How do healthcare professionals provide a clinical approach in the role of nursing to reducing pain in individuals?
Introduction
The practice of Registered Nurses (RN), Advanced Practice Registered Nurses (APRN), and Licensed Practical Nurses (L.P.N.) is governed by the Nurse Practice Act. Nurses working in the specializations above must keep up their practice skills and knowledge, which includes familiarity with the rules and regulations that pertain to their profession. Practicing practical nursing is authorized for Licensed Practical Nurses (L.P.N.s). Today’s article looks at the role of nursing. We discuss with certified associated medical providers who consolidate our patients’ information to assess any pain or discomfort they are experiencing. We also inform and guide patients while asking their associated medical provider intricate questions to integrate into their personalized treatment plan to manage the pain. Dr. Jimenez, DC, includes this information as an academic service. Disclaimer.
The Roles In Nursing
The Nurse Practice Act describes practical nursing as “the performance of selected various actions, including the administration of numerous treatments and medications, in the care of the ill, injured, and providing the promotion of wellness, health maintenance and prevention of illnesses while following under the direction of a registered nurse, a licensed physician, osteopathic physician, podiatric physician, or a licensed dentist.” It was revised in 2014 and now teaches broad health and wellness concepts to non-nursing students and the public. The main goal for an RN is to complement the access to health care for individuals in pain or who are dealing with chronic issues. (Cassiani & Silva, 2019)
Many individuals are under the supervision of a registered nurse, doctor, or dentist, individuals who have completed a prelicensure practical nursing education program approved by the Board, a professional nursing education program, and graduate practical nursing students qualifying as professional nursing students; however, licensed practical nurses who have not completed the specified course under Rule 64 B9-12.005, FAC, may perform a limited scope of intravenous therapy. This range consists of:
Intravenous Therapy Within the Scope of the Practical Nurse:
- Calculate and adjust the flow rate of IV therapy.
- Observe and report both subjective and objective signs of various reactions to IV administration to the patient.
- Must inspect the insertion site, change the dressing, and remove the intravenous needle or catheter from the peripheral veins
- Hanging bags or bottles of hydrating fluid.
Intravenous Therapy Outside the Scope of the Practical Nurse:
- Initiation of blood and blood products
- Initiation or administration of cancer chemotherapy
- Initiation of plasma expanders
- Initiation of administration of investigational drugs
- Making IV solution
- IV pushes, except for heparin flushes and saline flushes
It is appropriate for licensed practical nurses to provide treatment for patients undergoing such therapy, even though this rule restricts the practice of licensed practical nurses. 64B-12.005 Requirements for Competency and Knowledge required for the LPN to be qualified to give IV therapy. If the IV Therapy Course Guidelines published by the National Federation of Licensed Practical Nurses Education Department are completed, an LPN may be certified to administer IV therapy. The LPN can take part in further training to provide IV therapy via central lines while supervised by an RN. “The Central Lines. The Board acknowledges that a Licensed Practical Nurse, as defined in subsection 64B9-12.002, FAC, may provide intravenous therapy via central lines under a registered professional nurse’s supervision with the necessary education and training. Four hours of instruction is the minimum required for appropriate education and training. The thirty hours of education for intravenous therapy needed for this rule’s subsection may include four hours of training. At the very least, didactic and clinical practicum instruction in the following areas must be included in the education and training mandated by this subsection:
- Central venous anatomy and physiology
- CVL site assessment
- CVL dressing and cap changes
- CVL flushing
- CVL medication and fluid administration
- CVL blood drawing
- CVL complications and remedial measures
The Licensed Practical Nurse will be evaluated on clinical practice, competency, and theoretical knowledge and practice after completing the intravenous therapy course via central lines. A Registered Nurse must witness the clinical practice assessment and file a proficiency statement on a Licensed Practical Nurse. The Licensed Practical Nurse will be evaluated on clinical practice, competence, and theoretical knowledge and practice. A Registered Nurse who oversees the clinical practice assessment must sign a proficiency statement attesting to the Licensed Practical Nurse’s competence in administering intravenous treatment through central lines. The applicant’s Licensed Practical Nurse personnel file must contain the proficiency statement. 64B9-12.005 code.
