Table of Contents
Physical Therapy for Motor Vehicle Accident Recovery: A Comprehensive Guide
Motor vehicle accidents (MVAs) can have a profound impact on an individual’s physical and mental well-being, often resulting in injuries that require extensive rehabilitation. From whiplash to nerve damage, the consequences of these accidents can lead to chronic pain, mobility issues, and posture problems if not properly addressed. Physical therapy plays a critical role in helping MVA victims recover by restoring function, reducing pain, and preventing long-term complications. This blog post examines the impact of MVAs on the body, the significance of personalized physical therapy treatment plans, and the expertise of professionals like Dr. Alexander Jimenez, a renowned chiropractor and nurse practitioner in El Paso, Texas, who specializes in treating injuries related to MVAs. With a focus on evidence-based interventions, this guide aims to provide high school students and their families with a clear understanding of how physical therapy can aid recovery after a car accident.
The Impact of Motor Vehicle Accidents on the Body
Motor vehicle accidents can cause a wide range of injuries, from minor soft tissue damage to severe musculoskeletal trauma. The sudden force of a collision can result in indirect trauma, where the body experiences stress and strain without direct impact. Common injuries include:
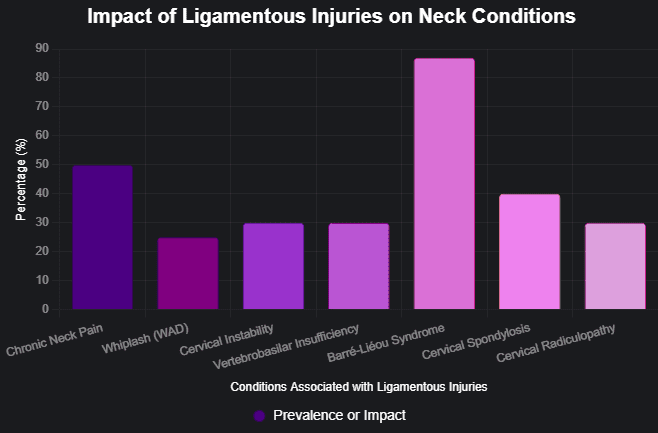
- Back and Neck Pain: Whiplash, a common MVA injury, occurs when the head is forcefully jerked forward and backward, straining the neck’s muscles, ligaments, and tendons. This can lead to chronic neck and upper back pain if not treated promptly.
- Nerve Damage: The force of an accident can compress or irritate nerves, particularly in the spine, leading to symptoms like tingling, numbness, or radiating pain (e.g., sciatica).
- Mobility and Flexibility Issues: Injuries to muscles, ligaments, or joints can reduce range of motion, making everyday movements painful or difficult to perform.
- Posture Problems: Misalignments caused by trauma, such as forward head posture or pelvic tilt, can develop over time, exacerbating pain and dysfunction.
- Musculoskeletal Joint Pain: The stress of an MVA can contribute to joint inflammation, stiffness, or degenerative conditions like arthritis if left untreated.
These injuries often have a cascading effect, where initial trauma leads to compensatory movements that strain other parts of the body. For example, a person with lower back pain may alter their gait, which can put additional stress on their knees or hips. Dr. Alexander Jimenez, a leading expert in MVA-related injuries, states that the musculoskeletal system is highly interconnected, and untreated injuries can lead to chronic conditions that negatively impact overall health and quality of life (Jimenez, 2025).
Why Physical Therapy Is Essential
Physical therapy is a non-invasive, evidence-based approach to treating injuries related to motor vehicle accidents (MVAs). It focuses on restoring mobility, alleviating pain, and preventing long-term complications through targeted exercises and therapeutic interventions. Unlike medication or surgery, physical therapy addresses the root cause of pain and dysfunction, promoting natural healing. According to Texas Physical Therapy Specialists, a personalized treatment plan is critical because each patient’s injuries and recovery needs are unique (Texas Physical Therapy Specialists, n.d.).
Physical therapists use a combination of modalities, exercises, and manual techniques to help patients regain function. These include:
- Stretching and Range-of-Motion Exercises: To improve flexibility and reduce stiffness.
- Strengthening Exercises: To rebuild muscle strength and support injured joints.
