Identifying the delayed symptoms that auto accident survivors may encounter is essential. Stay informed to ensure your health and safety.
Table of Contents
Introduction
Both the body and the psyche may be severely affected by auto accidents, even little ones. Some injuries may show up days, weeks, or months later, while others may be seen right away. It is possible to greatly enhance rehabilitation and quality of life by identifying these delayed symptoms, comprehending their effects, and knowing how to react. This article looks at seven typical delayed symptoms, describes what to do while the symptoms are gone, talks about how it affects the body and day-to-day activities, and looks at successful therapies such chiropractic adjustments.
Seven Common Delayed Symptoms
Delayed symptoms often arise due to the body’s initial adrenaline surge, which can mask pain, or because soft tissue injuries take time to manifest. Here are seven symptoms to watch for:
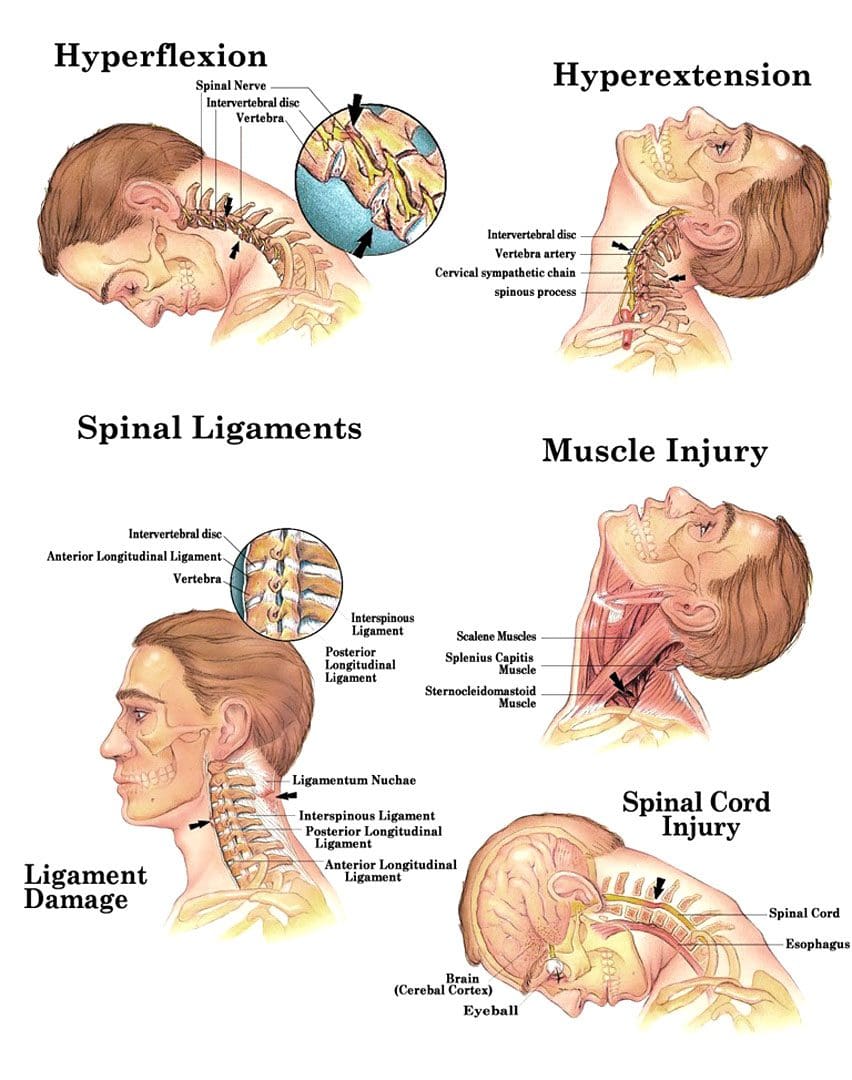
- Neck Pain or Stiffness: Whiplash, a common injury resulting from rear-end collisions, can cause neck pain, stiffness, or a reduced range of motion. Symptoms can emerge days or weeks after the accident. This common injury causes sudden biphasic movements, thus leading to injuries to the bony, muscular, and ligamentous structures of the body. (Alektoroff & Papanagiotou, 2021)
- Headaches: Post-traumatic headaches, often linked to whiplash or mild traumatic brain injury, may start days later and range from tension-type to migraines. These cause the individual to have increased pain sensitivity and cervical musculoskeletal impairments. (Di Antonio et al., 2023)
- Back Pain: Strains, sprains, or herniated discs in the lower or upper back may not cause immediate discomfort but can develop as inflammation builds. Additionally, back pain is associated with impaired movement coordination, which can affect the body’s sensory function. (Delitto et al., 2012)
- Numbness or Tingling: Nerve damage or compression, such as from a pinched nerve or herniated disc; these musculoskeletal issues can lead to tingling or numbness in the arms, legs, or hands.
