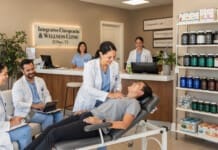
When stress is placed on the shins with physical activity from walking, running, or exercise, the connective tissues attaching the leg muscles to the tibia can become inflamed, causing medial tibial stress syndrome, more commonly known as shin splints. This inflammation is caused by tiny tears in the muscles and tendons of the shin. Chronic shin pain could be related to foot arch problems, underlying issues with the muscles, or shoes that don’t support the feet properly. Although it usually goes away within a few days, it’s important to monitor to ensure that it does not progress into a stress fracture. A chiropractor can offer treatments to relieve the pain and help prevent shin splints from recurring.
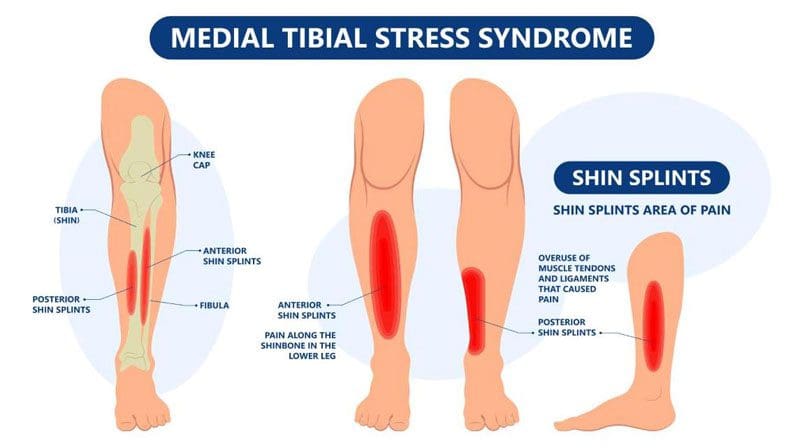
Table of Contents
Medial Tibial Stress Syndrome
Medial tibial stress syndrome can impact anyone. It can come from walking far distances or in awkward positions like going downstairs with small steps, jumping rope, and playing with the kids on the playground can all cause burning, tightness, and pain in the shins. Shin splints affect individuals differently. For some, the pain recedes when the triggering activity is stopped. For others, the pain can become a chronic condition that results in continuous pain, even when at rest.
The Shin
- The shin is a part of the tibia bone in the lower leg.
- This bone absorbs the shocks when moving through daily activities.
- The muscles that run along the shin support the foot’s arch and raise the toes during movement.
- Medial tibial stress syndrome is caused by excessive force on the shinbone and the tissue around it, which causes the muscles to swell and increases pressure around the bone.
- If left untreated, small tears in the muscle and the bone can form, leading to chronic pain and stress fractures.
Medial tibial stress syndrome is more likely to happen from:
- Not stretching before physical activity or exercise.
- Constantly walking or running on hard surfaces.
- Wearing the wrong shoes that don’t provide enough cushioning or arch support.
- Over-exertion on the body with activity and movement.
- The body is not given the proper amount of time to recover.
- Athletes often experience shin splints when they’ve intensified their training routine or changed it up.
Symptoms
- Pain during exercise or activity.
- Pain in the front of the lower leg.
- Soreness in the lower leg.
- Swelling in the lower leg.
- Shin is hot to the touch.
Treatment
Whenever pain is being experienced, some muscles will either get tight or weak in response. By identifying the weak and/or tight muscles, a chiropractor can prescribe stretches and exercises that will help alleviate the pain and prevent it. One of the main principles of chiropractic is to treat the body as an interconnected system. A chiropractor may work on an unrelated part of the body to treat the symptomatic area. For example, they may work to align the spine and pelvis to lessen the impact on the lower legs.
Part of a treatment plan may include:
Soft Tissue Mobilization
- A handheld instrument loosens tight tissues during soft tissue mobilization therapy and breaks scar tissue around the tibia.
- Massaging tight muscles in the leg keeps them loose and alleviates the pain.
- Percussion massage can be added to reduce muscle knots, improve blood flow, and loosen up scar tissue.
- The treatment relieves pain and can help avoid shin splints when returning to normal activities.
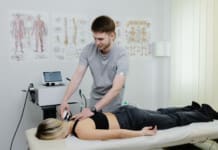
Ultrasound and Low Laser Therapy
- Ultrasound and low laser therapy use heat to warm the deep tissues in the lower leg gently.
- The treatment eases pain, reduces inflammation, swelling, and increases blood flow.
Kinesio Taping
- Applying flexible Kinesio tape to the foot and lower leg can reduce stress on the shins.
- The chiropractor or physical therapist will show how to apply the tape correctly.
Foot Orthotics
- Individuals may be more likely to develop shin splints if they have high or low arches or their feet tend to roll inward or outward when walking.
- Prescription foot orthotics can be made to keep the feet properly balanced and supported.
Stretching Exercises
- Shin splints could be related to tight muscles in the back of the calf and weak muscles in the front of the lower leg.
- A chiropractor or physical therapist will show stretching and strengthening exercises to maintain muscle balance.
Body Composition
Retaining Water Due To Salt Intake
Salt/sodium is everywhere and hard to avoid.
It might not be a surprise that a single patty cheeseburger contains over 500 mg of sodium – almost a quarter of the daily recommended level, but it is a surprise to know that the ranch dressing on a salad contains as much as 270 mg or a tablespoon of soy sauce on a healthy, vegetable-only stir-fry has 879 mg of sodium. The Mayo Clinic estimates that the average individual consumes about 3,400 mg of sodium a day: close to double what is recommended. Sodium is linked with water retention, and it is the kidneys’ job to expel unneeded sodium out of the body. Until the kidneys activate, an individual will temporarily be retaining extra water. If daily water and sodium intake habits change daily, this can contribute to water retention, causing fluctuations in daily weight. So, if an individual was on a diet but flooded the body with more salt than usual, expect to see a temporary increase in weight.
References
Bates, P. “Shin splints–a literature review.” British journal of sports medicine vol. 19,3 (1985): 132-7. doi:10.1136/bjsm.19.3.132
Chiropractic Economics: The Science Behind Percussion Massage.
Gross, ML et al. “Effectiveness of orthotic shoe inserts in the long-distance runner.” The American journal of sports medicine vol. 19,4 (1991): 409-12. doi:10.1177/036354659101900416
Heer, Martina et al. “Increasing sodium intake from a previous low or high intake affects water, electrolyte and acid-base balance differently.” The British journal of nutrition vol. 101,9 (2009): 1286-94. doi:10.1017/S0007114508088041
McClure, Charles J. and Robert Oh. “Medial Tibial Stress Syndrome.” StatPearls, StatPearls Publishing, 11 August 2021.
Professional Scope of Practice *
The information herein on "Medial Tibial Stress Syndrome: Shin Splints" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card