Professional nursing is practiced by registered nurses (RNs). The Nurse Practice Act defines this as “the performance of those numerous acts requiring substantial specialized knowledge, judgment, and nursing skill based upon the applied principles of psychological, biological, physical, and social sciences.” Professional nursing goes beyond hands-on care to include nursing diagnosis, planning, supervision, and training other staff members in the theory and execution of any tasks mentioned above. Additionally, nurses must use numerous experiences to assist patients with an understanding of empathy to make them feel comfortable and safe. (Torres-Vigil et al., 2021)
Delegations & Certificates For Nursing
The delegation of responsibilities to another healthcare provider or a competent unlicensed individual is permitted by the Florida Nurse Practice Act. When assigning a task or activity, the registered nurse (RN) or licensed practical nurse (L.P.N.) must consider appropriateness. They had to consider the possibility of patient injury, the difficulty of the work, the outcome’s predictability or unpredictability, and the resources—including staff and equipment—available in the patient environment. The RN and the LPN may assign tasks outside the supervising or delegating nurse’s scope of practice. These tasks include determining the nursing diagnosis or interpreting nursing assessments, developing the plan of care, establishing the goals of nursing care, and assessing the progress of the care plan. The role of nursing is to promote advocacy and create a direct relationship with patients. (Ventura et al., 2020)
464.0205 Retired Volunteer Nurse Certificate
A retired practical or registered nurse may apply for a retired volunteer certificate from the Board of Nursing to work with underprivileged, impoverished, or critically ill populations. They are directly supervised by a physician, advanced practice registered nurse, registered nurse, director of a county health department, and:
- Provides services under the certificate only in sponsored settings that the Board has approved
- The scope of practice for a certified volunteer is limited to primary and preventive health care by the Board.
A retired volunteer nurse shall not:
- Administer controlled substances
- Supervise other nurses
- Receive monetary compensation
464.012 Advanced Practice Registered Nurse (APRN)
“The Barbara Lumpkin Prescribing Act” was proposed towards the end of 2018. This Act helps many practitioners convert a certificate to a license, and it takes effect on October 1, 2018. This Act established a transition timeline and process for practitioners certified as advanced registered nurse practitioners or clinical nurse specialists as of September 30, 2018, to practice as advanced practice registered nurses (APRNs). Until the department and Board complete the transition from certification to licensure, established under this Act, an advanced registered nurse practitioner who is holding a certificate to practice on September 30, 2018, may continue to practice with all the rights, authorizations, and responsibilities under this licensure section as an advanced practice registered nurse. They may also use the applicable title under s.464.015 after this Act’s effective date.
The Board of Nursing requires the following to establish an APRN license:
- A nurse who wants to become an advanced practice registered nurse must apply to the APRN department, provide documentation that they meet the requirements set out by the Board, and have a valid license to practice professional nursing or an active multistate license to practice professional nursing by s. 464.0095.
- Accreditation by a relevant specialty board. To become a certified nurse in any nursing department and to renew your current state license, you must first obtain this certification. For a duration deemed suitable for preparing for and passing the national certification examination, the Board may, by rule, grant certified registered nurse anesthetists, clinical nurse specialists, certified nurse practitioners, psychiatric nurses, and certified nurse midwives provisional state licensure.
- Completing a master’s program in a clinical nursing specialty field and training in particular practitioner skills. For candidates who will graduate on or after October 1, 1998, paragraph (4)(a) requires completion of a master’s degree program to be eligible for initial certification as a certified nurse practitioner.
The Board of Nursing defines APRN’s role/duties:
- Prescribe, dispense, administer, or order any medication; however, an advanced practice registered nurse is only permitted to prescribe or dispense the controlled substance as specified in s.893.03 if they have completed a master’s or doctoral program that provides training in specialized practitioner skills and leads to a master’s or doctoral degree in clinical nursing.
- Initiate appropriate therapies for certain conditions.
- Performed additional functions as may be determined by rule under s.464.003.
- Order diagnostic tests and physical and occupational therapy.
- Order any medication for administration to a patient in a facility.
Beyond the general duties mentioned in subsection (3), an APRN is qualified to carry out the following tasks within their area of expertise:
- Within the confines of established protocol, the certified nurse practitioner may carry out any or all of the following actions:
- Manage selected medical problems.
- Order physical and occupational therapy.
- Initiate, monitor, or alter therapies for certain acute illnesses.
- To monitor and manage patients with stable chronic diseases.
