“For individuals looking to improve their spinal health, can understanding the anatomy of the intervertebral foramen help in injury rehabilitation and prevention?”
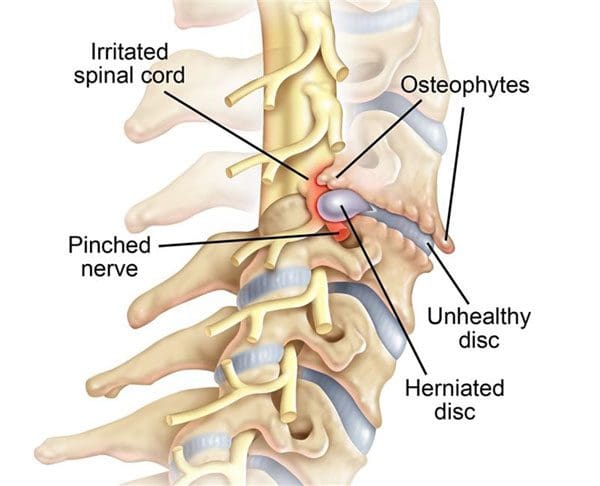
Intervertebral Foramen
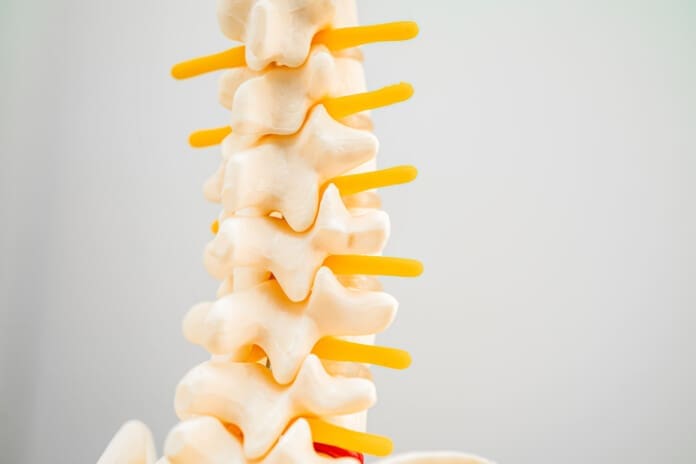
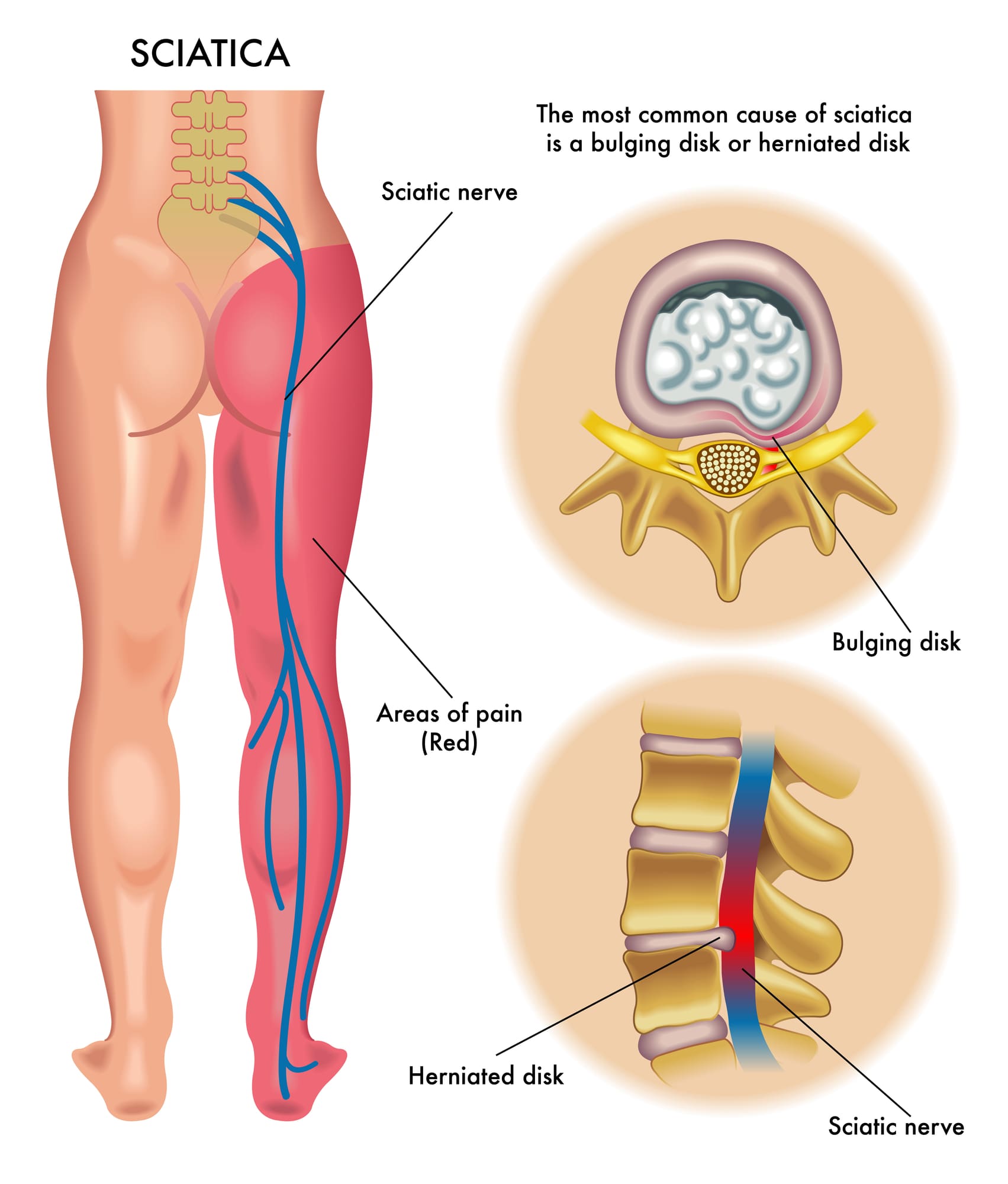
The intervertebral foramen, aka neural foramen, is the opening between