Fibromyalgia or FM is a condition that increases an individual’s sensitivity to pain. It causes extensive body pain among other issues including:
- Anxiety
- Depression
- Fatigue
- Numbness
- Poor sleep
- Bladder issues
- Bowel problems
Fibromyalgia includes multiple tender points at specific areas of the body and widespread musculoskeletal pain. Research suggests that the nervous system is the key factor in the pathology of fibromyalgia. This condition affects around four million adults in the United States and roughly two percent of the adult general population. Like most chronic disorders symptoms can extend far beyond the defining criteria. There are chances that a physical examination and tests appear normal.
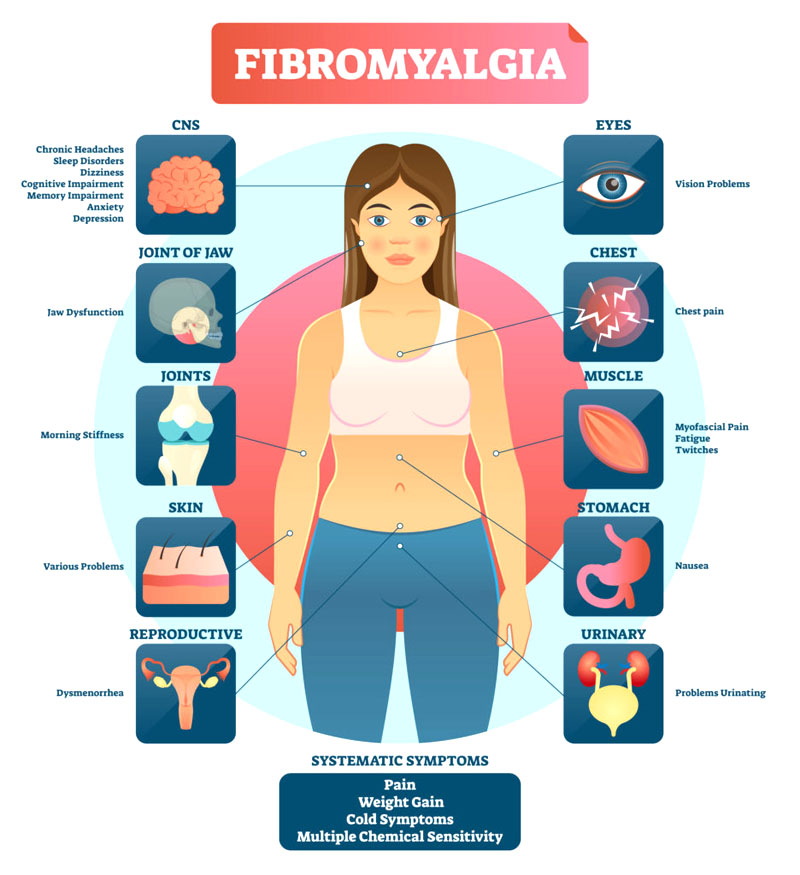
Table of Contents
About Fibromyalgia
The condition is a chronic syndrome that is associated with arthritis. The major statistics and facts about fibromyalgia include:
- Muscle tenderness is the primary syndrome
- There is widespread pain that is arthritis-related
- It can manifest as a primary or secondary condition
- It can present unrecognized symptoms that can be difficult to identify
- A high percentage of individuals suffer from sleep problems and fatigue
- It affects physical and mental health
- There are no specific tests to diagnose the condition

Causes
There are several theories or triggers that contribute to the progression of fibromyalgia. They are:
Peripheral Sensitization
Injury or trauma to the nervous system or musculoskeletal system can lead to peripheral sensitization of the sensory nervous system. This tends to be the case with arthritis and peripheral nerve damage. Peripheral sensitization leads to increased sensitivity to sensory nerve stimuli. This results in increased sensitivity to touch and heat and can potentially lead to primary allodynia.
