Table of Contents
Integrative Shockwave Therapy for Joint and Muscle Pain
Abstract
In this educational post, I walk you through how modern shockwave technologies—specifically radial and focused extracorporeal shockwave therapy—can be integrated into comprehensive musculoskeletal care. I explain their underlying biomechanics, bioeffects, and clinical protocols; compare their FDA status and practical considerations; and demonstrate how integrative chiropractic care optimizes outcomes when combined with rehabilitative exercise, manual therapies, and functional medicine. Drawing on leading research and my clinical observations at Sciatica Clinic and in daily practice, I clarify why and when each modality is chosen, how to set therapeutic parameters, what patients should expect, and how to structure series-based care for conditions such as lateral epicondylalgia, plantar fasciitis, tendinopathy, and post-whiplash cervical pain.

Understanding Shockwave Therapy: Radial vs. Focused Energy Delivery
I often introduce shockwave therapy by describing the simple physics: high-pressure acoustic waves transmitted into tissue to evoke a controlled mechanotransductive response. But not all shockwaves are the same. The clinical art lies in matching the wave profile to the target tissue depth and pathology.
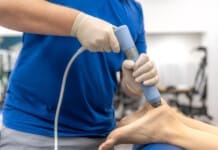
- Radial Shockwave (RSWT)
- Highest energy concentration at the skin surface.
- Energy disperses and fans out, penetrating typically up to about 6 cm.
- Ideal for superficial tendons, myofascial restrictions, and large muscle groups.
- Produces a broad field of mechanical stimulation, useful for global soft-tissue tone regulation.
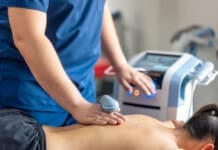
- Focused Shockwave (FSWT)
- Acoustic energy converges to a precise focal point at depth, reaching up to ~12.5 cm.
- Excellent for deep tendons, entheses, bone, ligaments, and joint regions.
- A pinpoint-accurate approach: think “dart to a bullseye” at the pathological locus.
In practice, I combine both to treat a primary lesion and its secondary myofascial consequences. For example, in tennis elbow (lateral epicondylalgia), I will:
- Use radial shockwave across the entire forearm flexor and extensor chains and into the biceps to downregulate hypertonicity and improve regional circulation.
- Then apply focused shockwave precisely at the common extensor tendon origin to address the enthesopathic and neovascular changes driving pain.
This sequence provides immediate analgesia and range-of-motion gains, with recurrent symptoms diminishing progressively across a series of visits as the tissue biologically remodels (Gerdesmeyer et al., 2008; Speed, 2014).
How Shockwave Promotes Regeneration: Mechanotransduction, Microtrauma, and Biological Cascades
Patients often ask, “What does regeneration mean here?” Shockwave therapy uses controlled microtrauma to activate repair signaling. The physiology is deep, but the narrative is straightforward:
- Mechanotransduction
- Acoustic pressure waves deform cell membranes and ECM (extracellular matrix), opening mechanosensitive ion channels and modulating integrin-focal adhesion complexes.
- This triggers intracellular cascades involving MAPK/ERK, PI3K-Akt, and NF-κB, promoting cell proliferation, matrix turnover, and anti-inflammatory shifts (Schmitz et al., 2015).
- Angiogenesis and Neovascularization
- Upregulation of VEGF and eNOS leads to microvascular sprouting, thereby improving oxygenation and nutrient delivery to hypoxic regions of the tendon (Wang et al., 2003).
- Stem/Progenitor Cell Recruitment
- Signals attract mesenchymal stem cells and enhance tenocyte activity, supporting reparative collagen synthesis and alignment (Zelle et al., 2010).
- Neuromodulation and Analgesia
- Immediate analgesia arises from hyperstimulation analgesia, transient nociceptor desensitization, and modulation of substance P and CGRP at free nerve endings (Manganotti & Amelio, 2005).
- Over time, central sensitization attenuates via improved input quality and reduced peripheral drivers.
Practically, shockwave moves a chronic, degenerative tendon into an acute, reparative phase, then shepherds it through remodeling over a protocolized series. That is why transient relief after a session can recede within about 72 hours, yet returns less intensely as sessions accumulate—a hallmark of progressive biological change rather than mere symptomatic masking (Rompe et al., 2009).
FDA Status, Indications, and Real-World Boundaries
Clarity about regulation and indications is essential for patient trust and clinical compliance.
- Focused Shockwave
- FDA-approved for chronic plantar fasciitis.
