Belly fat is a gateway to back pain/spinal issues that can lead to various health problems. The bulging belly population has grown a bit since the beginning of the COVID-19 pandemic. 37% of individuals have gained weight since it began, according to a global Ipsos survey. If back pain is presenting and there is excess weight around the abdomen known as abdominal obesity, this could be a contributing factor.
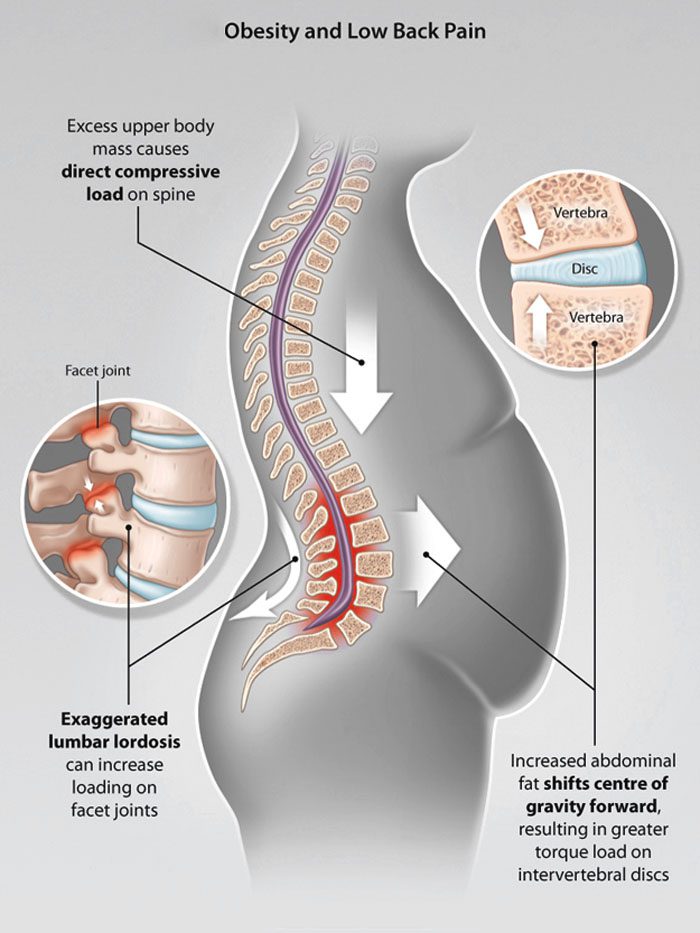
Table of Contents
Belly fat and posture
When the natural curves of the spine are normal, the core is stable and well-supported. Excessive weight, including a large abdomen, shifts these curves out of correct alignment. Excessive abdominal fat has been associated with lordosis, which is an excessive inward curve of the spine toward the lower back. One study found that severely obese individuals had pain and changes in posture. This was especially visible in the spine, knees, and feet.
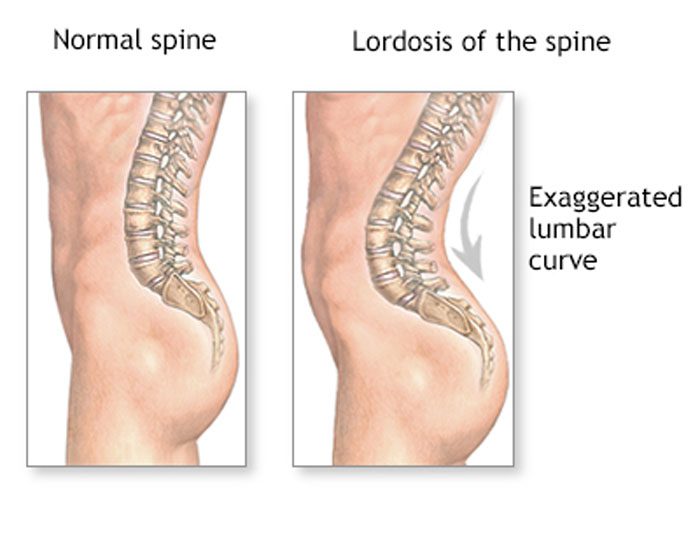
Front-loading shift
The back pain felt from a bulging belly can be caused by a shift in posture and body mechanics. Studies show these can have a negative impact on back pain and body positioning. All or most of the weight is placed on the lower back.
