Can individuals relieve back pain by incorporating core strength training to reduce pain and discomfort in their lower backs?
Table of Contents
Introduction
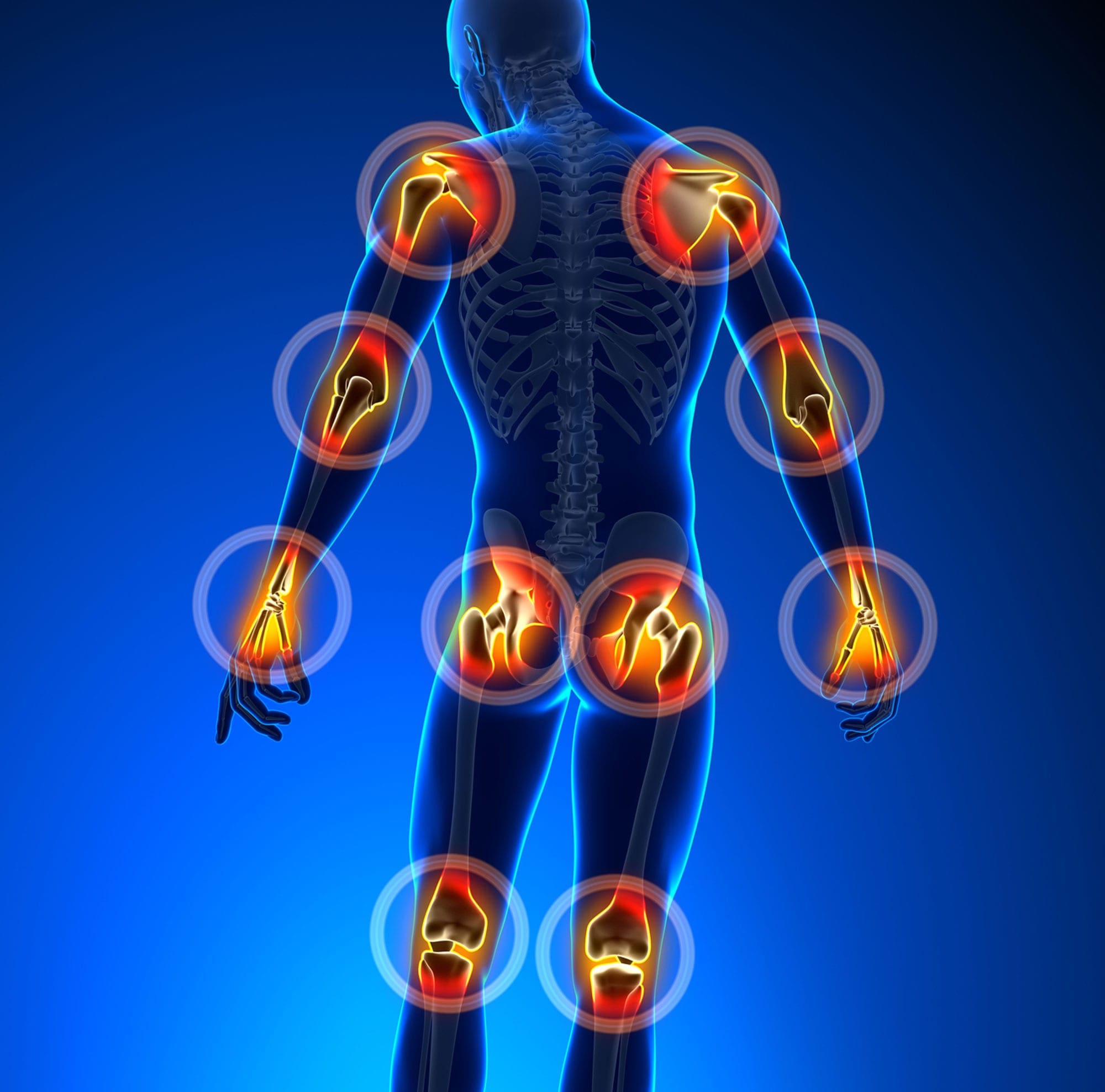
Many individuals worldwide have dealt with back issues that make it difficult to complete any task that they are doing. Many often feel pain and discomfort radiating from the three sections of the back and can radiate from the neck, shoulders, and hips. When these areas of the musculoskeletal system are being affected, it can lead to a life of pain and chronic conditions that cause overlapping risk profiles. At the same time, some causes of back pain often correlate with environmental factors and weak core muscles. When a person is dealing with weak core muscles, they will experience instability and pain when they are mobile, leading to back pain. In today’s article, we look at what the core muscles are, how they are connected to back pain, and how strengthening them can reduce the effects of back pain. We discuss with certified medical providers who inform our patients how strengthening the core muscles can reduce back pain. While asking informed questions to our associated medical providers, we advise patients to incorporate various core strengthening exercises to prevent overlapping risk profiles correlated with back pain. Dr. Alex Jimenez, D.C., encompasses this information as an academic service. Disclaimer.
What Are The Core Muscles?