the vertebrae through which spinal nerve roots connect and exit to other body areas. If the foramina narrows, it can place added pressure on the nerve roots near and around them, causing pain symptoms and sensations. This is known as neuroforaminal stenosis. (Sumihisa Orita et al., 2016)
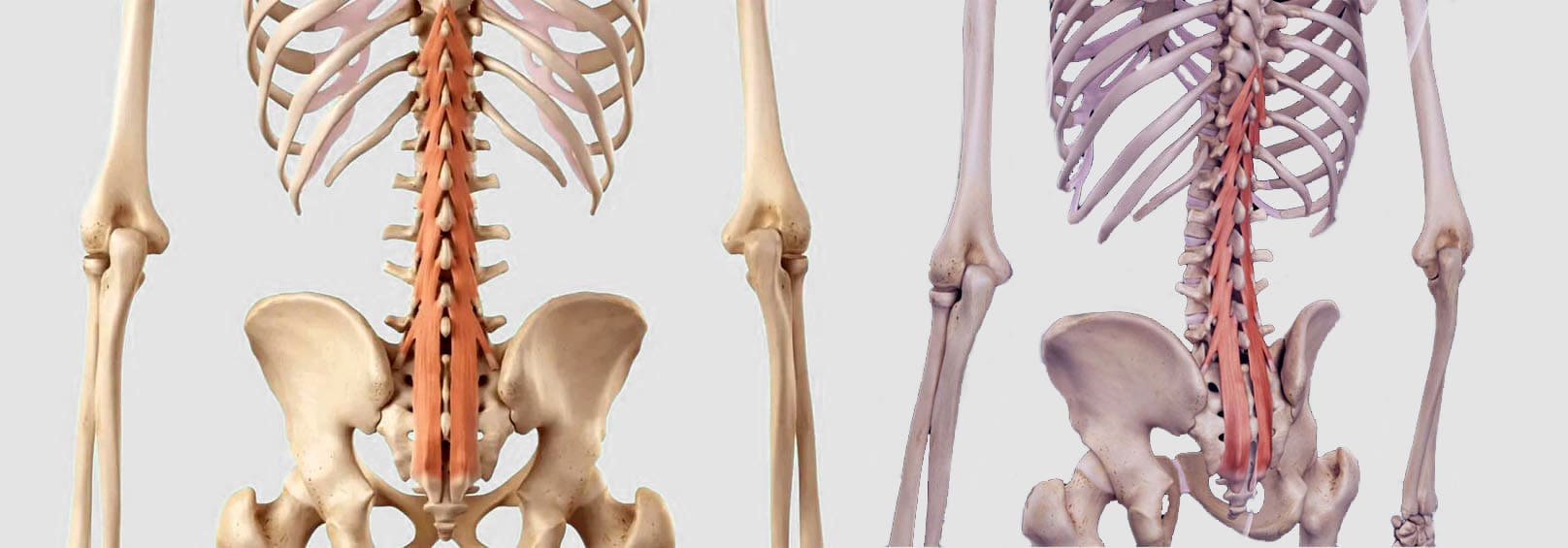
Anatomy
- The vertebrae comprise the spinal column.
