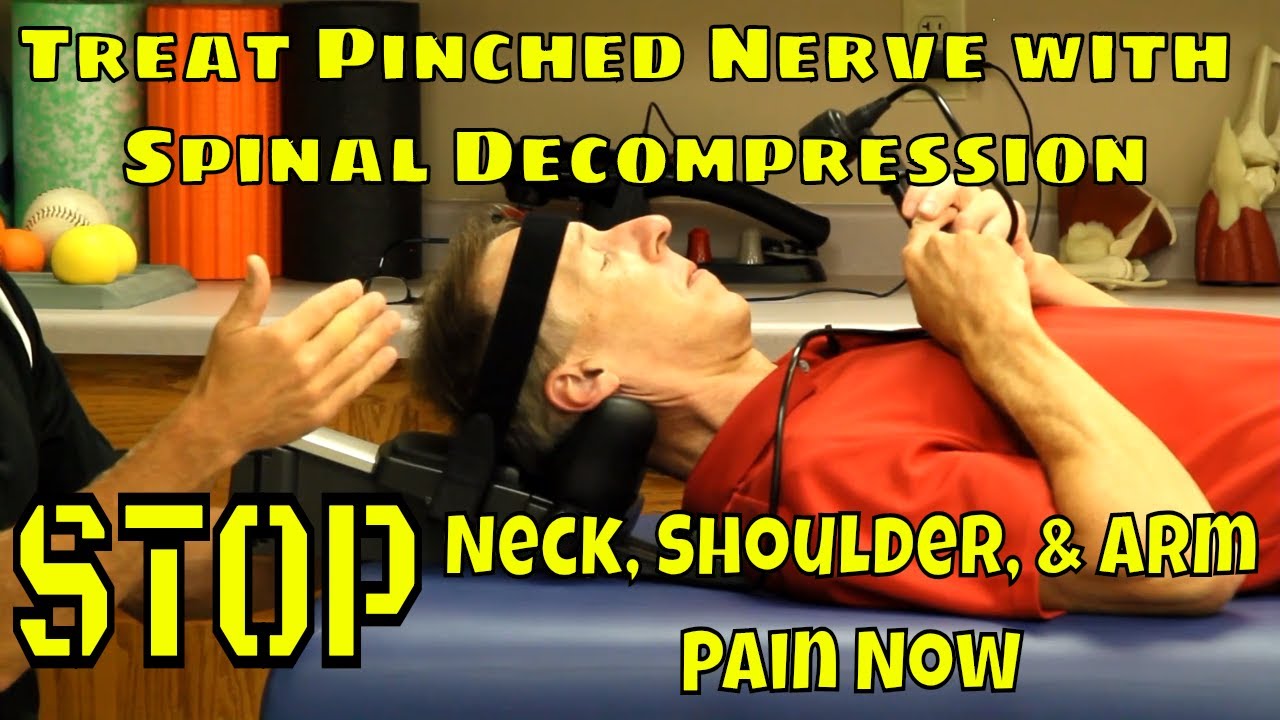
Introduction
The body is a functional machine that constantly moves and can twist, bend, turn, and do everyday movements without feeling pain. This is due to the spine, as its primary function is to keep the body upright and perform properly. The spine and the ligaments, the spinal cord, nerve roots, and spinal discs are all part of the central nervous system. When the body becomes injured due to accidents, many complications like spinal injuries, low back pain, herniated discs, or degenerative issues will affect the body, back, and spine. Fortunately, when problems like this happen to the spine, non-surgical therapies can help alleviate the pain and help restore the spine to its original functioning state. Today’s article dives in on the function of the central nervous system and how the spinal cord plays its role, and how spinal decompression therapy can affect the central nervous system. By referring patients