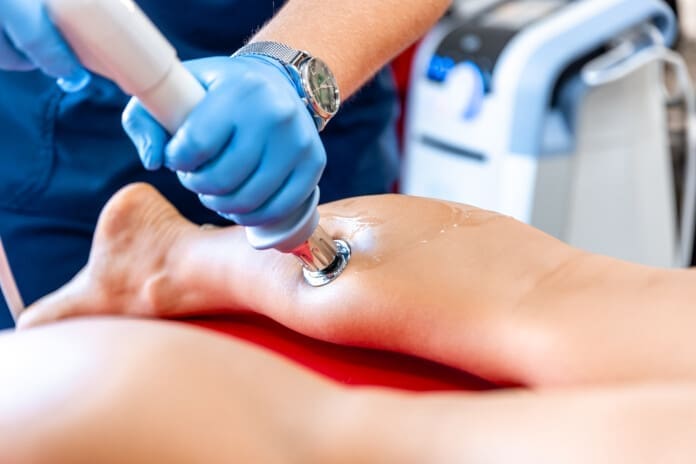
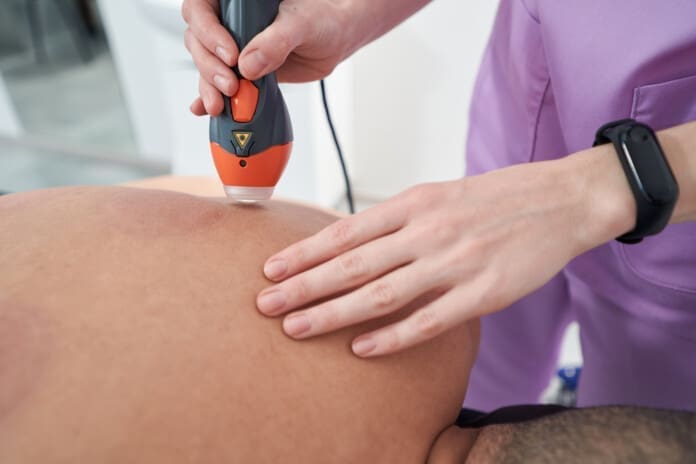
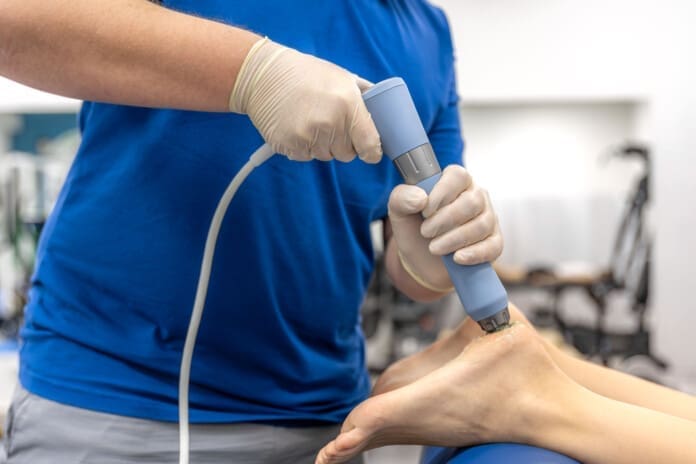
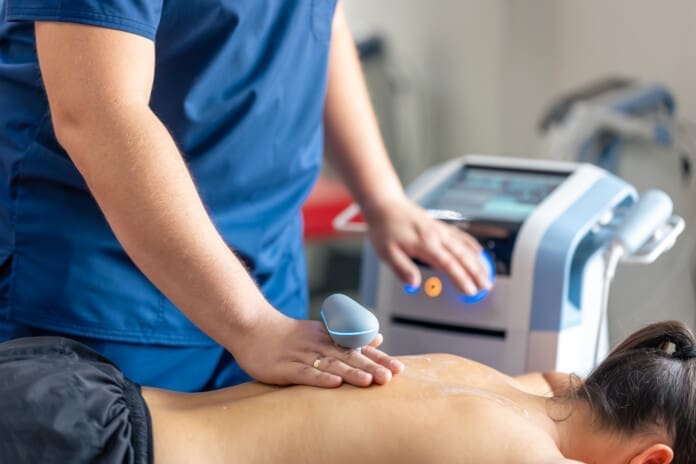
Uncover the power of therapeutic photobiomodulation for tissue regeneration, effective healing, and tissue repair.