- Fatigue or Sleep Issues: Physical trauma or stress from the accident can disrupt sleep patterns, leading to chronic fatigue or insomnia over time.
- Cognitive or Emotional Changes: Symptoms like difficulty concentrating, memory problems, anxiety, or irritability may indicate a concussion or post-traumatic stress.
- Joint Pain or Swelling: Joint injuries, such as those to the shoulders or knees, may cause delayed swelling, stiffness, or pain due to inflammation or damage to the cartilage.
What to Do During the Delay Period
The period before symptoms appear is critical for protecting your health and legal rights. Here are key steps to take:
- Seek Medical Evaluation: Even if a person feels fine, visiting a healthcare provider within 24–72 hours is crucial. They can perform a thorough exam, order imaging (e.g., X-rays or MRIs), and document latent injuries.
- Monitor Your Health: Keep a daily journal of physical and mental changes, no matter how minor. Note pain, discomfort, or mood shifts to help identify patterns.
- Avoid Strenuous Activity: Individuals should refrain from heavy lifting, intense exercise, or activities that could exacerbate underlying injuries, such as running or participating in contact sports.
- Document the Accident: Individuals should take photos of everything, including the accident scene, vehicle damage, and any visible injuries that may have occurred during the accident. They should also collect witness statements and file reports with the police for insurance and legal purposes within the time frame of the accident.
- Consult a Specialist: If symptoms emerge or your primary provider recommends it, schedule appointments with specialists, such as chiropractors, neurologists, or orthopedic doctors.
- Follow Up Regularly: Schedule follow-up visits to track your condition, as some symptoms may take several weeks to appear.
- Notify Your Insurance: Make sure to report the accident to the insurance company promptly, but avoid giving detailed statements about your health until you have been fully evaluated.
Car Accident Injury Rehabilitation- Video

Impact on Quality of Life & the Body
Delayed symptoms can significantly affect both physical health and daily life. Physically, untreated injuries may worsen, leading to chronic conditions. For example:
- Musculoskeletal Damage: Whiplash or back injuries can lead to muscle spasms, reduced mobility, or chronic pain if left untreated.
- Neurological Effects: Concussions or nerve compression may impair cognitive function, balance, or sensation, complicating daily tasks.
- Inflammation and Scarring: Soft tissue injuries can lead to prolonged inflammation or the formation of scar tissue, which can limit flexibility and cause discomfort. Additionally, chronic inflammation, when left untreated, can lead to joint damage and tenderness if there are pre-existing conditions like rheumatoid arthritis. (Gessl et al., 2021)
Quality of life often suffers as a result. Chronic pain or fatigue can hinder work performance, leading to lost income or job stress. Sleep disturbances and emotional changes, like anxiety or depression, may strain relationships or reduce social engagement. Simple activities, such as driving, exercising, or sitting for extended periods, may become painful or difficult, which can lower overall well-being.
Treatment Options: Chiropractic Care & More
Treating delayed symptoms requires a comprehensive approach tailored to the injury. Below are effective treatments with a focus on chiropractic care:
- Chiropractic Care: Chiropractors specialize in diagnosing, assessing, and treating musculoskeletal injuries, especially those involving the spine. They use spinal adjustments, manipulations, and soft tissue therapies to:
- Restore joint mobility and alignment to reduce pain from whiplash or back injuries. (Stephen Dies, 1992)
- Relieve nerve compression to address numbness or tingling.
- Chiropractic care promotes natural healing by improving blood flow and reducing inflammation.