- Widely supported in tendinopathies, bone marrow edema, and delayed unions as per international literature (Gerdesmeyer et al., 2008; Lou & Hu, 2019).
- Radial Shockwave
- FDA-cleared for acute and chronic musculoskeletal pain.
- Effective for myofascial pain syndromes, tendinopathies, and soft-tissue overuse patterns (Notarnicola & Moretti, 2012).
- Neurocranial Applications
- Emerging in Europe for certain brain-related protocols, but currently contraindicated in the U.S. pending further approval.
- For safety, I treat from the occipital base downward in cervical applications, avoiding cranial targets.
In my clinic, this framework guides informed consent, candid expectation-setting, and appropriate documentation for personal injury and sports scenarios. For whiplash, we target cervical paraspinals, levator scapulae, upper trapezius, and deep posterior chain patterns while respecting neurovascular structures.
Evidence-Based Protocol Design: Dosing, Frequency, and Patient Feedback
A consistent finding in the literature—and in my practice—is that dosing should be titrated to patient feedback and pathology depth.
- Session Duration
- Typical treatments last about 10 minutes total.
- Combination sessions are often split into 5 minutes radial + 5 minutes focused.
- Pulse Counts and Energy
- Radial protocols: approximately 2,000–3,000 pulses per region per session, with preset counters to standardize delivery.
- Focused shockwave dosing is set in mJ/mm² and titrated from low energy to the patient’s therapeutic window (perceived intensity around 5–6 out of 10), ensuring a biological stimulus without undue discomfort (Schmitz et al., 2015; Speed, 2014).
- Treatment Series
- Expect 3–6 sessions at weekly intervals for common tendinopathies, adjusting based on chronicity, imaging, and response.
- Acute overuse syndromes may respond in fewer visits; long-standing degenerative changes often need the full series plus progressive loading.
- Diagnostic Value of Sensitivity Mapping
- Shockwave is inherently diagnostic: patient-perceived focal tenderness helps locate primary enthesopathic sites, guide energy focus, and track change session-to-session.
Clinically, I pair every shockwave series with graded-loading programs that progressively challenge the tendon within its elastic range, restoring tensile strength and collagen alignment. This combination—mechanical stimulus plus mechanotherapeutic exercise—is central to sustained outcomes.
Integrative Chiropractic Care: Why Combining Modalities Elevates Outcomes
Shockwave is powerful, but outcomes truly accelerate when integrated within a chiropractic-functional medicine framework that addresses biomechanics, behavior, and biology.
- Manual Therapy and Joint Mechanics
- I employ precise chiropractic adjustments to normalize joint play and arthrokinematics, reducing aberrant shear and compressive loads on tendons.
- Soft-tissue mobilization and instrument-assisted techniques break down maladaptive cross-links and restore gliding, easing nociceptive input.
- Neuromuscular Re-education
- Proprioception and motor control training restore firing patterns, especially in scapular stabilizers for elbow pain or in the intrinsic foot muscles for plantar fasciitis.
- This reduces recurrent overload at the enthesis and augments the biotensegrity of the kinetic chain.
- Functional Medicine and Recovery Biology
- Address glycemic variability, vitamin D, collagen cofactor sufficiency (e.g., vitamin C, copper), and omega-3 intake to modulate inflammation and collagen synthesis.
- Optimizing sleep and stress physiology supports hormonal balance and matrix turnover, both of which are essential for remodeling (Ackermann et al., 2015).
- Load Management and Ergonomics
- Correct training errors and workplace biomechanics to prevent relapse.
- Progressive eccentric-concentric protocols are matched to tissue healing stages, informed by shockwave-induced vascular changes.
Over the years at Sciatica Clinic, integrating these pillars consistently outperforms monotherapy. Patients report faster pain relief, better function, and lower recurrence when shockwave is embedded in a structured, holistic plan.
Clinical Scenarios and Protocol Reasoning
Tennis Elbow (Lateral Epicondylalgia)
- Pathophysiology: Microtears at the extensor carpi radialis brevis origin, neovascularization, nociceptive sprouting, and ECM disarray.
- Why Shockwave: Focused energy reduces neovascular complexes and stimulates tenocyte-driven collagen I synthesis; radial addresses myofascial tone in the forearm-biceps continuum.
- Protocol:
- Radial: 2,000–3,000 pulses over forearm compartments and biceps, titrated to 5–6 out of 10 sensations.
- Focused: Focal dosing at the enthesis, starting low and increasing within tolerance.
- Integrative: Scapular stabilization, wrist extensor eccentric loading, and ulnar nerve mobility as indicated.