- Manual Therapy: Hands-on techniques like joint mobilization or soft tissue massage to relieve pain and restore mobility.
- Pain-Relieving Therapies: Modalities such as ultrasound, electrical stimulation, or hot/cold therapy to reduce inflammation and discomfort.
- Therapeutic Interventions: Functional training to improve balance, coordination, and overall physical performance.
By tailoring these interventions to the patient’s specific injuries, physical therapists can help individuals return to their pre-accident level of function or even surpass it.
Citations
Jimenez, A. (2025). Chiropractic and functional medicine for MVA injuries. Retrieved from https://dralexjimenez.com/
Texas Physical Therapy Specialists. (n.d.). Motor vehicle accident physical therapy. Retrieved from https://texpts.com/primary-services/motor-vehicle-accident/
Common MVA Injuries and Their Long-Term Effects
Whiplash and Neck Pain
Whiplash is one of the most common injuries sustained in MVAs, particularly in rear-end collisions. The rapid motion of the head can strain or tear the soft tissues in the neck, leading to pain, stiffness, and reduced mobility. If not properly treated, whiplash can contribute to chronic neck pain, headaches, and even neurological symptoms like dizziness or tinnitus (Breakthrough Physical Therapy, n.d.).
Dr. Jimenez emphasizes that whiplash can also cause subluxations—misalignments in the spine—that compress nerves and disrupt normal function. These subluxations may not be immediately apparent but can lead to long-term posture problems and joint pain if left unaddressed (Jimenez, 2025).
Back Pain and Sciatica
The lower back is particularly vulnerable in MVAs due to the force transmitted through the spine during a collision. Injuries like herniated discs, muscle strains, or facet joint dysfunction can cause acute or chronic back pain. In some cases, spinal injuries can lead to sciatica, a condition in which the sciatic nerve is compressed, causing radiating pain, numbness, or weakness in the legs. (Synergy Rehab, n.d.).
Dr. Jimenez’s clinical observations underscore the importance of early intervention in preventing the progression of back pain into degenerative conditions. For example, a herniated disc left untreated can lead to spinal stenosis or arthritis, significantly impacting mobility and quality of life. (Jimenez, 2025).
Nerve Damage
Nerve damage from MVAs can result from direct trauma (e.g., a fracture compressing a nerve) or indirect trauma (e.g., inflammation or swelling pressing on nerve roots). Symptoms include tingling, numbness, burning sensations, or muscle weakness. Physical therapy can help reduce inflammation, improve circulation, and promote nerve healing through targeted exercises and modalities. (Rocky Mountain Physical Therapy, n.d.).
Mobility and Flexibility Issues
Injuries to muscles, ligaments, or joints often result in reduced range of motion, making it difficult to perform daily activities like walking, bending, or lifting. Without intervention, scar tissue can form, further limiting flexibility and increasing the risk of re-injury. Physical therapy exercises, such as stretching and range-of-motion activities, are designed to restore flexibility and prevent these complications (OneRehab, n.d.).
Posture Problems
Poor posture is a common consequence of MVA injuries, as individuals may unconsciously adopt compensatory positions to avoid pain. For example, someone with neck pain may tilt their head forward, resulting in a forward head posture that strains the upper back and shoulders. Over time, these postural changes can lead to musculoskeletal joint pain and increase the risk of conditions such as kyphosis or scoliosis. (Jimenez, 2025).
Musculoskeletal Joint Pain
The cumulative effect of MVA injuries can contribute to musculoskeletal joint pain, particularly in the spine, shoulders, and hips. Joint inflammation, cartilage damage, or ligament laxity can result from trauma, leading to conditions like osteoarthritis or tendinitis. Physical therapy helps by strengthening the muscles around affected joints, improving stability, and reducing pain (Benchmark Physical Therapy, n.d.).