- They protect and support the spinal cord and most of the weight placed on the spine.
- Foramen is the singular form, and foramina is the plural form.
Structure
- The body is the large, round part of the bone that makes up each vertebra.
- The body of each vertebra is attached to a bony ring.
- As the vertebrae are stacked on each other, the ring creates a tube through which the spinal cord passes. (American Academy of Orthopaedic Surgeons 2020)
- The intervertebral foramen opening is between every two vertebrae, where the nerve roots exit the spine.
- Two neural foramina exist between each pair of vertebrae, with one on each side.
- The nerve roots move through the foramen to the rest of the body.
Function
- The intervertebral foramina are exits from which the nerve roots leave the spine and branch out to the rest of the body.
- Without the foramen, nerve signals cannot transmit to and from the brain to the body.
- Without nerve signals, the body is unable to function correctly.
Conditions
A common condition that can affect the neuroforamina is spinal stenosis. Stenosis means narrowing.
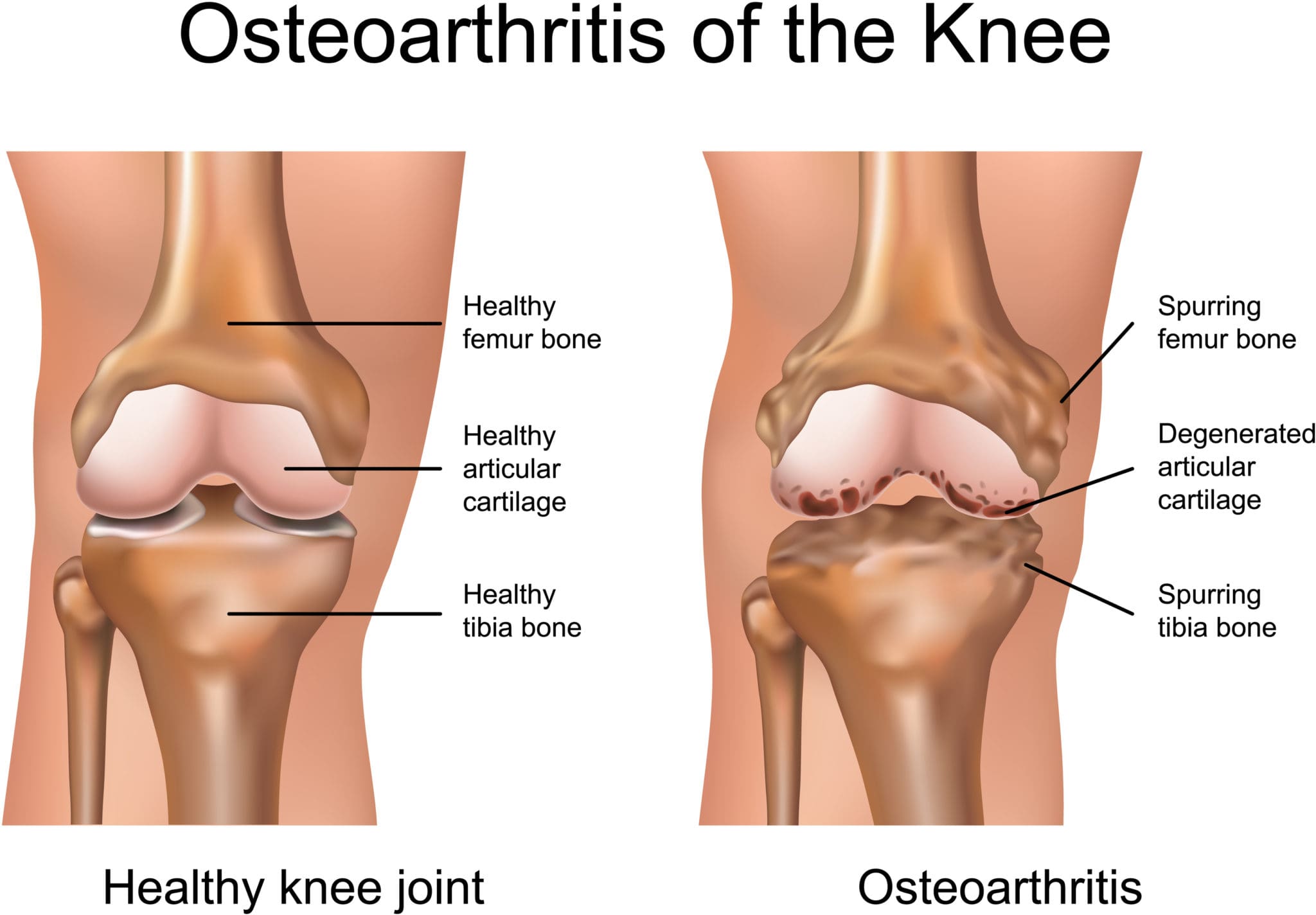
- Spinal stenosis is (not always) usually an age-related disorder associated with arthritis. (American Academy of Orthopaedic Surgeons, 2021)
- Stenosis can occur in the spinal canal, known as central canal stenosis, and the foramina.