to qualified and skilled providers specializing in spinal decompression therapy. To that end, and when appropriate, we advise our patients to refer to our associated medical providers based on their examination. We find that education is the key to asking valuable questions to our providers. Dr. Alex Jimenez DC provides this information as an educational service only. Disclaimer
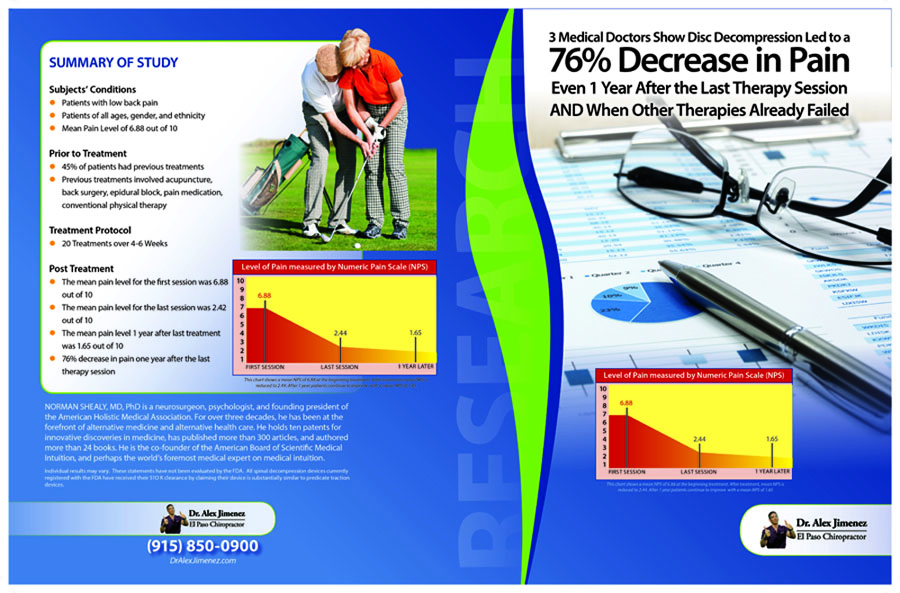
Can my insurance cover it? Yes, it may. If you are uncertain, here is the link to all the insurance providers we cover. If you have any questions, please call Dr. Jimenez at 915-850-0900.
How Does The Central Nervous System Function?
Research studies have mentioned that the central nervous system controls everything in the body. Since the body can function with everyday movements and get to different places through any means, it is due to the central nervous system. The central nervous system consists of the brain and the spinal