First, know that it is not crazy, and you’re not alone. It is difficult for individuals to achieve health and fitness goals when they don’t like to eat vegetables. Intermittent fasting, Paleo, vegan, Mediterranean, or New Nordic, almost all healthy nutrition plans require vegetable consumption to achieve optimal health. However, it is never too late to learn to enjoy vegetables. Injury Medical Chiropractic and Functional Medicine Clinic can recommend ways not just to eat vegetables because they are healthy but to truly enjoy them.
Training Oneself To Enjoy Vegetables
Everyone’s taste preferences are different.
- Many individuals grew up in homes where vegetables were prepared in unappetizing ways.
- Over boiling and steaming are common preparation methods that many had experience with, including broccoli, cauliflower, asparagus, and Brussels sprouts, which made them flavorless, mushy and is where many decided they were not going to eat these foods.
- Many don’t like vegetables because many have chemical compounds that make them taste bitter.
- If food intake is more packaged and less fresh, an individual’s palate will be more conditioned to seek out processed food’s fatty, sweet flavors.
- Some individuals may be genetically inclined to dislike vegetables.
Vegetable Purpose
Vegetables are full of nutrients that are very beneficial to the body.
- Vegetables contain antioxidants, vitamins, minerals, fiber, and phytonutrients.
- These nutrients help keep the mind and body healthy and avoid deficiencies.
- Vegetables add fiber that provides a feeling of fullness by giving volume to fill the stomach without added calories.
- This controls energy balance/calories in vs. calories out, which helps shed body fat without feeling hungry and maintain body weight.
- Vegetables feed the intestinal bacteria that help the digestive tract.
- Vegetables provide hydration that helps the fiber eliminate waste products.
- Vegetables add variety to help maintain healthy nutrition.
Branching Out
The key is to branch out incrementally. Most individuals will have a vegetable or two that they can tolerate. This could be a starting point by expanding on new variations on those tolerable vegetables that will lead to broadened taste preferences. This can be done through different cooking methods that include:
Regardless of where you’re starting, there are simple ways to make the vegetable bitterness less intense, more palatable, and more enjoyable that consists of:
- Vegetable Challenge
- Vegetable Complement
- Vegetable Cushion
Vegetable Challenge
- Pick a vegetable that you would not normally eat that requires effort to try.
- Motivate yourself to try it – health reasons, children, family, friends, etc.
- Take a small bite; you may hate it, like it, or it has no effect.
- You at least tried it.
- Research suggests that individuals may need to try new foods many times (prepared differently) before tolerating or liking them.
Vegetable Complement
- Build on flavor perception
- Well-developed recipes have flavor harmony.
- It means pairing food with a vegetable to activate various tastes and flavors pleasing to the palate simultaneously.
Vegetable Cushion
- On the tongue are a variety of receptors that bind to the chemicals in food.
- When these receptors are activated, they send a chemical signal to the brain about the taste.
- Variations in the number and type of receptors help develop flavor preferences.
- Basic tastes – sweet, sour, spicy, salty, bitter, and umami.
- Pairing bitterness with other distinct flavors, like sweet and spicy, can develop and change the brain’s perception of bland or bitter vegetables to tasty and delicious.
- Cushions for bitterness include honey, real maple syrup, sour cream, Mexican crema, hot sauce, oils, almonds, and butter used in balance to enhance and bring out flavors.
The objective is to start small and work your way to becoming more comfortable with experimenting and combining more flavors. Consultation with a professional nutritionist can help individuals get on a healthy nutrition plan that they can enjoy.
Tip From A Dietitian
References
Christoph, Mary J et al. “Intuitive Eating is Associated With Higher Fruit and Vegetable Intake Among Adults.” Journal of nutrition education and behavior vol. 53,3 (2021): 240-245. doi:10.1016/j.jneb.2020.11.015
Melis M, Yousaf NY, Mattes MZ, Cabras T, Messana I, Crnjar R, Tomassini Barbarossa I, Tepper BJ. Sensory perception of salivary protein response to astringency as a function of the 6-n-propylthioural (PROP) bitter-taste phenotype. Physiol Behav. 2017 Jan 24;173:163-173.
Mennella JA. Development of food preferences: Lessons learned from longitudinal and experimental studies. Food Qual Prefer. 2006 Oct;17(7-8):635-637.
Tordoff, Michael G, and Mari A Sandell. “Vegetable bitterness is related to calcium content.” Appetite vol. 52,2 (2009): 498-504. doi:10.1016/j.appet.2009.01.002
Wallace, Taylor C et al. “Fruits, vegetables, and health: A comprehensive narrative, umbrella review of the science and recommendations for enhanced public policy to improve intake.” Critical reviews in food science and nutrition vol. 60,13 (2020): 2174-2211. doi:10.1080/10408398.2019.1632258
Wieczorek, Martyna N et al. “Bitter taste of Brassica vegetables: The role of genetic factors, receptors, isothiocyanates, glucosinolates, and flavor context.” Critical reviews in food science and nutrition vol. 58,18 (2018): 3130-3140. doi:10.1080/10408398.2017.1353478





