“For individuals looking to improve overall health and wellness, how can paying attention to non-exercise activities help burn more calories and improve metabolic rates?”
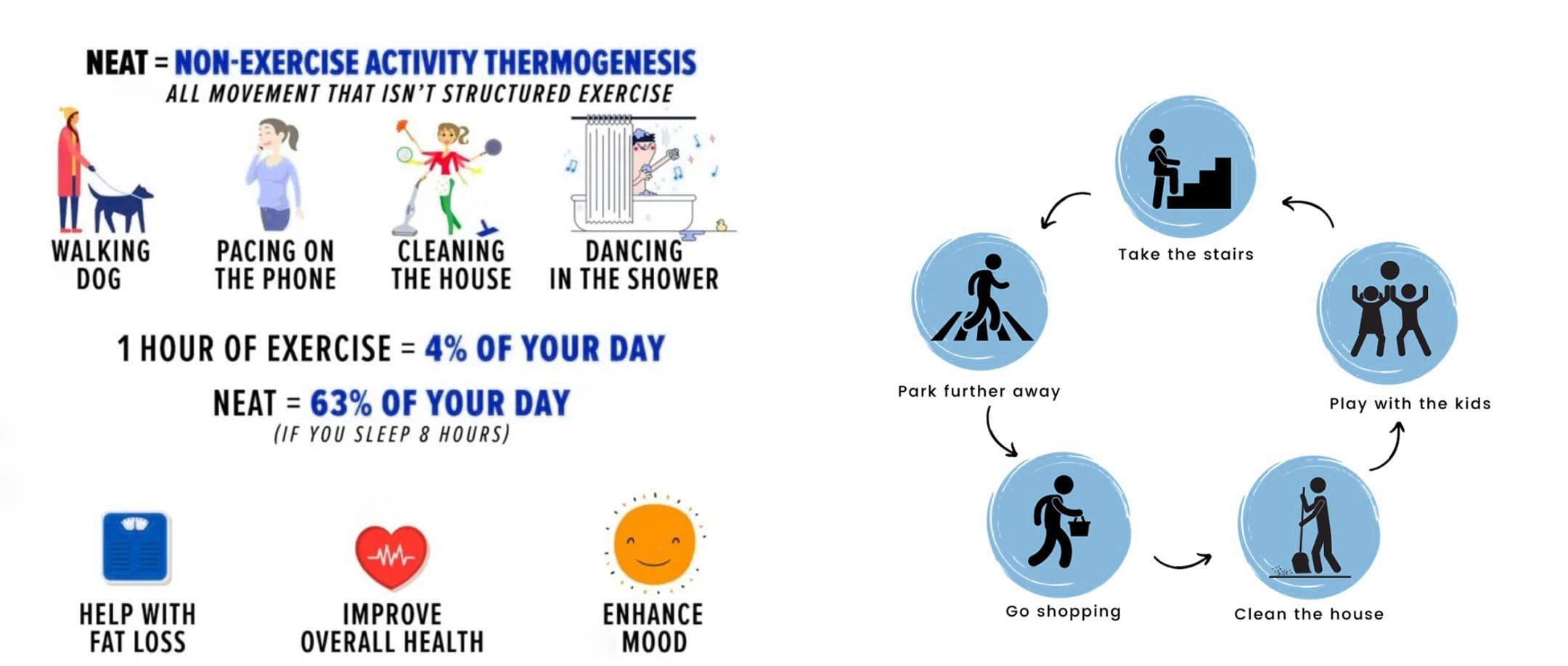
Table of Contents
Non-Exercise Activity Thermogenesis – NEAT
Non-exercise activity thermogenesis, or NEAT, describes the calories burned by daily movements and activities. These physical movements are not planned or structured exercises, workouts, or sports. It is also referred to as non-exercise physical activity or NEPA. Examples include activities like:
- Cleaning
- Cooking
- Shopping
- Playing a musical instrument
- Small movements like fidgeting
- When buying a few items, carry a basket instead of a shopping cart.
- Take the stairs instead of the elevator or escalator.
While these movements might not seem like a lot, they can have a substantial impact on metabolic rates and calorie expenditures. A study followed over 12,000 women for 12 years and found that fidgeting can reduce the risk of death associated with excessive sedentariness. (Gareth Hagger-Johnson et al., 2016)
Calories Burned
The amount of calories burned varies from person to person. A study reported that the number of calories burned from non-exercise activity thermogenesis varies up to 2000 kilocalories a day between two individuals of similar size. (Christian von Loeffelholz et al., 2000). A number of factors can account for this difference, including environment and genetics. Individuals’ occupations and lifestyles can also influence non-exercise activity thermogenesis. For example, two individuals with similar body mass indexes or BMIs but different jobs, sedentariness versus activity, will burn different calorie amounts.
Improving Health
Non-exercise activity thermogenesis is thought to be one of the ways the body manages weight. When gaining weight, NEAT tends to increase, whereas when losing weight, NEAT decreases with individuals sitting more without moving as much. A research review noted that the benefits of non-exercise go well beyond the extra calories expended. (Pedro A. Villablanca et al., 2015). Increasing non-exercise activity thermogenesis reduces the risk of metabolic syndrome, cardiovascular issues, and other health problems. Plus, research shows that inactivity can negate the time and effort put into structured exercise. (John D. Akins et al., 2019). Combating sedentary behavior with non-activity thermogenesis helps increase the benefits of regular workouts.
Incorporating NEAT
There are small ways to incorporate non-exercise activity thermogenesis at work and at home. This could be using a standing desk or stability ball. According to the National Academy of Sports Medicine, a 145-pound person can approximately burn:
- 102 calories an hour while sitting at work.
- 174 calories if standing at work.
- 72 calories extra may not seem like a lot, but it can add up to more than 18,000 calories burned per year, leading to an approximate 5-pound weight loss.
If waiting in line or sitting in traffic, finding small ways to move, like tapping the hands or feet or moving the head to music, helps the body take advantage of non-exercise activity thermogenesis. Making more conscious efforts to move can go a long way in improving health.
Is Motion Key To Healing?
References
Hagger-Johnson, G., Gow, A. J., Burley, V., Greenwood, D., & Cade, J. E. (2016). Sitting Time, Fidgeting, and All-Cause Mortality in the UK Women’s Cohort Study. American journal of preventive medicine, 50(2), 154–160. https://doi.org/10.1016/j.amepre.2015.06.025
von Loeffelholz, C., & Birkenfeld, A. L. (2022). Non-Exercise Activity Thermogenesis in Human Energy Homeostasis. In K. R. Feingold (Eds.) et. al., Endotext. MDText.com, Inc.
Villablanca, P. A., Alegria, J. R., Mookadam, F., Holmes, D. R., Jr, Wright, R. S., & Levine, J. A. (2015). Nonexercise activity thermogenesis in obesity management. Mayo Clinic proceedings, 90(4), 509–519. https://doi.org/10.1016/j.mayocp.2015.02.001
Akins, J. D., Crawford, C. K., Burton, H. M., Wolfe, A. S., Vardarli, E., & Coyle, E. F. (2019). Inactivity induces resistance to the metabolic benefits following acute exercise. Journal of applied physiology (Bethesda, Md. : 1985), 126(4), 1088–1094. https://doi.org/10.1152/japplphysiol.00968.2018