cord, and its primary function is to receive, process, and respond to all sensory information that the body is going through. The brain is in the central nervous system that sends out neuron signals that travel down through the spinal cord and to every nerve root in the body. These nerve roots not only send out sensory information back to the brain but also protect the spine. Other research studies have shown that the central nervous system’s network has motor components that respond to its surroundings. The body’s central nervous system can also respond to environmental and injury stimuli.
The Spinal Cord
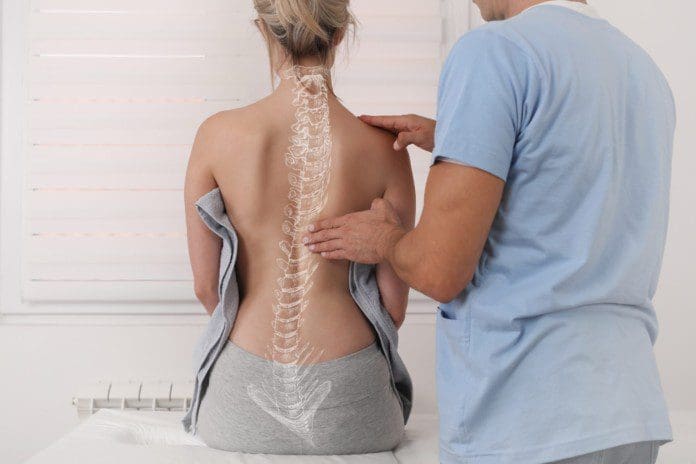
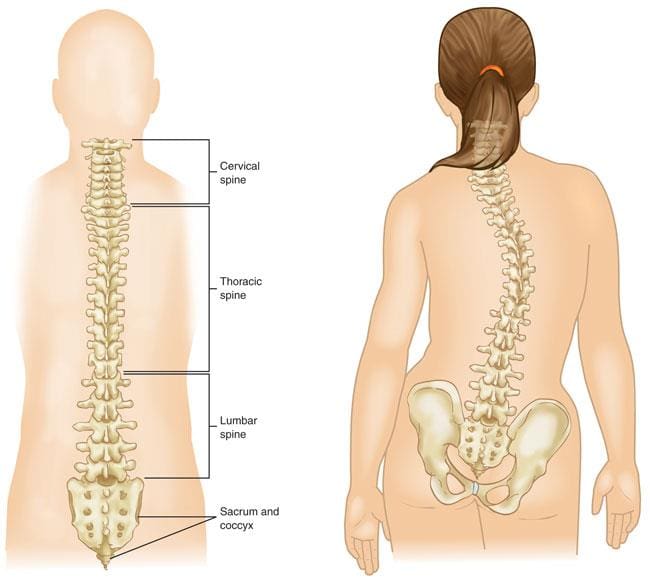
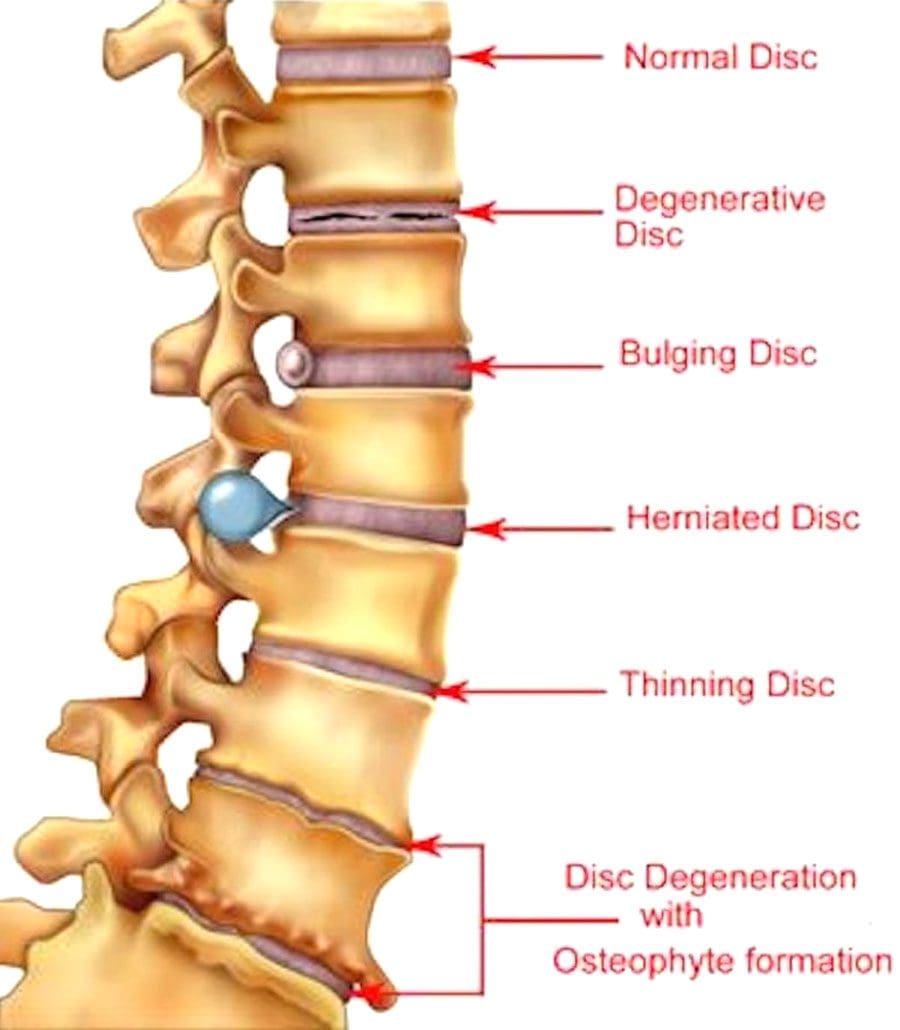
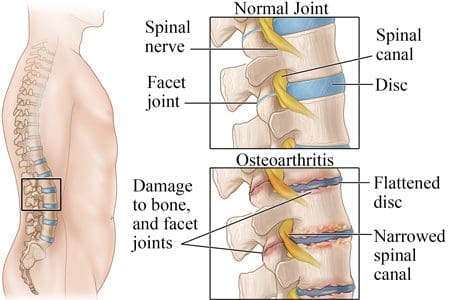
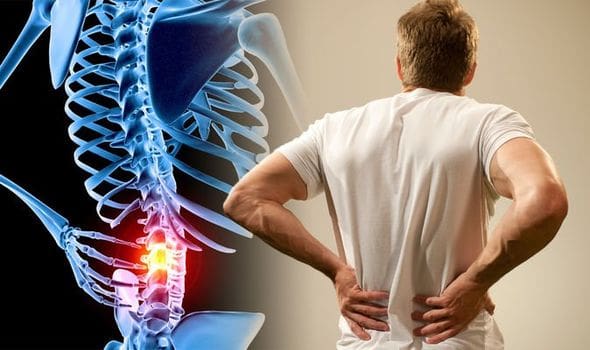
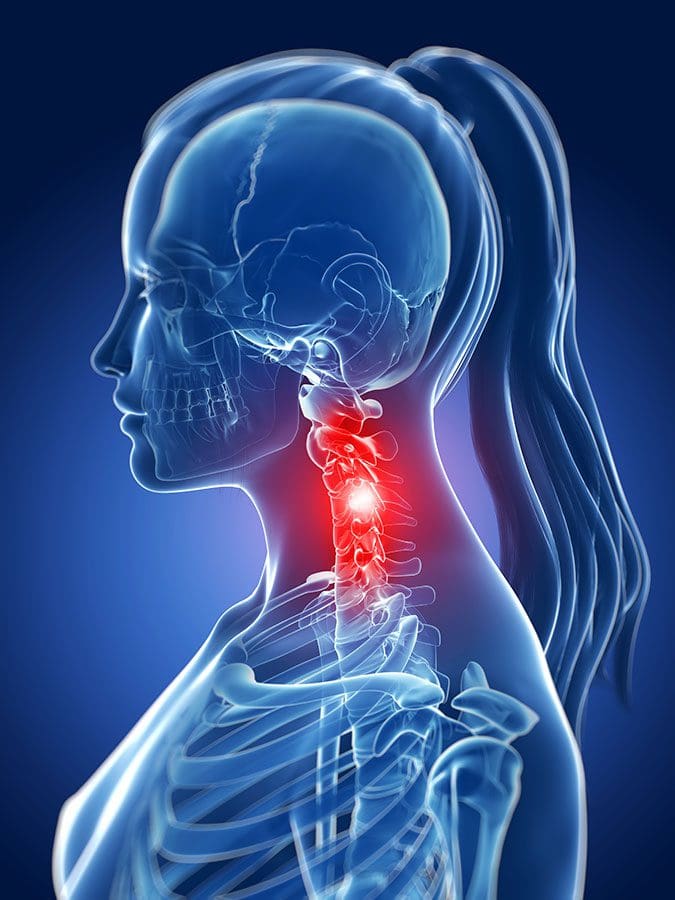
As part of the central nervous system, the spinal cord’s primary function is to send out information from the brain through the nerves. Research studies have shown that the spinal cord is protected by the spine, an S-shaped curve that helps keep the body upright. What the spinal cord does is that it is within the spinal canal, and the spinal nerves that are attached to the spinal cord are spread out throughout the spine. Since the spinal cord helps the brain by sending out information to the body, research shows that when many disorders and injuries affect the spine, it can cause a range of symptoms that can affect the many parts of the body. These disorders and injuries can be mild, like low back pain, while others can be severe, like spinal stenosis or sciatica. These symptoms can cause immense pain to the body and the spine, but there are different ways to alleviate the pain so it won’t affect the spinal cord or the spine anymore. When many factors cause harm to the spinal cord, it can cause severe damage to the spine if it is not treated right away.
