Table of Contents
Understanding the Sciatic Nerve: Optimal Function and Chiropractic Relief for Sciatica

The sciatic nerve plays a big role in how we move and feel in our lower body. It is the longest and widest nerve in the human body. This nerve starts in the lower back and runs all the way down to the feet. When it works well, it helps us walk, run, and stand without pain. But when something goes wrong, it can cause a condition called sciatica, which brings sharp pain or numbness. Many people deal with this issue, but integrative chiropractic care offers a natural way to fix it. This article explains the sciatic nerve’s job, what optimal health looks like for it, and how chiropractors can help without surgery.
What Is the Sciatic Nerve?
The sciatic nerve is a key part of our nervous system. It forms from nerve roots in the lower spine. These roots originate in the lumbar and sacral regions, specifically L4 through S3. This means it begins in the lower back and branches out. The nerve travels through the buttocks, down the back of each thigh, and splits near the knee. Smaller branches reach the hips, lower legs, and feet.
It is a mixed nerve, meaning it handles both movement and feeling. The nerve is wrapped in protective tissue. In some people, the path varies, such as passing under certain muscles, which can affect the nerve’s function and sensation in the areas it innervates, potentially leading to pain, weakness, or altered sensation in the legs and feet. This nerve is somatic, meaning it controls voluntary movements, such as leg movements.
- Length and Width: It is the body’s longest nerve, stretching from the spine to the feet. It can be as wide as a finger in some spots.
- Pathway: Starts at the base of the spine, goes through the gluteal area, and ends in the foot.
- Branches: Splits into tibial and common fibular nerves near the knee.
Understanding its structure helps explain why problems here affect so much of the body.
Motor and Sensory Functions of the Sciatic Nerve
The sciatic nerve does two main jobs: motor and sensory. Motor functions help control muscles. It sends signals from the brain to make the legs move. For example, it powers the hamstring muscles in the back of the thigh. These muscles bend the knee and help with hip movement.
It also indirectly controls muscles in the lower leg and foot through its branches. This lets us walk, run, and stand on our toes. Without it, simple actions like lifting a foot would be hard.
For sensory functions, it carries feelings back to the brain. This includes touch, pain, and temperature from the legs and feet. It covers the back of the thigh, parts of the lower leg, and the sole of the foot. The tibial branch senses the bottom of the foot, while the common fibular nerve handles the top and sides.
- Motor Examples: Bending the knee, flexing the foot, rotating the leg outward.
- Sensory Areas: Skin on the lateral leg, dorsum of the foot, and plantar surfaces.
- Overall Role: Connects the brain to the lower body for balance and stability.
These functions make everyday movement comfortable and stable.
Optimal Function for Health and Mobility
For optimal health, the sciatic nerve should act as a pain-free pathway. It transmits signals without blocks or irritation. This means smooth motor control for legs and clear sensory feedback to the spine. When it works right, we get a full range of motion in the lower body without pain.
An optimal function allows free signal flow from the lumbar spine to the foot. This supports comfortable walking, standing, and feeling sensations. It helps with balance and prevents issues like foot drop.
To keep it healthy, stay active and strengthen core muscles. Use proper posture and avoid long sitting. Regular exercise, like walking or swimming, helps.
- Signs of Good Function: No pain during movement, full leg flexibility, strong sensations in the feet.
- Benefits: Better stability, easier daily tasks, and less risk of injury.
- Daily Tips: Stretch hamstrings, use lumbar support, and manage weight.
Keeping the nerve unobstructed leads to better overall well-being.
When the Sciatic Nerve Faces Problems: Understanding Sciatica
Sciatica occurs when a nerve is compressed or irritated. This causes pain that starts in the lower back and shoots down the leg. It often affects one side. Symptoms include numbness, tingling, or weakness.
Common causes are herniated discs, spinal misalignment, or muscle imbalances. Things like pregnancy or stress can make it flare up. Prolonged sitting or heavy lifting adds risk.
- Flare Triggers: Bad posture, weight gain, tight muscles.
- Effects: Hard to walk, stand, or sit comfortably.
- Who It Affects: About 8 in 10 people at some point.
Sciatica disrupts daily life, but it can be managed.
Causes and Prevention of Sciatica
Sciatica flares from nerve compression. Herniated discs press on roots. Spinal stenosis narrows the path. Muscle issues like piriformis syndrome trap the nerve.
To prevent it, exercise regularly and lift properly. Quit smoking for better blood flow. Manage stress to reduce tension.
