Hiking is a form of exercise accessible to a wide range of physical abilities, which makes it a great outdoor activity for all. The health benefits include improved blood pressure, sleep, and reduced stress and anxiety. However, being out in the elements without conditioning the body can lead to serious injuries and other health issues. Many trails are rough, uneven, and have elevation gain, so even the easiest courses require balance and strength to avoid injury. Hiking training that includes strength, cardio, and practice will help condition the body to allow the trip to be more enjoyable and safe.

Table of Contents
Hiking Training
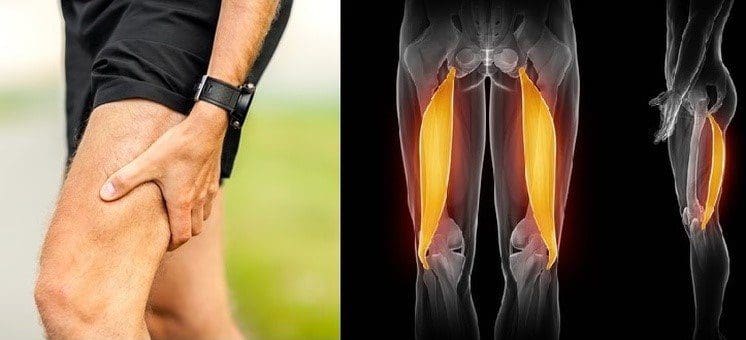
Two of the most common hiking injuries are rolling the ankle and ankle sprains. Individuals that are out of shape or haven’t been active for some time are recommended to start with basic movements and exercises to warm up the muscles and increase heart rate.
Walk/Run Through Sand
- This builds the muscles that protect the knees and ankles.
Increase Range of Motion
- Using a resistance band will strengthen muscles through their full extension.
- Standing on a tennis ball or balance disc is great as it builds the small stabilizer muscles around the ankles and knees.
Crunches
- Building core strength will help maintain balance on uneven surfaces.
Squats and Lunges
- Keep the back straight and take each squat and lunge slowly to strengthen the core muscles.
Push-ups
- Sufficient upper body strength, especially the back muscles will help on long trips and when carrying a heavy pack.
Cardiovascular
- Walking around the neighborhood, on a treadmill, or stationary bike will work to increase cardiovascular ability.
- The objective is to get the heart rate up to build lung capacity.
Step-ups
- Before a backpacking trip, weigh the pack – try 20 lbs. – and step up onto a park bench 16 to 18 inches high.
- Add 5 pounds a week until the pack is as heavy as it will be on the hike.
Strength Hiking Training for Backpacking
Carrying a heavy pack activates many muscles, including those of the arms and shoulders, and back. Hiking for an extended period with a backpack requires getting used to the weight and feel of it. Nothing conditions the body for a pack better than actually experiencing it.
Shoulder and Neck
- The trapezius muscles radiate out from the base of the neck.
- This is where the shoulder harness of the pack sits.
- Strong traps help prevent soreness.
- Most of the pack’s weight should be on and around the hips, but it doesn’t always happen due to pack design and body shape.
Shoulder and Arm
- The shoulder of the arm used to put on and take off the pack does a lot of work at awkward angles.
- The rotator cuff of the shoulder is vulnerable to these loads.
Upper Back
- The muscles of the upper and mid back contract to stabilize the pack, especially with heavy loads.
- Beginning hikers and backpackers tend to get a dull pain right in the center of the shoulder blades.
Lower Back
- The lower back takes the brunt of the force from lifting and twisting the posterior chain of muscles.
Abdominal Muscles
- The abdominal muscles work to stabilize the pack when twisting and turning.
Legs
- Walking, squatting, and standing with the pack requires strong support from the legs.
- Strong legs, especially thighs, make a difference.
- An all-around beginner’s workout is a good place to begin.
Hiking Training: Preparing For A Weekend Hike
- Go out for a walk two or three times during the week.
- Make sure to move briskly enough to get the heart rate up, and keep it up for at least 30 minutes.
- Wear a lightly-weighted daypack on weekday walks to prepare for the essential gear.
- Wear the same shoes that you will be wearing on the hike.
- A definite way to get blisters is to walk for a long time in shoes that haven’t been worn in a while or at all.
Take The Essentials
For simple day hikes, here are some essentials to have on hand:
- Plenty of water
- Simple first-aid kit
- Map – paper type
- Compass
- Food
- Fire-starter or matches
- Multi-purpose knife or tool
- Flashlight and batteries
- Sun hat
- Sunscreen and sunglasses
Start small and go slow until you feel comfortable in the surroundings. Start off with lightweight and short distances and gradually extend to heavier weights and longer distances. Remember to go at your own pace and don’t try to be an expert.
Hikers Strength Training
References
Chrusch, Adam, and Michelle Kavin. “Survey of Musculoskeletal Injuries, Prehike Conditioning, and On-Trail Injury Prevention Strategies Self-Reported by Long-Distance Hikers on the Appalachian Trail.” Wilderness & environmental medicine vol. 32,3 (2021): 322-331. doi:10.1016/j.wem.2021.04.004
Fleg, Jerome L. “Aerobic exercise in the elderly: a key to successful aging.” Discovery Medicine vol. 13,70 (2012): 223-8.
Gatterer, H et al. “Effect of weekly hiking on cardiovascular risk factors in the elderly.” Zeitschrift fur Gerontologie und Geriatrie vol. 48,2 (2015): 150-3. doi:10.1007/s00391-014-0622-0
Huber, Daniela, et al. “Sustainability of Hiking in Combination with Coaching in Cardiorespiratory Fitness and Quality of Life.” International journal of environmental research and public health vol. 19,7 3848. 24 Mar. 2022, doi:10.3390/ijerph19073848
Liew, Bernard, et al. “The Effect of Backpack Carriage on the Biomechanics of Walking: A Systematic Review and Preliminary Meta-Analysis.” Journal of applied biomechanics vol. 32,6 (2016): 614-629. doi:10.1123/jab.2015-0339
Li, Simon S W, et al. “Effects of a backpack and double pack loads on postural stability.” Ergonomics vol. 62,4 (2019): 537-547. doi:10.1080/00140139.2018.1552764
Li KW, Chu JC, Chen CC. Strength decrease, perceived physical exertion, and endurance time for backpacking tasks. Int J Environ Res Public Health. 2019;16(7):1296. doi:10.3390/ijerph16071296
Mitten, Denise, et al. “Hiking: A Low-Cost, Accessible Intervention to Promote Health Benefits.” American Journal of lifestyle medicine vol. 12,4 302-310. 9 Jul. 2016, doi:10.1177/1559827616658229