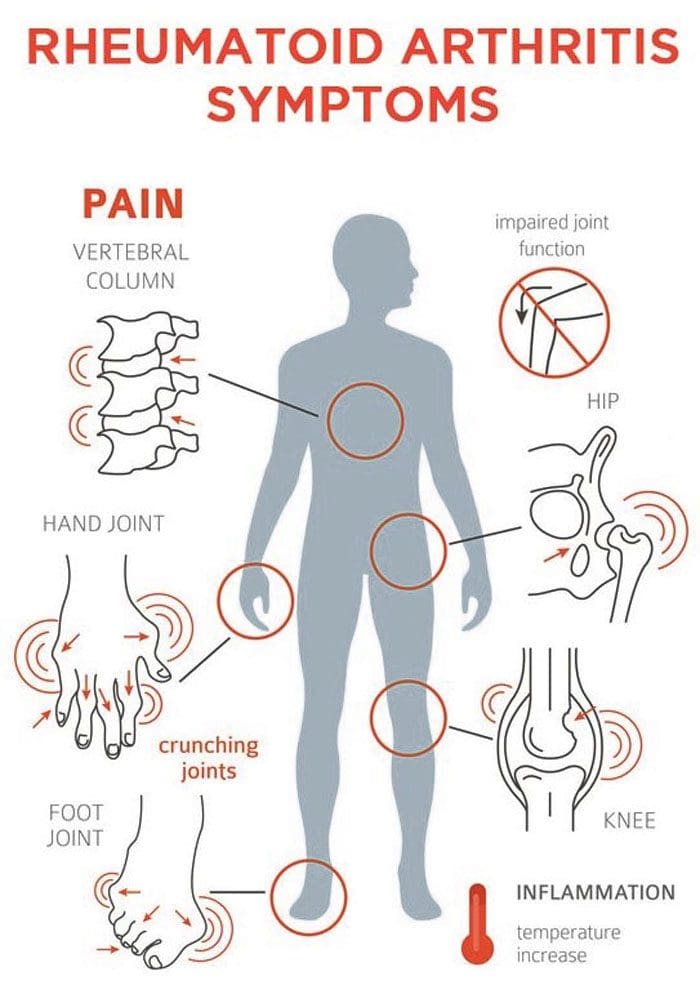
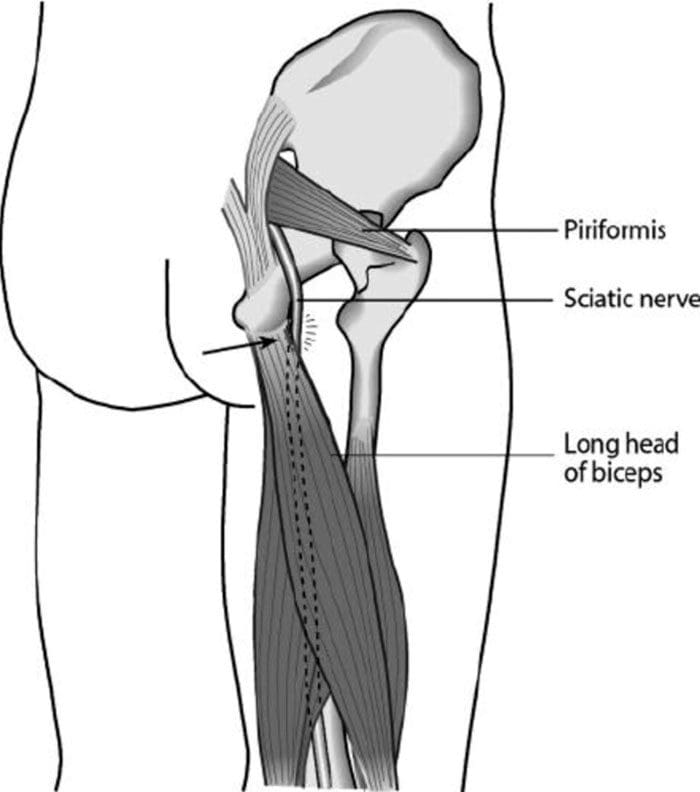
Calf pain is common in individuals that are on their feet for long periods. This could be standing, walking, as part of a job or jogging, and running. In most cases, calf soreness and/or pain result from repetitive/overuse strain/injury/tear of the calf muscles. Pain along with stiffness presents with physical activity, exercise, movement. Chiropractic treatment and Active Release can help alleviate and eliminate calf pain.