How Spinal Decompression Helps The Spine-Video

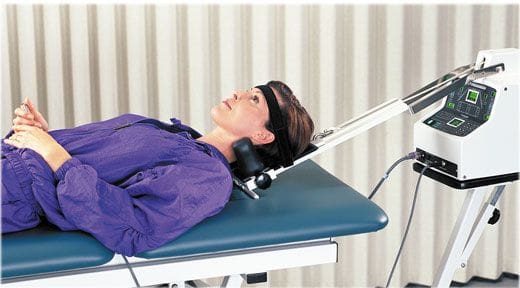
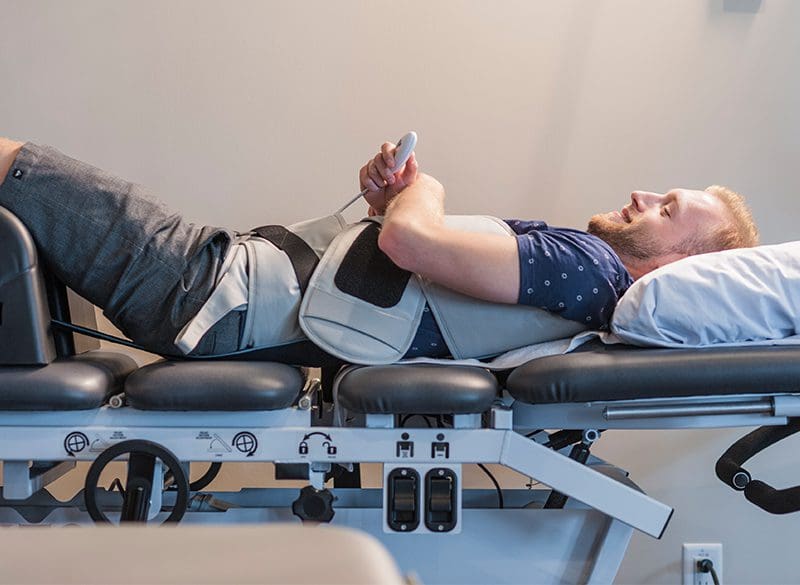
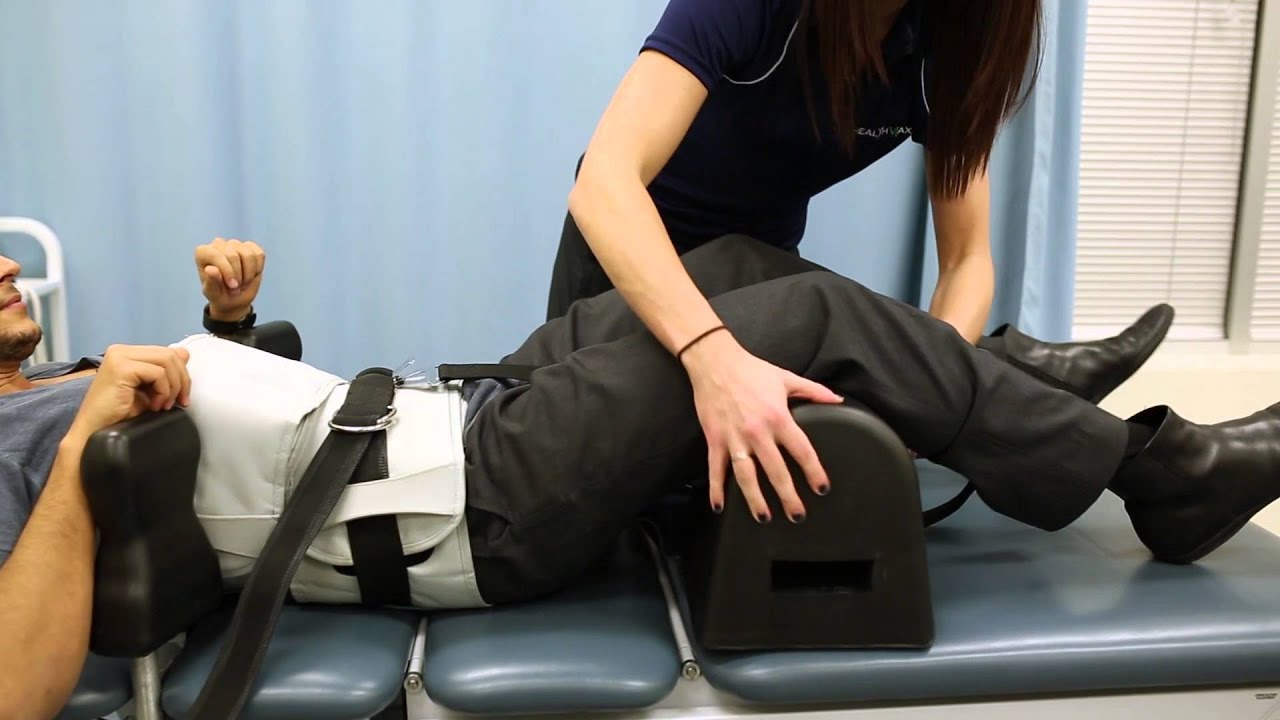
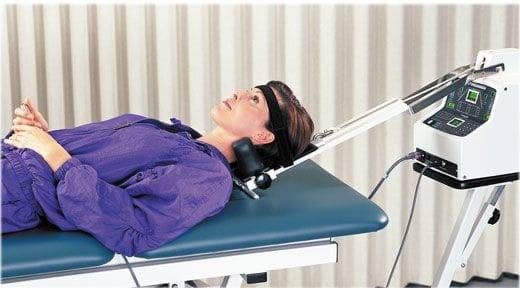
Is your spine feeling a bit stiff from twisting and turning excessively? How about feeling tenderness in certain areas located on the back? How about sharp shooting pain that radiates down to your leg? If you are experiencing any of these painful symptoms, why not incorporate spinal decompression therapy into your wellness journey. The video above explains how spinal decompression therapy can help alleviate compressed spinal discs and release the pressure off the nerve roots along the spine. Since the central nervous system sends out information throughout the entire body, spinal decompression help alleviate the painful signals coursing throughout the body through traction and helps restore the spine to its original function. Suppose you want to learn more about spinal decompression therapy and how it can benefit you? In that case, this link will explain what spinal decompression does for the spine and the central nervous system.
How Spinal Decompression Affects The Central Nervous System
