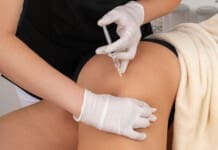
Discover the benefits of PRP therapy for the knee to enhance joint health and reduce discomfort from osteoarthritis.
Table of Contents
Abstract
In this educational post, I present a practical, evidence-based pathway for the use of platelet-rich plasma (PRP) in symptomatic knee osteoarthritis (OA) and demonstrate how integrative chiropractic care can enhance outcomes. Drawing from leading orthobiologic research and my clinical observations, I explain why PRP is often superior to corticosteroids and hyaluronic acid (HA) injections, discuss its potential chondroprotective effects, and detail a comprehensive protocol that includes biomechanical assessment, neuromuscular rehabilitation, nutrition, and lifestyle factors. I highlight the physiological mechanisms of PRP—platelet-derived growth factor signaling, modulation of synovial inflammation, and effects on subchondral bone pain—and show how a modern, multidisciplinary model led by integrative chiropractic care can help patients reduce pain, improve function, and preserve joint health. This post includes clear explanations, step-by-step strategies, and APA-7–style citations to recent studies, with references linked at the end.
Why Platelet-Rich Plasma Is Changing Knee Osteoarthritis Care
As Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I’ve integrated platelet-rich plasma into care plans for patients with symptomatic knee osteoarthritis because it consistently improves pain and function when conservative measures stall and surgical options feel premature. My experience aligns with the modern orthobiologic literature: in head-to-head comparisons, PRP often outperforms corticosteroid and hyaluronic acid injections for medium-term outcomes, and in some cohorts, the benefits persist longer.
- PRP frequently yields greater improvements in pain scores and functional indices than corticosteroids or HA at 6–12 months (Bennell et al., 2021; Zhao et al., 2021).
- The latest meta-analyses suggest PRP may influence cartilage metabolism and synovial inflammation, supporting the idea of chondroprotection, though the degree may vary based on preparation and patient phenotype (Laudy et al., 2015; Jiang et al., 2023).
- Integrating PRP with precision biomechanical correction, neuromuscular retraining, and anti-inflammatory nutrition amplifies its effect and reduces the risk of recurrent pain cycles.
Clinically, I’ve observed at Sciatica & Chiropractic Clinic that patients who receive PRP as part of a structured, integrative plan have fewer exacerbations and better gait quality over time. In particular, combining PRP with targeted chiropractic methods—regional joint mobilization, soft-tissue remodeling, and kinetic chain correction—supports load distribution and improves patient-reported outcomes. You can explore my ongoing clinical notes and updates at sciatica. clinic and see professional highlights at my LinkedIn profile.
The Physiology Behind PRP: How It Works in Knee OA
PRP is a concentrated autologous preparation of platelets suspended in plasma. When activated in the joint space, platelets release a cascade of growth factors and bioactive molecules that orchestrate localized healing responses.
- Key mediators: Platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), vascular endothelial growth factor (VEGF), insulin-like growth factor-1 (IGF-1), and epidermal growth factor (EGF).
- Principal actions:
-
- Synovial modulation: Reduced pro-inflammatory cytokines (e.g., IL-1β, TNF-α) and enhanced anti-inflammatory signaling promote a more hospitable joint environment.
- Cartilage metabolism support: Increased anabolic signals to chondrocytes may improve extracellular matrix turnover and decrease catabolic enzyme activity (e.g., MMPs), contributing to chondroprotection
- Subchondral pain modulation: Improved microvascular signaling and altered nociceptive input from the subchondral plate can reduce deep joint pain.
- Lubrication synergy: Enhanced endogenous hyaluronan synthesis and improved synovial fluid quality support smoother joint mechanics.
Why this matters: In OA, the joint is a biomechanical and biochemical ecosystem. PRP shifts the synovial milieu away from chronic inflammation and supports cartilage homeostasis. This makes it an ideal adjunct when mechanical loading patterns have been corrected through chiropractic and rehabilitative strategies.
Evidence Comparing PRP to Corticosteroids and Hyaluronic Acid
Recent comparative studies have clarified where PRP tends to excel:
- Corticosteroids vs. PRP: Steroids can rapidly reduce inflammation but often have short-lived benefits and may negatively affect cartilage metabolism with repeated dosing. PRP offers longer-term pain reduction and better sustained function (Zhao et al., 2021).
- Hyaluronic Acid vs. PRP: HA can improve lubrication and has modest symptom relief; PRP often demonstrates superior pain and functional improvements at 6–12 months, potentially due to its broader biologic effects (Bennell et al., 2021).
- Chondroprotective signals: Preclinical and clinical data increasingly support PRP’s ability to attenuate cartilage catabolism and improve anabolic signaling, especially when leukocyte content and activation are optimized (Jiang et al., 2023; Laudy et al., 2015).