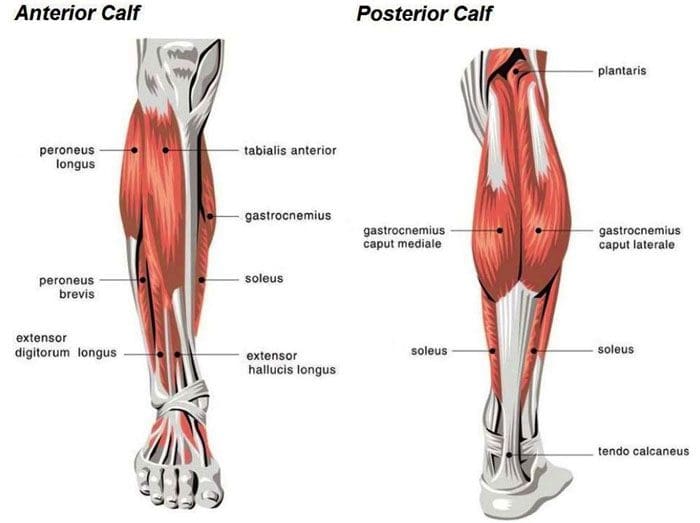
Table of Contents
Calf Muscles
The calf muscle is in the back of the lower leg, behind the shin bone, and consists of three muscles. The calf muscle supports the body when standing and enables movement of the foot and lower leg. The calf muscles support the body when:
- Walking
- Running
- Jumping
- Standing on the toes.
- Flexing the foot – lifting the toes toward the knee.
- It helps push the body forward and allows jumping, ankle rotation, and flexing of the foot.
Causes, Conditions, and Disorders
The overuse of the calf muscles usually causes calf soreness, discomfort, and pain. Over time, tiny tears develop in the muscles of the lower legs and calves. Repeated use can lead to more severe injury or condition without proper treatment. Conditions include:
Strain
The most common injury is a strain. Strains happen when the muscle fibers are overused and get stretched too far and/or tear. However, the fibers may not tear in that instance, and so the tear could occur at a later time while doing a basic movement like slightly bending or kneeling to tie a shoe. This is when individuals wonder how a tear happened with a simple action. But the tear was already present, just not fully torn.
Cramps
Muscle cramps and muscle spasms in the calves can be excruciating limiting mobility. Calf cramps can happen during the day or at night. They can result from several factors that include:
- Health conditions
- Dehydration
- Medications
- Pregnancy
Tennis leg
Healthcare providers call this strain tennis leg because it happens when the leg extends and the foot flexes. Tennis players are in this position when they serve and push themselves off into motion; however, it can happen in any sport, job, chore that involves the same movement. This type of muscle strain injury affects the gastrocnemius muscle.
Compartment syndrome
Compartment syndrome happens when pressure builds up inside a muscle. The pressure significantly reduces the flow of blood and oxygen. It can result from trauma like a fracture or strenuous exercise/activity.
Symptoms
Calf muscle issues can cause calf muscle:
- Pain
- Tightness
- Stiffness
- Pain may be sharp or dull
- Pain can start as mild pain and progressively worsen.
- Limited mobility
- Limited range of motion
- Muscle weakness
- A bump, bulge, or lump in the back of the lower leg.
- Tenderness
- Bruising
- General leg cramps are common and are more likely to happen as the body ages.
- Healthcare professionals estimate around 75% of individuals over 50 have had leg cramps and pain.
Calf Health
To prevent and avoid problems with the calf muscles, individuals are recommended to:
Maintain a healthy diet and weight
- Individuals that are overweight are more likely to pull or strain a muscle.
- Excess pounds add pressure on the legs placing individuals at a higher risk of an injury.
- If obese or overweight, talk to a healthcare professional about healthy weight.
Stay hydrated
- Drink the proper amount of water and other fluids
- This decreases the chance of causing a cramp.
Stretch and warm-up
- Warmed-up calf muscles are less likely to stretch too far or tear.
- Before engaging in physical activity at work or school, do a few warm-up stretches to increase flexibility.
- When exercising, gradually increase the intensity.
Stay aware of medications.
- Certain medications can cause leg cramps and/or dehydration.
- Talk to a doctor about taking another medication that does not cause these side effects.
Body Composition
Nutrients of Protein
Protein is necessary for all of the body’s physiological functions. Protein and amino acids are the building blocks of the muscle tissue in the body. The body’s muscles are a house, protein is the bricks, and the amino acids that form protein are the building blocks of muscle. The body manufactures various amino acids, but nine are essential amino acids – EAA because they are not made in the body. Individuals have to consume EAAs from food sources like:
- Meat
- Beans
- Nuts
- Soy
A diet that consists of mixed amino acids can help maximize muscle protein synthesis. Protein is essential in building muscle because amino acids help repair and maintain muscle tissue. After a strenuous activity or a workout, protein helps the body repair muscles that are slightly torn. To build a healthy body, the body needs to have the right amount of protein. Protein is an essential component of:
- Muscle development
- Bone density
- Muscle mass
- Lean tissue
References
Binstead JT, Munjal A, Varacallo M. Anatomy, Bony Pelvis, and Lower Limb, Calf. [Updated 2020 Aug 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan-. . Accessed 6/4/2021.https://www.ncbi.nlm.nih.gov/books/NBK459362/ (https://www.ncbi.nlm.nih.gov/books/NBK459362/)
Bright JM, Fields KB, Draper R. Ultrasound Diagnosis of Calf Injuries. Sports Health. 2017 Jul-Aug;9(4):352-355. . Accessed
6/4/2021.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5496702/ (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5496702/)
Young G. Leg cramps. BMJ Clinical Evidence. 2015 May 13;2015:1113. . Accessed 6/4/2021.https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4429847/ (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4429847/)