Do you feel a constant ache or pain in your back after lifting or carrying objects in a hunched position? Do you experience muscle weakness in your torso that you can’t stay in a plank position for a few seconds? Or do you experience radiating pain from your lower back to your leg? The core muscles are a group of muscles wrapped around the torso like a support belt that helps with stability, balance, and protecting the lumbar from injuries. The core muscles are found in the lower body’s front, back, and sides. At the same time, the core muscles can help generate intrabdominal pressure while moving the vertebral column. (Flynn & Vickerton, 2024) In the core muscles, the transverse abdominis muscle or the seatbelt muscle. This muscle works with the inspiratory muscles through elastic loading to evoke transversus expiratory activity when breathing and functioning in motion. (De Troyer et al., 1990)
Core Muscles & Back Pain
The core muscles, especially the transverse abdominis muscles, are often overlooked as many individuals frequently deal with numerous factors that cause low back pain. Common core muscles are associated with back pain because environmental factors can neglect the transverse abdominis muscles. Fatigue in the core muscles can cause repetitive asymmetric loading on the spine, which enhances susceptibility to back pain and other injuries. (Zemkova & Zapletalova, 2021) Since back pain is a multifactorial condition that is one of the leading causes of hospital visits and socio-economic issues, many individuals start to neglect the core muscles over time, causing them to be weak. Some symptoms correlated with weak core muscles include:
- Muscle weakness.
- Numbness in the lower extremities.
- Alterations in the truck movement when standing. (Wattananon et al., 2020)
When this happens, many people start looking for treatment to reduce their back pain and help strengthen their core muscles.
Discover The Benefits Of Chiropractic Care- Video

Strengthening Core Muscles
Before people reduce their back pain and return to their daily routine, they would have to be assessed by a pain specialist like a chiropractor to assess fully what environmental factors are causing the back pain. After the assessment, a chiropractor can work with a physical therapist to reduce back pain and strengthen the core muscles to prevent back pain from returning. When it comes to core strengthening exercises, they focus on either the deep or superficial muscles of the torso, which might produce different effects on lumbar motion. (Puntumetakul et al., 2021) Additionally, core stability exercises can reduce pain in the back and disability reduction and improve a person’s quality of life. (Kanwal et al., 2021) Engaging the muscles through core strengthening exercises can help achieve optimal strength with twisting and side-bending movements to reduce back pain.
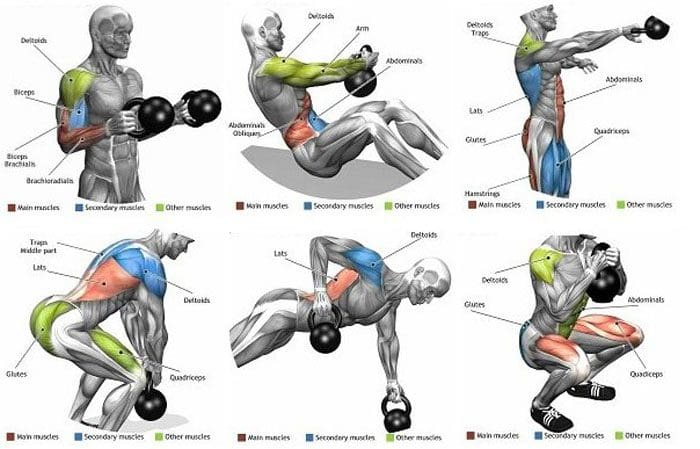
Pay Attention To Engaged Core Muscles
However, individuals need to pay attention to engaging their core muscles while maintaining a neutral spine position for stability and preventing back pain. (Cigdem Karacay et al., 2022) This allows individuals to be consistent with strengthening their core and to commit to short workouts incorporated as part of not only their routine but also as part of their customized treatment plan. When it comes to reducing back pain, it is important to ensure that the core muscles are engaged to help build strength and stability, decrease back pain, and improve functionality. When people start strengthening their core muscles, they will be able to be more mindful about how to present themselves and live healthier lives.
References
Cigdem Karacay, B., Sahbaz, T., Gurtekin, B., Yildiz, S., & Ozcan, E. (2022). Effectiveness of whole-body vibration exercise and core stabilization exercise in chronic non-specific low back pain: A randomized-controlled study. Turk J Phys Med Rehabil, 68(2), 184-194. https://doi.org/10.5606/tftrd.2022.7060
De Troyer, A., Estenne, M., Ninane, V., Van Gansbeke, D., & Gorini, M. (1990). Transversus abdominis muscle function in humans. J Appl Physiol (1985), 68(3), 1010-1016. https://doi.org/10.1152/jappl.1990.68.3.1010
Flynn, W., & Vickerton, P. (2024). Anatomy, Abdomen and Pelvis: Abdominal Wall. In StatPearls. https://www.ncbi.nlm.nih.gov/pubmed/31869113
Kanwal, S., Yaqoob, I., Shakil-Ur-Rehman, S., Ghous, M., Ghazal, J., & Namroz, N. (2021). Effects of core muscle stability on low back pain and quality of life in post-menopausal women: A comparative study. J Pak Med Assoc, 71(1(A)), 37-40. https://doi.org/10.47391/JPMA.151
Puntumetakul, R., Saiklang, P., Tapanya, W., Chatprem, T., Kanpittaya, J., Arayawichanon, P., & Boucaut, R. (2021). The Effects of Core Stabilization Exercise with the Abdominal Drawing-in Maneuver Technique versus General Strengthening Exercise on Lumbar Segmental Motion in Patients with Clinical Lumbar Instability: A Randomized Controlled Trial with 12-Month Follow-Up. Int J Environ Res Public Health, 18(15). https://doi.org/10.3390/ijerph18157811
Wattananon, P., Sinsurin, K., & Somprasong, S. (2020). Association between lumbopelvic motion and muscle activation in patients with non-specific low back pain during forward bending task: A cross-sectional study. Hong Kong Physiother J, 40(1), 29-37. https://doi.org/10.1142/S1013702520500043
Zemkova, E., & Zapletalova, L. (2021). Back Problems: Pros and Cons of Core Strengthening Exercises as a Part of Athlete Training. Int J Environ Res Public Health, 18(10). https://doi.org/10.3390/ijerph18105400