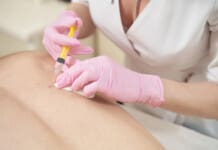
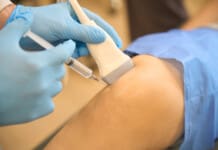
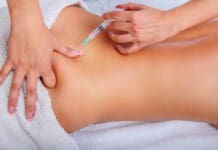
“Hamstring muscle tears are common, especially in athletes and individuals with physically demanding jobs. Is there a better chance of full recovery with surgical repair and post-op rehabilitation?”
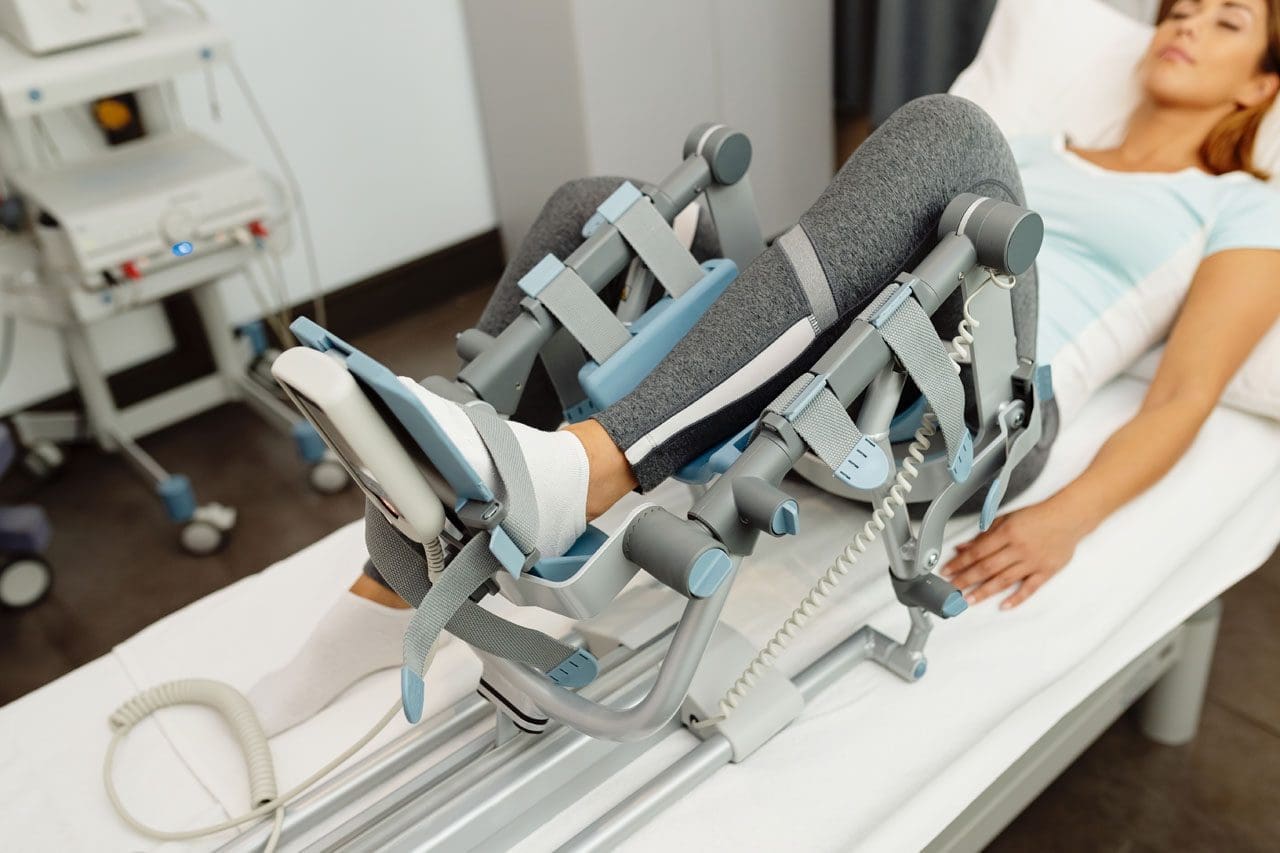
Table of Contents
Hamstring Muscle Tear
Most often, a hamstring muscle tear is a partial tear of the muscle. These types of injuries are muscle strains that occur when the muscle fibers are stretched beyond their normal limits. Complete tears of the hamstring muscle are unusual, but they do occur in both athletes and non-athletes. Determining the optimal treatment plan depends on:
- The severity of the tendon tear
- The expectations of the injured individual.
- Incomplete tears are when the hamstring muscle is stretched too far, but not completely detached.
- If the tear completes, the injury is more significant, as the ends are no longer connected. (American Academy of Orthopaedic Surgeons. 2021)
- Complete tears usually occur at the top of the muscle where the tendon tears away from the pelvis.
