Table of Contents
Introduction
Everyone worldwide knows that feet are important. The feet allow many individuals to run, walk, or jog for long periods without feeling pain for a moderate amount of time. To that point, the various muscles and tendons surrounding the foot provide full body flexion, extension, and stability. Even though it is very easy to get in the recommended amount of steps into being healthy, around 75% of individuals will have foot pain that can impact their ability to walk. One of the most common foot pains is plantar fasciitis, which can become a painful foot condition if it is not treated as soon as possible. Today’s article looks at plantar fasciitis, its symptoms, how trigger points correlate, and treatments for it. We refer patients to certified providers incorporating techniques and therapies for individuals dealing with plantar fasciitis. By locating where the trigger points are coming from, many pain specialists can develop a treatment plan to reduce the effects that plantar fasciitis is causing on the feet. We encourage and appreciate each patient by referring them to associated medical providers based on their diagnosis when it is appropriate. We understand that education is a terrific way when asking our providers intricated questions at the patient’s request and understanding. Dr. Jimenez, D.C., only utilizes this information as an educational service. Disclaimer
What Is Plantar Fasciitis?
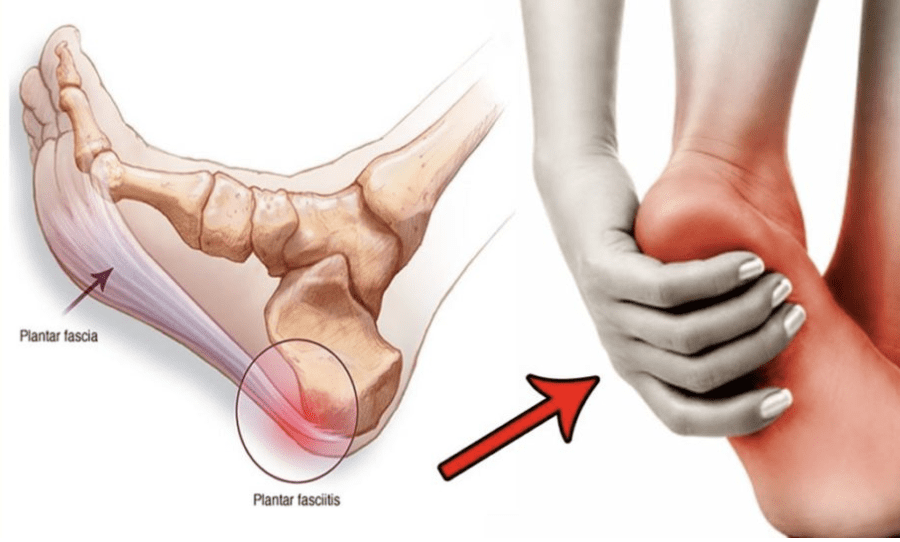
Have you been dealing with constant heel pain? Do you feel pain shooting up your leg when you step or walk? Or do you feel a stabbing ache in your heel? Many of these pain issue people are dealing with correlate with plantar fasciitis. Studies reveal that plantar fasciitis results from degenerative irritation on the plantar fascia and its ligaments. This causes the muscle ligaments to become inflamed, swollen, and weak, which then causes the bottom of the foot or heel to hurt when a person is walking or standing. To that point, when there is a repetitive strain on the feet, it causes microtears in the plantar fascia. The plantar fascia in the foot plays an important role as it comprises three segments that support the medial arch and shock absorption when stepping down. As one of the most common causes of heel pain, the residual pain from plantar fasciitis tends to be a sharp, stabbing sensation. Plantar fasciitis is more prominent in middle-aged people. Still, anyone at any age can develop plantar fasciitis, especially if they have labor jobs requiring them to be constantly on their feet.
Symptoms Of Plantar Fasciitis
Since around 2 million Americans could potentially develop plantar fasciitis, it is important to know that when a person has been on their feet constantly, there will be inflammation along the tissues in the feet. Many individuals with a busy lifestyle that requires them to be on their feet frequently would often ignore the pain or discomfort. Some of the symptoms that plantar fasciitis causes include the following:
- Pain on the bottom of the heel
- Pain in the arch
- Pain that is usually worse when waking up
- Pain that increases over months
- Swelling on the bottom of the heel
However, when the pain becomes overbearing, many people would often think they have sore feet or low back pain from being overly tired from work, under constant stress, or over-exerting their bodies. When this happens, many would think the pain would go away in a few days after resting for a short period.