Citations
Benchmark Physical Therapy. (n.d.). Motor vehicle accident recovery. Retrieved from https://www.benchmarkpt.com/conditions/motor-vehicle-accident/
Breakthrough Physical Therapy. (n.d.). MVA-related injuries. Retrieved from https://breakthrough-pt.com/conditions/mva-related-injuries/
Jimenez, A. (2025). Posture and musculoskeletal health. Retrieved from https://dralexjimenez.com/
Jimenez, A. (2025). Sciatica and spinal injuries. Retrieved from https://sciatica.clinic/
Jimenez, A. (2025). Chiropractic care for MVA injuries. Retrieved from https://elpasochiropractic.com/
OneRehab. (n.d.). Physical therapy exercises after a car accident. Retrieved from https://onerehab.com/physical-therapy-exercises-after-a-car-accident/
Rocky Mountain Physical Therapy. (n.d.). Post-auto collision recovery. Retrieved from https://rockymountain.urpt.com/conditions/post-auto-collision/
Synergy Rehab. (n.d.). Physical therapy after auto accident. Retrieved from https://synergyrehabinc.com/physical-therapy-after-auto-accident/
The Role of Physical Therapy in MVA Recovery
Physical therapy is a cornerstone of MVA recovery, offering a holistic approach to healing that addresses both symptoms and underlying causes. A physical therapist begins by conducting a thorough evaluation of the patient’s injuries, which may include physical assessments, range-of-motion tests, and imaging studies (e.g., X-rays or MRIs). Based on this evaluation, the therapist develops a personalized treatment plan tailored to the patient’s needs (Apex Orthopedic Sports & Neurology, n.d.).
Key Components of Physical Therapy
-
Stretching and Range-of-Motion Exercises
Stretching exercises help restore flexibility by lengthening tight muscles and reducing stiffness. Range-of-motion exercises, such as shoulder circles or knee bends, help improve joint mobility and reduce the formation of scar tissue. These exercises are often introduced gradually to avoid aggravating injuries. (Sports Physical Therapy, n.d.). -
Strengthening Exercises
Strengthening exercises target weakened muscles to improve stability and support injured areas. For example, core-strengthening exercises can alleviate lower back pain, while resistance band exercises can strengthen the rotator cuff muscles after a shoulder injury. These exercises are critical for preventing re-injury and promoting long-term recovery (Texas Physical Therapy Specialists, n.d.). -
Manual Therapy
Manual therapy techniques, such as joint mobilization, soft tissue massage, or myofascial release, are used to reduce pain, improve circulation, and restore mobility. These hands-on interventions are particularly effective for addressing muscle spasms, joint stiffness, and scar tissue (Bay State Physical Therapy, n.d.). -
Pain-Relieving Therapies
We utilize modalities such as ultrasound, electrical stimulation, or hot and cold therapy to reduce inflammation, alleviate pain, and promote healing. For example, electrical stimulation can stimulate muscle contractions to prevent atrophy, while cold therapy reduces swelling in the acute phase of injury (Rocky Mountain Physical Therapy, n.d.). -
Functional Training
Functional training focuses on improving everyday movements, such as walking, lifting, or climbing stairs. These exercises mimic real-life activities to enhance coordination, balance, and overall physical performance. For example, multi-joint exercises such as squats or lunges enhance lower body strength and stability. (Release Physical Therapy, n.d.). -
Education and Guidance
Physical therapists educate patients on proper body mechanics, posture, and injury prevention strategies. This empowers patients to take an active role in their recovery and maintain their progress after therapy ends (Apex Orthopedic Sports & Neurology, n.d.).
Benefits of Physical Therapy
- Pain Reduction: Physical therapy reduces pain through targeted exercises and modalities, often eliminating the need for long-term medication.
- Improved Mobility: Exercises and manual therapy restore range of motion, allowing patients to perform daily activities with ease.
- Prevention of Long-Term Issues: Early intervention prevents complications like chronic pain, joint degeneration, or postural deformities.
- Non-Invasive Approach: Physical therapy avoids the risks and recovery time associated with surgery.
- Personalized Care: We tailor treatment plans to each individual, ensuring optimal outcomes.