- Established behavioral problems and diagnoses and made treatment recommendations.
The Stature goes on to define the functions of anesthetists and nurse midwives. Refer to the Statue for more details.
Obtaining & Maintaining Nursing License
A license may be acquired through testing, endorsement, or the Nurse Licensure Compact’s enactment. Upon application and a non-refundable payment fee determined by the Board, the department will grant the necessary license by endorsement to engage in professional or practical nursing to the applicant who can provide proof to the Board that they:
- Possesses a valid license to practice professional or practical nursing in another state or territory in the United States, provided that the requirements for licensure in that state were either more stringent or substantially equivalent to those in Florida when the applicant obtained their original license.
- Fulfills the requirements outlined in s.464.008 for licensing and has passed a state, regional, or national exam that is at least as difficult as the one administered by the department.
- Has spent two of the previous three years actively practicing nursing in a different state, territory, or jurisdiction within the United States without having any action taken against their license by any jurisdiction’s licensing body. Under this paragraph, applicants who obtain a permit must finish a board-approved Florida laws and rules course within six months of receiving their license. After reviewing the findings of the national criminal background check, the applicant will be granted the relevant license by endorsement as soon as the department determines that the applicant has no criminal history.
It will be assumed that any exams and requirements from other US states and territories are roughly the same or more demanding than those from this state. This assumption will materialize on January 1, 1980. The Board may, however, establish rules designating some states and territories, the qualifications and exams for which shall not be deemed to be substantially similar to those of this state.
When an individual submission of the appropriate application and fees, as well as the successful completion of the criminal background check that is required under subsection (4), an applicant for licensure by endorsement who is relocating to this state due to the official military orders of their spouse with a military connection and who is a member of the Nurse Licensure Compact in another state will have all the requirements satisfied.
The applicant must submit a set of fingerprints to the department on a form and per departmental rules. The applicant must also pay the department a sum equal to the expenses the Department of Health paid for the applicant’s criminal background check. For a statewide criminal history check, the Department of Health will send the applicant’s fingerprints to the Florida Department of Law Enforcement, and the Florida Department of Law Enforcement will forward the fingerprints to the FBI for a nationwide criminal history check. When an applicant satisfies all other requirements for licensure and has no criminal record, the Department of Health will review the results of the criminal history check, issue a license, and refer all other applicants who have a criminal history back to the Board for a decision on whether or not to issue a permit and under what circumstances.
Until the investigation is finished, at which point the requirements of s.464.018 will take effect, the department will not grant an endorsement license to any applicant who is being investigated in another state, jurisdiction, or territory of the United States for an act that would violate this part or chapter 456. After completing all necessary data collection and verification, the department will issue a license within 30 days. It will also develop an electronic applicant notification process and provide electronic notifications upon application receipt and completion of background checks. Suppose the applicant must appear before the Board because of information on their application or because of screening, data gathering, and verification procedures. In that case, the 30-day license issuance time will be extended. The qualifications for licensure by endorsement in this section do not apply to an individual with an active multistate license in another state under s. 464.0095.
Licensure By Examination
Anyone who wants to take the licensing exam to become a registered nurse must apply to the department. The department will assess each candidate who:
- The applicant has fulfilled the requirements by filling out the application form and paying the $150 fee set by the Board. Additionally, they have paid the $75 examination fee set by the Board and the actual cost per applicant to the department for purchasing the exam from the NCSBN (National Council of State Boards of Nursing) or a comparable national organization.
- Possesses enough information as of October 1, 1989, or later, which the department needs to provide to conduct a statewide criminal records correspondence check with the Department of Law Enforcement.
- Possesses a high school diploma or its equivalent, is in good mental and physical health, and has fulfilled the prerequisites for:
- Graduation from an approved program
- Graduation from a pre-licensure nursing education program equivalent to an approved program determined by the Board.
- Graduated on or after July 1, 2009, from an accredited program
- Graduation before July 1, 2009, from a pre-licensure nursing education program whose graduates were eligible for examination.
Completing courses in a professional nursing education program may satisfy the educational criteria for licensing as a licensed practical nurse. Possesses the ability to communicate in English, as assessed by a department exam. Unless rejected by s.464.018, any applicant who passes the exam and has completed the educational requirements listed in subsection (1) is eligible to become a licensed practical nurse or registered professional nurse, as the case may be.