- Pain brought on by neuroforaminal spinal stenosis and arthritis-related bone growth/bone spurs/osteophytes that are present in one or more foramen rub against the nerve root that passes through the space, causing radicular pain.
- Pain accompanied by other sensations, like tingling or numbness, is known as radiculopathy. (Young Kook Choi, 2019)
- The main symptom is pain.
- Numbness and/or tingling can present depending on the injury.
- Neurogenic claudication occurs as a result of ischemia or a lack of blood circulation to the nerves and typically presents with a heaviness in the legs.
- It is typically associated with central stenosis rather than foraminal stenosis.
- Most individuals with spinal stenosis feel better when flexing or bending forward and worse when arching their backs.
- Other symptoms include weakness and/or difficulty walking. (Seung Yeop Lee et al., 2015)
Treatment
Stenosis treatment aims to relieve pain and prevent nerve symptoms from occurring or worsening. Conservative treatments are recommended and can be highly effective.
These include:
- Physical therapy
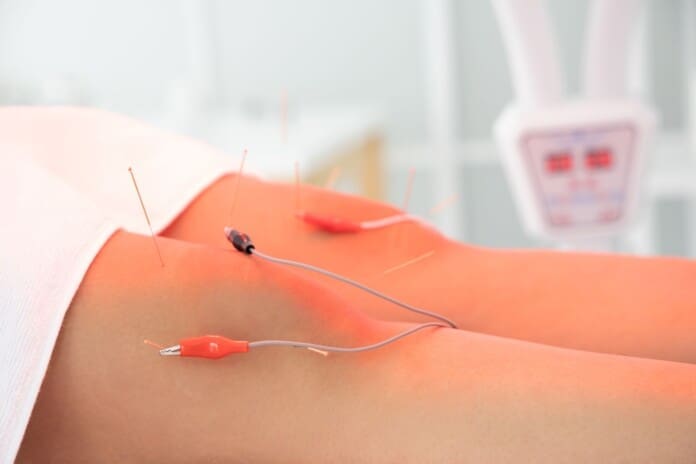
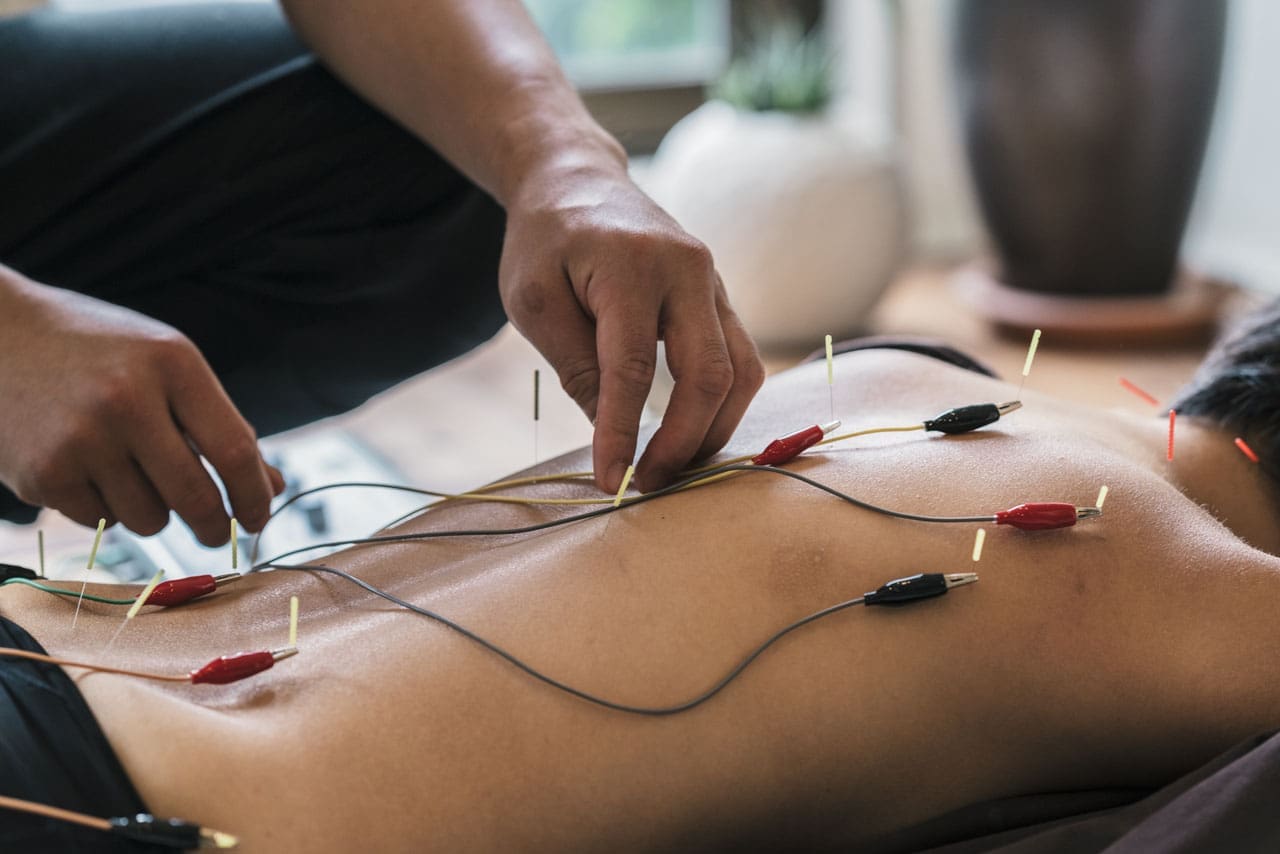
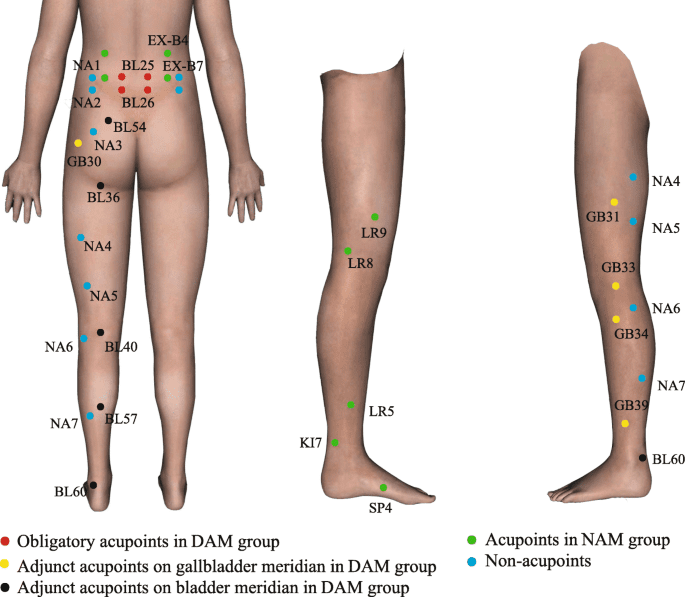
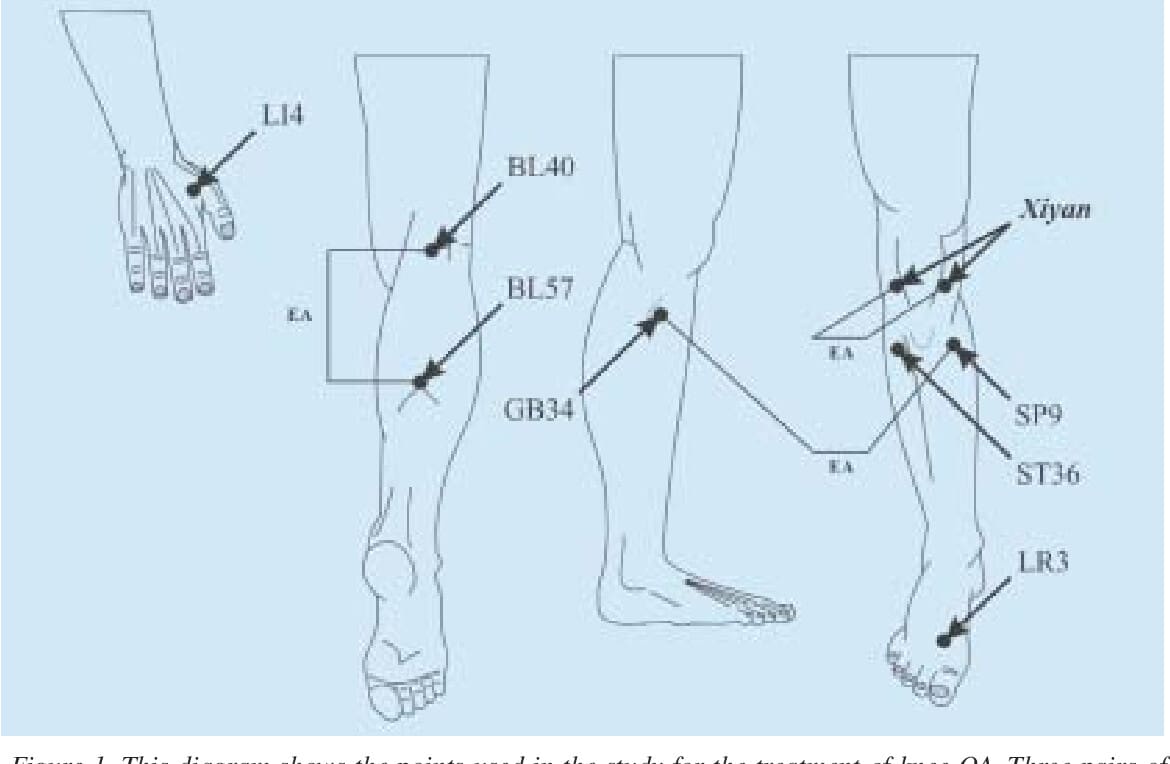
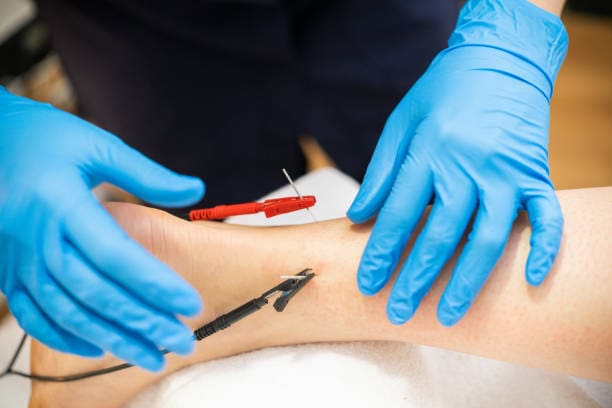
- Acupuncture and Electroacupuncture
- Chiropractic
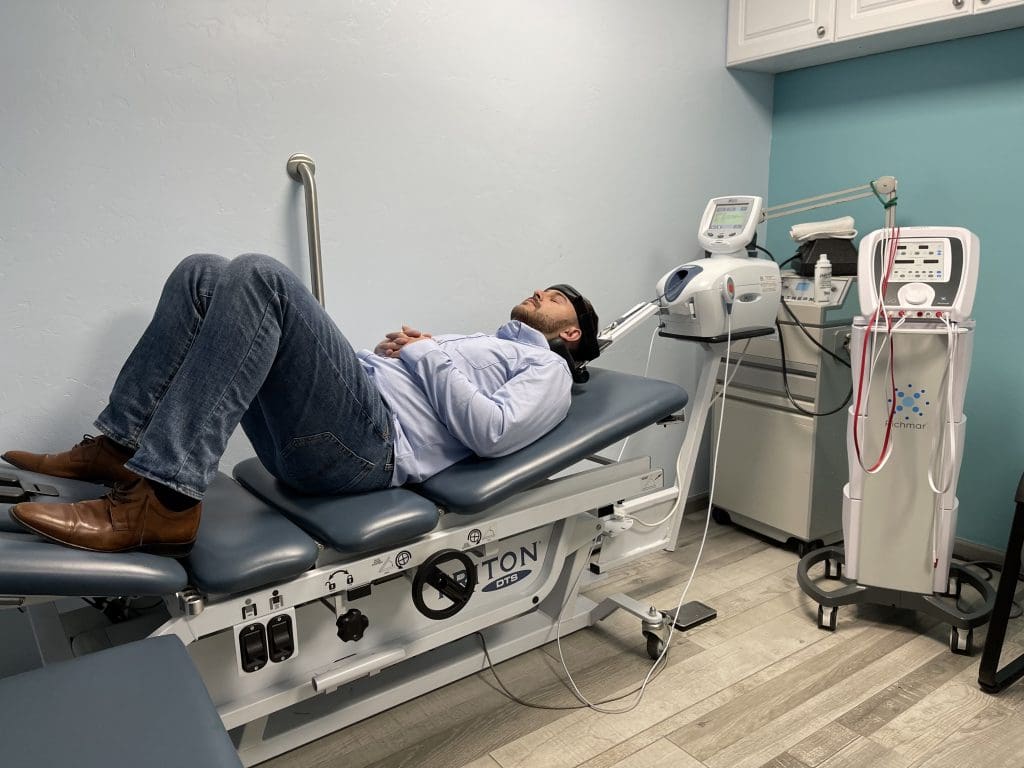
- Non-surgical decompression
- Therapeutic massage
- Nonsteroidal anti-inflammatory drugs/NSAIDs
- Targeted exercises and stretches
- Cortisone injections. (American Academy of Orthopaedic Surgeons, 2021)
- Surgery is usually not necessary.
However, a doctor may recommend surgery for an individual who is experiencing:
- Radiculopathy – pain, pins and needles, electrical sensations, and/or weakness going down one arm or leg (Jon Lurie, Christy Tomkins-Lane, 2016)
