Table of Contents
Keeping Pain at Bay: Preventing Sports Injuries with Chiropractic and Holistic Care

Sports fuel excitement, fitness, and camaraderie. Whether you’re dashing across a soccer field, swinging a golf club, or jogging through El Paso’s scenic trails, the thrill of movement is hard to beat. But injuries—like muscle strains, joint sprains, or nerve irritation—can halt your momentum. The good news? Many of these setbacks are preventable with a strategic, multifaceted approach. At our El Paso clinic, led by Dr. Alexander Jimenez, DC, APRN, FNP-BC, we combine chiropractic expertise, functional medicine, and integrative therapies to help athletes stay injury-free and perform at their peak.
This article examines practical habits to prevent sports injuries, including warm-ups, proper form, balanced conditioning, technique, and effective recovery. We’ll highlight how our clinic’s chiropractic adjustments and holistic care—rooted in personalized assessments and natural healing—build resilience. Drawing from trusted sources and Dr. Jimenez’s 30+ years of experience, we’ll demonstrate how our patient-centered approach enables El Paso athletes, from casual players to professionals, to move freely. Let’s build a game plan to keep you active and pain-free.
The Power of Prevention: Why It Matters
Sports injuries are a common hurdle, with studies indicating that up to 30% of athletes experience issues such as sprains or tendonitis each year, often due to avoidable causes like poor posture or overexertion (Abernethy & Bleakley, 2007). These injuries can disrupt play and, if ignored, lead to chronic pain or reduced mobility. For example, repetitive stress on nerves or joints can cause discomfort that radiates, making daily tasks challenging.
A multifaceted approach—blending daily routines with expert care—slashes injury rates by up to 50% (Abernethy & Bleakley, 2007). At our El Paso clinic, Dr. Jimenez utilizes advanced diagnostics, including neuromusculoskeletal imaging, to identify risks early. “Pain often signals underlying imbalances we can address before they worsen,” he says, drawing on his dual expertise as a chiropractor and nurse practitioner (Jimenez, n.d.a). Our goal is to keep you moving, not sidelined.
Warm-Ups and Cool-Downs: Your First Step to Safety
Kick off every session with a warm-up. A 5-10 minute routine of light activity—such as jogging in place or arm swings—followed by dynamic stretches like lunges, prepares your body for action (Mount Sinai Health System, n.d.). This reduces the risk of muscle strain by approximately 30% (Keck Medicine of USC, 2023).
Post-workout, cool-downs are key. Spend 10 minutes on static stretches, such as holding a hamstring stretch for 20 seconds, to reduce tension and clear metabolic waste (Nationwide Children’s Hospital, n.d.). Our clinic’s imaging demonstrates that consistent warm-ups enhance joint mobility, particularly for individuals with a history of injuries (Jimenez, n.d.a). A local basketball player, for instance, avoided repeat calf strains after adopting our tailored warm-up plan.
This habit lays the groundwork for all prevention efforts.
Proper Form: Move Right, Stay Strong
Good technique is your body’s armor. Poor form—such as twisting awkwardly during a golf swing or slumping while lifting—strains muscles and joints, increasing the risk of injury by up to 40% (Greater Pittsburgh Orthopaedic Associates, n.d.). Proper form ensures forces spread evenly, protecting nerves and tissues.
Work with a coach to perfect movements. Runners should land mid-foot to spare joints; weightlifters need a straight back to avoid nerve compression (University of Texas Medical Branch, 2017). Dr. Jimenez’s clinic utilizes dual-scope assessments—combining chiropractic and medical evaluations—to identify faulty patterns. “A misaligned spine can pinch nerves, causing pain down the leg,” he notes, using adjustments to restore balance (Jimenez, n.d.b). A soccer player we treated dodged knee pain by correcting her kicking form after our analysis.
Form is a vital layer in our comprehensive plan.
Balanced Conditioning: Build a Durable Body
Conditioning creates a body that can withstand the demands of sports. Strength exercises, such as core planks or leg presses, stabilize joints (Bayfront Health, n.d.). Flexibility routines, like yoga, keep muscles pliable (Hyperice, n.d.). Endurance, built through steady cardio exercises such as swimming, helps prevent fatigue-related missteps (Long Island Spine Rehabilitation Medicine, 2024).