Regardless of the jurisdiction in which the examination is administered, any applicant who fails the test three times in a row will need to finish a remedial course approved by the Board to be eligible for reexamination. The candidate may be permitted to attempt the test up to three times after completing the remedial course before being forced to undertake remediation. After the remedial process, the applicant has six months to petition for a reexamination. By regulation, the Board will set requirements for remedial education.
An applicant who completes an approved program must be enrolled in and complete a board-approved licensure examination preparing course if they choose not to take the license examination within six months of graduation. The applicant cannot use federal or state financial aid to cover any course-related expenses; they are solely responsible for covering them. The Board will set rules for the preparatory courses for licensing exams. Section 464.0095 exempts an individual from the licensure requirements if they currently have an active multistate license in another state (2).
Licensure Upon Enactment of the Nurse Licensure Compact
Florida passed the Nurse Licensure Compact into law. This allows nurses to participate in 26 states’ licensing compacts. The call to remove the burdensome and redundant system of duplicate licensure and to advance public safety and health advantages led to the enactment of this law. The official statement is as follows:
- “This agreement becomes operative and legally binding on December 31, 2018, whichever comes sooner, or on the day it is enacted into law by at least 26 states. Within six months following the implementation date of this compact, any member states that were also parties to the previous Nurse Licensure Compact (“prior compact”) that this compact replaced are considered to have withdrawn from the previous compact.”
Until a party state is withdrawn from the prior compact, each party state to this one shall respect a nurse’s multistate licensure privilege to practice in that party state granted under the preceding compact. Any party state may opt out of the compact by passing a law canceling it. A party state’s departure becomes effective six months after the repealing Act is passed. Any cooperative arrangement, including nurse licensure agreements, between a party state and a nonparty state that complies with the other conditions of this compact remains valid and unaffected by this compact. The party states may alter this contract. Only when it is incorporated into the laws of every party, state a modification to this compact is binding on the party states and becomes effective. Before all party states adopt this compact, representatives of nonparty states to the agreement will be invited to engage in commission activities without being able to vote.
Unlocking Vitality: Chiropractic Wisdom & The Science of Functional Healing-Video

Continuing Nursing Education Requirement
Licenses need to be renewed every biennium or every two years. One contact hour must be completed for each calendar month of the licensure cycle in a given year. The hours stipulated in subsection (1) at the designated times must include the following continuing education courses as a necessary component:
- A 2-hour course in prevention of medical errors must be completed each biennium.
- A 1-hour course in HIV/AIDS in the first biennium only
- A 2-hour course in Florida laws and rules in each biennium
- Effective August 1, 2017, a 2-hour course in recognizing impairment in clinical approach and every other biennium after that.
- On or after January 1, 2019, a 2-hour course on human trafficking and each biennium after that.
- A 2-hour course in domestic violence is required every third biennium.
In addition, the Florida Board of Nursing requires general hours of continuing education to fulfill the requirement of one contact hour for each calendar month of the licensure cycle. These hour requirements are updated on their website. In addition to the courses mentioned above, they currently demand 16 hours of continuing education in general nursing.
Nurse Licensee With Two Licenses & CE Requirements
A licensee with an RN and an LPN license may fulfill CE requirements by completing the necessary RN-specific continuing education. Visit the Board of Nursing website for further information regarding the rules, as mentioned earlier, and the exceptions.
Standards For Continuing Education
Learner Objectives: The objectives should outline the anticipated behavioral outcomes of the learners and be measurable, reachable, and pertinent to the state of nursing practice today. The goals will dictate the curriculum, mode of instruction, and assessment strategy.
Subject Matter: The content must be specifically created to satisfy the participants’ learning needs, levels, and objectives. The information will be arranged logically and incorporate advice from subject-matter experts. Appropriate subject matter for continuing education offerings should include information from one or more of the following. It should represent the learner’s professional educational needs to address the consumer’s health care demands:
- Nursing areas and special health care problems.
- Biological, physical, behavioral, and social sciences.
- Legal aspects of healthcare
- Management/administration of health care personnel and patient care
- Teaching/ learning process of health care personnel and patients
Evaluation: It must be demonstrated in a way that satisfies the Board that participants are given the chance to assess the educational opportunities, delivery strategies, facilities, and resources utilized in the offering. At the end of the learning process, self-directed learning activities—such as computer programs, web-based courses, internet research, and home study—must be used to assess student knowledge. There must be ten questions or more in the assessment. For the learner to be eligible for the contact hours, they must receive an evaluation score of at least 70%. The provider is required to grade the assessment.