- Neurogenic claudication in the lower back (Jon Lurie, Christy Tomkins-Lane, 2016)
- Myelopathy in the neck and/or upper or mid-back (myelopathy symptoms are spinal cord related and occur in central canal stenosis) (Cleveland Clinic. 2021)
- Intense incapacitating pain
Different surgical techniques include:
- Decompression laminectomy – entails removing the buildup of bone in the spinal canal.
- Spinal fusion – when there is instability of the spine or severe foraminal stenosis.
- However, most cases don’t require fusion. (American Academy of Orthopaedic Surgeons, 2021)
Root Causes Spinal Stenosis
References
Orita, S., Inage, K., Eguchi, Y., Kubota, G., Aoki, Y., Nakamura, J., Matsuura, Y., Furuya, T., Koda, M., & Ohtori, S. (2016). Lumbar foraminal stenosis, the hidden stenosis including at L5/S1. European journal of orthopaedic surgery & traumatology : orthopedie traumatologie, 26(7), 685–693. https://doi.org/10.1007/s00590-016-1806-7
American Academy of Orthopaedic Surgeons. (2020). Spine Basics (OrthoInfo, Issue. https://orthoinfo.aaos.org/en/diseases–conditions/spine-basics/
American Academy of Orthopaedic Surgeons. (2021). Lumbar spinal stenosis (OrthoInfo, Issue. https://orthoinfo.aaos.org/en/diseases–conditions/lumbar-spinal-stenosis/
Choi Y. K. (2019). Lumbar foraminal neuropathy: an update on non-surgical management. The Korean journal of pain, 32(3), 147–159. https://doi.org/10.3344/kjp.2019.32.3.147
Lee, S. Y., Kim, T. H., Oh, J. K., Lee, S. J., & Park, M. S. (2015). Lumbar Stenosis: A Recent Update by Review of Literature. Asian spine journal, 9(5), 818–828. https://doi.org/10.4184/asj.2015.9.5.818
Lurie, J., & Tomkins-Lane, C. (2016). Management of lumbar spinal stenosis. BMJ (Clinical research ed.), 352, h6234. https://doi.org/10.1136/bmj.h6234
Cleveland Clinic. (2021). Myelopathy (Health Library, Issue. https://my.clevelandclinic.org/health/diseases/21966-myelopathy