Table of Contents
Shockwave Therapy and Chiropractic for Soft Tissue Pain and Musculoskeletal Recovery
Abstract
This post explains how electrohydraulic SoftWave technology activates the body’s repair systems to accelerate recovery from conditions like plantar fasciitis, adductor strains, bone edema, and postoperative delayed healing. Using current evidence, clinician-reported outcomes, and real-world sports-performance cases, I explain the physics of true shockwaves versus radial “pressure wave” devices, how cellular mechanotransduction drives angiogenesis and modulates inflammation, and why combining shockwave therapy with integrative chiropractic care and orthobiologics can optimize patient outcomes. I also share practical protocols, patient communication strategies, and clinical observations from my practice, along with insights offered by leading orthopedic consultants to NBA and NFL teams. This guide is designed to help you understand what works, why it works, and how to implement it safely and effectively.

Introduction: How a Technology Changed My Clinical Path
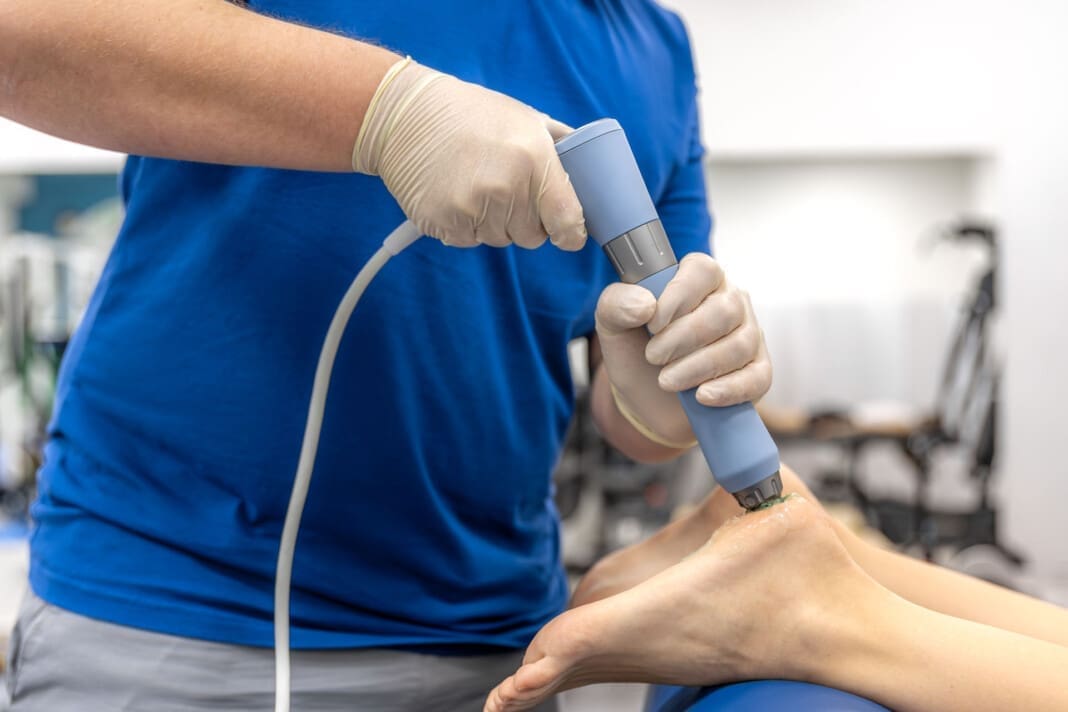
Seven years ago, a patient suffered from severe plantar fasciitis in both feet. They were offered corticosteroid injections, a conventional treatment with known risks, but declined. Instead, a colleague introduced them to SoftWave electrohydraulic shockwave therapy. Following an initial treatment, the patient’s pain briefly resurfaced before gradually resolving over several weeks, without the need for additional stretching or care. Remarkably, they remained symptom-free for approximately four years before requiring another session. This experience demonstrated the technology’s effectiveness in tissue repair and its potential for durable outcomes.