- Regular chiropractic sessions can prevent chronic pain and improve recovery outcomes.
- Physical Therapy: Targeted exercises and stretches strengthen muscles, improve flexibility, and restore range of motion. Therapists may use heat, ice, or ultrasound to relieve pain. To that point, physical therapy can improve the individual’s body function and reduce disability. (Hon et al., 2021)
- Pain Management: Over-the-counter medications (e.g., ibuprofen) or prescription drugs can reduce inflammation and pain. In severe cases for pain management, corticosteroid injections may be recommended.
- Massage Therapy: This complements chiropractic care by relaxing tight muscles, reducing spasms, and improving circulation, especially for neck or back pain.
- Cognitive or Psychological Therapy: For concussion-related symptoms or emotional distress, cognitive behavioral therapy (CBT) or counseling can address anxiety, memory issues, or PTSD.
- Lifestyle Adjustments: Incorporating rest, a balanced diet, and stress management techniques (e.g., meditation or yoga) supports recovery and reduces fatigue.
- Medical Interventions: In rare cases, surgery may be needed for severe injuries like herniated discs or fractures. Consult an orthopedic specialist for evaluation.
Conclusion
After an automobile accident, delayed symptoms might be unexpected, but they can be lessened with prompt action and appropriate care. By identifying symptoms such as headaches, neck discomfort, or cognitive problems, getting medical attention quickly, and implementing therapies like chiropractic adjustments, you can always safeguard your health and well-being. To restore strength and well-being, be proactive by keeping an eye on your symptoms, heeding your doctor’s recommendations, and making your recovery a top priority. For tailored medical advice on your health and well-being, generally speaking, you should always speak with a healthcare provider.
Injury Medical Chiropractic & Functional Medicine Clinic
We associate certified medical providers who understand the importance of assessing individuals with pain-like delayed symptoms affecting their musculoskeletal system when involved in an auto accident. When asking important questions to our associated medical providers, we advise patients to incorporate customized treatment plans for their pain correlated with musculoskeletal issues after being involved in an auto accident to promote recovery. Dr. Alex Jimenez, D.C., utilizes this information as a professional academic service. Disclaimer
References
Alektoroff, K., & Papanagiotou, P. (2021). [Whiplash injury of the cervical spine]. Radiologe, 61(8), 710-713. https://doi.org/10.1007/s00117-021-00877-5 (Schleudertrauma der Halswirbelsaule.)
Delitto, A., George, S. Z., Van Dillen, L., Whitman, J. M., Sowa, G., Shekelle, P., Denninger, T. R., & Godges, J. J. (2012). Low Back Pain. Journal of Orthopaedic & Sports Physical Therapy, 42(4), A1-A57. https://doi.org/10.2519/jospt.2012.42.4.a1
Di Antonio, S., Arendt-Nielsen, L., & Castaldo, M. (2023). Cervical musculoskeletal impairments and pain sensitivity in migraine patients. Musculoskelet Sci Pract, 66, 102817. https://doi.org/10.1016/j.msksp.2023.102817
Gessl, I., Popescu, M., Schimpl, V., Supp, G., Deimel, T., Durechova, M., Hucke, M., Loiskandl, M., Studenic, P., Zauner, M., Smolen, J. S., Aletaha, D., & Mandl, P. (2021). Role of joint damage, malalignment and inflammation in articular tenderness in rheumatoid arthritis, psoriatic arthritis and osteoarthritis. Ann Rheum Dis, 80(7), 884-890. https://doi.org/10.1136/annrheumdis-2020-218744
Hon, S., Ritter, R., & Allen, D. D. (2021). Cost-Effectiveness and Outcomes of Direct Access to Physical Therapy for Musculoskeletal Disorders Compared to Physician-First Access in the United States: Systematic Review and Meta-Analysis. Phys Ther, 101(1). https://doi.org/10.1093/ptj/pzaa201
Stephen Dies, J. W. S. (1992). Chiropractic treatment of patients in motor vehicle accidents: a statistical analysis †. J Can Chiropr Assoc., 36(3), 139-145. https://pmc.ncbi.nlm.nih.gov/articles/PMC2484939/















 Common Causes Of Whiplash
Common Causes Of Whiplash