- Expected Course: Immediate analgesia, then partial recurrence within ~72 hours; progressive reduction across 4–6 sessions (Rompe et al., 2009).
Plantar Fasciitis (Chronic)
- Pathophysiology: Degenerative changes at the medial calcaneal enthesis; reduced perfusion; altered fascial stiffness.
- Why Shockwave: Strong evidence base for FSWT; promotes angiogenesis, ECM remodeling, and pain modulation (Gerdesmeyer et al., 2008).
- Protocol:
- Focused: Target the medial calcaneal origin; titrate mJ/mm² within therapeutic range.
- Radial: Address calf complex and plantar fascia length-tension.
- Integrative: Foot intrinsic activation, calf flexibility, hip-knee alignment, and orthotic or footwear guidance as needed.
- Expected Course: 3–5 sessions with graded return to loading; outcome enhanced by gait retraining.
Cervical Myofascial Pain Post-Whiplash
- Pathophysiology: Hypertonicity in deep and superficial cervical chains, altered sensorimotor control, and possible facet irritation.
- Why Shockwave: Radial reduces myofascial hyperalgesia; focused can precisely address deeper entheses or periarticular structures below the occipital base.
- Protocol:
- Radial: Posterior cervical chain, levator scapulae, upper trapezius.
- Focused: Deeper pain loci below the occipital line; avoid cranial structures.
- Integrative: Cervical stabilization, vestibular-ocular motor drills, postural retraining, stress regulation.
- Expected Course: Pain relief within sessions; functional gains with neuromuscular retraining across 4–6 weeks.
Patient Experience, Session Flow, and Comfort
- Sensory Profile:
- Radial can sound like a “mini jackhammer”; modern devices have substantially reduced noise levels compared to older platforms.
- Focused is quieter; sensations range from tapping to deep pressure at the focal zone.
- In-Session Monitoring:
- I adjust energy at the handpiece based on real-time patient feedback, staying inside the therapeutic window.
- Built-in pulse counters ensure dosing consistency; pre-set stops help avoid over- or under-treatment.
- Post-Session Expectations:
- Immediate lightness and mobility are common.
- Mild soreness may appear, akin to a good workout; it typically resolves quickly as remodeling continues.
Maintenance, Reliability, and Clinical Uptime
In practice management, uptime matters. Vendors specify maintenance cycles by pulse counts:
- Radial
- An internal guide tube and bullet assembly drives the acoustic wave.
- Replace approximately every 1,000,000 pulses; kits often include two assemblies, equating to ~2,000,000 pulses (~1,000 treatments at 2,000 pulses/session).
- On-screen notifications prompt service; replacement is straightforward with guided videos.
- Focused
- A handpiece electromagnetic coil generates the focused wave.
- Replacement typically every 2,000,000 pulses (~1,000 treatments), serviced by the distributor with quick turnaround.
- Plan to ship the handpiece late in the week to minimize downtime; overnight exchanges are common.
This reliability ensures continuity in series-based plans, which is crucial for tissue remodeling timelines.
Billing, Access, and Practice Economics
While many clinicians ask about insurance coverage, most shockwave implementations remain cash-based in the U.S. This has practical advantages:
- Transparent Value
- Typical per-session pricing: $250–$300 for combined radial + focused sessions, sold in 4–6 treatment packages.
- The series model aligns with pathophysiology—patients understand they are buying a course of regenerative care, not a single symptom-relief visit.
- Financing and ROI
- Some practices utilize equipment financing with low initial monthly costs, allowing immediate clinical use and revenue generation.
- The economic viability is driven by high patient satisfaction and repeat demand across musculoskeletal indications.
Even for veterans and personal injury cases, I position shockwave as a value-driven modality, emphasizing outcomes, rapid function restoration, and reduced need for invasive care when appropriate.
Safety, Contraindications, and Clinical Judgment
Primum non nocere guides every session:
- Avoid: Malignancy at the treatment site, active infection, pregnancy over the uterine regions, acute DVT, and direct cranial applications in the U.S.
- Cautions: Anticoagulated patients, peripheral neuropathy with reduced sensation, recent corticosteroid injection at the target tissue, and severe osteoporosis near bony focal points.
- Technique: Maintain coupling gel integrity, keep transducer motion controlled, and monitor patient-reported thresholds continuously.
My approach uses incremental titration and careful tissue mapping to protect sensitive structures while ensuring sufficient biological stimulus.