- A complete tear usually occurs when there is a sudden flexion of the hip and extension of the knee joint – when the muscle contracts in this position, it gets stretched beyond its limits.
- Complete tears are recognized as different injuries and may require more invasive treatments. (American Academy of Orthopaedic Surgeons. 2021)
- Individuals who sustain this type of injury describe a sharp stabbing in the back of the thigh.
- The injury may occur in athletes or middle-aged individuals. (American Academy of Orthopaedic Surgeons. 2021)
Basic hamstring strains can be treated with simple steps – rest, ice, anti-inflammatory medications, and conservative therapies.
Symptoms
Symptoms of a hamstring muscle strain can include pain, bruising, swelling, and movement difficulty. (American Academy of Orthopaedic Surgeons. 2021) Individuals who sustain this injury typically experience sudden sharp pain. Signs of a tear can include:
- Sharp pain where the buttock and thigh meet.
- Difficulty walking.
- Sitting can be difficult as the edge of a chair can place pressure directly on the injury.
- Spasms and cramping sensations in the back of the thigh.
- Weakness in the leg, specifically when bending the knee or lifting the leg behind the body.
- Numbness or burning sensations as a result of sciatic nerve irritation.
- Swelling and bruising in the back of the thigh – over time it can travel down to the back of the knee and calf and possibly into the foot.
- With a complete hamstring tear, there is usually significant swelling and bruising that develops in the back of the thigh.
Diagnosis
The symptoms can be difficult to spot in the early stages which is why X-rays of the hip or thigh are usually obtained.
In some situations, a fragment of bone can get pulled off the pelvis along with the hamstring muscle attachment. MRI testing can be performed to evaluate the attachment and can define critical features of a complete hamstring muscle tear, including: (American Academy of Orthopaedic Surgeons. 2021)
- The number of tendons involved.
- Complete versus incomplete tearing.
- The amount of retraction – the amount the tendons have pulled back.
- This will guide the development of treatment.
Treatment
The treatment of a complete tear will depend on different factors. The other variable is the patient and their expectations.
- Treatment is more aggressive in younger individuals like high-level athletes.
- Treatment is less aggressive in middle-aged individuals.
- Often a single tendon tear can be treated non-surgically.
- When one tendon is involved, it is typically not pulled very far from its normal attachment and will develop scar tissue in a positive position.
- Conversely, when three tendons have been torn, they usually pull more than a few centimeters away from the bone. These cases have better results with surgical repair. (UW Health. 2017)
- Surgeons will use patient characteristics – high-level athletes or less physically active individuals – to guide treatment recommendations.
Rehabilitation
- Rehabilitation following surgery can take 3-6 months or longer.
- The first six weeks limit weight-bearing with the use of crutches.
- Patients may be recommended to wear a brace to reduce tension on the repaired hamstring tendons.
- Strengthening does not begin until three months post-op, and even light activities are usually delayed. (UW Health. 2017)
- Because this injury can have a long recovery time, some individuals may choose nonsurgical treatment.
- Sometimes these individuals experience symptoms of discomfort from sitting and may exhibit long-term weakness of the hamstring muscle.
Full recovery from a complete hamstring muscle injury takes time. Studies have shown high-level athletes are able to resume competitive sports after the repair and rehabilitation of an acute hamstring muscle injury. (Samuel K. Chu, Monica E. Rho. 2016)
- Delaying surgical treatment may not always lead to optimal results.
- When the tendon is torn away from its normal attachment, it begins to scar around the surrounding soft tissues.
- When there is a delay of more than a few weeks following the initial injury, regaining the full length of the tendon and muscle can be challenging.
- This could delay the rehabilitation process and may limit the potential for full recovery. (Ho Yoon Kwak, et al., 2011)
With severe injuries, there is a better chance of full recovery with surgical repair but could involve a long recovery and commitment to a post-op rehabilitation plan.
Understanding Long-Lasting Injuries
References
American Academy of Orthopaedic Surgeons. (2021) Hamstring muscle injuries.
UW Health. (2017) Rehabilitation guidelines following proximal hamstring primary repair.
Chu, S. K., & Rho, M. E. (2016). Hamstring Injuries in the Athlete: Diagnosis, Treatment, and Return to Play. Current sports medicine reports, 15(3), 184–190. https://doi.org/10.1249/JSR.0000000000000264
Kwak, H. Y., Bae, S. W., Choi, Y. S., & Jang, M. S. (2011). Early surgical repair of acute complete rupture of the proximal hamstring tendons. Clinics in orthopedic surgery, 3(3), 249–253. https://doi.org/10.4055/cios.2011.3.3.249
Professional Scope of Practice *
The information herein on "Healing a Hamstring Muscle Tear: What You Need to Know" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card