Trigger Points Associated With Plantar Fasciitis
Now many individuals would often think that plantar fasciitis just only affects the heels, however, it can affect any part of the structure of the foot since all the surrounding muscle tissues are at risk of inflammation. When people start to ignore the pain and discomfort that plantar fasciitis is causing on the feet, it can overlap and develop trigger points in other areas of the body:
- Ankles
- Knees
- Hips
- Lower back
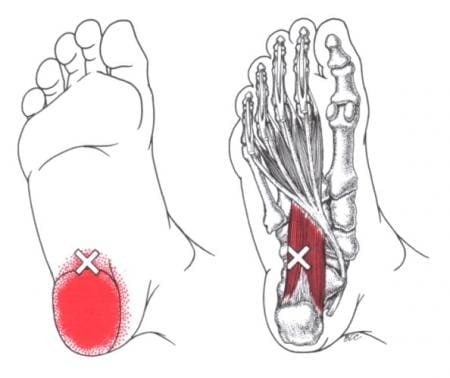
Studies reveal that trigger points or myofascial pain syndrome are hard, discrete, small nodules that are along the taut musculoskeletal band that causes numerous issues like inflammation, hypersensitivity, and pain to the affected muscle groups in the body. According to “Myofascial Pain and Dysfunction” written by Dr. Travell, M.D., it mentions that when the deep intrinsic muscles that work with the plantar fascia are affected by trigger points, would cause symptoms of numbness and the feeling of swelling in the foot. This causes many people to have limited mobility and have intense pain when walking, which can negatively impact their lifestyle.
An Overview Of Plantar Fasciitis- Video
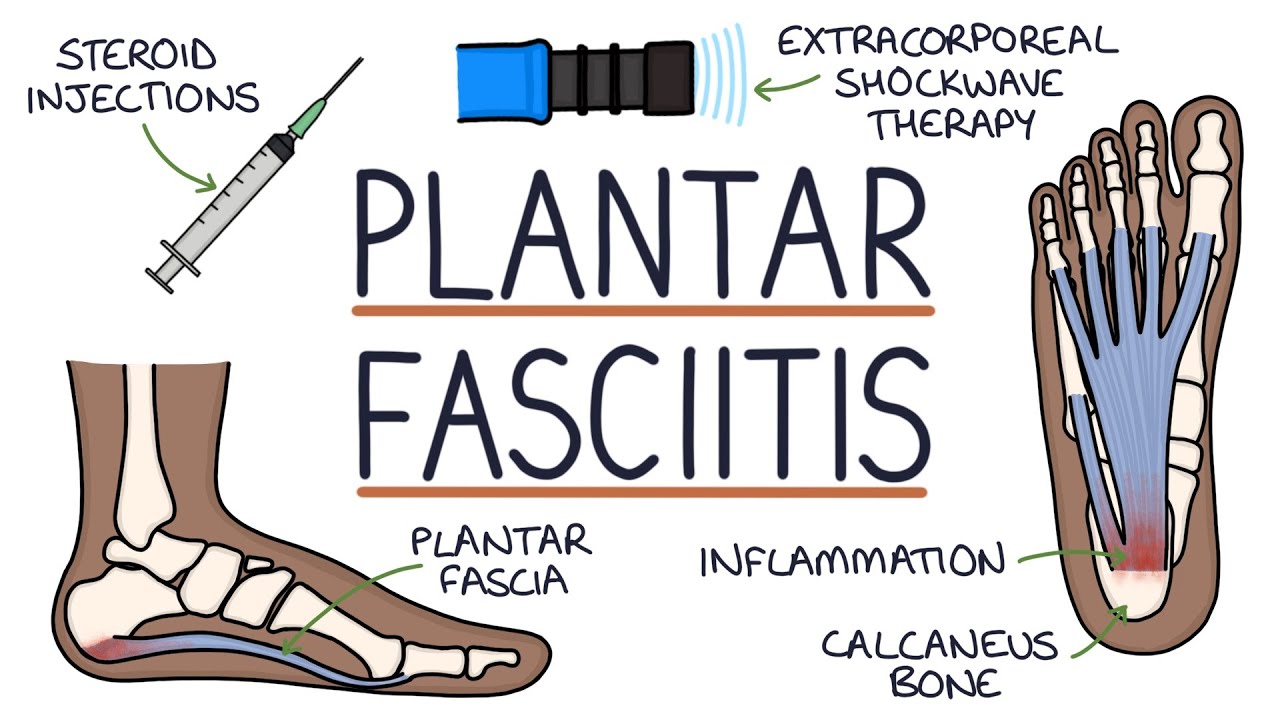
Have you been dealing with aching feet? Do you feel a sharp, radiating pain in your feet? Or do you have difficulty walking? Many often think they are dealing with sore feet or other issues causing them pain. Around 75% of Americans often have foot pain affecting their ability to walk, and one of them is plantar fasciitis. The video above explains plantar fasciitis and how it can affect the feet. When the plantar fascia tendons become overused, it causes micro-tears in the muscle ligaments. When added compressive force starts to push against the heel boner, it can lead to a pathological state whereby the plantar fascia degenerates and creates dysfunction and pain. When this happens, it can lead to other conditions like trigger point pain along the muscle fibers in the foot. The pain and tenderness caused by trigger points in the plantar muscles may mask as plantar fasciitis. To that point, when plantar fasciitis becomes an issue and causes the individual to be in immense pain, it can become problematic. As luck would have it, treatments are available to reduce the pain from plantar fasciitis.
