Degenerative disc disease is a health issue which occurs when one or more of the discs found between the vertebrae of the spine break down, causing painful symptoms and other problems. Common symptoms may include pain, tingling sensations, weakness, and numbness. Despite its name, degenerative disc disease is actually not a disease, but rather, a natural process which occurs with aging. The rubbery discs found between the vertebrae function like shock absorbers, allowing the back to flex and bend accordingly. When they wear out, however, they no longer provide as much protection as before.
Table of Contents
Causes
The intervertebral discs also referred to as spinal discs or intervertebral fibrocartilage, provide the padding required between the vertebrae of the spine. The intervertebral discs are an elastic structure made from fibrocartilage tissue. The outer part of the disc is referred to as the annulus fibrosus. The annulus fibrosus is tough and it’s made up of many overlapping layers. The inner part of the disc is referred to as the nucleus pulposus. The nucleus pulposus is soft and gelatinous. The intervertebral discs cushion the stress of the spine, bears weight, and also helps the spine bend and flex.
As people age, repeated daily stresses on the backbone and occasional trauma and/or injuries, including minor, undetected health issues, may ultimately damage the intervertebral discs in the back. Changes caused by damage may include:
- Decreased fluid: The intervertebral disks of a healthy young adult are made up of around 90 percent fluid. With age, the fluid material decreases, causing the disc to become thinner. The distance between each vertebra, in turn, becomes smaller and it makes them even less effective to function as a cushion or shock-absorber.
- Disc structure: Small tears or cracks can become larger in the outer layer of the disc. The soft and gelatinous material from the inner part may push through the disc, causing a bulging or ruptured disc. The disc may break into fragments.
If the vertebrae have less padding between them, the backbone also becomes less stable. To compensate, the human body builds osteophytes, or bone spurs, small bony structures which develop along the edge of bones. These structures can compress or impinge the spinal cord or nerve roots. Other health issues caused by degenerative disc disease includes the breakdown of cartilage or the tissue which cushions the joints, a bulging disc, known as a herniated disc, and a narrowing of the spinal cord, also referred to as spinal stenosis. These changes can cause painful symptoms and lead to fatigue.
Symptoms
Degenerative disc disease can either cause no symptoms or the pain and discomfort may be so severe, it can tremendously affect an individual’s quality of life. This health issue generally aggravates due to injury or trauma to the backbone, however, symptoms can also affect other parts of the human body, depending on the direct location of the degenerative disc disease. The pain and discomfort can range from mild to severe and it may often be debilitating. It may ultimately result in osteoarthritis, with pain and discomfort along with stiffness in the back. Fatigue can generally accompany other symptoms.
If degenerative disc disease affects the low back or the lumbar spine, the pain and discomfort may radiate down the buttocks, hips, and thighs, into the knees and feet. There might also be tingling sensations and numbness, a collection of symptoms known as sciatica, caused due to the compression or impingement of the sciatic nerve. If degenerative disc disease affects the neck or the cervical spine, the pain and discomfort may radiate into the shoulders, arms, and hands. The painful symptoms may worsen when sitting, bending, twisting or lifting. Rest may help provide some pain relief.
Diagnosis
A healthcare professional will ask the patient about their symptoms, including where and when the pain developed as well as whether there are tingling sensations or numbness. The doctor may also need to know which circumstances cause the most painful symptoms and if the patient suffered any injuries and/or aggravated conditions. A physical evaluation may examine pain and discomfort in response to touch or movement, muscle strength, flexibility, and performance, as well as nerve structure and function. The healthcare professional may also order diagnostic tests, such as MRI or CT scans.
Treatment
Treatment for degenerative disc disease might include occupational therapy, physical therapy, chiropractic care, exercise or physical activity, drugs and/or medications, weight loss, and surgery. Medical options include injecting the joints next to the broken disc with steroids and a local anesthetic. Medicines include pain relief medicine, such as Tylenol, and non-steroidal anti-inflammatory medications, or NSAIDs, including ibuprofen. Muscle relaxers and steroids may also be prescribed.
A corset or brace may also offer back support. Patients who don’t respond well to conservative treatment options might require surgery. Furthermore, a patient who develops osteoarthritis, a herniated disc, or spinal stenosis may require a combination of different types of treatment approaches to achieve pain relief. It’s fundamental for a healthcare professional to provide a patient with the proper diagnosis of their symptoms to follow-up with the most appropriate treatment.
