Table of Contents
Introduction
The body has specific roles for each of the systems that are inside. The musculoskeletal system makes sure that the body is moving, while the central nervous system sends signals from the brain to the rest of the body. The gut system makes sure that the body is getting the nutrients from foods and excreting out the bad toxins out of the body and the cardiovascular system is pumping blood to each of the muscle tissue and organs so the body can function. When chronic illnesses start to affect each of the body’s systems, it can cause many problems that make the body become dysfunctional. In this 2 part series, we will be taking a look at the body’s microbiome and how it plays a role in cardiovascular disease. In part 2, we will discuss how different organisms are associated with cardiovascular disease and how to improve the microbiome’s health. By referring patients to qualified and skilled providers who specialized in cardiovascular services. To that end, and when appropriate, we advise our patients to refer to our associated medical providers based on their examination. We find that education is the key to asking valuable questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, in case you are uncertain here is the link to all the insurance providers we cover. If you have any questions, please call Dr. Jimenez at 915-850-0900.
The Microbiome
The best way to describe the body’s microbiome is like a bustling city with people commuting to work. Research shows that the body’s microbiome is entirely unique to individuals and is considered a supporting organ that has many key roles in the body. The microbiota in the body can also help stimulate the body’s immune system to break down compounds, vitamins, and amino acids in the body. With the body’s ability to deal with stressors, the body needs a greater microbial diversity to deal with opportunistic pathogens or dietary perturbations that enter. Individuals with any chronic diseases are more likely to have alterations in the gut microbiome compared to healthy controls and the associations between reduced microbial diversity and illness.
Microbiome Diversity Begins at Birth
So in the formation of the gut microbiota, bacterial colonization during birth plays a major role for expecting mothers. Studies have shown that the gut microbiome can influence immunological, endocrine, and neural pathways in infant development. However, there are factors that can affect both the mother and the infant, these include:
- Premature birth
- Caesarean section versus vaginal birth
- Breast milk versus commercial formula
The study also shows that when infants are born vaginally will have a gut microbiome that is similar to the mother’s microbiota. In the vaginally-born infant’s microbiota, they will have Lactobacillus, Prevotella, or Sneathia spp in their system, while Caesarean section-born infants are colonized by bacteria found on the skin surface like Staphylococcus, Corynebacterium, and Propionibacterium species in their microbiota. When there is reduced bacterial diversity of the infant’s intestinal flora was associated with increased risk of allergic sensitization, allergic rhinitis, and peripheral blood eosinophilia.
Factors to Influence Microbiome Diversity
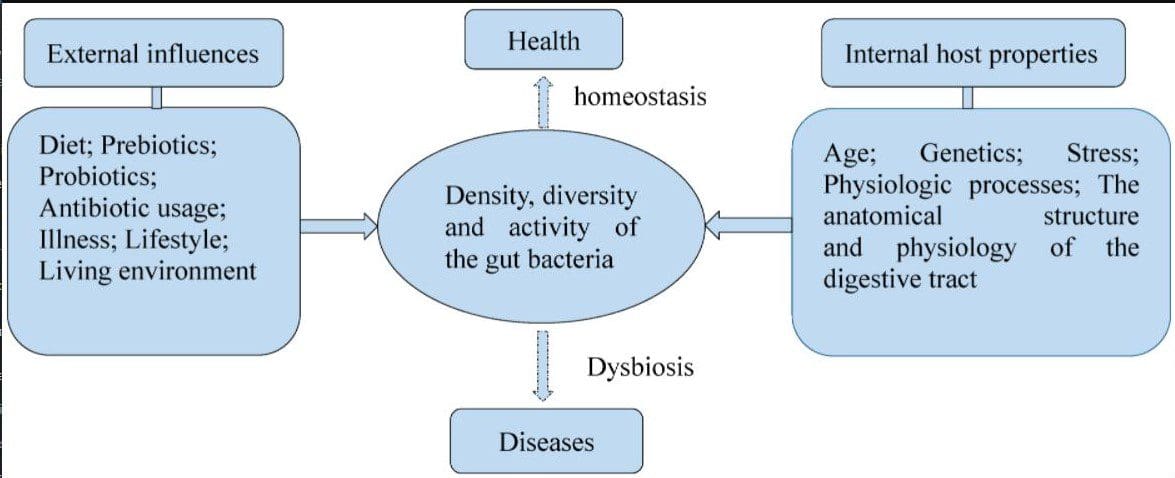
There are actually many factors that can influence the gut microbiota diversity in the body, studies have found that when the gut microbiota is being established early in the life stage and can be altered through various factors that influence the homeostasis and diversity of the microbiota. The factors that can influence the gut include:
- External influences: Diets, lifestyle, illnesses
- Health & diseases: The density, diversity, and activity of the gut bacteria
- Internal host properties: Age, genetics, stress
When there are factors that can influence the gut microbiota,s sometimes it can cause dysbiosis if there are illnesses that can affect the gut. Studies show that the mechanics that influence dysbiosis in the gut microbiota can cause intestinal disorders like IBS, metabolic syndrome, and cardiovascular disease.