- Prevention Steps: Strengthen core, stretch daily, and avoid twists when lifting.
- Lifestyle Changes: Maintaining a healthy weight, taking frequent breaks from sitting, and practicing yoga for flexibility.
- Why It Works: These keep the nerve free from pressure.
Prevention keeps the nerve functioning smoothly.
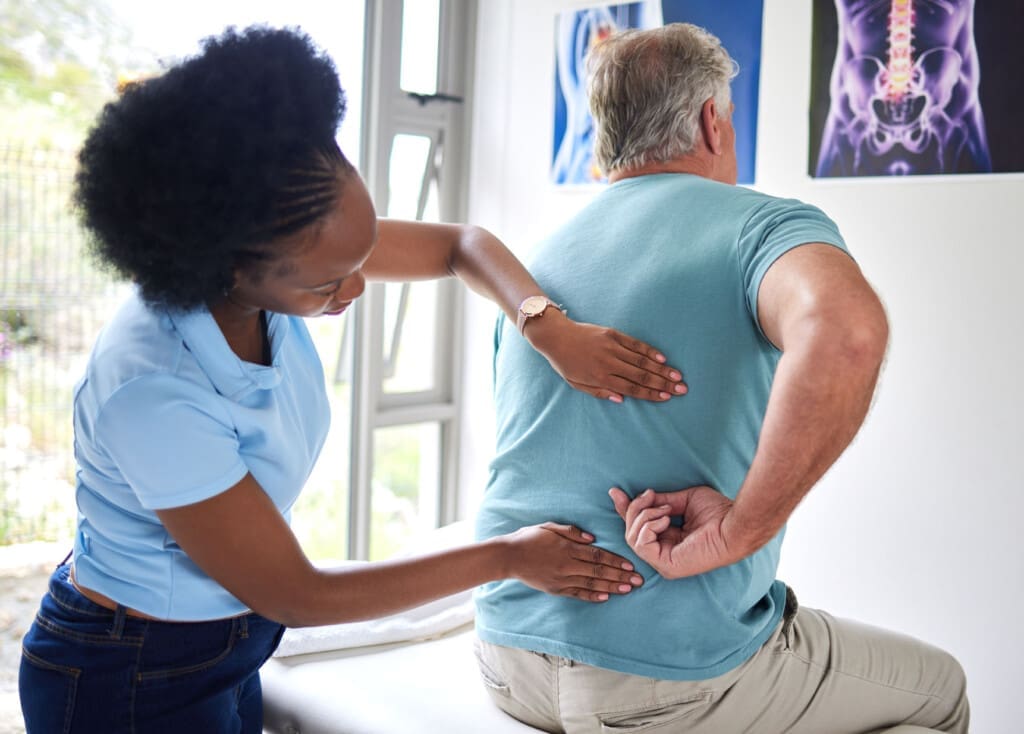
How Integrative Chiropractic Clinics Address Sciatica
An integrative chiropractic clinic focuses on root causes without surgery. They treat compression from misalignments or discs. Adjustments realign the spine to ease pressure.
They use soft tissue therapy to relax muscles and reduce inflammation. Exercises build strength and flexibility. This holistic approach includes nutrition and posture advice.
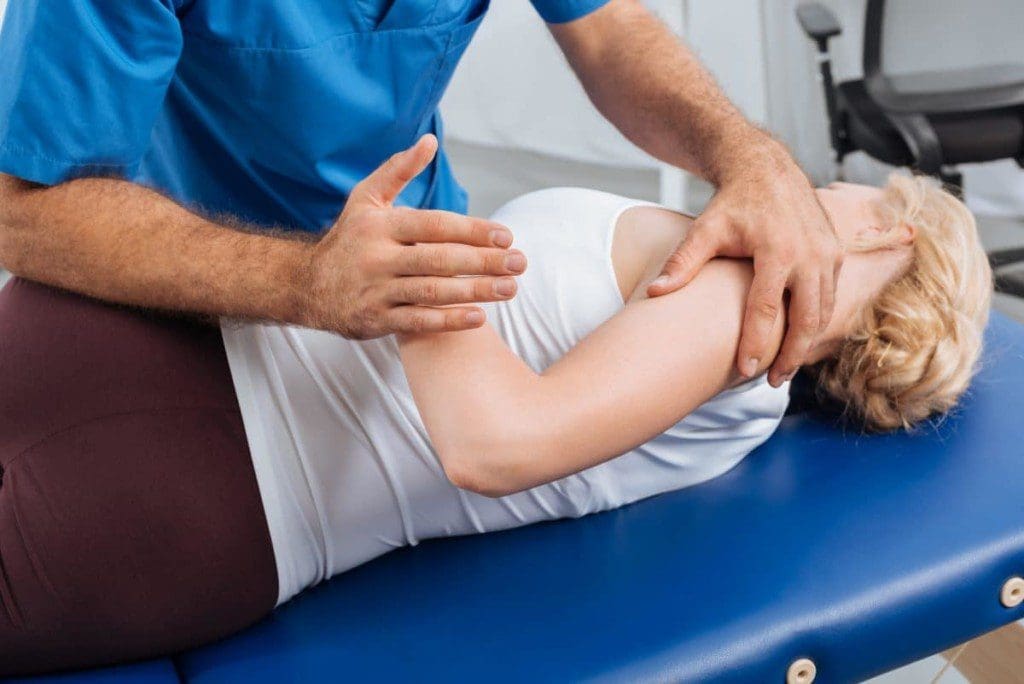
- Techniques Used: Spinal manipulations, massage, and stretches such as knee-to-chest.
