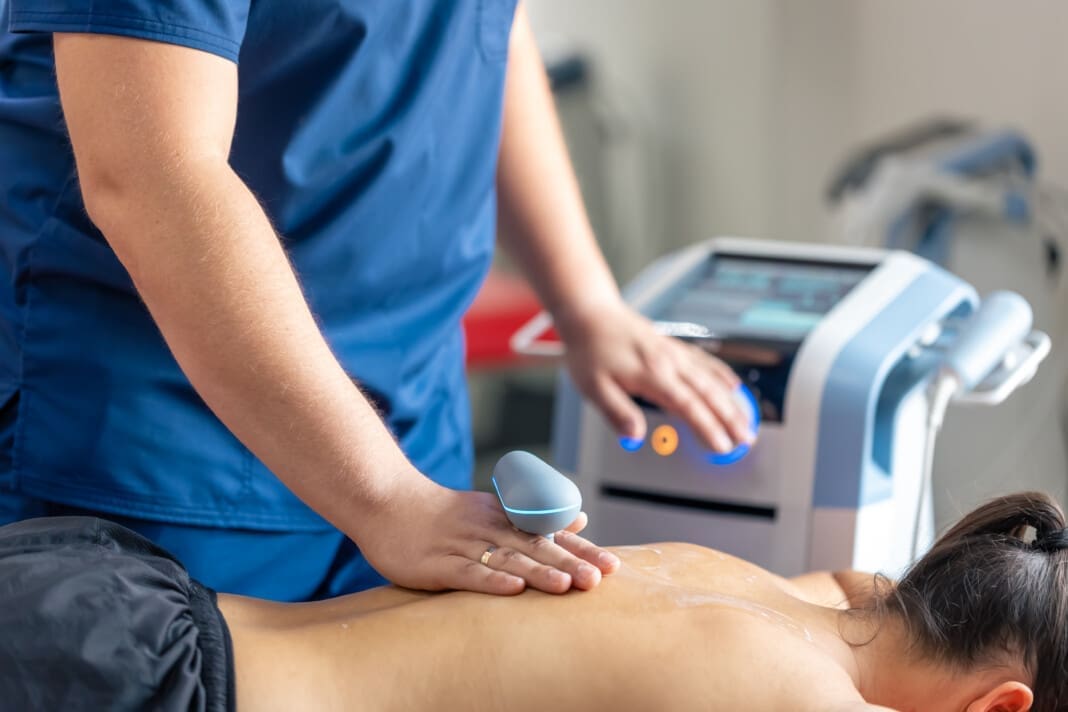
Learn about the effectiveness of ultrasound therapy in enhancing recovery and managing musculoskeletal pain.
Table of Contents
Abstract
In this educational post, I guide you through a practical, first-person journey on musculoskeletal ultrasound (MSK-US): how to recognize normal patterns of tendons, muscles, cartilage, ligaments, and nerves; how to avoid common pitfalls like anisotropy; and how to handle the probe with precision for both diagnostic and interventional applications. I explain why perpendicular insonation matters, how to differentiate hyperechoic and hypoechoic structures, and how to perform dynamic stress testing for the medial collateral ligament (MCL) and similar structures—often even as a single clinician. I integrate the latest research with what I see daily in the clinic, connecting imaging findings with functional outcomes and manual, rehabilitative, and lifestyle strategies. Throughout, I show where integrative chiropractic care fits: linking high-fidelity imaging, hands-on assessment, targeted soft-tissue and joint techniques, neuromuscular re-education, loading protocols, and procedural guidance into a coherent, individualized plan.
Introduction: Why Ultrasound Is My “Glorified Flashlight”
As a DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST, I rely on ultrasound as a real-time, nonionizing “flashlight” to see living anatomy in motion. Point-of-care ultrasound (POCUS) allows me to stress a ligament. At the same time, I watch its fibers approximate or gap, glide a tendon, and assess its fibrillar integrity, or visualize a nerve’s honeycomb architecture as it tracks through the forearm. The value is twofold:
- It enhances diagnostic specificity by mapping structural, load-response, and pain behaviors at the bedside.
- It accelerates intervention by guiding precise manual therapy, rehabilitation progressions, and, when indicated, needle-based procedures.
Done well, MSK-US is predominantly pattern recognition. I am constantly asking: “Do I see the expected echotexture, orientation, and continuity for this structure—at rest and under stress?” The following sections outline how I approach these questions and how they translate into integrative chiropractic care.