Bringing It All Together: A Patient-Centered Pathway
Here is how I orchestrate care from start to finish:
- Assessment and Imaging
- Clinical exam plus ultrasound, where appropriate, to visualize tendon thickness, neovessels, and fiber disorganization.
- Functional assessment of kinetic chain drivers (foot-hip for plantar fasciitis, scapulo-thoracic mechanics for elbow).
- Education and Consent
- Explain mechanotransduction, series expectations, and the 72-hour symptom dynamics.
- Align goals around function and performance, not just pain scores.
- Shockwave Series
- Combine radial for regional soft-tissue modulation and focused for the primary lesion.
- Titrate energy within the therapeutic window, track pulse counts, and document session parameters.
- Integrative Plan
- Prescribe graded loading, mobility drills, ergonomic corrections, and nutritional cofactor support.
- Use chiropractic adjustments to normalize joint mechanics and reduce aberrant load on healing tissues.
- Outcome Tracking
- Measure PROMs (pain, function), range, strength metrics, and return-to-activity milestones.
- Adjust the plan based on the response; consider adjuncts such as low-level laser therapy, blood flow restriction, or dry needling where indicated.
Through this structured, evidence-aligned approach, I see consistent improvements across complex cases. It is the synergy—precise energy delivery plus comprehensive integrative care—that transforms outcomes.

References
- Gerdesmeyer et al. (2008). Randomized controlled trial of shockwave therapy for chronic plantar fasciitisGerdesmeyer, L., Frey, C., Vester, J., Maier, M., Weil, L., Weil, L., Russlies, M., & Stienstra, J. (2008). Radial extracorporeal shock wave therapy is safe and effective for chronic plantar fasciitis. Journal of Bone and Joint Surgery, 90(3), 524–534. https://doi.org/10.2106/JBJS.G.02442
- Schmitz et al. (2015). Efficacy and safety of extracorporeal shockwave therapy for orthopedic conditionsSchmitz, C., Császár, N. B., Rompe, J. D., Choi, J. K., Furia, J. P., & Dedes, V. (2015). Efficacy and safety of extracorporeal shockwave therapy in musculoskeletal disorders: A systematic review. Archives of Orthopaedic and Trauma Surgery, 135(11), 1547–1562. https://doi.org/10.1007/s00402-014-2081-2
- Speed (2014). A systematic review of shockwave therapy for tendinopathiesSpeed, C. (2014). A systematic review of shockwave therapy for chronic tendinopathies. British Journal of Sports Medicine, 48(21), 1538–1547. https://doi.org/10.1136/bjsports-2012-091961
- Rompe et al. (2009). Plantar fasciopathy: Evidence-based treatmentRompe, J. D., Cacchio, A., Weil, L., & Furia, J. (2009). Plantar fasciopathy: From diagnosis to treatment. British Journal of Sports Medicine, 43(6), 461–468. https://doi.org/10.1136/bjsm.2008.052506
- Wang et al. (2003). Shockwave therapy and tendon angiogenesisWang, C. J., Wang, F. S., Yang, K. D., Weng, L. H., Hsu, C. C., Huang, C. S., & Yang, L. C. (2003). Shock wave therapy induced angiogenesis and improved healing in tendons. Clinical Orthopaedics and Related Research, 387, 337–346. https://doi.org/10.1097/01.blo.0000092973.12414.0a
- Manganotti & Amelio (2005). Neuromodulatory effects of shockwave therapyManganotti, P., & Amelio, E. (2005). Long-term effect of shock wave therapy on peripheral nerve and pain pathway. Clinical Rheumatology, 24(3), 245–248. https://doi.org/10.1007/s00296-004-0533-1
- Notarnicola & Moretti (2012). RSWT for myofascial painNotarnicola, A., & Moretti, B. (2012). Radial shock wave therapy in the treatment of myofascial pain syndrome. Clinical Rheumatology, 31(3), 465–469. https://doi.org/10.1007/s00296-011-2147-8
- Zelle et al. (2010). Shockwave therapy and progenitor cellsZelle, B. A., Gollwitzer, H., & Schmitz, C. (2010). Extracorporeal shock wave therapy: Cellular effects in tendons. International Orthopaedics, 34(4), 583–587. https://doi.org/10.1007/s00264-009-0741-1
- Lou & Hu (2019). Focused ESWT for bone pathologyLou, S., & Hu, J. (2019). Extracorporeal shock wave therapy in treating bone disorders. International Orthopaedics, 43(4), 781–791. https://doi.org/10.1007/s00264-019-04380-5
Professional Scope of Practice *
The information herein on "Integrative Shockwave Therapy and Chiropractic Integration" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card