- Non-Surgical Focus: Avoids meds or cuts, promotes natural healing.
- Assessment: Exams, history, imaging if needed.
This method restores function gently.
Benefits of Chiropractic Care for Sciatica
Chiropractic care restores mobility and cuts pain. It improves flexibility by loosening tight areas. Patients rely less on pain pills.
It offers long-term relief by addressing the root causes. Better alignment means fewer flares. It boosts overall health and productivity.
- Key Benefits: Pain reduction, better sleep, enhanced stability.
- Holistic Gains: Drug-free, improved posture, faster recovery.
- Patient Outcomes: Quick relief, back to activities.
These perks make it a top choice.
Clinical Observations from Dr. Alexander Jimenez
Dr. Alexander Jimenez, DC, APRN, FNP-BC, has over 30 years of experience in chiropractic care. He notes sciatica often comes from a disc herniation in 90% of cases. Symptoms include burning, tingling, and numbness in the leg.
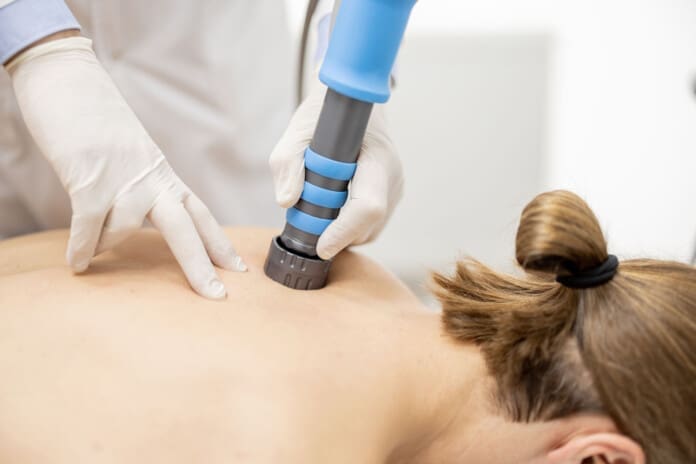
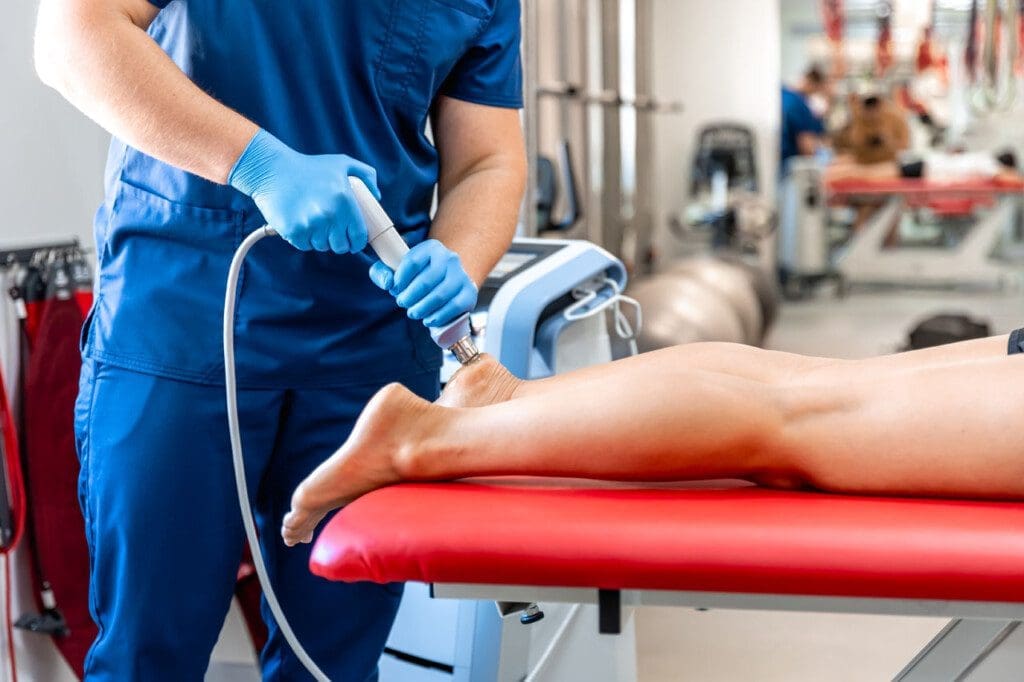
He uses adjustments to realign the spine and ease symptoms. Integrative methods like functional medicine address root causes through nutrition and therapy, which can improve overall health and potentially reduce symptoms such as burning, tingling, and numbness in the legs. His clinic offers non-surgical options like shockwave therapy.
- Observations: Affects daily activities, treatable without drugs.
- Approaches: Personalized plans, education via podcasts.
- Results: Improved mobility, pain relief.
His work supports natural recovery.
Wrapping Up: A Path to Better Nerve Health
The sciatic nerve is vital for lower-body function. Optimal health means pain-free movement and sensation. Sciatica disrupts this, but chiropractic care fixes the causes naturally. By using adjustments and exercises, clinics restore well-being. Prevention through activity and posture keeps issues away. With experts like Dr. Jimenez, relief is possible without invasive steps.