Tendon Sonography: Fibrillar Stripes, Hyperechoic Patterns, and the Perils of Anisotropy
When I scan a tendon, I look for the characteristic, tightly packed, parallel, hyperechoic fibrillar pattern in the long axis and a punctate, stippled pattern in the short axis. For example, in a long-axis view of the patellar tendon, I expect:
- Patellar tendon: bright, linear, hyperechoic “stripes” running parallel to fiber direction.
- Fat pad (infrapatellar): relatively hypoechoic, softly undulating band deep to the tendon.
- Bony cortex of patella and tibia: sharply hyperechoic line with posterior acoustic shadowing.
Why this matters: Tendons are highly ordered arrays of collagen. The collagen fascicles and interfascicular matrix reflect sound strongly when the ultrasound beam is perpendicular to the fibers. If I am off-angle, those same fibers may appear falsely hypoechoic or “dark.” This phenomenon—anisotropy—is both the tendon’s friend and our diagnostic trap.
- Anisotropy explained: Collagen behaves like a mirror. A perpendicular beam reflects echoes (appearing hyperechoic). An angled beam reflects away (appearing hypoechoic), mimicking a tear.
- Clinical protocol: I “prove” a suspected hypoechoic defect by:
-
- Re-optimizing perpendicular insonation (“heel-toe” or toggle to 90 degrees).
- Scanning in orthogonal planes (long and short axis).
- Performing dynamic tests (e.g., resisted abduction for supraspinatus).
- Confirming persistent hypoechoic discontinuity or gapping under stress.
If a dark region disappears when I correct the angle, I attribute it to anisotropy. If it persists in multiple planes and widens with load, I consider partial- or full-thickness tearing.
Integrative chiropractic care fit:
- Imaging informs manual care: With an intact tendon but pain and hypoechoic peritendinous edema, I emphasize graded loading, tendon isometrics progressing to eccentrics, and instrument-assisted or hands-on soft-tissue techniques to address tenosynovitis or compressive tendinopathy, while correcting proximal and distal joint mechanics.
- If true tearing is present, I adjust load, protect, and coordinate regenerative or orthopedic consultation as indicated, using ultrasound to monitor healing and guide any procedure.
Muscle Imaging: Normal Hypoechoic Muscle With Hyperechoic Strands and Fascial Planes
Healthy skeletal muscle appears predominantly hypoechoic with fine hyperechoic stranding from connective tissue (perimysium/epimysium). Over a humerus, whether deltoid or biceps region, I expect to see:
- Muscle belly: hypoechoic “meat” with subtle bright intramuscular septa.
- Myotendinous junction: tapering into a more hyperechoic, organized tendon.
- Underlying bone: bright cortical line with shadowing.
Physiology and clinical meaning:
- Muscle fibers contain water and contractile proteins that scatter sound, producing a relatively darker echotexture.
- In strain injuries, I look for acute localized hyperechoic disruption (hemorrhage can vary), hypoechoic clefts, fascial discontinuity, and fluid along fascial planes.
- Dynamic contraction helps identify functional deficits: does the suspected region bulge, shorten, or exhibit pain inhibition?
Integrative chiropractic care fit:
- I combine ultrasound findings with strength and control tests. If I see myotendinous strain without retraction, I often prescribe isometrics for analgesia, followed by isotonic loading within pain thresholds, and manual therapy to reduce guarding and restore fascial glide.
- Joint adjustments can normalize arthrokinematics where altered joint motion is driving muscle overload (e.g., scapulothoracic dyskinesis contributing to rotator cuff strain).
Cartilage on Ultrasound: Hyaline Versus Fibrocartilage in the Shoulder
Posterior shoulder views nicely demonstrate hyaline cartilage over the humeral head—typically a thin, smooth hypoechoic band superficial to subchondral bone. Adjacent fibrocartilaginous structures (such as the labrum) tend to be relatively hyperechoic and heterogeneous.
Why this matters:
- Hyaline cartilage’s high water content scatters and absorbs ultrasound, making it appear darker than bone.
- Fibrocartilage’s dense collagen content is more reflective, appearing brighter.
- Although ultrasound is limited for deep intra-articular cartilage, peripheral margins, labral recesses, and posterior joint effusions are often visible, helping determine whether pain is intra-articular or peri-tendinous.