Citations
Apex Orthopedic Sports & Neurology. (n.d.). Physical therapy after a car accident. Retrieved from https://www.apexosn.com/physical-therapy-after-a-car-accident/
Bay State Physical Therapy. (n.d.). Motor vehicle accident injuries. Retrieved from https://baystatept.com/specialties-provided/motor-vehicle-accident-injuries/
Release Physical Therapy. (n.d.). Functional training. Retrieved from https://releasept.com/functional-training/
Rocky Mountain Physical Therapy. (n.d.). Post-auto collision recovery. Retrieved from https://rockymountain.urpt.com/conditions/post-auto-collision/
Sports Physical Therapy. (n.d.). How to start exercising following a motor vehicle accident. Retrieved from https://sportsptcenters.com/how-to-start-exercising-following-a-motor-vehicle-accident/
Texas Physical Therapy Specialists. (n.d.). Motor vehicle accident physical therapy. Retrieved from https://texpts.com/primary-services/motor-vehicle-accident/
Dr. Alexander Jimenez: A Leader in MVA Treatment
Dr. Alexander Jimenez, DC, APRN, FNP-BC, is a board-certified chiropractor and family nurse practitioner based in El Paso, Texas, with over 25 years of experience treating injuries related to motor vehicle accidents (MVAs). His dual licensure allows him to combine the biomechanical expertise of chiropractic care with the diagnostic and therapeutic capabilities of a nurse practitioner, making him uniquely qualified to address the complex needs of MVA victims (Jimenez, 2025).
Clinical Rationale for Advanced Diagnostics
Dr. Jimenez emphasizes the importance of advanced imaging (e.g., X-rays, MRIs, CT scans) and diagnostic assessments in accurately identifying the extent of MVA injuries. For example, an X-ray can reveal fractures or subluxations, while an MRI can detect soft tissue damage or nerve compression. Dual-scope procedures, including motion and static palpation, enable Dr. Jimenez to assess spinal alignment, joint mobility, and muscle tenderness, providing a comprehensive understanding of the patient’s condition.
These diagnostic tools are critical for several reasons:
- Accurate Diagnosis: Advanced imaging ensures that hidden injuries, such as microfractures or disc herniations, are not overlooked.
- Personalized Treatment Plans: Diagnostic assessments guide the development of tailored interventions that address the specific injuries and needs of each patient.
- Legal Documentation: In personal injury cases, detailed diagnostic reports provide evidence of the injury’s severity and its impact on the patient’s life, supporting legal compensation claims (Jimenez, 2025).
Integrating Medical and Legal Needs
In El Paso, personal injury cases often involve complex legal proceedings, as victims seek compensation for medical expenses, lost wages, and pain and suffering. Dr. Jimenez’s expertise serves as a bridge between medical treatment and legal documentation. His clinic, Injury Medical & Chiropractic Clinic, provides detailed medical records, expert testimony, and comprehensive treatment plans that align with the requirements of personal injury cases (Jimenez, 2025).
For example, a patient with whiplash may receive a combination of spinal adjustments, physical therapy, and pain-relieving modalities, with each intervention documented to demonstrate medical necessity. This documentation is critical for attorneys and insurance companies, ensuring that patients receive fair compensation while focusing on their recovery.
Customized Treatment Plans
Dr. Jimenez’s approach to MVA treatment is highly individualized, recognizing that no two injuries are the same. His treatment plans often include:
- Chiropractic Adjustments: To correct spinal misalignments and reduce nerve compression.
- Physical Therapy: Incorporating stretching, strengthening, and functional exercises to restore mobility and strength.
- Functional Medicine: Addressing systemic factors like inflammation or nutritional deficiencies that may impede healing.
- Lifestyle Interventions: Educating patients on posture correction, stress management, and injury prevention (Jimenez, 2025).
By combining these modalities, Dr. Jimenez helps patients achieve optimal recovery while minimizing the risk of long-term complications.
Citations
Jimenez, A. (2025). Advanced diagnostics for MVA injuries. Retrieved from https://dralexjimenez.com/
Jimenez, A. (2025). Chiropractic care for personal injury cases. Retrieved from https://sciatica.clinic/
Jimenez, A. (2025). Integrative treatment for MVA recovery. Retrieved from https://elpasochiropractic.com/
Jimenez, A. (2025). Professional profile. Retrieved from https://www.linkedin.com/in/dralexjimenez/
Jimenez, A. (2025). Functional medicine and chiropractic. Retrieved from https://www.linkedin.com/in/alexander-jimenez-a654a6349/
Sample Physical Therapy Treatment Plan for MVA Injuries
To illustrate how physical therapy is applied in MVA recovery, consider the following sample treatment plan for a patient with whiplash and lower back pain:
Week 1–2: Acute Phase
- Goals: Reduce pain and inflammation, promote healing.