Abstract
In this educational post, I walk you through how I assess and implement modern photobiomodulation (PBM) protocols using multiwavelength, pulsed MLS laser systems for low back pain, facet-mediated joint stiffness, and lower-extremity arthritic pain. I translate device setup into clinical reasoning, explain why energy density (J/cm²) matters more than total joules, and show how to combine robotic and handheld lasers for target precision and tissue coverage. I discuss dosing for acute vs. chronic conditions; how to avoid bioinhibition and thermal overload; and how integrative chiropractic care—manual therapy, neuromuscular re-education, targeted mobility, and metabolic optimization—fits into a comprehensive, evidence-based protocol. I also outline practical pathways for pairing laser therapy with orthobiologics (e.g., PRP) to enhance outcomes, address mitochondrial and inflammatory mechanisms, and sequence care from preparation to post-injection recovery. Clinical insights reflect my day-to-day observations with patients at my rehab-focused practice and the literature from leading researchers in PBM, neuromusculoskeletal pain, and regenerative medicine.
Patient-Centered Setup: Comfort, Precision, and Safety
As a clinician, the priority is simple: patient comfort and positioning. When I set up for low back pain—especially suspected facet irritation around L4-L5—I prefer the patient prone, with direct skin access for accurate targeting. With MLS robotic platforms, stable positioning is crucial; if the patient shifts during treatment, the beam may drift off the intended region.
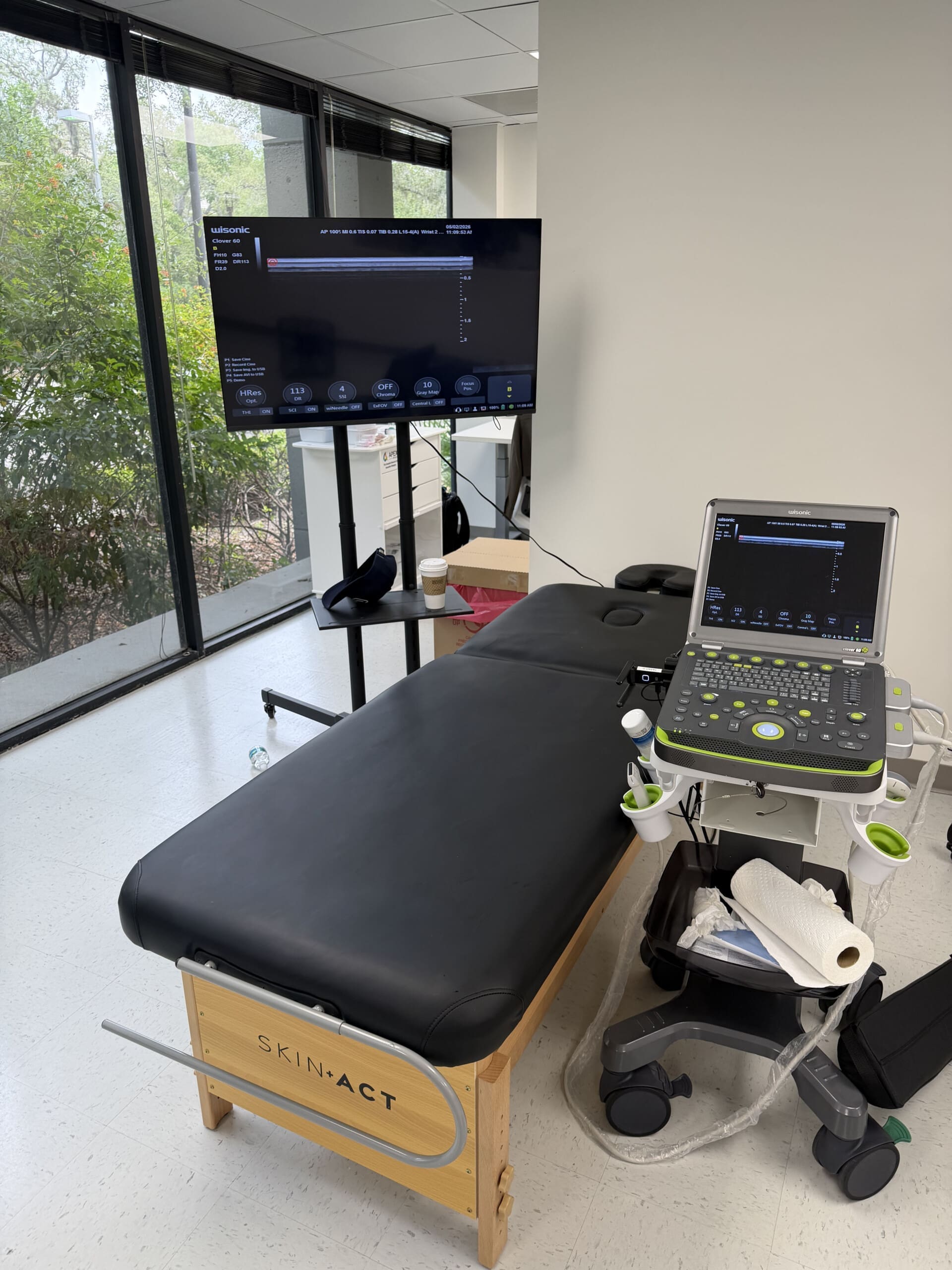
Key clinical steps I follow:
- Ensure the treatment area is exposed and comfortable to minimize movement.
