Table of Contents
Introduction
The brain’s main function in the central nervous system is to make sure that the neuron signals that the brain produces are transferring throughout the entire body. These neuron signals also have a function as they help the body feel pain, sense moods, aid in organ function, and have a bidirectional connection to the brain as the body sends the signals back and forth. When there are unwanted pathogens that start to disrupt the neuron signals and start to affect the brain, it can lead to neurodegenerative disorders causing the entire body to be dysfunctional. In this 2 part series, we will be taking a look into what is Alzheimer’s and how does it affect the brain. In Part 2, we will take a look at what S.H.I.E.L.D. is and how can it help prevent Alzheimer’s disease from progressing further in the brain. By referring patients to qualified and skilled providers who specialized in neurological services. To that end, and when appropriate, we advise our patients to refer to our associated medical providers based on their examination. We find that education is the key to asking valuable questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
Can my insurance cover it? Yes, in case you are uncertain here is the link to all the insurance providers we cover. If you have any questions, please call Dr. Jimenez at 915-850-0900.
What Is Alzheimer’s Disease?
So Alzheimer’s disease is the most common form of dementia in the elderly that ranges from ages 65 and older. About 5.5 million patients in the U.S. would spend about $300B per year in medical costs while getting treated for Alzheimer’s. Research shows that since Alzheimer’s disease is a progressive neurologic disorder, it will cause brain shrinkage and cause brain cells to die over time. Some of the major risk factors that can cause Alzheimer’s disease to progress in an individual are family history, age, head injury, stroke, high blood pressure, and gender. It turns out that females actually make up about 2/3 of developing Alzheimer’s disease. Other research studies have shown that Alzheimer’s disease is classified as preclinical or presymptomatic depending on how severe the cognitive impairment is in a person. Since about 30-40% over the age of 85 have Alzheimer’s disease the current lifespan is about 80 years.
The Symptoms
Since age plays a huge role as a risk factor to aid the progression of Alzheimer’s disease the symptoms can actually range from mild to severe as research found that when there is damage to the brain, Alzheimer’s disease can start in a decade or more before memory loss and other cognitive problems start to appear as it progresses. Even though Alzheimer’s is starting in the preclinical stage, a person may look symptom-free, however, the changes are taking place in the brain and causing cognitive disorders. Some of the symptoms of Alzheimer’s disease actually depends on how severe is the progression and they include:
- Repeating questions
- Memory loss
- Shortened attention span
- Problems recognizing family and friends
- Inability to communicate
- Seizures
HCTP Therapy

Stem cells* or HCTP (human cellular tissue products) have been used in both international and nationally affiliated clinics and distribution organizations to help boost the body’s own natural healing process. As a form of regenerative cellular treatment, HCTP can help repair and regenerate damaged cells, tissues, and organs back to their original state and function properly in the body. As more and upcoming research finds more information on the beneficial properties of HCTP and its uses, individuals with chronic pain can begin their wellness journey pain-free.
How Does Alzheimer’s Disease Affect The Brain?
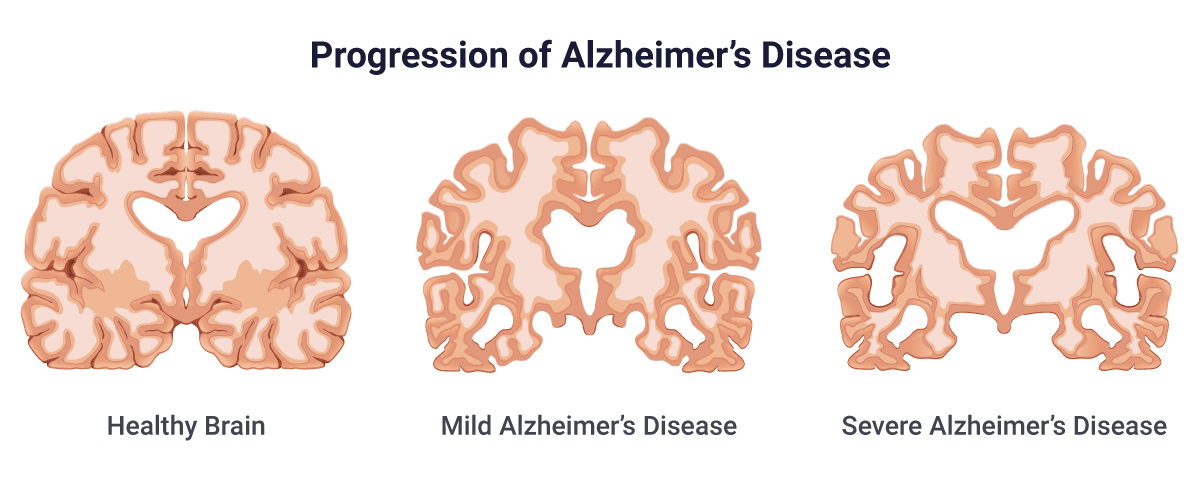
In a normal healthy brain, the brain does shrink naturally while still retaining normal cognitive functions, like memory skills and motor skills. In an Alzheimer’s brain, the brain is shrunk but the cognitive functions are disrupted causing neurodegenerative disorders. Research shows that Alzheimer’s disease causes widespread damage to the brain causing many neurons in the brain to stop functioning, lose connection and eventually die. Not only that but in an Alzheimer’s brain, it will form plaque modules known as amyloid plaque and neurofibrillary tangles in the brain.