Follow the 10% rule: Increase intensity by no more than 10% weekly to avoid overuse (Bayfront Health, n.d.). Cross-training—mixing running with biking—rests specific muscle groups. Balanced programs reduce injuries, such as ligament tears, especially in young athletes (Abernethy & Bleakley, 2007). Our clinic’s functional assessments, including lab work, identify weaknesses such as low nutrient levels that can stress joints. Dr. Jimenez designs custom exercise and nutrition plans to address these (Jimenez, n.d.a).
Conditioning strengthens the base established by warm-ups and form.
Recovery: Recharge to Thrive
Recovery is your secret weapon. Muscles repair during rest, so aim for 7-9 hours of sleep and one rest day weekly (Made for This Moment, n.d.). Active recovery, such as light stretching, eases soreness without strain (Fick PT & Performance, n.d.).
Nutrition and hydration are critical. Eat protein-rich foods (lean meats, lentils) and carbs (quinoa, fruits) to rebuild tissue. Drink half your body weight in ounces of water daily, or more in El Paso’s heat, to prevent muscle cramps (LispineMed, 2024). Our clinic’s functional nutrition plans, guided by lab tests, target inflammation. A runner with joint pain experienced relief after we boosted her omega-3 intake (Jimenez, n.d.a).
Recovery ties all prevention strategies together.
Gear and Environment: Simple Safeguards
Wear the right gear—running shoes with good support, helmets for contact sports (Johns Hopkins Medicine, n.d.). Check playing surfaces for hazards like uneven ground (Nicklaus Children’s Hospital, n.d.). These steps add a practical shield to your plan.
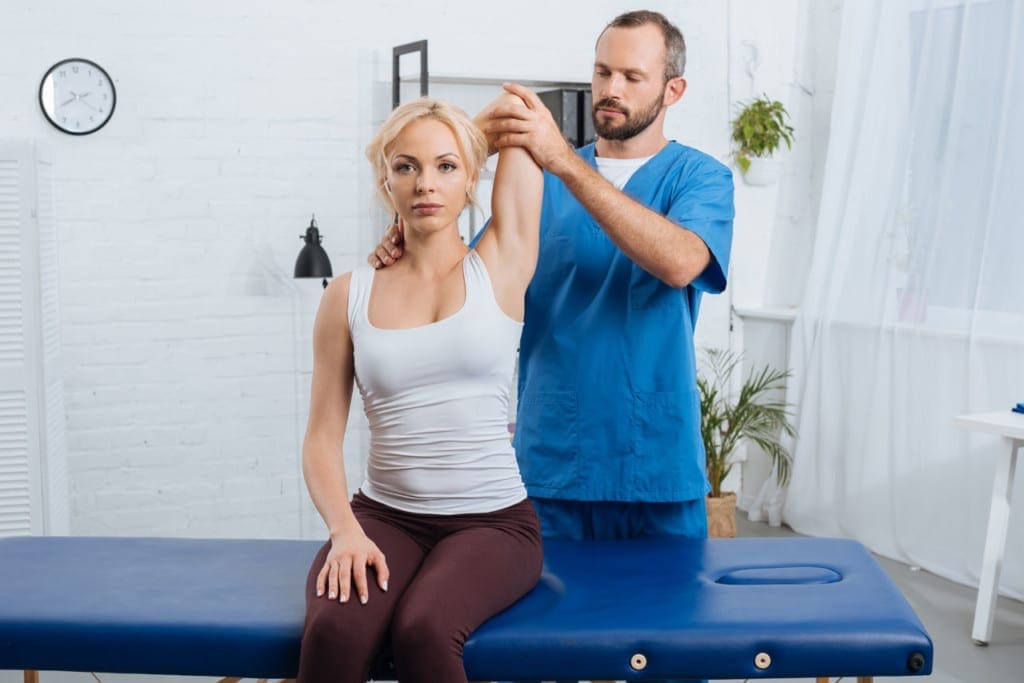
Chiropractic Care: Align for Resilience
Chiropractic care enhances prevention by aligning joints, improving nerve function, and relieving muscle tension (Premier Injury Clinics of DFW, n.d.). Adjustments correct misalignments that could pinch nerves, boosting mobility and reducing pain (Evolved Health Chiropractic, n.d.). Techniques like massage or kinesio taping aid recovery (Advanced Spine & Posture, n.d.).
At our El Paso clinic, Dr. Jimenez’s adjustments help athletes stay agile and maintain their optimal performance. A cyclist with hip pain returned to racing after we realigned her spine, easing nerve pressure (Jimenez, n.d.b). Our care often speeds up recovery by 50%, allowing you to stay active. We also treat work and auto accident injuries, using chiropractic to restore function.