References
Cassiani, S. H. B., & Silva, F. (2019). Expanding the role of nurses in primary health care: the case of Brazil. Rev Lat Am Enfermagem, 27, e3245. https://doi.org/10.1590/1518-8345.0000.3245
Licensure/Certification – Florida Nurses Association. (2022). www.floridanurse.org. https://www.floridanurse.org/page/Licensure
Resources – Florida Nurses Association. (2022). www.floridanurse.org. https://www.floridanurse.org/resources/documents/HistoryofFloridaNursesAssociation.doc
Selecting a Nursing Program – Florida Nurses Association. (2022). www.floridanurse.org. https://www.floridanurse.org/page/SelectingaNursingProgram
Torres-Vigil, I., Cohen, M. Z., Million, R. M., & Bruera, E. (2021). The role of empathic nursing telephone interventions with advanced cancer patients: A qualitative study. Eur J Oncol Nurs, 50, 101863. https://doi.org/10.1016/j.ejon.2020.101863
Ventura, C. A. A., Fumincelli, L., Miwa, M. J., Souza, M. C., Wright, M., & Mendes, I. A. C. (2020). Health advocacy and primary health care: evidence for nursing. Rev Bras Enferm, 73(3), e20180987. https://doi.org/10.1590/0034-7167-2018-0987















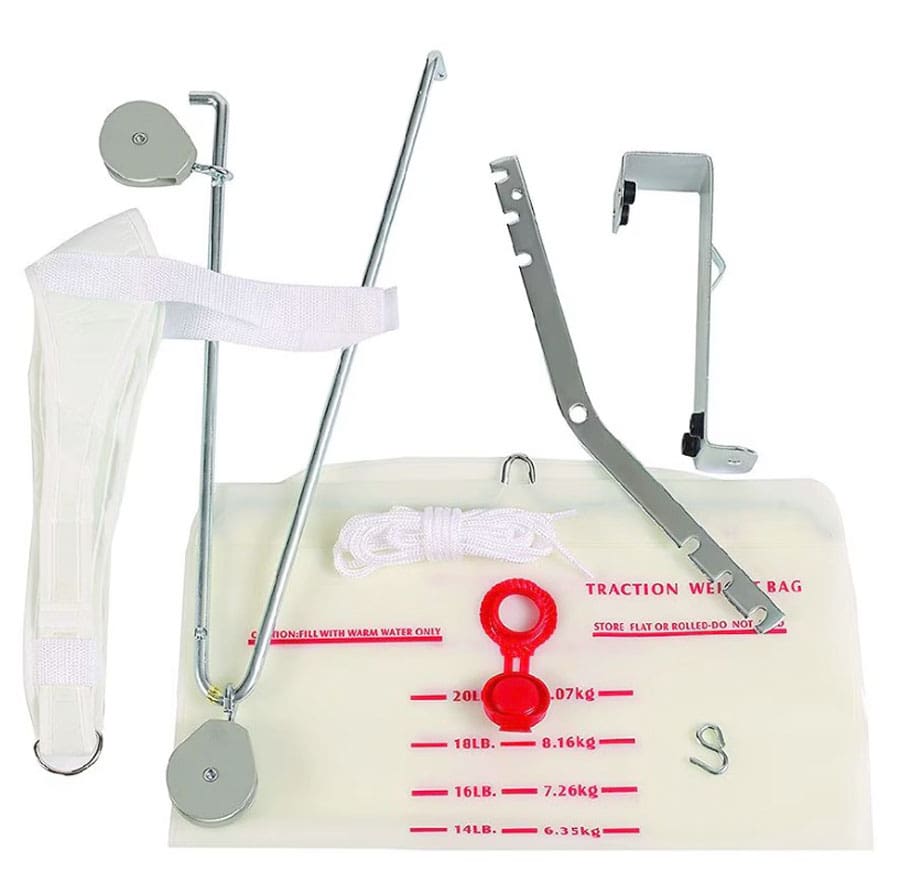 The traction unit must be hung over a door secured to the top and closed.
The traction unit must be hung over a door secured to the top and closed.