References
- Health.com. (n.d.). The Sciatic Nerve Is the Largest Nerve in Your Body—Here Are 3 Ways To Keep It Healthy
- Cleveland Clinic. (n.d.). Lower Back & Leg Pain? It Might Be Sciatica
- Pangea Chiropractic. (n.d.). Sciatica: Causes, Symptoms & Treatment Options
- TeachMeAnatomy. (n.d.). The Sciatic Nerve – Course – Motor – Sensory
- Hinge Health. (n.d.). What Causes Sciatica to Flare Up, Plus 12 Ways to Prevent It
- Hinge Health. (n.d.). Sciatic Nerve: Definition, Function, Common Conditions & More
- Ohio State Wexner Medical Center. (n.d.). Sciatica (Lumbar radiculopathy)
- YogaUOnline. (n.d.). Yoga for Pain Relief – Managing and Preventing Sciatica
- Active Health Center. (n.d.). Sciatica and Chiropractic Care: Natural Solutions for Nerve Pain
- Cardinal Chiro Sports. (n.d.). 5 Benefits of Working with a Chiropractor for Sciatica
- Mesquite Chiropractic. (n.d.). Why Chiropractic Care is a Natural Solution for Sciatica
- Renton Chiropractic Care. (n.d.). From Agony to Mobility: How Chiropractic Care Can Alleviate Sciatica and Restore Well-Being
- Enhanced Living Chiro. (n.d.). How Chiropractic Care Can Help with Sciatica
- MedlinePlus. (n.d.). Sciatica
- Tigard Chiropractic Auto Injury. (n.d.). Sciatica Solutions: How Chiropractic Care Can Help Office Professionals Find Relief
- Bell District Spine and Rehab. (n.d.). The Benefits of Chiropractor Services for Sciatica
- Elite Doctor. (n.d.). Can a Chiropractor Help Sciatica?
- Spine-health. (n.d.). Sciatic Nerve: Muscle Innervation and Function
- Wikipedia. (n.d.). Sciatic nerve
- Optimal PT LV. (n.d.). Optimal Therapy Sciatica Early Stage Rehab
- Injury 2 Wellness. (n.d.). Sciatica Pain Relief: How Chiropractic Adjustments Offer Solutions
- Oak Street Health. (n.d.). 7 Ways to Manage Sciatica Pain
- Dr. Alex Jimenez. (n.d.). Injury Specialists
- LinkedIn. (n.d.). Dr. Alexander Jimenez, DC, APRN, FNP-BC, IFMCP, CFMP, ATN ♛