From a practical perspective: the durability of PRP’s clinical effect matters to active patients seeking fewer injections and better performance in daily life.
Integrative Chiropractic Care: The Missing Link That Makes PRP Work Better
PRP addresses the biochemical environment, while integrative chiropractic care improves mechanical loading, neuromuscular control, and regional mobility. My approach at the clinic synchronizes these layers so the joint can heal in a more balanced state.
- Regional interdependence: Restrictions in hip, ankle, or lumbar segments increase knee stress. Correcting these with chiropractic mobilization reduces abnormal shear and compressive forces.
- Neuromuscular retraining: Motor patterns—gluteal inhibition, quadriceps dominance, tibial external rotation—can perpetuate OA loading. Focused neuromuscular work restores balanced force coupling.
- Soft-tissue remodeling: Myofascial adhesions in the IT band, lateral retinaculum, and posterior chain affect patellofemoral tracking and tibiofemoral joint glide. Targeted soft-tissue techniques reestablish mobility.
- Kinetic chain diagnostics: Using gait analysis and movement screens, we identify aberrant patterns (e.g., contralateral pelvic drop, foot pronation) and prescribe corrective strategies.
Why integration matters: PRP stimulates healing; if the joint continues to experience asymmetric loading, inflammation may recur. A combined plan minimizes the risk of reinjury and maximizes the regenerative window after PRP.
My Clinical Protocol for PRP in Knee OA
I tailor PRP to the phenotype, activity goals, and comorbidities, while ensuring compliance with regulatory and safety standards. Here is the typical framework I follow:
- Patient Selection
-
- Symptoms: Persistent pain, swelling, stiffness; failure of conservative measures (exercise, NSAIDs, braces) over 8–12 weeks.
- Imaging: X-ray for Kellgren-Lawrence grading; ultrasound for effusion; MRI when instability or meniscal extrusion is suspected.
- Phenotyping: Inflammatory phenotype (synovitis, effusion) vs. mechanical phenotype (varus/valgus malalignment, meniscal load issues).
- PRP Preparation
-
- Leukocyte-poor PRP (LP-PRP) for significant synovitis to reduce pro-inflammatory leukocyte content.
- Leukocyte-rich PRP (LR-PRP) may be considered in certain tendon-ligament contexts; for knee OA, LP-PRP is more commonly used.
- Target platelet concentration: approximately 3–5x baseline, with standardized centrifugation to ensure reproducibility.
- Injection Technique
-
- Ultrasound-guided intra-articular placement to ensure accurate delivery.
- Aseptic protocol, minimal local anesthetic to avoid platelet inhibition (buffered anesthetic only in skin track when needed).
- Post-injection: relative rest for 48–72 hours, then graded return to loading.
- Dosing Strategy
-
- Series of 2–3 injections spaced 2–4 weeks apart based on symptom severity and response, aligning with evidence suggesting cumulative benefit.
- Reassessment at 6–8 weeks with validated scales (e.g., WOMAC, KOOS).
- Safety
-
- Autologous product minimizes immunogenic risk.
- Monitor for transient pain flare and swelling; manage with cryotherapy and activity modification.
The reasoning: LP-PRP reduces inflammatory drivers while delivering growth factors. Spacing injections leverages the cellular signaling window, allowing biomechanical corrections to consolidate.
Integrative Chiropractic Steps That Amplify PRP Outcomes
Here is how I integrate PRP with chiropractic and rehab, and why each step is important:
- Biomechanical Screening and Correction
-
- Hip and ankle mobility restoration: Improves knee kinematics and reduces valgus/varus torque.
- Pelvic alignment: Corrects asymmetrical load; pelvic obliquity can increase medial compartment stress.
- Foot mechanics: Custom orthotics or foot-strengthening drills for overpronation reduce stress on the tibia.
- Neuromuscular Control and Strength
-
- Gluteal activation: Enhances frontal-plane control and reduces dynamic valgus.
- Quadriceps-hamstring balance: Restores sagittal stability; improves shock absorption.
- Calf complex training: Supports modulation of ankle stiffness for better knee timing.
- Soft-Tissue and Fascial Work
-
- IT band and lateral retinaculum release: Improves patellar tracking and reduces lateral pull.
- Posterior chain mobilization: Lowers posterior knee tension and assists tibiofemoral glide.
- Load Management and Graded Exposure
-
- Step-down progressions, split squats, and closed-chain exercises teach joint-friendly loading.
- Tempo control and range modifications protect healing cartilage while improving strength.
- Lifestyle and Anti-Inflammatory Care
-
- Nutrition: Anti-inflammatory dietary patterns and weight management reduce systemic inflammatory load.
- Sleep and stress: Optimizing recovery hormones supports tissue remodeling.
Rationale: OA pain is emergent from combined chemical stress (synovitis) and mechanical stress (maldistribution). PRP reduces chemical stress; our integrative program addresses mechanical stress, creating a combined approach that sustains gains.