Shockwave Therapy 101: What a True Shockwave Is and Why It Matters
- Key terms:
- Shockwave: A supersonic, high-pressure acoustic wave with a steep pressure gradient and non-linear propagation.
- Electrohydraulic generation: Produces authentic shockwaves at the source using submerged electrodes.
- Radial “pressure wave”: A lower-velocity, surface-biased acoustic wave; often marketed as shockwave but mechanistically distinct.
What defines a true shockwave?
A true shockwave is a supersonic acoustic impulse traveling faster than the speed of sound through tissue, with a steep, rapidly rising pressure front. This wave imparts mechanical shear and transient cell membrane deformation, triggering downstream biochemical signaling. In clinical devices, shockwaves are characterized by their peak pressure, energy flux density, and rise time—parameters that influence tissue penetration and therapeutic effect (ISMST guidelines) (International Society for Medical Shockwave Treatment, n.d.).
Why electrohydraulic shockwaves lead the field
Electrohydraulic systems generate the shockwave inside the applicator via a controlled micro-cavitation event: an electrical discharge across submerged electrodes forms a rapidly expanding plasma bubble. The leading edge of this bubble is the shockwave, already formed and at therapeutic velocity as it exits the applicator. This produces:
- Consistent therapeutic energy across a deep field (often measured up to 10–12 cm in soft tissue).
- A focused primary wave plus a reflected broad focus, covering a larger treatment column than single-focus systems (International Society for Medical Shockwave Treatment, n.d.).
Other generators—electromagnetic and piezoelectric—produce acoustic waves that converge to form a shockwave outside the applicator. While effective, they may require precise focal adjustments and deliver shorter zones of therapeutic energy compared to electrohydraulic approaches (International Society for Medical Shockwave Treatment, n.d.).
Radial pressure wave devices: clinically useful but different
Radial devices produce pressure waves that disperse laterally and primarily affect superficial tissues. Their mechanism relies on microtrauma and hyperemia to modulate pain, which can be uncomfortable and tends to produce more transient outcomes, especially beyond the acute phase (International Society for Medical Shockwave Treatment, n.d.).
Physiological Underpinnings: How Shockwaves Stimulate Repair
- Mechanotransduction: The rapid pressure change causes the cell membrane to deform and become transiently permeable, activating integrin-linked pathways, MAPK/ERK, and PI3K/Akt signaling cascades. These pathways modulate gene expression for growth factors and extracellular matrix turnover (International Society for Medical Shockwave Treatment, n.d.).
- Angiogenesis: Shockwaves upregulate VEGF, eNOS, and related angiogenic mediators, promoting neovascularization. Clinical reports describe marked improvements in microvascular perfusion that correlate with reductions in pain and gains in function (International Society for Medical Shockwave Treatment, n.d.).
- Inflammation modulation: Shockwave exposure can shift macrophage polarization towards M2 phenotypes, lower NF-κB activity, and reduce pro-inflammatory cytokines while enhancing anti-inflammatory mediators—helpful for tendinopathies and fasciopathies (International Society for Medical Shockwave Treatment, n.d.).
- Nociceptive effects: By influencing substance P, CGRP, and peripheral sensitization, shockwaves can reduce pain signaling while the tissue remodels (International Society for Medical Shockwave Treatment, n.d.).
- Matrix remodeling: Enhanced activity of tenocytes and fibroblasts supports collagen alignment and fascia elasticity, contributing to improved load tolerance and function (International Society for Medical Shockwave Treatment, n.d.).
Why these mechanisms matter clinically
In conditions like plantar fasciitis, adductor strains, bone edema, and delayed union, we require both short-term pain relief and durable remodeling. Shockwaves uniquely combine analgesic, pro-angiogenic, and pro-regenerative signals—allowing patients to move earlier and more effectively while tissue quality improves, especially when paired with integrative chiropractic care that corrects biomechanical drivers.