- Interventions:
- Cold Therapy: Apply ice packs to the neck and lower back for 15 minutes, 3–4 times daily, to reduce swelling.
- Gentle Range-of-Motion Exercises: Perform slow neck rotations and pelvic tilts to maintain mobility without aggravating pain.
- Manual Therapy: Soft tissue massage to relieve muscle spasms in the neck and lower back.
- Education: Teach proper posture and body mechanics to avoid further strain (Apex Orthopedic Sports & Neurology, n.d.).
Weeks 3–6: Subacute Phase
- Goals: Improve flexibility, begin strengthening, restore function.
- Interventions:
- Stretching Exercises: Introduce neck and lumbar stretches to improve flexibility (e.g., chin tucks, cat-cow stretch).
- Strengthening Exercises: Begin core and neck strengthening with exercises like planks and isometric neck exercises.
- Manual Therapy: Joint mobilization to restore spinal mobility.
- Modalities: Use electrical stimulation or ultrasound to reduce residual pain (Rocky Mountain Physical Therapy, n.d.).
Weeks 7–12: Rehabilitation Phase
- Goals: Enhance strength, improve functional performance, and prevent re-injury.
- Interventions:
- Functional Training: Incorporate multi-joint exercises like squats, lunges, and step-ups to improve balance and coordination.
- Advanced Strengthening: Use resistance bands or bodyweight exercises to strengthen the core, neck, and back muscles.
- Posture Correction: Practice exercises to correct forward head posture and lumbar lordosis.
- Home Exercise Program: Develop a daily routine for the patient to maintain progress (Release Physical Therapy, n.d.).
Long-Term Maintenance
- Goals: Maintain mobility, prevent recurrences, promote overall health.
- Interventions:
- Regular Exercise: Encourage aerobic activities like walking or swimming to improve cardiovascular health and maintain muscle strength.
- Periodic Check-Ins: Schedule follow-up appointments to monitor progress and adjust the treatment plan as needed.
- Lifestyle Modifications: Promote ergonomic adjustments at work or home to support proper posture (Texas Physical Therapy Specialists, n.d.).
This sample plan demonstrates the progressive nature of physical therapy, starting with pain management and gradually transitioning to functional restoration. The duration of therapy varies depending on the severity of the injuries and the patient’s progress, typically ranging from a few weeks to several months (Georgia Spine & Orthopaedics, n.d.).
Citations
Apex Orthopedic Sports & Neurology. (n.d.). Physical therapy after a car accident. Retrieved from https://www.apexosn.com/physical-therapy-after-a-car-accident/
Georgia Spine & Orthopaedics. (n.d.). Physical therapy after a car accident. Retrieved from https://www.gaspineortho.com/physical-therapy-after-a-car-accident/
Release Physical Therapy. (n.d.). Functional training. Retrieved from https://releasept.com/functional-training/
Rocky Mountain Physical Therapy. (n.d.). Post-auto collision recovery. Retrieved from https://rockymountain.urpt.com/conditions/post-auto-collision/
Texas Physical Therapy Specialists. (n.d.). Motor vehicle accident physical therapy. Retrieved from https://texpts.com/primary-services/motor-vehicle-accident/
The Importance of Early Intervention
Early intervention is critical for preventing the progression of MVA injuries into chronic conditions. Delaying treatment can lead to complications like scar tissue formation, joint degeneration, or nerve damage, which are more difficult to treat. Physical therapy started within days or weeks of an accident can significantly improve outcomes by reducing inflammation, restoring mobility, and preventing compensatory injuries (Synergy Rehab, n.d.).
Dr. Jimenez’s clinical approach emphasizes the importance of prompt evaluation and treatment. His use of advanced imaging and diagnostic assessments ensures that even subtle injuries are identified early, allowing for targeted interventions that prevent long-term disability (Jimenez, 2025).
