Table of Contents
PRP Therapy for Spinal Care: A Natural, Minimally Invasive Option for Pain Relief and Healing
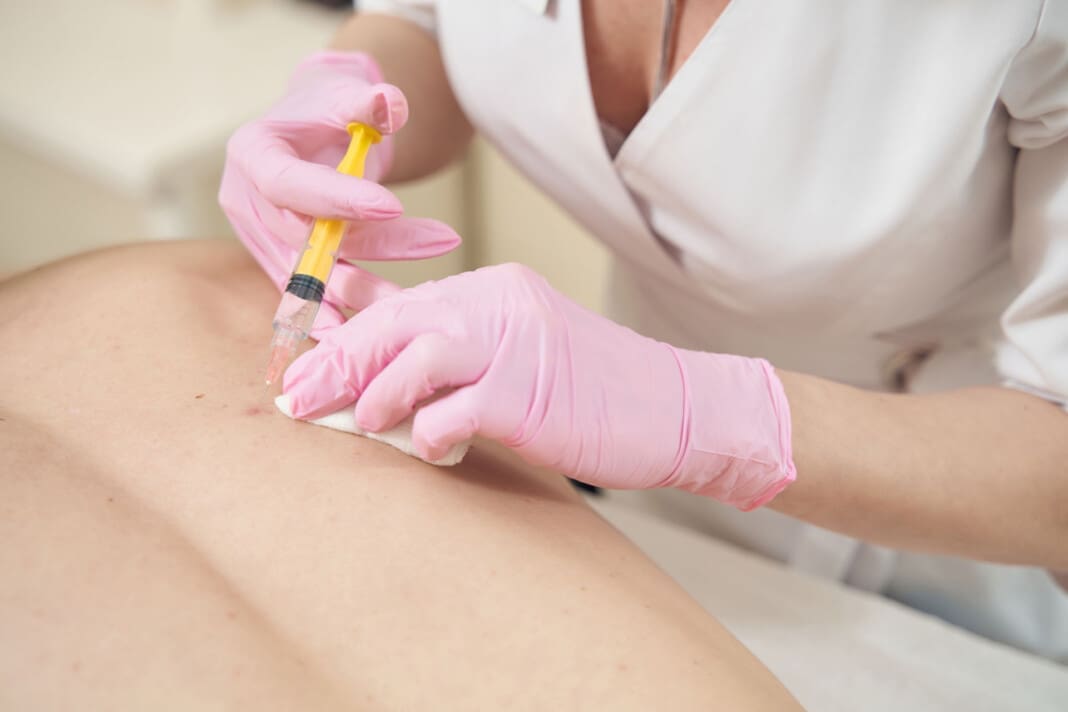
Platelet-Rich Plasma (PRP) therapy is gaining attention in spinal care because it uses a person’s own blood to support the healing of painful or damaged tissues. In simple terms, a small blood sample is taken, processed to separate the platelet-rich portion, and then placed into the target area. Platelets carry growth factors and signaling proteins that may help calm inflammation and support tissue repair. In spine care, PRP is being studied and used to treat conditions such as disc-related low back pain, facet-related pain, sacroiliac joint pain, and certain supportive soft tissue injuries around the spine.

What makes PRP appealing is that it is less invasive than surgery and aims to support healing instead of only numbing pain for a short time. That does not mean it is a miracle cure. It means PRP is an emerging regenerative option that may help the right patient when the pain source is correctly identified, and the treatment is part of a broader recovery plan. Recent reviews describe PRP as promising for spinal pain, but they also stress that treatment protocols still need better standardization.
What PRP Therapy Does in the Spine
The spine is made of more than bones. It includes discs, facet joints, ligaments, tendons, muscles, nerves, and stabilizing soft tissues. When these tissues break down or remain inflamed for too long, people may experience chronic low back pain, stiffness, reduced mobility, or pain that radiates into the hips or legs. PRP is meant to place healing signals right where the tissue is struggling. Research reviews describe PRP as a treatment that may support tissue regeneration, modulate inflammation, and improve function in some patients with spinal pain. Laboratory and animal research also suggest that PRP may support nerve recovery, which helps explain why it is being explored in nerve-related spine conditions, although this does not prove equal results in every human case.
