Table of Contents
Platelet-Rich Plasma (PRP) Therapy: A Powerful Tool for Healing Sports Injuries Faster
Sports injuries happen fast. One wrong move on the field or in the gym can tear a muscle, strain a ligament, or inflame a tendon. For years, people relied on rest, ice, and pain pills to get better. Today, a natural treatment called platelet-rich plasma therapy, or PRP therapy, is changing how injuries heal. This method uses the patient’s own blood to speed up recovery without surgery. It helps repair damaged tissue and gets people back to their favorite activities sooner.

PRP therapy expedites the healing process in sports injuries by injecting a concentrated solution of the patient’s own platelets directly into damaged tissue. This process releases growth factors that enhance tissue repair, reduce inflammation, and shorten recovery periods. It is frequently employed to treat osteoarthritis, muscle injuries, ligament strains, and chronic tendinitis. Many athletes and active adults now choose PRP because it works with the body’s natural repair system instead of fighting against it.
What Is Platelet-Rich Plasma Therapy and How Does It Work?
Platelets are tiny cells in your blood that help stop bleeding and start healing. In PRP therapy, doctors take a small sample of your blood and spin it in a machine called a centrifuge. This step concentrates the platelets, so the solution has three to five times as many platelets as normal blood. The result is a rich plasma full of healing signals.
When the doctor injects this PRP into the injured spot, the platelets get to work right away. They release growth factors—special proteins that tell cells to grow and repair. These factors also reduce swelling and increase blood flow to the area. Over time, the body builds stronger tissue in place of the damaged parts. Studies show this natural boost can cut healing time in half for some injuries.
Here is how the process breaks down in simple steps:
- A small amount of blood is drawn from your arm, just like a regular lab test.
- The blood spins in the centrifuge for about 15 minutes to separate the PRP.
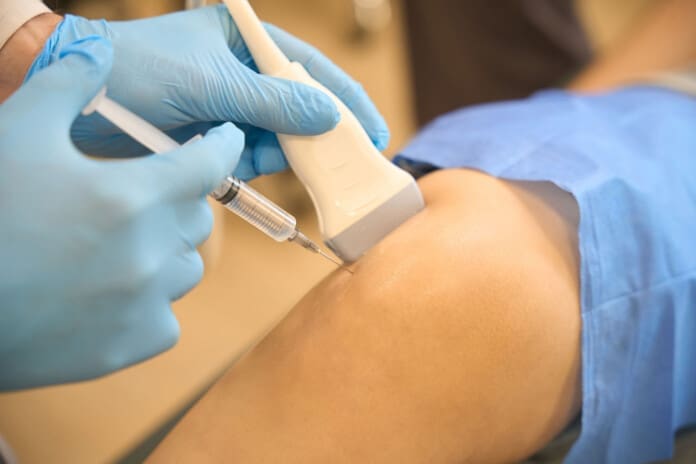
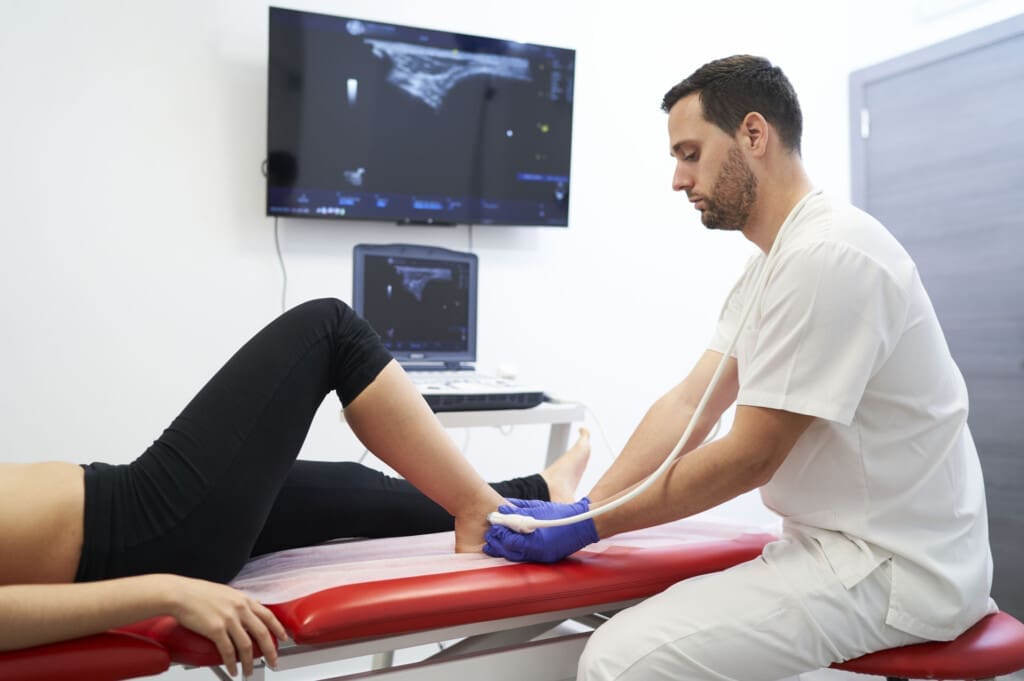
- The doctor uses an ultrasound to guide the injection straight into the exact damaged spot.