Electrohydraulic vs. Radial: Outcomes and Patient Experience
- Comfort and dosage: Electrohydraulic systems with a soft, water-mediated contact surface distribute energy more evenly across the skin, enabling higher therapeutic doses with improved comfort. This reduces the need for local anesthesia and enhances patient tolerance, even in acute sports settings (International Society for Medical Shockwave Treatment, n.d.).
- Coverage and efficiency: The broad focus increases the treated tissue volume, improving detection of reactive areas through biofeedback—patients feel increased intensity over inflamed or damaged tissue. This speeds mapping and reduces technician dependency.
- Durability: Third-party outcome tracking has reported more sustained pain reduction with electrohydraulic shockwave compared to radial devices, which tend to regress toward baseline by six months—consistent with a stronger physiologic effect and more comprehensive tissue coverage (DataBiologics, n.d.).
Sports Medicine Case Insight: Rapid Return-To-Play
When a professional pickleball athlete suffered an adductor strain, team clinicians reported a typical recovery window of 6–10 weeks. Using electrohydraulic shockwave as part of multimodal care, the athlete returned closer to 3–4 weeks. Functionally, this suggests shockwave supported both pain modulation and accelerated remodeling, permitting earlier graded loading and neuromuscular retraining.
Orthopedic Perspective: High-Level Usage in Pro Sports
Orthopedic consultant Dr. Mark O’Malley (Hospital for Special Surgery; consultant to multiple NBA/NFL teams) emphasizes that SoftWave therapy is now routinely used for bone edema, slow-healing fractures, and postoperative cases due to its comfort and ability to deliver higher energy levels without anesthesia. In busy team clinics, multiple shockwave stations run continuously to maintain athletes’ readiness and post-op progress (O’Malley, n.d.).
Integrative Chiropractic Care: Closing the Loop for Resilience
In my practice, integrative chiropractic care ensures that the gains from shockwave translate into longer-term resilience:
- Segmental and regional mobility: Joint restrictions in the foot/ankle, pelvis, and thoracolumbar spine alter load distribution, fueling plantar fascia stress and adductor overload. Targeted spinal and extremity adjustments, combined with instrument-assisted soft tissue work, restore mechanical efficiency.
- Neuromuscular retraining: We couple shockwave with motor control exercises to normalize timing, co-contraction, and eccentric control—critical for adductor strains and tendinopathies.
- Load management and gait: With improved perfusion and reduced pain, patients can re-enter graded loading and gait retraining sooner. We address cadence, step width, foot strike, and hip-knee-ankle alignment to reduce re-injury.
- Fascial continuity: The plantar fascia-posterior chain connection means we treat not only the foot but also calf, hamstrings, and lumbar mechanics—shockwave improves tissue pliability, while chiropractic restores segmental motion and fascial glide.
- Biochemical support: Where indicated, we integrate anti-inflammatory nutritional strategies and sleep optimization to support collagen remodeling and endothelial function.
Clinical observations: What I see in practice
- Patients with chronic plantar fasciitis often report a meaningful pain drop immediately after electrohydraulic shockwave, with further reduction over 2–8 weeks as angiogenesis and remodeling accumulate. When paired with calcaneal and midfoot adjustments, plus calf-soleus eccentric loading, long-term outcomes improve significantly.
- In adductor strains, combining shockwave with pelvic alignment, hip mobility, and adductor/abductor balance training decreases reinjury rates. Biofeedback during shockwave therapy helps pinpoint high-reactivity zones to guide the focus of manual therapy.
- For bone edema and post-op delayed healing, shockwave complements orthopedic timelines by enhancing local perfusion; we integrate gentle regional mobilization and edema management to sustain gains without jeopardizing surgical protocols.
Patient Communication: Clearing Up Device Confusion
Because many communities have providers offering radial pressure wave treatments under the “shockwave” label, patients may arrive skeptical or report prior discomfort. We clarify:
- Pressure wave vs. shockwave differences in depth, mechanism, and expected durability.
- Why electrohydraulic systems can be more comfortable and effective for deeper structures.
- How biofeedback during treatment helps us localize target tissue and individualize dosing.