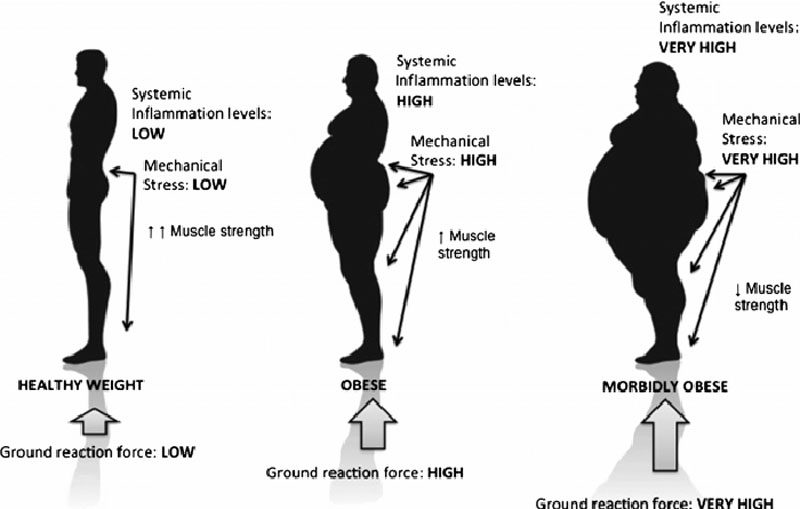
Overloaded discs
Abdominal obesity can damage/injure the discs/shock absorbers of the spine. This leads to:
- Increased pressure
- Annular tears
- Herniation
- Pinched/compressed nerves
And a bulging belly can flatten the height of the intervertebral discs.
Fat pollutants in the blood
Fat can accumulate and secrete toxins that contribute to swelling and inflammation that can be painful. Over time, these toxins wear down components of the skeletal system. A study found potential links between obesity and degenerative disc disease. Scientists found a connection in obese men, but not obese women. This is believed to be because men tend to store fat in their bellies, and women tend to store fat in the buttocks and thighs.
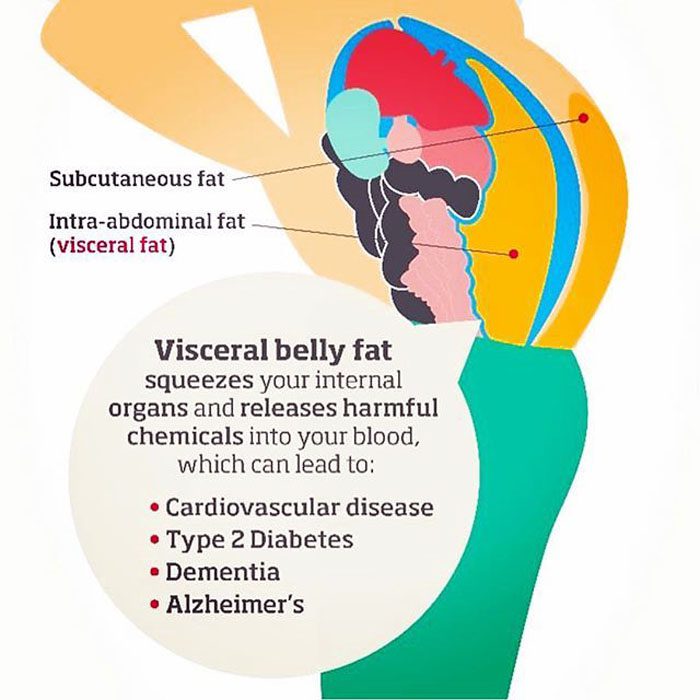
Damage to the musculoskeletal system
The bones constantly renew themselves, but when there is excess body fat it can interfere with the process. This has the potential to turn into osteoporosis over time. Studies associate visceral fat with lower bone mineral density, and an increase in the risk of fractures.