- Palpate and identify the patient’s symptomatic corridor (e.g., paraspinals, facet line) and any radiating points.
- Center the robotic head over the primary pain generator and adjacent fascial/connective tissue networks to create a therapeutic field, not just a dot.
- Confirm the device-to-skin distance using the supplied ruler at the robot’s focal plane; handheld diodes are placed directly on the skin.
Why this matters:
- The MLS system employs a collimated multi-diode beam whose focal characteristics demand a consistent distance to maintain fluence.
- Comfort stabilizes the patient and preserves dose fidelity.
- Covering the symptomatic region plus the fascial continuity supports a more complete neuromyofascial response rather than a single-point analgesic effect.
Why We Treat Energy Density, Not Just Total Joules
In photobiomodulation, I target an energy density—typically 4–10 J/cm²—rather than chasing a total number of joules. Energy density (fluence) is the biologically relevant “dose” per unit area that tissues respond to.
Key points:
- For lumbar facet pain and paraspinal myofascial involvement, I often target approximately 6 J/cm² with pulsed, dual-wavelength MLS (808 nm + 905 nm).
- Robotic software that automatically recalculates treatment time as you adjust the X–Y treatment area is clinically valuable; it preserves the intended J/cm² without manual calculation errors.
- I avoid “overcooking” tissue. Excess fluence can move past the optimal biphasic window (Arndt-Schulz law), risking bioinhibition where therapeutic effects plateau or reverse.
Physiology in focus:
- At appropriate fluences, photons are absorbed by mitochondrial chromophores (notably cytochrome c oxidase) and secondary photoacceptors, thereby increasing electron transport chain efficiency and ATP synthesis, and modulating reactive oxygen species (ROS) within a hormetic window.
- These changes alter transcription factors (e.g., NF-κB, Nrf2), downregulate pro-inflammatory cytokines (e.g., TNF-α, IL-1β), and upregulate antioxidant defenses, thereby promoting tissue repair and analgesia (Anders et al., 2015; Hamblin, 2016).
- Too much energy can elevate ROS beyond the hormetic range, dampen beneficial signaling, or generate superficial heating without deeper benefit.
Clinical takeaway: Energy density aligns dosing to tissue biology. I set J/cm² for the target pathology and let the device time adjust to the area, not the other way around.
Dual Modality Targeting: Robotic Coverage Plus Handheld Precision
I frequently combine:
- The robotic head (multi-diode, set off the skin at a defined focal distance) for broader coverage of the pain region and surrounding connective tissue.
- The handheld diode (single diode, on-skin) for precise trigger points, facet line, joint spaces, and dynamic maneuvers.
Why both?
- The robot blankets the primary painful field and adjacent myofascial lines, ensuring a uniform dose.
- The handheld allows “search-and-treat” for taut bands and nodules—what some clinicians colloquially call “cooked meat” compared to soft “raw meat.” In practice, this means targeting dense, hyperirritable loci within muscle or periarticular tissue that perpetuate nociception and altered motor patterns.
Physiological rationale:
- Trigger points often harbor local ischemia, altered nociceptive neurochemistry, and dysfunctional endplate potentials. PBM may enhance microcirculation, normalize motor endplate behavior, and reduce peripheral sensitization (Dompe et al., 2020).
- Treating both field and foci reduces central nociceptive drive and restores segmental mobility.