PRP is most often discussed for discogenic low back pain, meaning pain that seems to come from a damaged or degenerating disc. It has also been studied for facet joint problems and used in other areas of spine-related pain care. In a systematic review of low back pain studies, most research focused on discogenic pain and intradiscal biologic treatments. That matters because PRP is not one single treatment for every back problem. The exact injection target should match the actual pain generator.
What the Evidence Says Right Now
The evidence for PRP in spinal care is encouraging, but not definitive. A 2023 systematic review found 13 randomized controlled trials and 27 non-randomized studies on PRP for low back pain and concluded that it appears to be a less invasive and generally safe option for chronic low back pain. Another clinical trial found that intradiscal PRP improved pain and lumbar function over a 48-week follow-up period in patients with discogenic low back pain. A health technology review from the NCBI Bookshelf also reported that PRP injections might be more effective than some other injections for lower back pain without increasing the risk of major complications.
At the same time, major guidelines still urge caution. The North American Spine Society guideline states that there is insufficient evidence to recommend for or against intradiscal PRP for discogenic low back pain. The same guideline notes that one randomized study showed meaningful improvements in pain and function for some patients, but the field still needs more high-level trials. That is why the most honest way to describe PRP for the spine is this: promising, useful for selected patients, but not yet a universally accepted standard treatment for every spinal condition.
Who May Be a Good Candidate for PRP Therapy for Spine Pain
People often look into PRP after more common treatments have not given enough relief. In the randomized study cited in the spine guideline, the patients had chronic lumbar discogenic pain for at least 6 months and had not improved with conservative treatment. Public-facing spine clinics also commonly list chronic back or neck pain, degenerative disc disease, facet joint pain, sacroiliac pain, spinal soft tissue problems, and some ligament-related injuries among the situations where PRP may be considered.
A possible PRP candidate often has these features:
- Ongoing low back or neck pain that has lasted for months
- A diagnosis that points to a disc, facet joint, SI joint, or supportive soft tissue source
- Limited response to physical therapy, exercise, medications, or other conservative care
- A desire to try a less invasive option before moving toward surgery
- A willingness to follow a full recovery plan, not just receive one injection and hope for the best
In cases of advanced degeneration, such as stage III and IV degenerative disc disease, PRP may still be a topic of discussion, but ongoing research is still in its infancy. Reviews of advanced disc degeneration report pain reduction and functional improvement in some studies, yet they also stress that more consistent protocols and stronger clinical evidence are still needed.
What a PRP Spine Visit Usually Looks Like
Most PRP spine visits follow a simple pattern. First comes a detailed history, physical exam, and review of imaging to confirm where the pain is really coming from. Next, blood is drawn and centrifuged to separate the platelet-rich portion. Thereafter, the PRP is placed into the target area using image guidance, often ultrasound or fluoroscopy, to improve accuracy. Clinics and public patient guides also note that PRP is usually done as an outpatient procedure, so many patients go home the same day.
Recovery is usually gradual, not instant. Mild soreness or temporary stiffness for a few days is common. Many clinics advise avoiding heavy lifting or strenuous exercise for about 1 to 2 weeks, depending on the area treated, while improvement in pain and mobility may take several weeks to months. Some patient guides report that many people return to normal activities within a day or two, but that should be understood as light daily activity, not a full return to heavy spinal loading right away.
Why an Integrative APRN, Functional Medicine, and Chiropractic Model Can Matter
PRP works best when it is part of a full plan. A needle alone cannot fix poor movement patterns, weak support muscles, poor sleep, chronic inflammation, nutritional gaps, or repeated overload on the spine. Dr. Alexander Jimenez’s public materials describe a dual-scope model that combines chiropractic care, family nurse practitioner medicine, functional medicine, acupuncture, sports medicine principles, individualized examinations, and image-guided procedures. His public content also describes PRP as something that may work best when paired with rehabilitation, imaging-guided precision, and metabolic or nutritional support, rather than being treated as a stand-alone fix. His LinkedIn profile summary similarly emphasizes helping the body heal without drugs or invasive procedures when appropriate.