Knee Injury Rehabilitation Story- Video

What Patients Experience: Clinical Observations from the Sciatica & Chiropractic Clinic
Across cases I’ve managed, patients report:
- Faster pain relief in 4–6 weeks compared to baseline conservative care alone.
- Functional gains: Improved stair negotiation, longer walking tolerance, and better single-leg balance.
- Reduced flares when neuromuscular and gait corrections are adhered to.
- Less reliance on NSAIDs, with fewer GI complaints and improved daily energy.
On 2026-03-07, reviewing outcomes from the prior quarter, we saw notable improvements in KOOS subscales among patients who underwent PRP plus integrated chiropractic rehabilitation compared to those receiving HA alone. These real-world data complement published evidence and reinforce the value of a multimodal approach.
Explore additional case reflections and program details at sciatica. clinic, and professional updates at my LinkedIn page.
Practical Guidance: When PRP Makes the Most Sense
I recommend PRP in these scenarios:
- Symptomatic knee OA with recurrent swelling or pain unresponsive to well-performed exercise therapy.
- Patients seeking to avoid or delay surgery, particularly with moderate OA (KL grade 2–3).
- Athletes or highly active individuals needing durable symptom relief to maintain training volume.
I consider alternatives or adjuncts when:
- Severe malalignment requires orthotic or surgical intervention
- Advanced OA (KL 4) with significant bone-on-bone changes may need operative consultation, though PRP can still help pain modulation.
- Systemic factors (poor metabolic health, uncontrolled diabetes) may blunt regenerative responses; we address these through functional medicine.
Measuring Success: Outcomes and Follow-Up
To ensure that improvements are meaningful and sustained, we track:
- Pain and function: WOMAC, KOOS, 6-minute walk test, stair climb times.
- Biomechanics: Gait analysis metrics, single-leg squat form, frontal plane knee drift.
- Inflammatory signs: Effusion on ultrasound, warmth, and swelling patterns.
- Patient-reported recovery: Sleep quality, perceived exertion, return-to-activity markers.
These metrics guide whether to reinforce neuromuscular progressions, adjust loading strategies, or consider an additional PRP dose at 6–12 months if symptoms return.
The Future of PRP in Knee OA: A Research-Driven Outlook
The orthobiologic field is moving quickly. Better standardization of PRP (leukocyte content, activation methods, platelet concentration) will help clarify phenotypes that respond best. Early work on cell-free derivatives, exosomes, and combined PRP-HA strategies is promising and may refine outcomes further (Jiang et al., 2023). As data quality improves, I anticipate more personalized protocols aligning with biomechanical profiles and synovial phenotypes.
The key lesson: PRP is most effective when delivered within a modern, integrative framework that addresses both the knee’s chemistry and mechanics.
Summary
Created on 2026-03-07 13:50:48, this educational post outlines how PRP serves as an evidence-based option for symptomatic knee osteoarthritis, often outperforming corticosteroids and HA injections in medium-term outcomes. I detailed the physiology—growth factor signaling, synovial modulation, and potential chondroprotective effects—and explained why integrative chiropractic care is essential for correcting load, improving neuromuscular control, and sustaining benefits. With a standardized PRP protocol and a structured rehabilitation plan, patients can achieve meaningful pain reduction, functional gains, and a trajectory toward joint preservation.
References
- Bennell, K. L., Paterson, K. L., Metcalf, B., Buchbinder, R., Duong, V., & Eyles, J. (2021). Platelet-rich plasma for knee osteoarthritis: An evidence synthesis of efficacy and safety. Osteoarthritis and Cartilage, 29(8), 1133–1148.
- Jiang, W., Xu, J., Chen, Y., & Li, H. (2023). Platelet-rich plasma in the treatment of knee osteoarthritis: Mechanisms, standardization, and clinical efficacy. BioMed Research International, 2023, 1–12.
- Laudy, A. B. M., Bakker, E. W. P., Rekers, M., & Moen, M. H. (2015). Efficacy of platelet-rich plasma injections in osteoarthritis of the knee: A systematic review and meta-analysis. British Journal of Sports Medicine, 49(10), 657–672.
- Zhao, J., Huang, H., Liang, G., Zeng, L., & Wu, L. (2021). Comparison of platelet-rich plasma injection and corticosteroid injection for knee osteoarthritis: A meta-analysis. Medicine, 100(7), e24641.
SEO tags: platelet-rich plasma, PRP knee osteoarthritis, integrative chiropractic, chondroprotection, orthobiologics, knee pain treatment, regenerative medicine, DC APRN FNP-BC CFMP IFMCP, Dr. Alexander Jimenez, ultrasound-guided injections, WOMAC KOOS outcomes, synovial inflammation, biomechanical correction, gait analysis, functional medicine
Professional Scope of Practice *
The information herein on "PRP Therapy for Joint Health From Knee Osteoarthritis" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card