The Science Behind MLS Pulsing: High Peak, Short Pulse, Thermal Neutrality
The MLS configuration pairs an 808 nm continuous/semicontinuous component with a 905 nm superpulsed component, reaching high peak powers with very short duty cycles. This creates a “pulsed punch”: ample photon delivery during pulses with intervening off-time for heat dissipation.
Why this matters clinically:
- Tissue temperature over time remains relatively stable despite high peak power; perceived warmth is minimal. Patients may note mild warmth or tingling, but thermal buildup is not the goal.
- Short pulses and rest periods facilitate deeper photon penetration by reducing superficial thermal saturation and allowing photons to reach chromophores at depth without overheating the epidermis (Hamblin, 2016; Chung et al., 2012).
- If you feel excessive heat at the surface, the wavelength, pulse pattern, or fluence may be mismatched to the tissue’s absorptive and conductive properties.
In my clinic, maintaining thermal neutrality preserves comfort, prevents defensive muscle guarding, and supports cumulative dosing strategies.
Acute vs. Chronic Dosing: Building a Cumulative Response
PBM effects are cumulative. I align intensity and cadence to the condition’s acuity and the tissue response curve.
Typical programs I use:
- Acute conditions
-
- 6 sessions as a starting block
- Aim for 24-hour spacing; practical cadence is 3 sessions/week (e.g., Monday–Wednesday–Friday)
- Early gains often appear after 1–3 sessions as nociceptive and microcirculatory effects mount
- Chronic conditions
-
- 12-session series to cross an efficacy threshold, again 3 sessions/week if possible
- Patients often feel better after 3–5 sessions; however, stopping early risks regression before adaptive changes consolidate.
Why complete the series?
- PBM modulates neuroimmune signaling over time. Premature cessation often leads to symptom rebound because central sensitization and dysfunctional motor patterns are not fully remodeled.
- Completing a planned series ensures adequate dose density across all involved tissues and permits layering integrative chiropractic interventions that stabilize new movement patterns.
Integrative Chiropractic Care: Where PBM Fits
PBM is a powerful adjunct within an integrative chiropractic model—not a replacement for precise manual and movement care. My approach typically includes:
- Spinal and joint assessment
-
- Identify segmental restrictions, facet tenderness, and load-intolerant planes of motion.
- Correlate with functional movement screens and neurologic findings.
- Manual therapies and adjustments
-
- Use gentle mobilization or HVLA where appropriate to restore joint play and reduce reflexive guarding.
- Employ soft-tissue techniques on the paraspinals, gluteals, hip rotators, and thoracolumbar fascia to normalize tone.
- Neuromuscular re-education
-
- Retrain lumbo-pelvic control (e.g., abdominal canister activation, hip hinge, gluteal sequencing).
- Introduce graded exposure to movement to reduce fear-avoidance and central sensitization.
- PBM sequencing
-
- Apply robotic coverage to the pain field and handheld precision to focal generators before or after manual work, depending on irritability.
- In irritable states, I often lead with PBM to reduce pain and muscle guarding, then mobilize.
- In stiff, less-irritable states, I mobilize first to restore alignment and immediately follow with PBM to consolidate an anti-inflammatory, pro-repair milieu.
- Lifestyle and load management
-
- Educate on spine-sparing strategies and progressive loading to avoid re-igniting nociceptive input while tissues recondition.
Clinical observation: By pairing PBM with targeted chiropractic adjustments and corrective exercise, I observe faster reductions in morning stiffness, improved flexion tolerance, and more durable outcomes—particularly for facet-mediated low back pain and degenerative knee complaints. See ongoing case reflections and protocols at my practice sites: sciatica.clinic and linkedin.com/in/dralexjimenez.
Knee Osteoarthritis: Anterior, Posterior, and Compartment-Specific Dosing
For knee OA, geometry matters. Treating only the anterior knee risks energy reflection by the patella. I typically:
- Position the knee in gentle flexion to open the joint space.
- Treat the anterior, posterior, and compartment-specific zones based on symptoms and imaging findings.
- Maintain target energy density per zone (e.g., 4–10 J/cm²), rather than diluting dose by spreading the same joules too thinly across multiple compartments.
Rationale:
- Posterior coverage improves access to the synovium and the posterior capsule, where inflammatory mediators accumulate.
- Compartmental dosing acknowledges localized cartilage wear, meniscal pathology, and capsular fibrosis, each of which contributes to nociception and stiffness.
