Can Old Car Accident Injuries Still Improve? How Chiropractic, PRP, MFAT, MLS Laser, and Shockwave Therapy May Help
Introduction: Old Injuries Can Still Matter
Yes, people with long-term, chronic, or unresolved injuries from motor vehicle accidents can still benefit from a well-planned integrative care approach. Even if the crash happened months or years ago, the body may still carry hidden soft tissue damage, joint irritation, ligament strain, tendon injury, nerve sensitivity, or spinal dysfunction. These problems may not always heal fully with rest, pain medicine, or time alone.
A motor vehicle accident can injure muscles, ligaments, tendons, joints, nerves, and spinal tissues. Some injuries appear right away, while others build slowly and become chronic pain problems later. ChiroMed notes that accident recovery may include chiropractic care, rehab, shockwave therapy, platelet-rich plasma, platelet-poor plasma, and microfragmented adipose tissue when clinically appropriate.
The goal is not simply to cover up pain. The goal is to locate the source of pain, improve movement, calm inflammation, support tissue repair, and help the body function better.

Why Pain Can Last Months or Years After an MVA
After a crash, the body may go into protection mode. Muscles tighten. Joints stiffen. The spine may lose normal motion. Ligaments may become stretched or weakened. Tendons and soft tissues may form scar tissue. Over time, these changes can create a cycle of pain and poor movement.
Common long-term MVA problems may include:
- Neck pain and whiplash symptoms
- Low back pain
- Shoulder, hip, knee, or ankle pain
- Headaches linked to neck injury
- Sciatica or nerve irritation
- Stiffness after sitting, standing, or driving
- Pain that flares with activity
- Weakness, guarding, or poor posture
- Lingering soft tissue pain
This is why chronic accident pain should not be dismissed as “just old pain.” In some people, the original injury never fully healed. Instead, it became a “latent” soft tissue injury that continues to affect movement and comfort.
The Idea of “Restarting” Healing
When a soft-tissue injury does not heal properly, the body may settle into a low-grade chronic pain pattern. The tissue may be weaker, less flexible, and more sensitive than it should be. Regenerative medicine is designed to support the body’s natural repair signals.
Platelet-rich plasma, or PRP, is made from a patient’s own blood. The blood is processed to concentrate platelets, which contain growth factors that help guide tissue repair. PRP is not used like a simple pain-numbing shot. It is used to support the healing process in injured tissues when the patient is a suitable candidate.
A review on PRP and musculoskeletal pain reported that PRP treatment appears to reduce pain and improve function in patients with several musculoskeletal pain conditions.
For people with old accident injuries, this matters because lingering pain often comes from tissues that still need biological support, not just temporary pain control.
How PRP May Help Chronic Accident Injuries
PRP may be considered for ligament sprains, tendon injuries, muscle injuries, joint pain, whiplash-related soft tissue injuries, chronic pain after trauma, or pain that has not improved with basic care.
PRP may help by:
- Supporting tissue repair signals
- Helping calm inflammation
- Encouraging collagen activity
- Improving tendon and ligament healing response
- Supporting joint function
- Reducing reliance on pain medicine in some patients
A randomized controlled trial found that PRP and PRP combined with extracorporeal shockwave therapy were both effective treatments for chronic patellar tendinopathy in athletes, with the combination showing earlier pain improvement.
This does not mean PRP is right for every old MVA injury. A proper exam, imaging when needed, and a clear diagnosis are important before treatment.
How MFAT May Help Joint and Soft Tissue Problems
Microfragmented adipose tissue, or MFAT, uses a small amount of the patient’s own fat tissue. The tissue is processed into tiny fragments and may be injected into joints or soft tissues when appropriate. MFAT is being studied for joint pain and degenerative conditions, especially knee and hip osteoarthritis.
A 2025 study following 335 patients with knee osteoarthritis found that MFAT treatment was linked with improved pain and function scores at 3 months, with improvements sustained through 3 years. The authors also noted that the study lacked a control group, so further research is still needed.
