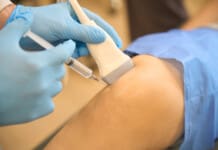
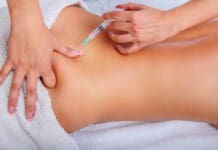
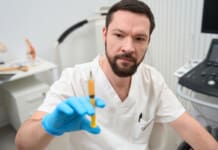
Living with sciatica can be debilitating and exhausting. Find out how different individuals reduced their pain from this condition. Sciatica has different treatment options. It is often a matter of trial and error to find a treatment/therapy that works for the individual. These include:
- Physical therapy
- Medication
- Chiropractic
- Injections
- Acupuncture
- Surgery

Different individuals with sciatica share what works for them. Here are their stories.
Table of Contents
Rudy Found Relief With Self Care
A bad fall left Rudy, a graphic designer, with a broken pelvis and broken foot. I was in the hospital for a few days, and when I came home, I noticed I was hobbling. I had developed sciatica. I was in a lot of pain but decided to try the treatment that had helped me manage chronic migraines. This was yoga. Specifically, it was hot yoga sessions that, despite the pain, worked. However, for others, he recommends not staying still. The body can’t stay stagnant with no movement.
Rudy follows a plant-based diet. Eating right has helped significantly. He starts the day with a green smoothie and sips one throughout the day. This reduces inflammation and pain. His stress would also contribute to the pain. Anything felt from a pain perspective becomes amplified when in a sad, frustrated, confused mood. Rudy’s advice is to get the body moving. And follow a plant-based anti-inflammation diet.
Medication and a Topical Pain Balm Work For Jose
Jose, 66, figured how his sciatica developed was when he decided to insulate the garage. I was bending, twisting, turning, and contouring my body every which way. A week after the job, I developed excruciating pain that got worse over the following weeks. I would jolt out of bed at 2-3 in the morning with severe pain. My doctor gave me steroids that didn’t do anything. I could barely sit down and had to go through a careful method of getting into a chair. I was prescribed Vicodin – hydrocodone/acetaminophen. I took them for a week and a half.
The pain went away, but it came right back as soon as I stopped taking the meds. The meds were only masking the pain. I decided only to use it when the pain was excruciating. This was because I was worried about addiction. I tried chiropractic, massage, acupuncture, cupping, and physical therapy. Unfortunately, I was not feeling any real relief. Then I went to a pain management doctor, who ordered an X-ray and an MRI.
The doctor informed me that my spine was in great shape. The pain management doctor gave me a piriformis injection and, later, an epidural steroid injection. There were still no positive results. My primary care doctor prescribed gabapentin. This is an anti-epilepsy medication that has been shown to help some cases of back pain. Most of the major pain is gone, and I’m pretty sure it’s from the gabapentin along with weekly deep massage sessions. I also use CBD cream with arnica. Movement is important; during the day, I make sure to stand up and walk around.
Epidural Injections Work For Isabel
Isabel has chronic pain. This comes from arthritis, migraines, and fibromyalgia. Sciatica developed as a result of these conditions. Soon she couldn’t get into the car or even empty the dishwasher without going through excruciating pain. Nerve ablation or physical therapy was ineffective at relieving the pain. Then my doctor suggested getting an epidural injection. This is not the same type of injection as when having a baby. It is not the same at all. The injection includes a steroid medication called a corticosteroid that is an anti-inflammatory, along with an anesthetic. I tried it and got some relief, but the pain came back. However, after a month and a half, I began to feel more relief. The pain is not completely gone. I do feel better, but there is still some pain. My doctor told me that patients are all different and require different amounts of medication and time to work.
Surgery Gave Pablo His Life Back
Pablo, 50, is no stranger to back pain or back surgery. After living with chronic back pain from a roll-over auto accident, Pablo underwent a laminectomy. A doctor removed a portion of the vertebra in 1998 and spinal fusion in 2004 that fused the discs from L5 to S1. Life was going well until I was laid off from my desk job. I started working at a warehouse doing light work, but I would still help lift moderate/heavy bags, boxes, etc. I just pushed through the pain, thinking it was a strain that would go away.
However, during the last six months, the pain was so bad I had to stop working. I needed a cane to get out of a chair. Friends and family told me I was walking like a 90-year-old. I also lost feeling in a couple of my toes. In 2021 I had another fusion and had a broken screw from my earlier fusion repaired. The surgery went well, and they said as long as I don’t do any heavy lifting, I should be alright. Although there is still pain, it is much less than it was before the surgery. My doctor recommended a new desk job and a physical therapy rehabilitation, stretching, and strengthening program.
Body Composition
Calories burned from 10,000 steps
Estimations of how many calories are burned from exercises like walking or running depends on how heavy an individual is. Heavier people use more energy to move than lighter people. Estimates revolve around 100 calories burned per mile for a 180-pound person. 10,000 steps comes to around roughly 5 miles. Assuming an individual weighs 180 pounds means 100 calories x 5 miles equals 500 calories. Over a week, it becomes 3,500 calories. However, lighter or heavier individuals will burn less or more calories while walking the same number of steps or distance.
Professional Scope of Practice *
The information herein on "Different Individuals Different Sciatica Treatment Approaches" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card