Integrative chiropractic care fit:
- If I find effusion or capsular thickening, I tailor care to unload irritated tissues, perform gentle joint mobilization (grades I–II for pain modulation), and implement progressive closed-chain control—often in concert with anti-inflammatory nutrition strategies and sleep optimization.
- Ultrasound helps me track capsular thickness and effusion over time as we progress from pain relief to mobility and strength.
Ligaments: Dense, Tightly Packed Fibrillar Patterns and Real-Time Stress Testing
Ligaments and tendons can look similar, but ligaments often appear as tightly packed, hyperechoic, fibrillar bands bridging bone to bone, whereas tendons continue into muscle. The power of ultrasound for ligaments is dynamic stressing:
- Example: MCL. With a linear probe on the medial knee in the long axis, I observe the MCL fibers while applying valgus stress.
-
- Grade 1: Pain with minimal fiber elongation; no gapping.
- Grade 2: Partial fiber disruption; measurable gapping compared to the contralateral side; intact endpoint.
- Grade 3: Near-complete disruption; significant gapping without a firm endpoint.
Why dynamic testing works:
- Collagen alignment and tautness under load reveal continuity. Ultrasound visualizes real-time changes in fiber apposition that static imaging (e.g., conventional radiographs) cannot.
Single-clinician stress techniques:
- For knees: I brace the patient’s thigh with my elbow/forearm and apply valgus force with my free hand while maintaining the probe position. Positioning and body mechanics are key, so I can stress and scan without losing the window.
- For elbows (UCL): I fix the humerus against the torso or table edge, then introduce valgus stress while the probe tracks the UCL at the sublime tubercle.
Integrative chiropractic care fit:
- Grade 1–2: Bracing as needed, early isometrics, neuromuscular control, and progressive frontal-plane and rotational stability work. Manual joint techniques address tibiofemoral and patellofemoral mechanics that heighten MCL load. Ultrasound confirms healing landmarks and informs return-to-sport timing.
- Grade 3: I coordinate orthopedic consultation for potential surgical evaluation while optimizing adjacent joint function and conditioning; ultrasound assists with triage and post-op monitoring.
Nerve Ultrasound: The Honeycomb Fascicles and How to Find Them
Peripheral nerves in short axis display a mixed echotexture: hypoechoic fascicles surrounded by hyperechoic epineurium and perineural fat, forming a classic “honeycomb” appearance. In the long axis, fascicles appear as parallel hypoechoic lines within a bright sheath.
Clinical pearls I use:
- Scan at first: Rapid sweeps help the eye detect the nerve’s distinct pattern as it “travels” relative to surrounding tissues. Once located, slow down for detail.
- Maintain perpendicularity: Nerves can also exhibit angle-dependent variability. If the honeycomb disappears, I correct the angle.
- Carpal tunnel: The median nerve’s echotexture contrasts with the brighter flexor tendons. I assess nerve cross-sectional area (CSA) proximal and within the tunnel, glide during finger and wrist motion, and look for bowing of the flexor retinaculum.
Why this matters physiologically:
- Fascicular bundles with myelinated axons have a different acoustic impedance than the surrounding connective tissue and fat, creating the mixed pattern.
- Swollen or hypoechoic nerves with loss of fascicular definition, increased CSA, or intraneural hypervascularity suggest entrapment or neuritis.
Integrative chiropractic care fit:
- I deploy neurodynamic mobilizations, carpal tunnel-specific load management, proximal kinetic chain corrections (cervicothoracic mobility, scapular control), and ergonomic retraining. Ultrasound guides splinting decisions and tracks nerve CSA over time—objective metrics that pair with symptom scores.
Avoiding Anisotropy: The Most Common Diagnostic Pitfall
Anisotropy is a change in echogenicity due to the angle of insonation, particularly in linear collagen structures.
My rule set:
- Always “heel-toe” to align the beam perpendicular to fibers.
- Never rely on a single image. “One image is no image.” I capture orthogonal views and repeat in different arm/leg positions.
- Use functional provocation. If a hypoechoic zone persists and demonstrates dynamic gapping with resisted contraction or ligament stress, I treat it as a true lesion.
Why this matters:
- Avoiding false positives prevents unnecessary immobilization or invasive procedures.
- Catching true pathology early lets me tailor load, manual therapy, or escalate to regenerative or surgical pathways appropriately.
Probe Handling Mastery: Tripod Control, Orientation, and Sterility for Procedures
Precision starts with how I hold the probe. I prioritize fine motor control and a clear path for needles during procedures.