HCTP Research

As a form of regenerative medicine, HCTP therapy can help the body heal faster by regenerating diseased cells, organs, and tissues back to their original forms. Both international and national affiliated clinics provide HCTP therapy services to individuals that are suffering from chronic illnesses that are affecting the body’s microbiome.
Cardiovascular Disease and The Microbiome
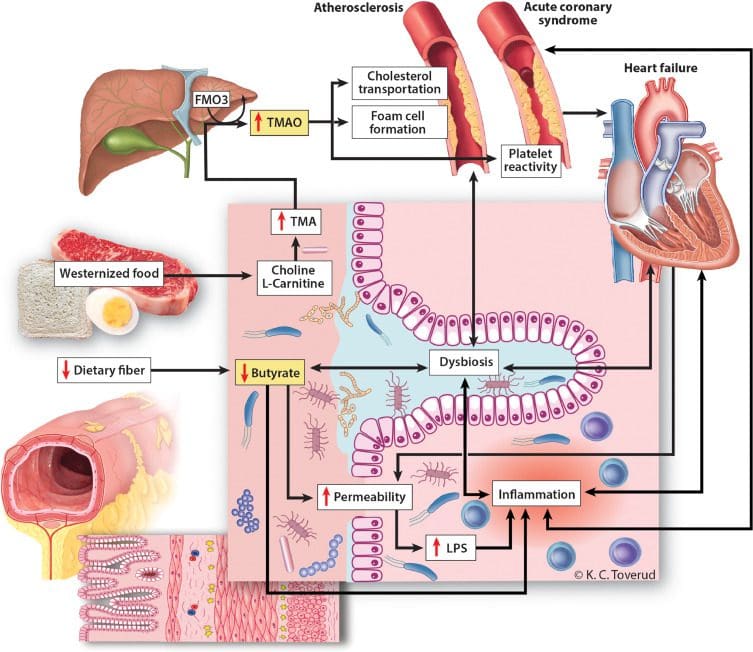
Since cardiovascular disease is one of the leading causes of mortality, it can actually cause the gut microbiota to be on the verge of dysbiosis in the body. Studies have shown that the intestinal microbiota and the body’s host interact and play a critical role in regulating human physiology. When there are deleterious changes that change the microbiota, it can cause imbalances and even activate multiple pathways in the body for cardiovascular disease risk factors to pop up. This will cause intestinal inflammation if the risk factors are not treated and even cause an increased circulation of bacterial structure components and microbial metabolites in the body to progress the development of cardiovascular diseases.
Cardiovascular Symptoms Affecting The Microbiome
When there are changes that affect the gut microbiome due to cardiovascular disease, the symptoms from CVD actually go hand in hand with gut dysbiosis. Studies have found that heart failure and impaired intestinal barrier function are the results of bacterial translocation and with its presence, it can circulate and heightened the gut’s inflammatory state. Other symptoms that cardiovascular disease and gut dysbiosis have in common include:
- Atherosclerosis
- Hypertension
- Heart failure
- Chronic kidney disease
- Obesity
- Type 2 diabetes mellitus
Conclusion
All in all, cardiovascular disease and the body’s microbiome are connected when it comes to chronic symptoms that are affecting the body. By eating a healthier diet, exercising regularly, and taking multi-vitamins and supplements that can lower the risk of cardiovascular diseases and can help flourish the microbiota’s beneficial bacteria to flourish in the gut. By lowering the risk of chronic symptoms, the body can begin the healing process, and the individual can begin living their best lives.
References
Carding, Simon, et al. “Dysbiosis of the Gut Microbiota in Disease.” Microbial Ecology in Health and Disease, Co-Action Publishing, 2 Feb. 2015, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4315779/.
Hasan, Nihal, and Hongyi Yang. “Factors Affecting the Composition of the Gut Microbiota, and Its Modulation.” PeerJ, PeerJ Inc., 16 Aug. 2019, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6699480/.
Medical Professionals, HSPH. “The Microbiome.” The Nutrition Source, 1 May 2020, https://www.hsph.harvard.edu/nutritionsource/microbiome/.
Novakovic, Marko, et al. “Role of Gut Microbiota in Cardiovascular Diseases.” World Journal of Cardiology, Baishideng Publishing Group Inc, 26 Apr. 2020, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7215967/.
Tang, W H Wilson, et al. “Gut Microbiota in Cardiovascular Health and Disease.” Circulation Research, U.S. National Library of Medicine, 31 Mar. 2017, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5390330/.
Yang, Irene, et al. “The Infant Microbiome: Implications for Infant Health and Neurocognitive Development.” Nursing Research, U.S. National Library of Medicine, 2016, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4681407.
Disclaimer
Professional Scope of Practice *
The information herein on "The Microbiome Role In Cardiovascular Disease | Part 1" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card