- The whole visit usually takes less than an hour, and you go home the same day.
This method avoids drugs or foreign materials because it comes from your body. That means almost no risk of rejection or allergic reaction.
Common Sports Injuries That PRP Therapy Treats
PRP shines when it comes to treating soft-tissue problems that slow athletes down. Doctors use it for many common issues that do not always need an operation. Ligaments, tendons, and muscles are repaired, and pain is alleviated through platelet-rich plasma (PRP) therapy.
Here are the main conditions. PRP helps:
- Osteoarthritis: The cartilage in the knees, hips, or shoulders wears down over time. PRP injections reduce pain and help the joint move better by calming inflammation.
- Muscle injuries: Strains or tears from sudden sprints or lifts heal faster when PRP brings growth factors to rebuild muscle fibers.
- Ligament strains: These tough bands that hold bones together often stretch or tear in sports. PRP speeds up scar tissue formation during repair.
- Chronic tendinitis: Tendons such as the Achilles tendon or the rotator cuff can become irritated by repeated motion. PRP helps reduce ongoing swelling and promotes fresh, healthy tendon growth.
Other problems, such as meniscus tears in the knee or sciatica from back strain, also respond well. Athletes who play basketball, soccer, or tennis, or who run long distances, often see significant improvements.
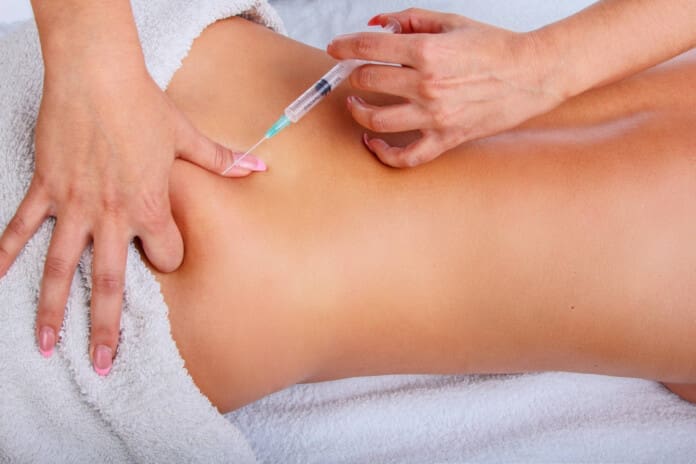
The PRP Injection Procedure: What to Expect
The treatment feels straightforward. First, the medical team cleans the skin and may numb the area with a local spray or shot. Then the ultrasound-guided injection goes in. Ultrasound lets the provider see the needle on a screen so it lands in the perfect spot every time.
Most people feel only mild pressure during the shot. The injection site may experience transient, short-term pain or soreness during the procedure. This discomfort usually fades within a day or two. Doctors tell patients to skip heavy exercise for 48 hours but encourage gentle walking to keep blood moving.
Some clinics combine PRP with other steps on the same visit. For example, a quick chiropractic adjustment can align the joints while PRP begins working within the tissue. Follow-up visits check progress, and many patients need two or three injections spaced a few weeks apart for the best results.
Key Benefits of PRP for Faster Recovery
The biggest win with PRP is how quickly it gets people moving again. Traditional rest can take months, but PRP shortens that timeline. Growth factors jump-start repair, so damaged areas rebuild stronger and with less scar tissue.
