Multiple sclerosis and sciatica can exist side by side or have overlapping symptoms. The sciatic nerve begins at the lower back, then through the hips into the buttocks, and separates into both legs into the feet. Sciatica is a type of pain caused by a compressed/pinched or damaged/injured sciatic nerve. The sensation radiates across the nerve with frequency and severity at varying levels, depending on the individual’s body position and/or movement. Individuals with multiple sclerosis can also experience sciatica, believing it’s their multiple sclerosis. Neuropathic pain is a common symptom in multiple sclerosis or MS. It is caused by injury or damage to the nerves of the central nervous system and can cause burning, or sharp, stabbing sensations.
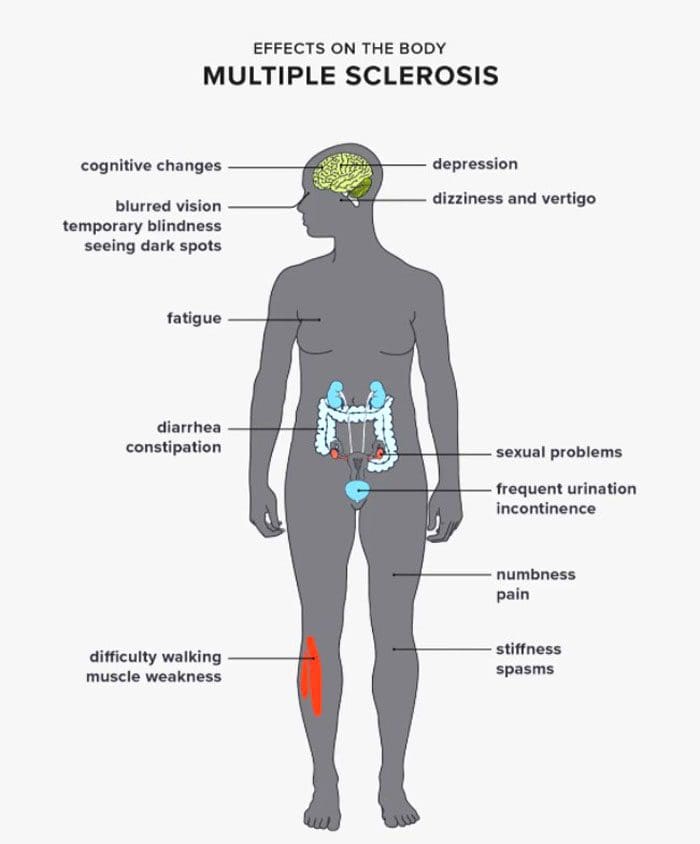
Table of Contents
Multiple Sclerosis and Sciatic Nerve Pain Difference
MS is an autoimmune disorder where the immune system attacks the protective layer around nerve fibers known as myelin. This affects the central nervous system pathways that regulate feeling and sensation in the body. It can cause painful sensations that include:
- Muscle spasms
- Burning, tingling, or aching in the lower legs
- Electrical shock-like sensations travel from the back toward the legs.
- Migraines
- The painful sensations result from the damaged nerve fibers creating interference in the brain’s neural pathways.
Sciatica works differently
An autoimmune response does not damage the sciatic nerve’s pathway, but an added stress/pressure compresses the sciatic nerve. The pain is usually caused by a quick, jerking, twisting, bending, reaching motion that pinches or twists the nerve. Herniated discs and bone spurs are another common cause, along with being overweight can place intense pressure on the sciatic nerve. The critical difference is that multiple sclerosis causes the central nervous system’s signaling pathways to malfunction.
MS and Sciatica
Most individuals, around 40%, will at some point experience some form of sciatica symptoms. This is from age, and all the wear and tear the low back goes through daily. This is why it’s not unusual for individuals with MS to experience sciatica as well. MS can cause body changes that affect activity levels.
- Decreased mobility can lead to sitting for extended periods that can strain the muscles, tendons, and ligaments, causing sciatica.
- There is evidence that the lesions that present from MS can extend to the sciatic nerve.
- One study compared 36 individuals with MS to 35 individuals that don’t have it.
- All of the participants underwent magnetic resonance neurography to obtain high-resolution nerve images.
- The research found that those with MS had slightly more lesions on the sciatic nerve than those without MS.
Sciatica Care
It can be challenging to figure out the types of pain being experienced. Sciatica travels down the length of the nerve uniquely and is often felt in only one leg. The pain, tingling, numbness, electrical sensations can present only in the lower back, the buttock, the back of the leg, hamstring, calf, and foot, or in a combination of all the areas. Treatments for sciatica depend on the severity. They include:
- Chiropractic
- Physical therapy
- Posture exercises
- Lifestyle adjustments
- Physical activity and exercise
- Weight loss
- Cold and hot packs
- Acupuncture
- Over-the-counter pain relievers
- Medications – anti-inflammatories, muscle relaxants, tricyclic antidepressants, and antiseizure medications.
- Steroid injections – corticosteroids
- Surgery is a last resort reserved for severe cases that did not improve with other treatments and therapies.
It can be easy to mistake sciatica as a symptom or related condition of multiple sclerosis. Chiropractic can help alleviate sciatica, and although treatment cannot directly treat MS or its symptoms, it can relieve pain and discomfort.
Body Composition
Diabetic Nephropathy
Diabetic nephropathy or diabetic kidney disease is the result of mismanaged diabetes. Kidney failure is a severe medical emergency and can be fatal if not treated. Chronic low kidney function results in:
- Fluid retention in the body.
- Inability to filter out metabolites and waste from the blood.
- Increased risk of infections.
Common symptoms of diabetic kidney disease include:
Increased blood pressure
- This is the result of increased stress on the body.
- The kidneys can no longer filter out all the metabolites and excess fluid needed to stabilize the blood pressure.
Proteinuria or protein in the urine
- Chronic kidney damage results in the protein being excreted through urine.
Fatigue
- Poor kidney function affects every organ in the body.
- The organs have to work harder to compensate, leading to fatigue and low energy.
Lower extremity edema
- Fluid retention usually presents in the lower extremities.
- Puffy, swollen ankles and legs may appear shiny or waxy.
- This is common in individuals that have severe diabetic nephropathy.
Shortness of breath
- As the fluid builds up in the body, additional weight can get stored on and around the lungs.
- This can make breathing very difficult when lying down or when engaged in physical activity.
Impaired cognition
- Metabolites in the blood can cause brain damage when not filtered properly.
- Memory loss
- Mood changes
- Loss of consciousness
References
Jende JME, et al. (2017). Peripheral nerve involvement in multiple sclerosis: Demonstration by magnetic resonance neurography. DOI:
10.1002/ana.25068
Mayo Clinic Staff. (2019). Sciatica.
mayoclinic.org/diseases-conditions/sciatica/symptoms-causes/syc-20377435
Murphy KL, et al. (2017). Chapter 4: Neuropathic pain in multiple sclerosis—current therapeutic intervention and future treatment perspectives.
ncbi.nlm.nih.gov/books/NBK470151/
Pain and itching. (n.d.).
nationalmssociety.org/Symptoms-Diagnosis/MS-Symptoms/Pain
Samson K. (2017). In the pipeline-multiple sclerosis neurography, MRI reveals peripheral nerve lesions in MS patients. DOI:
10.1097/01.NT.0000527861.27137.b0
Sciatica: Of all the nerves. (2016).
health.harvard.edu/pain/sciatica-of-all-the-nerve
Professional Scope of Practice *
The information herein on "Multiple Sclerosis, Sciatica, and Nerve Pain" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card