Journal of Cardiology, Baishideng Publishing Group Inc, 26 Apr. 2020, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7215967/.
Pastori, Daniele, et al. “Gut-Derived Serum Lipopolysaccharide Is Associated with Enhanced Risk of Major Adverse Cardiovascular Events in Atrial Fibrillation: Effect of Adherence to Mediterranean Diet.” Journal of the American Heart Association, John Wiley and Sons Inc., 5 June 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5669181/.
Tang, W H Wilson, et al. “Gut Microbiota in Cardiovascular Health and Disease.” Circulation Research, U.S. National Library of Medicine, 31 Mar. 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5390330/.
Zhang, Li-Zi, and Sun Lei. “Changes of Junctions of Endothelial Cells in Coronary Sclerosis: A Review.” Chronic Diseases and Translational Medicine, KeAi Publishing, 8 June 2016, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5643598/.
Disclaimer
Professional Scope of Practice *
The information herein on "The Gut's Role In Cardiovascular Disease | Part 2" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card