Table of Contents
Exercise Routine Optimization in El Paso, TX: How to Build a Weekly Workout Plan With Smart Warm-Ups and Cool-Downs

If you want real fitness results, the secret is not a “perfect” workout. The secret is a repeatable weekly plan you can stick to.
In El Paso, a healthy routine should balance:
-
Strength training (to build muscle and protect joints)
-
Cardio (to support your heart, lungs, and endurance)
-
Mobility (to move better and reduce stiffness)
-
Recovery (to avoid burnout and overuse injuries)
It also needs to be suitable for desert climates, where heat and dry air can affect hydration, energy, and training safety.
Below is a practical approach to organizing a weekly workout regimen (3–5 days per week), including warm-ups and cool-downs, and how integrative chiropractic care can help you move better, train smarter, and reduce injury risk.
What a “balanced” weekly workout plan looks like
Most beginners and intermediate exercisers do best with 3–5 training days per week, because it’s enough frequency to improve without leaving too little room for recovery. Many plans rotate upper-body, lower-body, full-body, and cardio days to avoid overworking the same muscles back-to-back.
A balanced week usually includes:
-
2–3 strength days (full body or split days)
-
2–3 cardio sessions (some can be shorter)
-
Daily “micro-mobility” (5–10 minutes counts)
-
At least 1 true rest day (or very light active recovery)
This approach aligns with common public health targets, such as 150 minutes/week of moderate activity and 2 days/week of muscle-strengthening activities.
El Paso-specific planning: desert climate + local convenience
Heat and timing matter
In warm weather, the body works harder to cool itself down. That can increase the risk of fatigue and dehydration. One simple strategy is to plan outdoor workouts earlier in the morning or later in the evening (and avoid the hottest midday hours when possible).
Hydration matters more than people think
Dry heat can make you lose fluid faster, even if you don’t feel “soaked.” A safe baseline is:
-
Drink water before, during, and after training
-
For longer/hotter sessions, consider electrolytes (especially if you sweat heavily), and tailor them to your needs and health conditions
Use local options to stay consistent
Consistency is easier when your workouts are close to home or work. In El Paso, many people rotate between:
-
A gym or strength sessions indoors (good for heat control)
-
A class-based option for motivation
-
Yoga or mobility sessions for recovery
For example, some local guides highlight places like Shanti Yoga for yoga-based mobility and recovery.
And boot-camp-style group classes (like Fit Body Boot Camp) are designed to fit busy schedules with shorter sessions.
Warm-up and cool-down: the simple 5–10 minute rule
A safe weekly plan is not just what you do—it’s also how you start and finish each session.
Why warm up?
A warm-up is typically a lower-intensity workout at the start. When done well, it helps prepare your cardiovascular system and muscles for greater effort and may reduce soreness and the risk of injury.
Why cool down?
A cool-down gradually reduces your effort, helping your body transition out of training more smoothly. Many guidance sources recommend slowing down for about 5–10 minutes, then stretching if it helps you feel better and move more freely.
The “plug-and-play” warm-up (5–10 minutes)
Think dynamic (moving) stretches and light movement.
A simple dynamic warm-up template:
-
2 minutes easy cardio: brisk walk, light bike, easy row
-
1 minute joint circles: ankles, hips, shoulders
-
2 minutes of movement prep (choose 2–3):
-
Bodyweight squats
-
Hip hinges (hands on hips, small range)
-
Arm circles/band pull-aparts
-
-
2–3 minutes of workout-specific prep:
-
If lifting: do 1–2 lighter “ramp-up” sets
-
If running: start slow and build pace gradually
-
Quick tip: Warm up large muscle groups first, then target the workout’s specific muscles.
The “easy exit” cool-down (5–10 minutes)
Consider downshifting, breathing, and static stretching (if it feels good).
A simple cool-down template:
-
3–5 minutes easy movement: slow walk, easy cycling, gentle rowing
-
2–5 minutes of static stretching (hold 10–30 seconds each):
-
Calves
-
Hamstrings
-
Hip flexors
-
Chest/shoulders
-
Upper back
-
The stretch should feel strong but not painful—no bouncing.
Choose your weekly schedule: 3-day, 4-day, or 5-day options
Below are realistic schedules you can use immediately. Pick the one you can repeat most weeks.
Option A: 3 days/week (beginner-friendly and sustainable)
This works well if you’re rebuilding consistency or balancing a busy schedule.