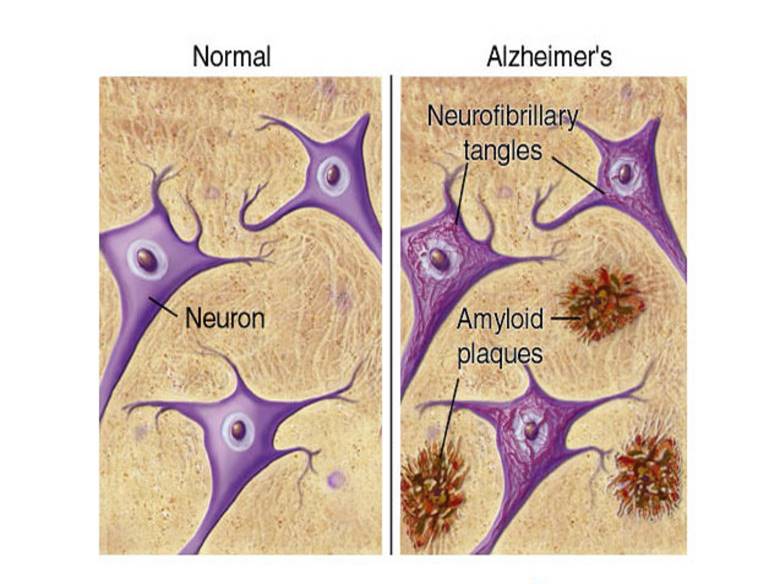
Amyloid Plaques & Neurofibrillary Tangles
Studies have found that the correlation of the behavioral symptoms of Alzheimer’s disease is due to the accumulation of amyloid plaques and neurofibrillary tangles in the brain causing damage and destruction to memory and cognitive function. Surprisingly, there are actually three tauopathies that can cause neuroinflammation to the brain and cause the start of cognitive decline. All three of these induced tauopathies require decades of tangles and neuroinflammation spreading through the brain eventually leading to dementia, which likely begins early in life, e.g. CTE and playing football as a young adult. These three tauopathies are:
- Alzheimer’s disease, which is an amyloid-induced tauopathy
- Frontotemporal Lobe Dementia (FTLD), which is a direct (often genetic-induced) tauopathy
- Chronic Traumatic Encephalopathy, which is a head trauma-induced tauopathy
Other studies have found that the neuropathological alternations in an Alzheimer’s brain can cause lesions to the brain while having an abundance of amyloid plaques and neurofibrillary tangles infesting the brain. This will cause neuronal dysfunction and degeneration to the brain causing cognitive disorders to progress further and causing the individual to have neurological problems as research shows.
Conclusion
Overall, the brain’s main function in the central nervous system is to transport neuron signals all throughout the body in a bidirectional connection as the neuron signals help keep the body functional and working properly. When neurodegenerative disorders like Alzheimer’s disease start to affect the brain, it can cause amyloid plaques and neurofibrillary tangles to infest the brain and disrupt the neuron signals in the brain. By treating Alzheimer’s disease from progressing further in the brain with whole nutritious food and exercising regularly (both mentally and physically) can help improve brain function as well as improve memory function in older adults.
References
Bloom, George S. “Amyloid-β and Tau: The Trigger and Bullet in Alzheimer Disease Pathogenesis.” JAMA Neurology, U.S. National Library of Medicine, Apr. 2014, https://pubmed.ncbi.nlm.nih.gov/24493463/.
Kumar, Anil, et al. “Alzheimer Disease.” StatPearls [Internet]., U.S. National Library of Medicine, 11 Aug. 2021, https://www.ncbi.nlm.nih.gov/books/NBK499922/.
Medical Professionals, NIA. “What Are the Signs of Alzheimer’s Disease?” National Institute on Aging, U.S. Department of Health and Human Services, 16 May 2017, https://www.nia.nih.gov/health/what-are-signs-alzheimers-disease.
Medical Professionals, NIA. “What Happens to the Brain in Alzheimer’s Disease?” National Institute on Aging, U.S. Department of Health and Human Services, 16 May 2017, https://www.nia.nih.gov/health/what-happens-brain-alzheimers-disease.
Paulson, Jennifer B, et al. “Amyloid Plaque and Neurofibrillary Tangle Pathology in a Regulatable Mouse Model of Alzheimer’s Disease.” The American Journal of Pathology, American Society for Investigative Pathology, Sept. 2008, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2527075/.
Serrano-Pozo, Alberto, et al. “Neuropathological Alterations in Alzheimer Disease.” Cold Spring Harbor Perspectives in Medicine, Cold Spring Harbor Laboratory Press, Sept. 2011, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3234452/.
Staff, Mayo Clinic. “Alzheimer’s Disease.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 19 Feb. 2022, https://www.mayoclinic.org/diseases-conditions/alzheimers-disease/symptoms-causes/syc-20350447.
Disclaimer
Professional Scope of Practice *
The information herein on "How To Detect Alzheimer's In The Brain | Part 1" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933