In practical terms, this kind of integrative model can add value in several ways:
- Medical evaluation by an APRN/FNP-BC to review symptoms, imaging, medications, and whole-person health factors
- Functional medicine support to address inflammation, blood sugar balance, nutrition, body composition, and recovery habits
- Precise image-guided placement of PRP into the right structure
- Chiropractic and movement-based care to improve joint motion, posture, and load management
- Rehabilitation and follow-up so the spine heals in a stronger mechanical environment
This does not prove that each added therapy automatically makes PRP stronger in every case. But it does fit what many spine and pain experts already recognize: chronic spinal pain usually responds better to a multimodal plan than to a one-step treatment. Reviews of spinal manipulative therapy and spine care also support using conservative care as part of a broader, patient-centered approach.
Benefits of PRP Therapy for Spinal Care
When PRP is used for the right patient and the right diagnosis, the possible benefits may include:
- A minimally invasive, non-surgical treatment option
- Use of the patient’s own blood product
- Reduced inflammation in some painful spinal tissues
- Improved pain and function in selected patients
- Low rate of serious adverse events in the published literature
- Potential support for tissue repair instead of temporary symptom masking alone
Important Limits to Remember
PRP is not the best answer for every back problem. It is not a guaranteed cure for advanced degeneration, spinal instability, fracture, tumor, severe nerve compression, or any cause of chronic pain. It also does not replace the need for a careful diagnosis. If the real source of pain is missed, even a well-done PRP injection may fail. That is one reason major guidelines still call for more high-quality randomized trials before stronger recommendations can be made.
Final Thoughts
PRP therapy for spinal care is one of the most intriguing regenerative options in modern back pain treatment. It uses the body’s own platelets to reduce inflammation and support healing of damaged spinal tissues, such as discs, facet-related structures, and other supportive soft tissues. The research so far is promising, especially for selected patients with chronic disc-related low back pain, but the science is still developing. The best outcomes are likely to come from careful diagnosis, precise image-guided treatment, and a full recovery plan that includes movement, structural care, and metabolic support. That is why an integrative model that combines regenerative medicine, functional medicine, and spine-focused rehabilitation may be especially valuable in real-world patient care.

References
- Apostolakis, S., et al. (2023). Platelet-Rich Plasma for Degenerative Spine Disease: A Brief Overview. PMC.
- Greater Austin Pain Center. (n.d.). PRP Injections for Joint and Spine Pain: What You Need to Know.
- Jimenez, A. (n.d.). PRP Therapy for Sciatica: The Future of Pain Management. DrAlexJimenez.com.
- Jimenez, A. (n.d.). Why Choose Our Clinical Team?. DrAlexJimenez.com.
- Machado, E. S., et al. (2023). Systematic Review of Platelet-Rich Plasma for Low Back Pain. PMC.
- Morrison Clinic. (n.d.). Platelet Rich Plasma Therapy for Spine: Effectiveness, Safety, and Clinical Applications.
- National Center for Biotechnology Information. (2023). Platelet-Rich Plasma Injections for Lower Back Pain. NCBI Bookshelf.
- North American Spine Society. (2020). Diagnosis and Treatment of Low Back Pain – Clinical Guideline.
- Ohio State Wexner Medical Center. (n.d.). The Benefits of Using Platelet-Rich Plasma Therapy to Treat Back Pain.
- Wang, S., et al. (2024). Platelet-rich Plasma (PRP) in Nerve Repair. PMC.
- Zhang, J., et al. (2022). Intradiscal Autologous Platelet-Rich Plasma Injection for Discogenic Low Back Pain: A Clinical Trial. PMC.
Professional Scope of Practice *
The information herein on "Spine Health: PRP Therapy for Pain Relief" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card