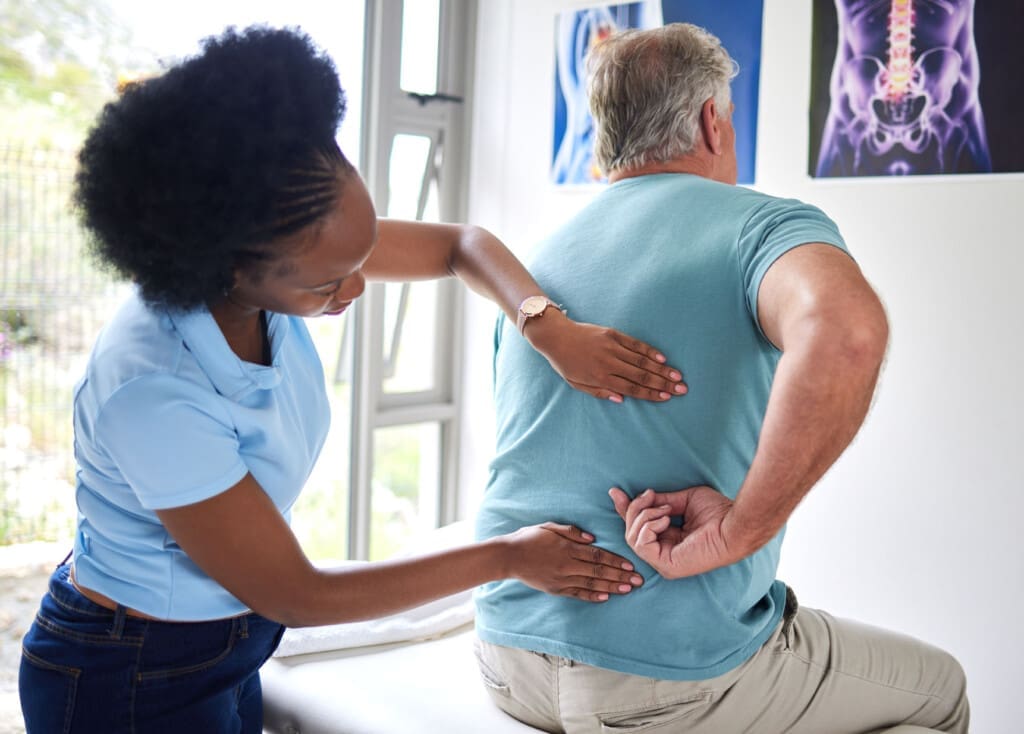
Functional Medicine: A Whole-Body Approach
Our functional medicine approach examines your entire health—encompassing nutrition, lifestyle, and genetics—to prevent injuries (El Paso Health Coach Clinic, n.d.). We integrate chiropractic care with physical therapy, nutritional coaching, and therapies such as acupuncture (Dallas Accident and Injury Rehab, n.d.a). PT strengthens muscles; nutrition reduces inflammation; acupuncture eases pain (Tigard Chiropractic Auto Injury, n.d.).
For a softball player with shoulder strain, we combined adjustments, PT, and a diet rich in anti-inflammatory foods, cutting recovery time (Jimenez, n.d.a). Lab work guides our plans, ensuring tailored care. For accident victims, we provide detailed legal documentation while promoting natural healing and recovery.
Dr. Jimenez’s Expertise: Personalized Care in El Paso
Dr. Alexander Jimenez, with over 30 years as a chiropractor and nurse practitioner, brings a dual perspective to our clinic. His advanced imaging and lab tests pinpoint the causes of injuries—whether from sports, work, or car accidents. A hiker’s leg pain was traced to a nutrient deficiency, fixed with supplements and adjustments (Jimenez, n.d.b). For auto accident cases, we document injuries for legal needs while addressing root issues.
“We aim for natural healing,” Dr. Jimenez says, using nutrition, exercise, and therapies to prevent chronic pain. His care empowers everyone, from teens to seniors.
Your Playbook for Staying Active
Combine warm-ups, proper form, balanced conditioning, recovery, gear, chiropractic care, and functional medicine for optimal performance. Track progress with a journal or app. At our El Paso clinic, we’re here to guide you. Call 915-412-6677 or visit our website to start your pain-free journey.