Differential Diagnosis of Hip Pain and Discomfort
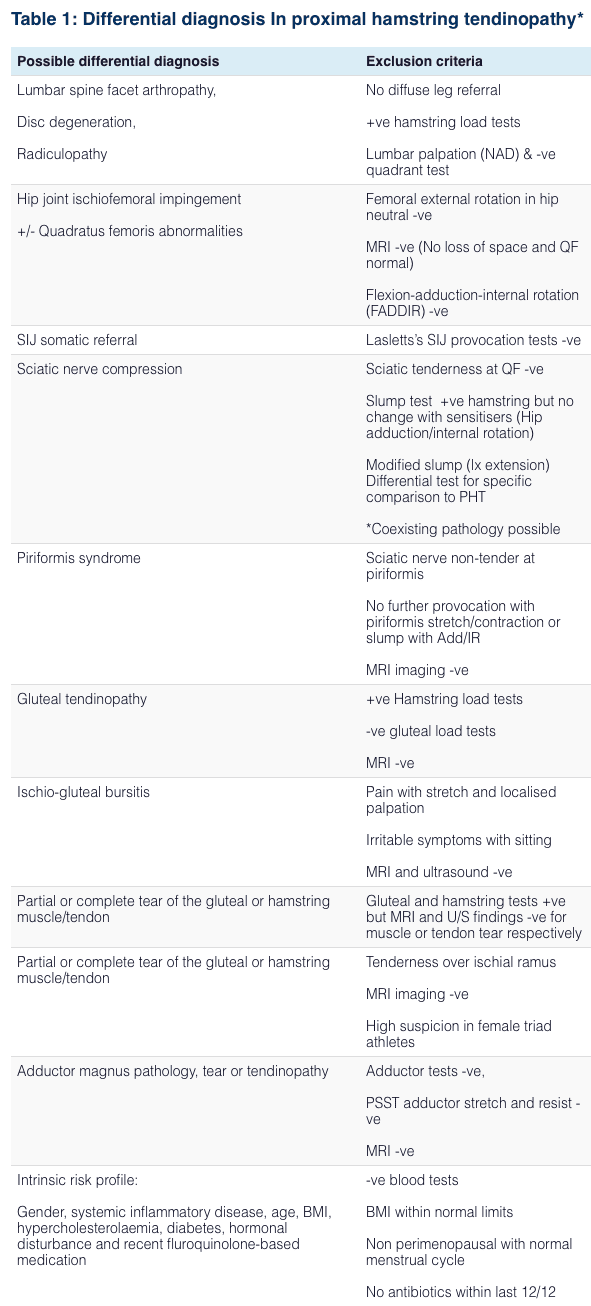

Degenerative disc disease is characterized as the normal, gradual deterioration of the intervertebral discs with age, which may occasionally cause a variety of painful symptoms. Common symptoms associated with degenerative disc disease can include pain and discomfort, tingling sensations, and numbness, similar to sciatica. Painful symptoms may also cause fatigue and other health issues. Nearly everyone’s intervertebral discs will break down over time, however, not everyone will develop painful symptoms. – Dr. Alex Jimenez D.C., C.C.S.T. Insight
Fibromyalgia Magazine
The purpose of the article was to discuss degenerative disc disease and sciatica. Degenerative disc disease is often associated with pain, tingling sensations, and numbness, similar to the symptoms of sciatica. The scope of our information is limited to chiropractic, musculoskeletal and nervous health issues as well as functional medicine articles, topics, and discussions. To further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900 .
Curated by Dr. Alex Jimenez
XYMOGEN’s Exclusive Professional Formulas are available through select licensed health care professionals. The internet sale and discounting of XYMOGEN formulas are strictly prohibited.
Proudly, Dr. Alexander Jimenez makes XYMOGEN formulas available only to patients under our care.
Please call our office in order for us to assign a doctor consultation for immediate access.
If you are a patient of Injury Medical & Chiropractic Clinic, you may inquire about XYMOGEN by calling 915-850-0900.
For your convenience and review of the XYMOGEN products please review the following link.*XYMOGEN-Catalog-Download
* All of the above XYMOGEN policies remain strictly in force.
XYMOGEN’s Exclusive Professional Formulas are available through select licensed health care professionals. The internet sale and discounting of XYMOGEN formulas are strictly prohibited.
Proudly, Dr. Alexander Jimenez makes XYMOGEN formulas available only to patients under our care.
Please call our office in order for us to assign a doctor consultation for immediate access.
If you are a patient of Injury Medical & Chiropractic Clinic, you may inquire about XYMOGEN by calling 915-850-0900.
For your convenience and review of the XYMOGEN products please review the following link.*XYMOGEN-Catalog-Download
* All of the above XYMOGEN policies remain strictly in force.
Additional Topic Discussion: Severe Sciatica
Back pain is one of the most prevalent causes of disability and missed days at work worldwide. Back pain attributes to the second most common reason for doctor office visits, outnumbered only by upper-respiratory infections. Approximately 80 percent of the population will experience back pain at least once throughout their life. Your spine is a complex structure made up of bones, joints, ligaments, and muscles, among other soft tissues. Injuries and/or aggravated conditions, such as herniated discs, can eventually lead to symptoms of sciatica, or sciatic nerve pain. Sports injuries or automobile accident injuries are often the most frequent cause of painful symptoms, however, sometimes the simplest of movements can have these results. Fortunately, alternative treatment options, such as chiropractic care, can help ease sciatic nerve pain, or sciatica, through the utilization of spinal adjustments and manual manipulations, ultimately improving pain relief.
Formulas for Methylation Support
XYMOGEN’s Exclusive Professional Formulas are available through select licensed health care professionals. The internet sale and discounting of XYMOGEN formulas are strictly prohibited.
Proudly, Dr. Alexander Jimenez makes XYMOGEN formulas available only to patients under our care.
Please call our office in order for us to assign a doctor consultation for immediate access.
If you are a patient of Injury Medical & Chiropractic Clinic, you may inquire about XYMOGEN by calling 915-850-0900.
For your convenience and review of the XYMOGEN products please review the following link.*XYMOGEN-Catalog-Download
* All of the above XYMOGEN policies remain strictly in force.
Professional Scope of Practice *
The information herein on "Degenerative Disc Disease and Sciatica" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card