Another study on MFAT and MFAT plus PRP in hip osteoarthritis found that both groups improved, suggesting a positive role for these approaches in some patients with joint degeneration.
MFAT may be considered when a person has:
- Chronic joint pain
- Post-traumatic joint irritation
- Cartilage-related pain
- Ligament or tendon support needs
- Arthritis changes after injury
- Pain that has not responded enough to conservative care
MFAT should be viewed as a possible part of a full recovery plan, not a stand-alone cure.
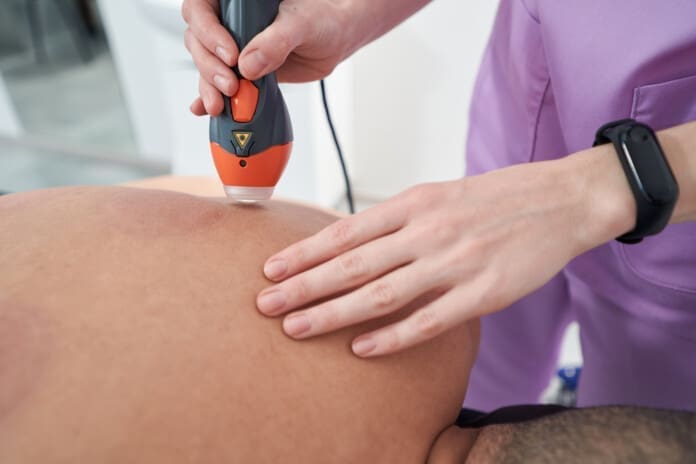
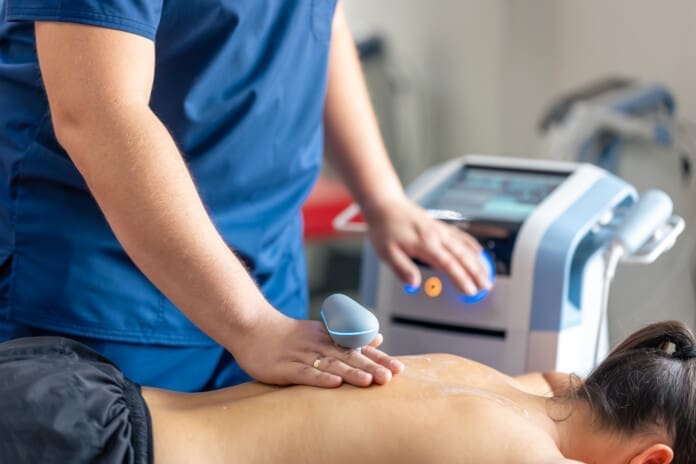
MLS Laser and Cold Laser Therapy for Soft Tissue Recovery
MLS laser and cold laser therapies use light energy to support tissue repair, reduce inflammation, and improve comfort. Laser therapy is non-invasive and is often paired with chiropractic care or physical rehab.
CARS Medical describes Class IV MLS laser therapy as a non-invasive treatment used for lingering auto injury problems such as soft tissue damage, inflammation, and nerve pain. It notes that MLS laser therapy may help reduce inflammation, decrease nerve-related pain, stimulate blood flow, and support tissue regeneration.
Cold laser therapy is also described as a method that uses light energy to stimulate healing in damaged tissues, increase blood flow, reduce inflammation, and support cell repair.
For chronic accident injuries, laser therapy may help by:
- Reducing pain sensitivity
- Supporting blood flow
- Helping soft tissue recovery
- Improving comfort before rehab exercises
- Calming inflammation around injured tissues
Laser therapy is usually not the only treatment. It often works best when combined with movement correction, strengthening, chiropractic care, and a full recovery plan.