Core techniques I teach and use:
- Tripod contact: I anchor one to three fingers on the patient for stability while my thumb and index finger control subtle rotations, tilts, and translations.
- Two grips for two tasks:
-
- In-plane procedures: “Pencil” grip allows fine alignment of the beam with the needle trajectory.
- Out-of-plane procedures: Edge grip improves toggling and perpendicularity for precise cross-sectional targeting.
-
- Avoid the “tail hold” and “wrap-around” grip: Holding the cable or wrapping fingers across the field reduces control and can obstruct the sterile needle path.
Orientation strategy:
- I orient the image to match the patient’s anatomy—right is right, left is left, cranial is cranial, caudal is caudal—so my hand movements intuitively align with on-screen motion. While ultrasonographers may standardize differently, this approach reduces cognitive load during delicate adjustments.
Why perpendicularity and planning win:
- Staying perpendicular maximizes echogenic contrast, making tendons, ligaments, and nerves stand out.
- Planning the path—find the target first, then bring “tip-to-target”—prevents chasing the needle or losing the lesion.
From Image to Intervention: How Ultrasound Shapes Integrative Care
In my clinic, ultrasound is not an endpoint—it is a bridge to better outcomes. Here’s how imaging guides care:
- Tendinopathy without tearing:
-
- Why: Painful but structurally intact collagen benefits from mechanotransduction.
- What I do: Isometric loading for analgesia; progress to eccentric-concentric regimes; cross-education strategies for pain modulation; targeted soft-tissue work to improve tendon sheath mobility; joint adjustments to offload pathological compression or shear.
- How ultrasound helps: Confirms integrity, detects peritendinous fluid, and tracks tendon thickness and neovascularity over time.
- Partial-thickness cuff tears:
-
- Why: Controlled loading improves tendon resilience while avoiding propagation; scapulothoracic mechanics reduce subacromial compression.
- What I do: Scapular setting and posterior capsule mobility, rotator cuff and lower trapezius strengthening, sleep-side modification; consider shockwave where evidence supports chronic tendinopathy without retraction.
- How ultrasound helps: Monitors defect size, detects bursal effusions, and guides subacromial injections if indicated.
- Ligament sprains:
-
- Why: Early mechanotherapy stimulates collagen alignment and strength; proprioceptive training restores joint stability.
- What I do: Brace when necessary, early isometrics, perturbation training, progressive return to cutting and pivoting; manual joint techniques to normalize accessory motion.
- How ultrasound helps: Quantifies valgus/varus gapping, visualizes fiber continuity, and times progression.
- Nerve entrapment:
-
- Why: Reducing intraneural pressure and improving glide enhances axoplasmic flow and symptom resolution.
- What I do: Neural sliders/tensioners, ergonomic changes, proximal mobility and strength, sleep and glycemic control for neuroinflammation; occasionally, ultrasound-guided hydrodissection when conservative care plateaus.
- How ultrasound helps: Measures CSA, visualizes glide, and verifies injectate spread during procedures.
Evidence-Based and Research Integration
- Tendon imaging and anisotropy: Modern MSK-US texts emphasize angle management to prevent false positives and endorse dynamic testing for rotator cuff and lower-limb tendons (Khan et al., 2022).
- Ligament stress sonography: Dynamic ultrasound gapping measures correlate with clinical grading for MCL and UCL injuries (Park et al., 2021).
- Nerve ultrasound: Cross-sectional area thresholds and fascicular pattern changes support carpal tunnel and other entrapment diagnoses with strong sensitivity and specificity, complementing electrodiagnostics (Hobson-Webb & Cartwright, 2020).
- Integrative load-based rehab: Progressive tendon-loading paradigms demonstrate improvements in pain and function in tendinopathy, aligning with the mechanotransduction model (Rio et al., 2016; Malliaras et al., 2013).
- Ultrasound-guided interventions: Guidance improves accuracy and safety for peri-tendinous, bursal, and perineural injections compared with landmark-only techniques (Finnoff et al., 2015).
My Clinical Observations: What I See in Daily Practice
Drawing from ongoing documentation and case trends I have shared publicly, several patterns consistently emerge:
- When I combine precise ultrasound diagnosis with targeted loading and manual strategies, recovery timelines shorten, and recurrence rates decline compared with non-imaged care.
- Patients with rotator cuff pain who demonstrate significant anisotropy-related false positives often avoid unnecessary immobilization when we dynamically validate fiber continuity, enabling earlier strengthening.