-
Mon: Full-body strength + short cardio finisher
-
Wed: Cardio + mobility
-
Fri: Full-body strength + core
-
Weekend: One optional light activity (walk, easy hike, yoga) + one rest day
Full-body days are often recommended when you train 2–3 times per week because they’re time-efficient.
Option B: 4 days/week (upper/lower split + cardio)
This is a classic structure: you train hard, but each area gets recovery time.
-
Mon: Lower-body strength
-
Tue: Upper-body strength
-
Thu: Lower-body strength + core
-
Fri or Sat: Upper-body strength + short cardio
Split routines help organize training volume and recovery across the week.
Option C: 5 days/week (strength + cardio + active recovery)
This is great if you like shorter workouts and frequent movement.
-
Mon: Cardio + upper-body strength
-
Tue: Cardio + lower-body strength
-
Wed: Active recovery (walk + mobility)
-
Thu: Lower-body (glute focus) or full-body strength
-
Fri: Upper-body + core
-
Sat: Optional easy cardio or yoga
-
Sun: Rest
This style matches many popular weekly plans that blend strength, cardio, and recovery days.
What to do inside each workout (so you don’t waste time)
A simple strength-training structure (45–60 minutes)
Use this order:
-
Warm-up (5–10 min)
-
Main lift (10–15 min)
-
Squat pattern, hinge pattern, press, or pull
-
-
Accessory work (15–25 min)
-
2–4 movements that support joints and balance the body
-
-
Core or carry (5–10 min)
-
Cool-down (5–10 min)
A weekly rotation of upper-, lower-, and full-body sessions is commonly used to maximize results without overtraining.
Examples of “big rock” movements (choose based on your ability):
-
Lower body: squat, deadlift pattern, lunges
-
Upper body: rows, presses, pull-downs/pull-ups
-
Full body: loaded carries, light kettlebell hinge patterns
Cardio: keep it simple
Cardio does not have to be complicated. Rotate options to reduce boredom:
-
Incline walking
-
Bike
-
Rowing machine
-
Swimming (if available)
-
Intervals 1–2x/week if your joints tolerate it
Mobility and recovery: the “missing piece” that keeps you training
If you want to stay consistent, recovery is not optional. It’s part of the plan.
Easy recovery tools that work in real life:
-
20–40 minute easy walk on recovery days
-
5–10 minutes of mobility before bed
-
Light stretching after workouts
-
Sleep and hydration as “training multipliers”
In Dr. Jimenez’s clinical writing, a common theme is that people do better when they build fitness around better movement quality—not just “more effort.” His posture-focused and movement-based content repeatedly highlights mobility, control, and consistency as the foundation for progress.
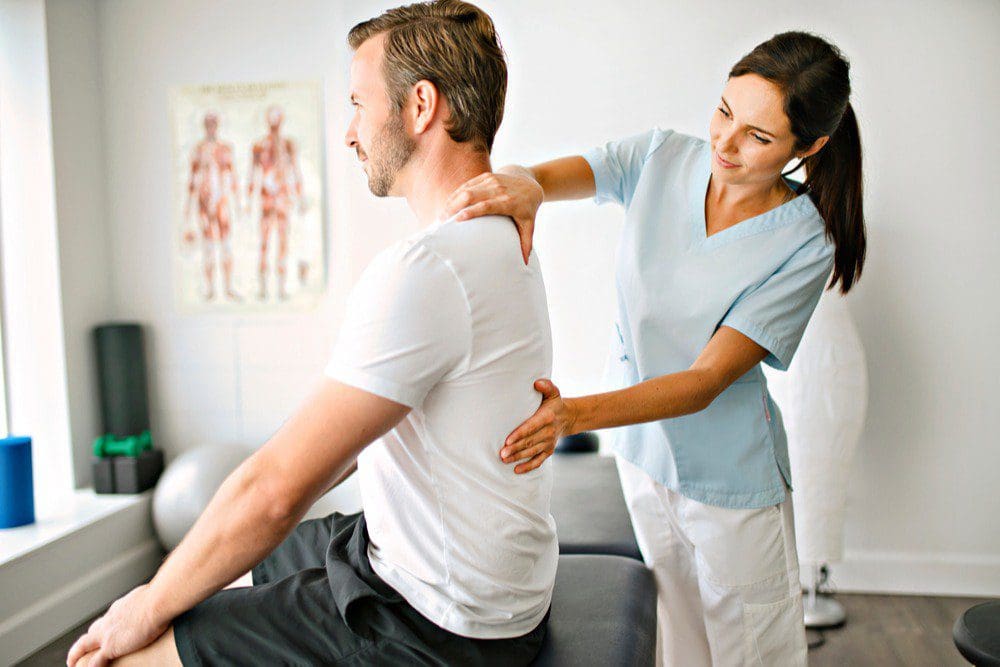
How integrative chiropractic can optimize your weekly routine
When people say they want to “work out more,” what they often mean is:
-
“I want to train without flare-ups.”