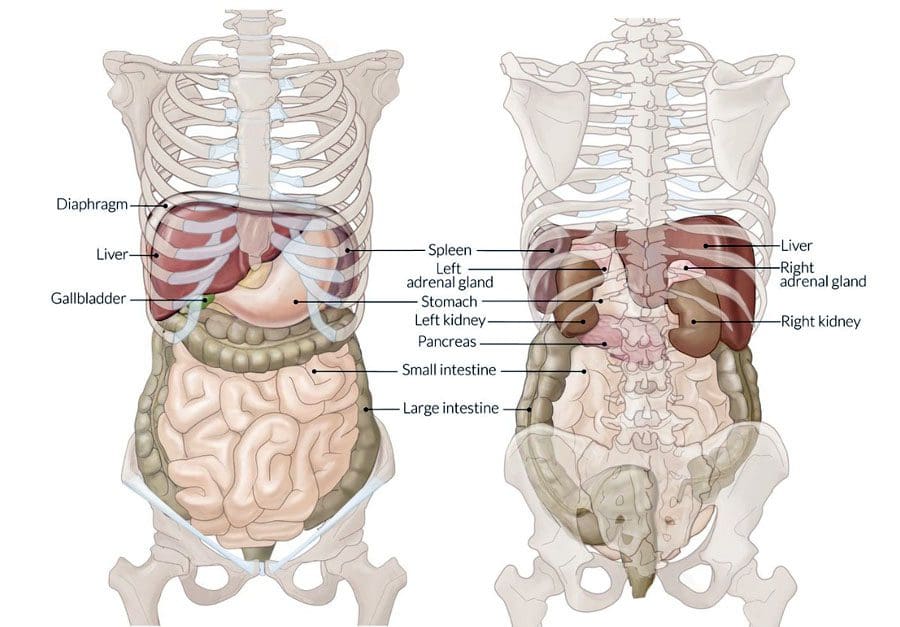 Stomach Back Pain Causes
Stomach Back Pain Causes





 Baseball Training
Baseball Training



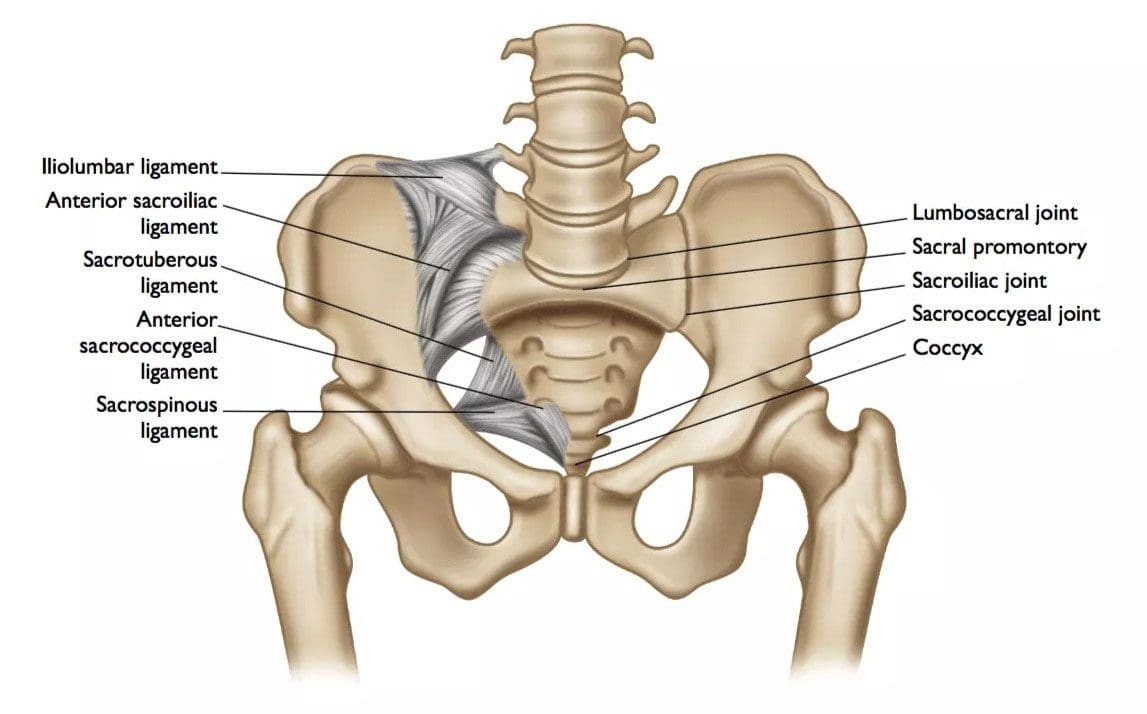 Sacroiliac Joint Surgery
Sacroiliac Joint Surgery