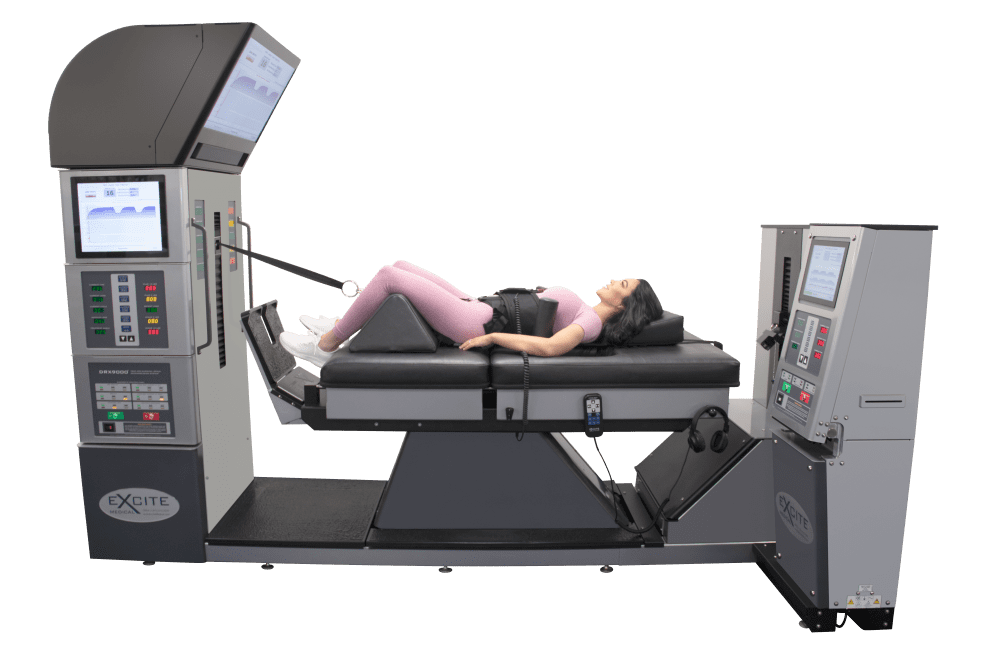
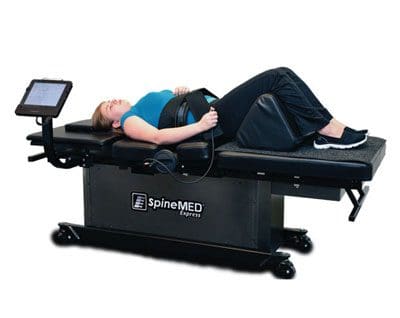
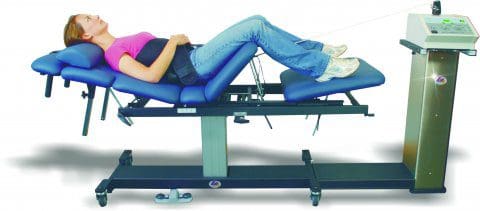
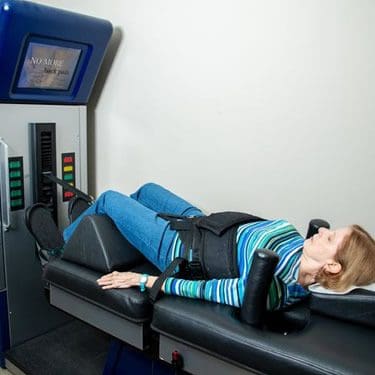
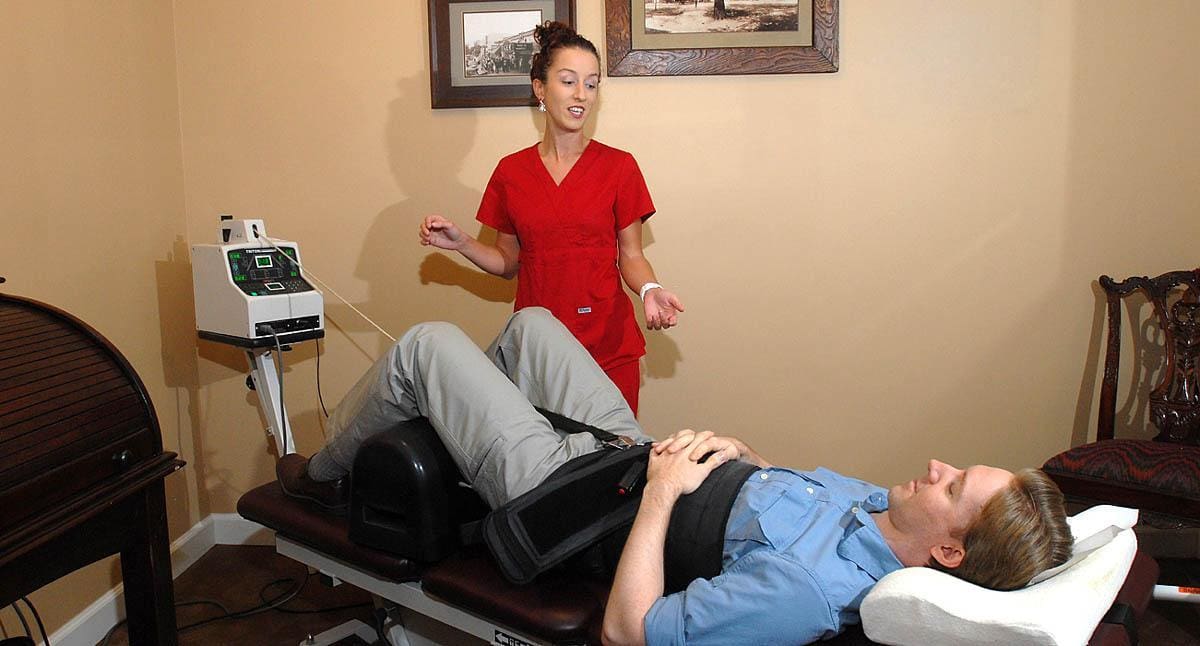
There are many ways to ensure that the spinal cord does not get injured severely and that the central nervous system is sending out the signals correctly. One of the ways is through spinal decompression therapy. Research studies have shown that spinal decompression therapy uses motorized non-surgical traction to help with low back pain and reduce the pressure on compressed spinal discs by increasing their disc height. When the spine starts to become compressed, it can affect the intervertebral discs causing them to be herniated and pressed on the spinal nerve root. This causes the brain in the central nervous system to send out signals to where the pain is located on the nerve root and causes many unwanted issues to affect the body. However, as research studies found, when utilizing spinal decompression, supine will help stretch the spine gently and help improve the lumbar range of motion in the spine. This will bring back a person’s quality of life and help them become pain-free.
Conclusion