Here are the top benefits athletes notice:
- Tissue repair: New cells grow faster, so muscles, tendons, and ligaments regain strength.
- Less inflammation: Swelling drops, which means less stiffness and pain.
- Shorter recovery periods: Many return to training within weeks rather than months.
- Pain relief: The same healing process eases discomfort without relying on pills.
- Non-surgical option: Avoid the risks and downtime associated with surgery.
Real-world examples back this up. Runners with Achilles tendinitis often resume training sooner. Basketball players with knee ligament issues report better stability on the court. Even weekend warriors who twist an ankle find they can hike or bike again without constant aches.
An Integrative Clinic Approach Makes PRP Even Better
PRP works best when it is part of a bigger plan. An integrative clinic that employs specialized APRNs and other providers offers a comprehensive, non-surgical approach to injury care, including ultrasound-guided injections, functional medicine to optimize healing, and structural care.
Clinics like Injury Medical Clinic PA in El Paso, Texas, follow this model. Board-certified APRNs and chiropractors team up to treat the whole person. Ultrasound ensures precise PRP placement. Functional medicine examines nutrition, hormones, and lifestyle to identify and remove anything that slows healing. Structural care uses gentle adjustments to keep the spine and joints aligned so the repaired tissue stays strong.
Dr. Alexander Jimenez, DC, APRN, FNP-BC, leads this kind of care. His clinical observations show that combining PRP with chiropractic and functional nutrition leads to faster tissue repair and fewer setbacks. He notes that PRP promotes blood flow and collagen remodeling, helping patients with meniscus tears or sciatica regain function without surgery. Dr. Jimenez emphasizes root-cause healing—fixing diet, stress, and movement patterns—so the body stays healthy long after the injection. Patients in his practice often report feeling stronger and more stable than before the injury.
This team approach means the PRP does not work alone. Physical therapy builds strength, nutrition plans fuel cell growth, and regular check-ins catch problems early. The result is a complete recovery plan tailored to each person’s body and goals.
What Patients Say and What Science Shows
Many people share success stories after PRP. One soccer player with a hamstring strain was back on the field in four weeks instead of eight. A golfer with tennis elbow could swing without pain after two treatments. These outcomes match what medical studies report. Research from top centers shows PRP increases the number of reparative cells and cuts pain while improving daily function.
Side effects stay mild. The most common side effect is temporary soreness at the injection site. Serious issues are very rare because the material comes from the patient’s own blood. Doctors advise avoiding anti-inflammatory pills for a short time before and after to allow platelets to do their job fully.
Why PRP Is Growing in Popularity for Active Lifestyles
In 2025 and beyond, athletes continue to look for ways to stay in the game longer. PRP fits perfectly because it is safe, natural, and effective. It helps professional players return to competition sooner and lets everyday people keep enjoying hobbies without long breaks. Clinics that blend PRP with advanced tools such as functional testing and structural realignment deliver the best results.
Dr. Jimenez and teams like his continue to track patient progress. Their observations highlight how PRP plus integrative care not only heals the injury but also prevents future problems by improving overall body balance.
Final Thoughts on Choosing PRP Therapy
PRP therapy offers a smart, body-friendly way to handle sports injuries. It turns your blood into a healing powerhouse that repairs ligaments, tendons, and muscles while easing pain. When paired with expert guidance from specialized providers, the results can be life-changing. If you deal with ongoing joint pain, a stubborn strain, or slow-healing tendinitis, talk to a clinic that offers ultrasound-guided PRP and full-body support. Recovery does not have to mean sitting on the sidelines. With PRP and the right care team, you can get back to doing what you love—faster and stronger than before.

References
Platelet-rich plasma (PRP) injections. (n.d.). Penn Medicine.
Platelet-rich plasma (PRP) injections in sports. (n.d.). Yale Medicine.
Dr. Alexander Jimenez DC, APRN, FNP-BC, IFMCP, CFMP, ATN. (2026). LinkedIn.
Injury specialists. (n.d.). Dr. Alexander Jimenez.
Platelet-rich plasma (PRP) treatment. (n.d.). Johns Hopkins Medicine.
PRP injections. (n.d.). Hospital for Special Surgery.