- For median nerve entrapment, tracking CSA changes alongside symptom scales helps tailor brace duration and confirm when to progress loading or consider hydrodissection.
- With MCL injuries, real-time gapping under standardized valgus stress allows more confident return-to-play decisions, synchronized with functional tests, rather than relying solely on time-based protocols.
Practical Tips You Can Use Today
- Always get two planes. One view is no view. Use dynamic tests whenever feasible.
- Scan fast to find nerves; then slow down to analyze. Look for the honeycomb in the short axis.
- Stay perpendicular first; heel-toe later. Fix the angle before diagnosing “tears.”
- Plan the procedure: find the target, align the beam, then bring the tip to the target. Don’t chase the needle.
- Orient intuitively to the patient so your hand movements match the screen.
- For single-operator ligament stress tests, position the body and your forearms to create a stable brace; practice the setup before imaging.
Putting It All Together: Integrative Chiropractic Care Fueled by Imaging
Ultrasound lets me integrate diagnosis and treatment into a single, fluid encounter:
- I visualize, test, and decide—then immediately adjust a joint restriction, release a myofascial tether, begin a graded isometric program, or perform a guided injection when indicated.
- I re-scan over visits to confirm that tissue quality and dimensions reflect the functional gains we measure in the clinic.
- Patients see their tissues in real time, which improves buy-in and adherence—a pivotal factor in successful tendon and ligament rehab.
The result is a modern, evidence-based care pathway where structural integrity, functional capacity, and patient experience move in step. That is the heart of integrative chiropractic care in the ultrasound era.
References
- Finnoff, J. T., Hall, M. M., Adams, E., Berkoff, D., Concoff, A. L., Dexter, W., … & Smith, J. (2015). American Medical Society for Sports Medicine position statement: Interventional musculoskeletal ultrasound in sports medicine. British Journal of Sports Medicine, 49(3), 145–150. https://doi.org/10.1136/bjsports-2014-094346
- Hobson-Webb, L. D., & Cartwright, M. S. (2020). Nerve ultrasound in neuromuscular disorders. Muscle & Nerve, 61(1), 5–20. https://doi.org/10.1002/mus.26764
- Khan, Y., Bhatnagar, A., & Jacobson, J. A. (2022). Fundamentals of musculoskeletal ultrasound. Ultrasound Clinics, 17(1), 1–25. https://doi.org/10.1016/j.cult.2021.10.001
- Malliaras, P., Barton, C. J., Reeves, N. D., & Langberg, H. (2013). Achilles and patellar tendinopathy loading programs: A systematic review comparing clinical outcomes and identifying potential mechanisms. Sports Medicine, 43(4), 267–286. https://doi.org/10.1007/s40279-013-0019-z
- Park, G.-Y., Kwon, D. R., & Park, J.-H. (2021). Diagnostic validity of dynamic ultrasound for collateral ligament injuries: A systematic review and meta-analysis. American Journal of Physical Medicine & Rehabilitation, 100(4), 339–347. https://doi.org/10.1097/PHM.0000000000001692
- Rio, E., Kidgell, D., Purdam, C., Gaida, J., Moseley, G. L., Pearce, A. J., … & Cook, J. (2016). Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy. British Journal of Sports Medicine, 50(24), 1534–1539. https://doi.org/10.1136/bjsports-2015-095245
Hyperlinked Reference List
- American Medical Society for Sports Medicine position statement: Interventional musculoskeletal ultrasound in sports medicine
- Nerve ultrasound in neuromuscular disorders
- Fundamentals of musculoskeletal ultrasound
- Achilles and patellar tendinopathy loading programs: A systematic review
- Diagnostic validity of dynamic ultrasound for collateral ligament injuries
- Isometric exercise induces analgesia and reduces inhibition in patellar tendinopathy
Author
Dr. Alexander Jimenez, DC, APRN, FNP-BC, CFMP, IFMCP, ATN, CCST
SEO tags
musculoskeletal ultrasound, anisotropy ultrasound, tendon imaging, ligament stress ultrasound, median nerve honeycomb, carpal tunnel ultrasound, MCL valgus stress, supraspinatus ultrasound, integrative chiropractic care, ultrasound-guided procedures, tendon loading, neurodynamic mobilization, point-of-care ultrasound, probe handling techniques, heel-toe ultrasound
Professional Scope of Practice *
The information herein on "Ultrasound Therapy in Musculoskeletal Pain Rehabilitation" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card