In the body, the central nervous system is the control center to ensure that the body is functioning correctly while being home to the brain and spinal cord. The spine protects the spinal cord while its primary job is to send out signals from the brain throughout the spinal nerves that branched out of the spine, ensuring that the information helps with the body’s motor functions. When the body becomes injured, it can stop the signals from reaching their necessary places and cause immense pain all over the body. Spinal decompression therapy can help alleviate the pain by using traction on the spine and gently stretching the compressed spinal discs. This will take the compressed disc off the nerve roots and rewire the signals to stop causing pain to the body. Afterward, many people suffering from a compressed spinal disc will feel instant relief and continue in their daily lives.
References
Amjad, Fareeha, et al. “Effects of Non-Surgical Decompression Therapy in Addition to Routine Physical Therapy on Pain, Range of Motion, Endurance, Functional Disability and Quality of Life versus Routine Physical Therapy Alone in Patients with Lumbar Radiculopathy; a Randomized Controlled Trial.” BMC Musculoskeletal Disorders, BioMed Central, 16 Mar. 2022, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8924735/.
Apfel;Cakmakkaya OS;Martin W;Richmond C;Macario A;George E;Schaefer M;Pergolizzi JV;, Christian C. “Restoration of Disk Height through Non-Surgical Spinal Decompression Is Associated with Decreased Discogenic Low Back Pain: A Retrospective Cohort Study.” BMC Musculoskeletal Disorders, U.S. National Library of Medicine, 8 July 2010, https://pubmed.ncbi.nlm.nih.gov/20615252/.
DeSai, Charisma, and Amit Agarwal. “Neuroanatomy, Spine.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 11 Aug. 2021, https://www.ncbi.nlm.nih.gov/books/NBK526133/.
Ludwig, Parker E, et al. “Neuroanatomy, Central Nervous System (CNS) – Statpearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 14 Oct. 2021, https://www.ncbi.nlm.nih.gov/books/NBK442010/.
Medical Professional, Cleveland Clinic. “Spinal Cord: Function, Anatomy and Structure.” Cleveland Clinic, 7 Oct. 2021, https://my.clevelandclinic.org/health/body/21946-spinal-cord.
Thau, Lauren, et al. “Anatomy, Central Nervous System – Statpearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 14 Oct. 2021, https://www.ncbi.nlm.nih.gov/books/NBK542179/.