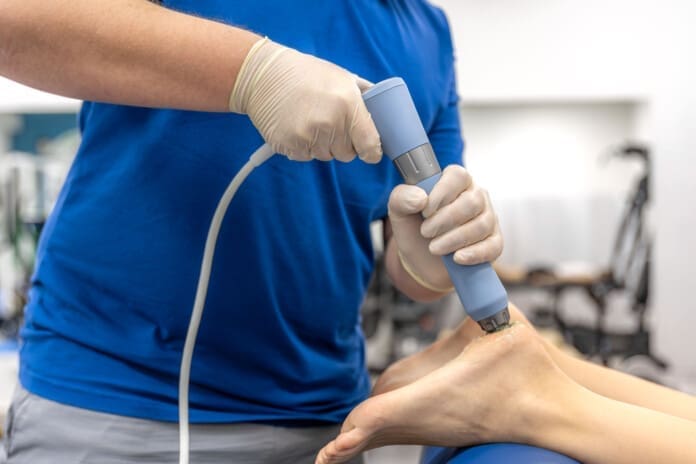
Shockwave Therapy for Chronic Soft Tissue Pain
Shockwave therapy uses acoustic energy to stimulate injured tissues. In accident recovery, it may be used for scar tissue stiffness, tendon irritation, muscle tightness, chronic inflammation, and pain that has lasted longer than expected. ChiroMed describes shockwave therapy as a non-surgical option that may support circulation, collagen activity, tissue remodeling, and pain reduction.
Shockwave therapy may be useful for:
- Chronic tendon pain
- Soft tissue tightness
- Scar tissue restrictions
- Muscle trigger points
- Poor tissue healing response
- Joint stiffness
- Chronic neck, back, shoulder, hip, knee, or ankle pain
A review on extracorporeal shockwave therapy noted that shockwaves have been used for sub-acute and chronic musculoskeletal pain problems since 2000.
Shockwave may also pair well with PRP or MFAT because it can help prepare tissues, improve blood flow, and support remodeling before or after regenerative treatment.
Why Chiropractic Care Is Still Important
Regenerative therapies may support tissue healing, but the body still needs proper motion. If a spinal joint is stuck, a hip is not moving well, or the neck remains guarded after whiplash, the injured area may stay irritated.
Chiropractic care may help by:
- Improving spinal and joint motion
- Reducing mechanical stress
- Supporting better posture
- Helping calm muscle guarding
- Improving movement patterns
- Supporting nerve function
- Helping patients return to daily activity
ChiroMed explains that chiropractic care can improve mobility, rehab can rebuild strength, shockwave therapy may support soft-tissue healing, and regenerative options may be considered when injured tissue needs additional support.
This is why a combined plan often makes sense. PRP or MFAT may support tissue repair, while chiropractic and rehab help the body move correctly as it heals.
Dr. Alexander Jimenez’s Clinical Observations
Dr. Alexander Jimenez, DC, APRN, FNP-BC, emphasizes a dual-scope approach to personal injury care. This means considering both the structural and medical aspects of an injury. In an MVA case, the provider may need to consider spinal function, joint mobility, nerve symptoms, soft-tissue injury, inflammation, imaging needs, and clear documentation.
Dr. Jimenez’s clinical site describes his practice as blending chiropractic, functional medicine, advanced diagnostics, rehabilitation, and personalized care plans. It also lists his credentials as a chiropractor and family nurse practitioner, with additional training in functional medicine and spinal trauma.
From this clinical viewpoint, chronic MVA care should not focus on a single painful spot. A patient may have neck pain, headaches, low back pain, nerve irritation, shoulder tightness, and changes in movement at the same time. Treating only the symptom may overlook the complete injury pattern.
What a Full Chronic MVA Recovery Plan May Include
A thoughtful plan may include:
- Detailed accident history
- Orthopedic and neurological testing
- Range of motion checks
- Posture and movement assessment
- Imaging referrals when needed
- Chiropractic adjustments
- Soft tissue therapy
- MLS laser therapy
- Shockwave therapy
- PRP or MFAT consultation
- Corrective exercises
- Strength and mobility training
- Follow-up progress exams
ChiroMed describes this type of accident care as a comprehensive plan that may include testing, imaging referrals, chiropractic adjustments, soft-tissue therapy, corrective exercises, shockwave therapy, regenerative medicine consultation, and progress exams.