Expectation management:
- PBM does not regenerate cartilage in bone-on-bone disease; it modulates pain and inflammation and may improve function, often delaying surgery.
- When combined with integrative chiropractic care, strengthening, weight optimization, and gait retraining, patients commonly report smoother movement and improved daily capacity.
Fracture Care and Bone Considerations: Practical Realities
While certain fracture applications may be off-label depending on jurisdiction, clinicians have reported potential benefits when initiated early (approximately within 7–10 days) to influence the inflammatory and early reparative phases. My caution:
- PBM does not “penetrate” cortical bone the way ionizing modalities do; rather, effects are mediated through soft tissues, periosteum, marrow interfaces, and systemic signaling.
- Nonunion states may be less responsive to PBM alone. Multimodal strategies (e.g., orthobiologics, mechanical stabilization, metabolic optimization) are often required.
Timing principle:
- Early PBM can modulate inflammatory cytokines and microcirculation, potentially supporting callus formation, but individual case factors dominate (stability, vascularity, comorbidities).
Exploring Integrative Medicine- Video

Orthobiologics Synergy: Preparing, Protecting, and Progressing
When integrating PBM with platelet-rich plasma (PRP) or similar biologics, I consider three phases:
- Preparation (Pre-injection priming)
- 2–3 PBM sessions aimed at improving local perfusion, downregulating excessive baseline inflammation, and optimizing cellular redox status.
- Practical objective: “Prepare the soil” so injected biologics interact with a receptive microenvironment.
- Day-of-injection support
- Adjust PBM parameters to avoid blunting the intended early inflammatory signaling of PRP while supporting comfort and microcirculation.
- Evidence suggests PBM can augment cellular energy systems and modulate inflammation without negating necessary regenerative cascades when properly dosed (Ferraresi et al., 2016).
- Post-injection consolidation
- Approximately 6 PBM sessions spaced to respect the PRP’s pro-inflammatory window (often 7–10 days for certain protocols) and the tissue’s remodeling timeline.
- Goal: Amplify mitochondrial efficiency, temper excessive inflammation, and support functional reintegration as loading resumes.
Why it works:
- PBM increases ATP availability and modulates mitochondrial biogenesis signals, potentially enhancing the metabolic competence of local cells that receive growth factors from PRP.
- In my clinic, I see greater pain reduction and a faster return to graded activity when PBM is integrated into orthobiologic care—especially in tendinopathies and knee OA.
Mitochondria, Inflammation, and the Acute-to-Chronic Cascade
A common question is how PBM spans immediate pain relief to longer-term remodeling. My clinical and research-informed view:
- Early effects (minutes to hours)
-
- Improved microcirculation and nitric oxide dynamics can reduce ischemic nociception.
- Peripheral nerve modulation may reduce the intensity of pain signals.
- Patients often describe easier movement the same day; I re-test function 4–6 hours post-session to capture early change.
- Intermediate effects (days)
-
- Mitochondrial upregulation supports ATP-dependent repair processes and ion homeostasis.
- Modulated cytokine profiles (↓TNF-α, ↓IL-1β, ↑anti-inflammatory mediators) shift the inflammatory milieu toward resolution rather than persistence.
- Longer-term effects (weeks)
-
- Repetitive PBM creates a pro-repair environment while integrative chiropractic care restores biomechanics and motor control.
- Together, they reduce the risk of central sensitization and improve tissue quality through consistent, sub-threshold mechanical loading.
Medication considerations:
- Some medications (e.g., statins) influence mitochondrial function; this may shape PBM responsiveness.
- In my practice, I collaborate with patients’ prescribing clinicians to assess cardiometabolic risks and, when appropriate, explore evidence-based mitochondrial support (e.g., CoQ10, creatine, riboflavin). These choices are individualized and medically coordinated.
Avoiding Bioinhibition and Thermal Pitfalls
Bioinhibition and surface heating reduce effectiveness. My safeguards include:
- Prioritize energy-density targets and avoid piling redundant doses in one spot. If additional time is needed, cover adjacent vectors (e.g., anterior-posterior or medial-lateral) rather than stacking on the same locus.
- Monitor patient sensation; PBM should be comfortable with minimal heat.
- Adhere to a consistent schedule to build cumulative benefits without overshooting per-session tissue tolerance.