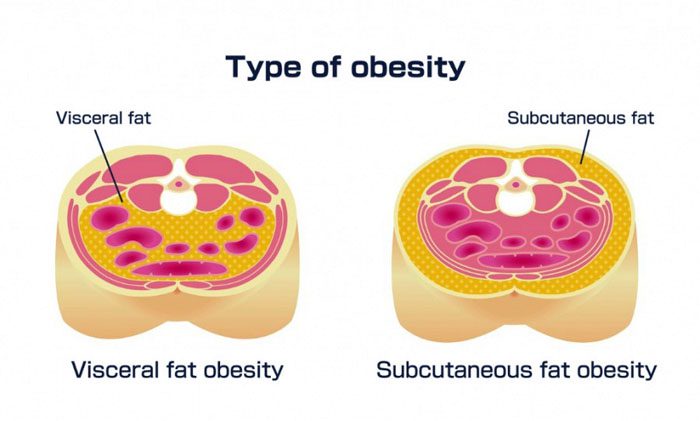
Ankylosing spondylitis treatment and fat interference
Ankylosing spondylitis is an inflammatory disease that causes chronic back pain and can cause the vertebrae to fuse. The back can be extremely stiff, and the condition can lead to a permanently hunched posture. There are medications to improve symptoms and slow the disease. However, being overweight reduces the drugs’ effectiveness. This is because belly fat can cause medication absorption problems.
Rare spinal condition linked to obesity
Obesity along with a high Body Mass Index increases the risk of a rare condition called spinal epidural lipomatosis or SEL. This is an overgrowth of body fat in the spinal canal. Spinal epidural lipomatosis can cause various types of back pain. This is why it is recommended to have a doctor examine and evaluate any aches or pains.
Body Composition
Kombucha beneficial for gut bacteria
Kombucha contains a wide variety of bacteria and fungi that helps ferment the sugar in kombucha drinks. It is able to affect the existing microbes in the gut by inhibiting the growth of various gut-dwelling pathogens. These include:
- Salmonella
- Campylobacter
- E. coli
- H. pylori

- It is a probiotic drink made from fermenting green or black tea
- It is made up of healthy bacteria that produce acetic acid that is beneficial for blood sugar, insulin levels, and body composition
- It helps the body process food by lowering insulin levels after a meal
- It contains polyphenols that reduce oxidative stress, to help fight disease risks
- It destroys unhealthy bacteria in the gut
- It helps increase healthy bacteria
Kombucha can be thought of as a natural antibiotic. However, it does not come with the weight-gain side effect. Improving the health of the gut through fermented foods like kombucha help reduce the risk for weight gain/obesity, as well as restore gut health for those trying to lose weight by creating a healthy gut environment.
Disclaimer
The information herein is not intended to replace a one-on-one relationship with a qualified health care professional, licensed physician, and is not medical advice. We encourage you to make your own health care decisions based on your research and partnership with a qualified health care professional. Our information scope is limited to chiropractic, musculoskeletal, physical medicines, wellness, sensitive health issues, functional medicine articles, topics, and discussions. We provide and present clinical collaboration with specialists from a wide array of disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for the musculoskeletal system’s injuries or disorders. Our videos, posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate to and support, directly or indirectly, our clinical scope of practice.* Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We provide copies of supporting research studies available to regulatory boards and the public upon request. We understand that we cover matters that require an additional explanation of how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900.
Dr. Alex Jimenez DC, MSACP, CCST, IFMCP, CIFM, CTG*
email: [email protected]
phone: 915-850-0900
Licensed in Texas & New Mexico
References
Osong Public Health and Research Perspectives. (2016) “Influence of Obesity on Postural Stability in Young Adults.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5194219/
Obesity Surgery. (2005) “Postural changes in morbidly obese patients.” https://pubmed.ncbi.nlm.nih.gov/16105399/
Arthritis Research & Therapy. (2017) “Fat mass and fat distribution are associated with low back pain intensity and disability: results from a cohort study.” https://arthritis-research.biomedcentral.com/articles/10.1186/s13075-017-1242-z
Clinical and Investigative Medicine. (2014) “Visceral fat reflects disease activity in patients with ankylosing spondylitis.” https://pubmed.ncbi.nlm.nih.gov/24895992/
European Spine Journal. (2012). “Rapid progression of spinal epidural lipomatosis.” https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3369035/
Professional Scope of Practice *
The information herein on "Belly Fat Can Cause Back Pain and Injury" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card