Treatments For Plantar Fasciitis
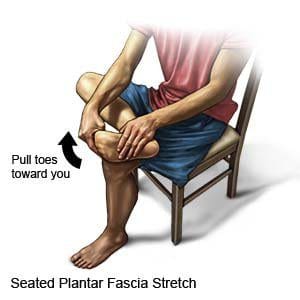
When treating plantar fasciitis, many available treatments can reduce the inflammatory effects in the heel and prevent trigger points from coming back. One of the available treatments is chiropractic care. Chiropractic care is an alternative treatment option to prevent, diagnose, and treat numerous injuries and conditions associated with the spine, primarily subluxations or spinal misalignments. Chiropractic focuses on restoring and maintaining the overall health and wellness of the musculoskeletal and nervous systems through spinal manipulation and adjustments. A chiropractor can carefully re-align the spine, improving a patient’s strength, mobility, and flexibility. Regarding plantar fasciitis, chiropractic care can work with other treatments, including physical therapy, massage, and even injections, to manage the pain and treat the condition. Even though plantar fasciitis takes several months to heal, chiropractic care can involve a precise technique that involves adjustments to the feet, ankles, and spinal alignment. This provides several benefits, which include the following:
- Reduces Stress in the Plantar Fascia
- Promotes Healing
- Provides Effective Pain Management
- Reduces the Risk of Further Injury
Conclusion
As many individuals worldwide are on their feet constantly, foot pain can hinder one’s ability to move. One of the most common foot pain is plantar fasciitis which can correlate with trigger points along the various muscles of the foot. Plantar fasciitis results from degenerative irritation on the plantar fascia and its ligaments, which causes sharp, stabbing pain on the heel. When this happens, it can cause the heel to be inflamed, swollen, and weak. To that point, it causes instability and pain when walking. However, plantar fasciitis can be treated when it is caught early through various treatments like chiropractic care. Chiropractic care can reduce the stress in the plantar fascia and help reduce the risk of further injuries. Combined with other therapies, many people can function normally and regain their walking ability without pain.
References
Buchanan, Benjamin K, and Donald Kushner. “Plantar Fasciitis – StatPearls – NCBI Bookshelf.” In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing, 30 May 2022, https://www.ncbi.nlm.nih.gov/books/NBK431073/.
Petrofsky, Jerrold, et al. “Local Heating of Trigger Points Reduces Neck and Plantar Fascia Pain.” Journal of Back and Musculoskeletal Rehabilitation, U.S. National Library of Medicine, 2020, https://pubmed.ncbi.nlm.nih.gov/31594202/.
Shah, Jay P, et al. “Myofascial Trigger Points Then and Now: A Historical and Scientific Perspective.” PM & R : the Journal of Injury, Function, and Rehabilitation, U.S. National Library of Medicine, July 2015, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4508225/.
Travell, J. G., et al. Myofascial Pain and Dysfunction: The Trigger Point Manual: Vol. 2:the Lower Extremities. Williams & Wilkins, 1999.
Disclaimer
Professional Scope of Practice *
The information herein on "Plantar Fasciitis & Trigger Points On The Feet" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card