References
Abernethy, L., & Bleakley, C. (2007). Strategies to prevent injury in adolescent sport: A systematic review. British Medical Journal, PMC2465167. https://pmc.ncbi.nlm.nih.gov/articles/PMC2465167/
Advanced Spine & Posture. (n.d.). Sports injuries treated with chiropractic care. https://advancedspineandposture.com/blog/sports-injuries-treated-with-chiropractic-care/
Bayfront Health. (n.d.). Guide to sports injury prevention [PDF]. https://www.bayfronthealth.com/-/media/files/orhe-0479-bhsp-guide-to-sports-injury-prevention_508.pdf
Current Physical Therapy. (2025, August 11). How chiropractic treatment for sports injuries helps athletes recover faster. https://www.currentphysicaltherapy.com/2025/08/11/how-chiropractic-treatment-for-sports-injuries-helps-athletes-recover-faster/
Dallas Accident and Injury Rehab. (n.d.a). Integrating chiropractic expertise and holistic sports medicine for enhanced athletic well-being. https://dallasaccidentandinjuryrehab.com/integrating-chiropractic-expertise-and-holistic-sports-medicine-for-enhanced-athletic-well-being/
Dallas Accident and Injury Rehab. (n.d.b). Preventing sports injuries with chiropractic care. https://dallasaccidentandinjuryrehab.com/preventing-sports-injuries-with-chiropractic-care/
El Paso Health Coach Clinic. (n.d.). Functional Medicine and Wellness. https://elpasofunctionalmedicine.com/
Evolved Health Chiropractic. (n.d.). Preventing sports injuries: The role of chiropractic in injury prevention. https://evolvedhealthchiropractic.com/blog/preventing-sports-injuries-the-role-of-chiropractic-in-injury-prevention/
Fick PT & Performance. (n.d.). Why injury prevention is the key to your football season. https://fickptandperformance.com/why-injury-prevention-is-the-key-to-your-football-season/
Greater Pittsburgh Orthopaedic Associates. (n.d.). The right gear matters: Choosing equipment to prevent sports injuries. https://www.gpoa.com/blog/the-right-gear-matters-choosing-equipment-to-prevent-sports-injuries
Hyperice. (n.d.). How to increase flexibility. https://hyperice.com/blog/performance/how-to-increase-flexibility/
Jimenez, A. (n.d.a). Injury specialists. https://dralexjimenez.com/
Jimenez, A. (n.d.b). Dr. Alexander Jimenez, DC, APRN, FNP-BC, IFMCP, CFMP, ATN ♛ – Injury Medical Clinic PA. LinkedIn. https://www.linkedin.com/in/dralexjimenez/
Johns Hopkins Medicine. (n.d.). Sports safety. https://www.hopkinsmedicine.org/health/wellness-and-prevention/sports-safety
Keck Medicine of USC. (2023). How to prevent sports injuries. https://www.keckmedicine.org/blog/how-to-prevent-sports-injuries/
LispineMed. (2024, August 1). 10 tips for preventing sports injuries. https://www.lispinemed.com/2024/08/01/10-tips-for-preventing-sports-injuries/
Made for This Moment. (n.d.). Youth sports injuries – Prevention & treatment. https://madeforthismoment.asahq.org/pain-management/types-of-pain/youth-sports/
Mount Sinai Health System. (n.d.). Preventing sports injuries. https://www.mountsinai.org/care/orthopedics/services/sports-medicine/conditions/sports-injury-prevention
Nationwide Children’s Hospital. (n.d.). Preventing sports injuries. https://www.nationwidechildrens.org/family-resources-education/family-resources-library/preventing-sports-injuries
Nicklaus Children’s Hospital. (n.d.). Sports injury prevention STOP sports injuries. https://www.nicklauschildrens.org/medical-services/sports-health/sports-injury-prevention-stop-sports-injuries
Premier Injury Clinics of DFW. (n.d.). Guide to preventing sports injuries. https://premierinjuryclinicsofdfw.com/guide-to-preventing-sports-injuries/
Tigard Chiropractic Auto Injury. (n.d.). Integrating exercise with chiropractic: A synergistic approach to sports medicine. https://www.tigardchiropracticautoinjury.com/integrating-exercise-with-chiropractic-a-synergistic-approach-to-sports-medicine
University of Texas Medical Branch. (2017, October 24). Top 6 sports injury prevention tips. https://www.utmb.edu/impact/home/2017/10/24/top-6-sports-injury-prevention-tips