Tips for Starting Physical Therapy
- Consult a Professional: Work with a licensed physical therapist or chiropractor like Dr. Jimenez to develop a safe and effective treatment plan.
- Start Slowly: Begin with low-impact exercises and gradually increase intensity to avoid aggravating injuries.
- Be Consistent: Follow the prescribed exercise and therapy schedule to achieve optimal results.
- Communicate: Report any pain or discomfort to your therapist so they can adjust the plan as needed (Sports Physical Therapy, n.d.).
Citations
Jimenez, A. (2025). Early intervention for MVA injuries. Retrieved from https://dralexjimenez.com/
Sports Physical Therapy. (n.d.). How to start exercising following a motor vehicle accident. Retrieved from https://sportsptcenters.com/how-to-start-exercising-following-a-motor-vehicle-accident/
Synergy Rehab. (n.d.). Physical therapy after auto accident. Retrieved from https://synergyrehabinc.com/physical-therapy-after-auto-accident/
Conclusion
Motor vehicle accidents can cause a range of injuries, from whiplash and back pain to nerve damage and posture problems, all of which can significantly impact quality of life. Physical therapy provides a non-invasive, personalized approach to recovery, enabling patients to regain mobility, alleviate pain, and prevent long-term complications. Professionals like Dr. Alexander Jimenez in El Paso, Texas, play a vital role in this process, combining advanced diagnostics, chiropractic care, and physical therapy to address both medical and legal needs. By starting physical therapy early and following a customized treatment plan, MVA victims can achieve optimal recovery and return to their daily activities with confidence.
For those in El Paso seeking expert care, Dr. Jimenez’s Injury Medical & Chiropractic Clinic offers comprehensive treatment plans tailored to your unique needs. Contact them at 915-850-0900 or visit https://dralexjimenez.com/ to schedule an appointment.
References
Apex Orthopedic Sports & Neurology. (n.d.). Physical therapy after a car accident. Retrieved from https://www.apexosn.com/physical-therapy-after-a-car-accident/
Bay State Physical Therapy. (n.d.). Motor vehicle accident injuries. Retrieved from https://baystatept.com/specialties-provided/motor-vehicle-accident-injuries/
Benchmark Physical Therapy. (n.d.). Motor vehicle accident recovery. Retrieved from https://www.benchmarkpt.com/conditions/motor-vehicle-accident/
Breakthrough Physical Therapy. (n.d.). MVA-related injuries. Retrieved from https://breakthrough-pt.com/conditions/mva-related-injuries/
Georgia Spine & Orthopaedics. (n.d.). Physical therapy after a car accident. Retrieved from https://www.gaspineortho.com/physical-therapy-after-a-car-accident/
Jimenez, A. (2025). Chiropractic and functional medicine for MVA injuries. Retrieved from https://dralexjimenez.com/
Jimenez, A. (2025). Sciatica and spinal injuries. Retrieved from https://sciatica.clinic/
Jimenez, A. (2025). Chiropractic care for MVA injuries. Retrieved from https://elpasochiropractic.com/
Jimenez, A. (2025). Professional profile. Retrieved from https://www.linkedin.com/in/dralexjimenez/
Jimenez, A. (2025). Functional medicine and chiropractic. Retrieved from https://www.linkedin.com/in/alexander-jimenez-a654a6349/
OneRehab. (n.d.). Physical therapy exercises after a car accident. Retrieved from https://onerehab.com/physical-therapy-exercises-after-a-car-accident/
Release Physical Therapy. (n.d.). Functional training. Retrieved from https://releasept.com/functional-training/
Rocky Mountain Physical Therapy. (n.d.). Post-auto collision recovery. Retrieved from https://rockymountain.urpt.com/conditions/post-auto-collision/
Sports Physical Therapy. (n.d.). How to start exercising following a motor vehicle accident. Retrieved from https://sportsptcenters.com/how-to-start-exercising-following-a-motor-vehicle-accident/
Synergy Rehab. (n.d.). Physical therapy after auto accident. Retrieved from https://synergyrehabinc.com/physical-therapy-after-auto-accident/
Texas Physical Therapy Specialists. (n.d.). Motor vehicle accident physical therapy. Retrieved from https://texpts.com/primary-services/motor-vehicle-accident/