When to Seek Emergency Care
Not every post-accident symptom should start in a chiropractic or regenerative setting. Some symptoms need urgent medical care first.
Seek emergency care for:
- Severe or worsening pain
- Chest pain
- Trouble breathing
- Sudden weakness
- Loss of bladder or bowel control
- Severe headache after trauma
- Confusion or fainting
- New numbness or major nerve symptoms
- Abdominal pain after a crash
Once serious problems are ruled out, an integrative recovery plan may help address chronic pain and function.
Conclusion: It Is Not Too Late to Support Healing
People with chronic or unresolved MVA injuries may still benefit months or years after the crash. Old soft tissue injuries, ligament damage, joint dysfunction, whiplash patterns, and spinal restrictions can continue to create pain if they are not properly addressed.
Chiropractic care helps restore motion and reduce mechanical stress. PRP and MFAT may support tissue repair in selected patients. MLS laser therapy may help calm pain and inflammation. Shockwave therapy may support circulation, tissue remodeling, and the recovery of chronic soft tissue.
The best results often come from a personalized plan that looks at the whole injury pattern. For many patients, the question is not simply, “How old is the injury?” The better question is, “What injured tissue is still driving the pain, and what can be done to help it heal and move better?”

References
AABP Integrative Pain Care and Wellness. (n.d.). 5 essential benefits of PRP for chronic pain.
CARS Medical. (n.d.). MLS laser therapy for auto injuries in Charlotte NC.
CHARM. (2023). Ankle injuries: The 2 regenerative medicine approaches to healing.
ChiroMed. (2026). Regenerative therapy for auto accident injury recovery.
Cotler, H. B., Chow, R. T., Hamblin, M. R., & Carroll, J. (2015). The use of low level laser therapy (LLLT) for musculoskeletal pain. MOJ Orthopedics & Rheumatology, 2(5).
Dallas Accident and Injury Rehab. (n.d.). Chiropractic and auto accident claims.
De la Corte-Rodríguez, H., et al. (2023). Extracorporeal shock wave therapy for the treatment of musculoskeletal pain.
Dr. Alex Jimenez. (n.d.). El Paso, TX chiropractor Dr. Alex Jimenez DC | Personal injury specialist.
Heidari, N., et al. (2021). Microfragmented adipose tissue injection (MFAT) may be a solution to the rationing of total knee replacement.
Heidari, N., et al. (2022). Comparison of the effect of MFAT and MFAT + PRP on osteoarthritis.
Jhan, S. W., Wu, K. T., Chou, W. Y., Chen, P. C., Wang, C. J., Huang, W. C., & Cheng, J. H. (2024). A comparative analysis of platelet-rich plasma alone versus combined with extracorporeal shockwave therapy in athletes with patellar tendinopathy and knee pain. Knee Surgery & Related Research, 36, 47.
Nob Hill Family Chiropractic. (2025). How cold laser therapy can speed up recovery from auto injuries.
Primary Health Clinic. (2025). Laser therapy for soft tissue recovery after injury.
PUSH as Rx. (n.d.). Healing after a car crash with regenerative therapies.
Stanciu, N., Heidari, N., Slevin, M., Ujlaki-Nagi, A.-A., Trâmbițaș, C., Arbănași, E.-M., Russu, O. M., Melinte, R. M., Azamfirei, L., & Brînzaniuc, K. (2025). Predicting long-term benefits of micro-fragmented adipose tissue therapy in knee osteoarthritis: Three-year follow-up on pain relief and mobility. Journal of Clinical Medicine, 14(13), 4549.
Thu, A. C., et al. (2022). The use of platelet-rich plasma in management of musculoskeletal pain.