Putting It All Together: A Sample Low Back Protocol
For a patient with right-sided L4–L5 facet-mediated low back pain and paraspinal stiffness:
- Visit 1–4 (first 10 days)
-
- PBM: 6 J/cm² over the symptomatic corridor using the robot, with handheld precision to facet line and trigger points.
- Integrative chiropractic: Gentle mobilization or HVLA (if indicated), soft tissue work to paraspinals and hip rotators, diaphragmatic breathing, and isometric glute activation.
- Education: Avoid provocative sustained flexion/extension; incorporate short movement snacks.
- Visit 5–8 (next 7–10 days)
-
- PBM: Maintain 6–8 J/cm²; expand coverage to include thoracolumbar fascia and contralateral stabilizers if compensations present.
- Progress exercise: Hip hinge patterns, anti-rotation core work, and graded walking.
- Visit 9–12 (final 10 days in block)
-
- PBM: Taper to 4–6 J/cm² as symptoms improve, focusing on durability and symmetry.
- Integrative chiropractic: Emphasizes load tolerance, lifting mechanics, and return to desired activities.
If PRP is planned for refractory facet or SI-mediated pain:
- Add 2–3 PBM sessions pre-PRP for microenvironment prep, adjust parameters day-of, and schedule 6 post-PRP sessions respecting the regenerative timeline.
What Patients Feel and When to Re-Test
Most patients feel little during treatment—sometimes light warmth or tingling. I ask them to re-assess functional tests (bend, twist, walk) about 4–6 hours after the session. For example, if treatment occurs at 11:00, I ask them to test at around 17:00 on the same day to gauge the early response. Sustained improvements typically consolidate across 3–5 visits, with fuller benefits unfolding by session 6–12, depending on chronicity.
Durability, Workflow, and Practice Integration
Modern MLS systems are engineered for reliability, with on-site service networks reducing downtime. In practice, I streamline workflow by:
- Using the robotic head for standardized area dosing.
- Adding handheld passes for focal generators.
- Building care plans in packages (e.g., 6 or 12 sessions) to ensure cumulative dosing and patient adherence.
- Synchronizing PBM with manual care blocks and exercise progressions.
This integrated approach yields consistent outcomes and aligns with how tissues biologically adapt: by repeated, well-dosed inputs over time.
Evidence Highlights and Ongoing Learning
Leading research supports PBM’s effects on mitochondrial activity, inflammation modulation, analgesia, and tissue repair signaling across musculoskeletal conditions. Dual-wavelength, pulsed systems are designed to balance depth, dose, and thermal neutrality, aligning with clinical goals of pain reduction and functional restoration (Chung et al., 2012; Hamblin, 2016; Ferraresi et al., 2016; Dompe et al., 2020). As always, patient selection, precise dosing, and integrative care pathways are the difference-makers.
For more of my clinical observations and case-driven insights, visit my resources:
References
- Photobiomodulation for the treatment of musculoskeletal pain: an update for clinicians (Chung, H., Dai, T., Sharma, S. K., et al., 2012). Seminars in Cutaneous Medicine and Surgery, 32(1), 41–52.
- Mechanisms and applications of the anti-inflammatory effects of photobiomodulation (Hamblin, M. R., 2016). AIMS Biophysics, 3(3), 337–361.
- Photobiomodulation and mitochondria: biogenesis, bioenergetics, and signaling (Ferraresi, C. et al., 2016). Journal of Photochemistry and Photobiology B: Biology, 155, 1–8.
- Photobiomodulation—biological mechanisms and clinical applications (Dompe, C. et al., 2020). Journal of Clinical Medicine, 9(6), 1724.
- World Association for Laser Therapy (WALT) recommendations on PBM dosing (Access guidelines for condition- and wavelength-specific parameters).
- Consensus on laser therapy parameters for musculoskeletal conditions (Clijsen, R. et al., 2017). Physiotherapy Research International, 22(2), e1662.
In-text citations (APA-7): (Chung et al., 2012; Hamblin, 2016; Ferraresi et al., 2016; Dompe et al., 2020; WALT, n.d.; Clijsen et al., 2017)
SEO tags: photobiomodulation, MLS laser therapy, low back pain, facet joint pain, knee osteoarthritis, integrative chiropractic, mitochondrial function, inflammation modulation, PRP synergy, regenerative medicine, energy density J/cm2, pulsed laser, chiropractic rehabilitation, sciatica clinic, Dr. Alexander Jimenez