Practical Protocols: How We Implement Care
- Pain mapping and biofeedback
- Begin with a broad sweep over the region using conservative energy.
- Identify reactive zones where patients feel increased intensity; document.
- Dosing rationale
- Use higher energy levels within the patient’s tolerance to drive mechanotransduction while maintaining comfort; progress across sessions as needed.
- Treat along kinetic chain connections (e.g., plantar fascia to calf and hamstrings).
- Integrative sequence options with orthobiologics
- Same-day approach: Shockwave first to reduce pain and prime perfusion, followed by PRP or cell-based injection—many report improved injection tolerance and early pain control (DataBiologics, n.d.).
- Preconditioning approach: Shockwave 2–3 days before the orthobiologic injection to enhance the local milieu, angiogenic signals, and patient readiness.
- Diagnostic-support approach: Use shockwave biofeedback the day prior to confirm symptomatic tissue; document findings to align patient, provider, and witness on injection targets.
- Workflow and staffing
- Because broad-focus energy covers more tissue with less dependence on precision, trained medical assistants can deliver sessions under supervision, improving clinic flow.
- Typical sessions last 10–15 minutes, making it compatible with chiropractic and rehab scheduling blocks.
Safety, Comfort, and Access
- Comfort: Water-mediated applicators and broad energy distribution improve tolerance—often no anesthesia required.
- Safety: When properly screened for contraindications (e.g., over lung fields, active infection, malignancy in treatment area, pregnancy over abdomen), electrohydraulic shockwave demonstrates a strong safety profile (International Society for Medical Shockwave Treatment, n.d.).
- Access and reimbursement: Many clinics operate shockwave on a cash-pay basis, though localized insurance pathways may exist. Quick sessions and immediate feedback foster patient buy-in.
How Integrative Chiropractic Amplifies Outcomes
- Shockwave can rapidly reduce nociceptive activity and increase perfusion, enabling earlier corrective care.
- Chiropractic adjustments restore joint mechanics that perpetuate soft tissue overload.
- Functional rehab cements gains through graded loading and movement quality.
- Together, this reduces recurrence by addressing both biology and biomechanics.
From the Field to the Clinic: Why Teams and Patients Choose This
Professional teams use electrohydraulic shockwave therapy because it is:
- Comfortable at higher energies, allowing effective dosing without anesthesia.
- Capable of addressing deep structures and bone-related pain.
- Efficient to deploy across multiple athletes daily.
Patients choose integrative pathways because they experience:
- Immediate pain changes, often within the same visit.
- A clear plan bridging shockwave, chiropractic care, and rehab.
- Sustained improvements when the kinetic chain is treated comprehensively.
Conclusion: A Modern Repair Signal, Optimized by Integrative Care
Shockwave therapy is more than a pain tool—it is a regenerative signal that activates the body’s repair programs. When delivered through electrohydraulic systems and combined with chiropractic adjustments, functional rehab, and, when appropriate, orthobiologics, patients experience faster relief and longer-lasting results. From patient relief from chronic pain to routine clinical use—reflects what I see daily at the clinic: this technology, applied in a patient-centered, evidence-informed manner, changes recovery timelines and reduces recurrence.
If you are curious about how these protocols could fit your case, call (915) 412-6677 or connect with me through my scheduler. Our focus remains clear: combine modern mechanobiology with precise biomechanics for results that last.

References
- International Society for Medical Shockwave Treatment. Shockwave Therapy Resources (n.d.). Guidelines and educational materials on medical shockwave mechanisms, indications, and safety.
- DataBiologics. Patient-Reported Outcomes in Musculoskeletal Care (n.d.). Third-party registry insights on shockwave modalities and orthobiologics in clinical practice.
- Hospital for Special Surgery. Sports Medicine and Orthopedic Care (n.d.). Clinical expertise and usage of shockwave techniques in high-performance athletes.
Professional Scope of Practice *
The information herein on "Shockwave Therapy and Chiropractic: Evidence and Insights" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card