-
“I want my neck, back, hips, or shoulders to stop limiting me.”
-
“I don’t want to keep restarting after injuries.”
Integrative chiropractic care is often used for performance and recovery support, especially when it includes movement coaching and exercise guidance.
Common training problems chiropractic care may help address
-
Stiff joints limiting the range of motion
-
Postural strain patterns (desk work + phone posture)
-
“Compensation” patterns (one hip takes over, one shoulder pinches)
-
Recurring tightness that keeps coming back
A common integrative approach includes:
-
Joint and spinal assessment
-
Soft tissue strategies
-
Corrective exercises
-
Movement retraining for better mechanics
Dr. Alexander Jimenez’s clinical observations (practical takeaways)
Across Dr. Jimenez’s educational content, he repeatedly emphasizes training outcomes tied to:
-
Posture and movement quality (how you move daily, not just in the gym)
-
Warm-ups with dynamic movement, followed by cool-down stretching to reduce tightness and improve mobility
-
Neuromuscular coordination—getting the brain-body connection working better so lifts and cardio feel smoother and safer
He also highlights how integrative care can support long-term training by identifying small movement problems early—before they become injuries.
A simple weekly checklist (so you stay consistent)
Use this as your weekly “scorecard”:
-
✅ 3–5 workouts completed (based on your plan)
-
✅ Every session had a 5–10 minute warm-up
-
✅ Every session had a 5–10 minute cool-down
-
✅ 2–3 strength sessions
-
✅ 2–3 cardio sessions (some can be short)
-
✅ 1 recovery day (walk + mobility)
-
✅ Hydration plan for the desert climate

Safety note (important)
If you have chest pain, fainting, severe shortness of breath, new neurologic symptoms (like weakness or numbness spreading), or a recent injury that’s getting worse, get medical care right away. And if you’re returning after an injury, it can help to get a personalized plan from a licensed clinician.
References
American College of Sports Medicine. (2007). Exercise and fluid replacement (Position Stand).
American Heart Association. (2024, January 12). How to be active safely in warm weather.
American Heart Association. (2024, January 16). Warm up, cool down.
EōS Fitness. (2024, June 15). Workout routine: How to create your weekly gym routine.
Fit Body Boot Camp. (n.d.). Fit Body Boot Camp gym in El Paso, TX.
Fit Body Boot Camp. (n.d.). 30-minute workout in El Paso, TX.
Fox Lexus of El Paso. (2020, August 12). Sweat it out at these El Paso workout spots.
Grinder Gym. (2025, March 17). How we structure your weekly workouts for maximum results.
Health. (n.d.). Weekly workout plan: A 7-day routine for strength and cardio.
Hancock Health. (n.d.). Aerobic exercise: How to warm up and cool down.
ISSA. (2022, March 4). How to structure a gym workout for optimal results.
Jimenez, A. (n.d.). Integrative chiropractic + NP care for lasting wellness.
Jimenez, A. (n.d.). Physical activities to improve posture with chiropractic support.
Jimenez, A. (n.d.). Tight hips and hamstrings and back pain treatment.
Jimenez, A. (n.d.). Sit and reach test for lower back and hamstring flexibility.
Jimenez, A. (n.d.). Neuromuscular retraining after accidents and healing.
Mayo Clinic. (2023, August 31). Aerobic exercise: How to warm up and cool down.
Mayo Clinic Press. (2025, March 11). How to warm up and cool down for exercise.
Military.com. (2024, July 10). How to adapt your hydration and nutrition when working out in extreme heat.
Mountain Movement Center. (n.d.). Integrating chiropractic into your fitness routine.
One Medical. (2023, July 18). 6 tips for safe summer workouts in the heat.
PushAsRx. (2026, January 28). Integrative chiropractic prevents future injuries for athletes.
Shanti Yoga. (n.d.). Shanti Yoga – El Paso.


























![What’s Causing Your Sciatica? [Tests and Treatment At Home]](https://i.ytimg.com/vi/JJj2hlBGDOk/maxresdefault.jpg)