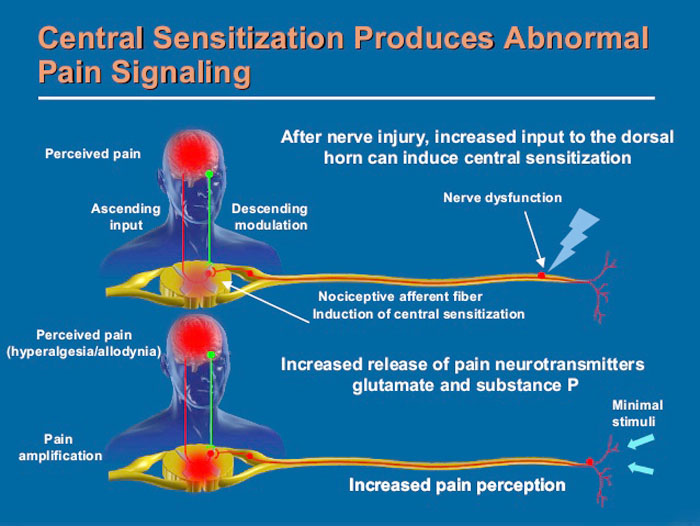
Central Sensitization
Central sensitization refers to changes in the central nervous system, specifically the brain and spinal cord. The condition amplifies pain. Individuals with fibromyalgia have a reduced threshold for pain. This is caused by amplified brain sensitivity to pain indicators with repeated nerve stimulation leading to changes in the brain.
Sleep Disturbance
Sleep disturbances have been associated with fibromyalgia. Studies show that sleep pattern disturbance could be a cause and not just a symptom of fibromyalgia. Poor sleep quality accounts for the majority between pain and fatigue. Major disturbances include:
- Shorter sleep time
- The beginning of sleep is delayed
- Waking right after sleep has begun starts to increase
- Sleep efficiency decreases
- Stirred/Waking out of sleep starts to increase
- Nighttime activity increases
Post-traumatic Stress
This could be a trigger of fibromyalgia. Patients are recommended to get examined for PTSD. Studies suggest that women suffering from chronic pain that is spread throughout the body and fibromyalgia have an increased risk for posttraumatic stress. Patients also show a reduced function of the HPA hormone. This is proof of an impaired transmitter system. An altered transmitter system in individuals with fibromyalgia interferes with the body’s stress regulators.

Hormones
Fibromyalgia is more common in women than men. Studies have found that many women find their symptoms improve during pregnancy. Individuals with fibromyalgia tend to yield less cortisol when responding to stress compared to individuals that do not have fibromyalgia. The condition is mirrored when the body is deficient in cortisol.
Changes in Muscle Metabolism
According to NCBI Resources, fibromyalgia is associated with altered skeletal muscles. Decreased blood flow and deconditioned muscles can lead to fatigue along with reduced endurance that can lead to fibromyalgia.
Genetics
There are some studies that suggest that pain can be influenced by environmental and genetic factors. The condition does not get passed down directly from the parents. But the ailment can present to a group of individuals within a family.
Chiropractic
Most reports suggest that fibromyalgia is a chronic condition. When it is related to trauma, the condition tends to be chronic and severe. Reduced pain and improved function can be achieved with the proper treatment. There are treatment options in place that can help individuals alleviate symptoms and prevent flare-ups.
Body Composition
Calorie Restriction and Fasting
Calorie restriction and fasting are traditional ways of losing weight and fat. While calorie restriction is self-descriptive, intermittent fasting and alternate-day fasting involves going for long stretches of the day and night without eating, then getting all of the nutrition in a shorter time. Alternating day fasting alternates days of eating normally, and then not eating at all. Calorie restriction will help an individual lose weight and fat in most cases. It is more effective than intermittent fasting, and not as difficult to maintain. Alternate Fasting results in the same amount of weight loss as calorie restriction. What makes maintaining Alternate Fasting long-term difficult is being able to fight off the hunger on the fasting days.
Dr. Alex Jimenez’s Blog Post Disclaimer
The scope of our information is limited to chiropractic, musculoskeletal, physical medicines, wellness, and sensitive health issues and/or functional medicine articles, topics, and discussions. We use functional health & wellness protocols to treat and support care for injuries or disorders of the musculoskeletal system. Our posts, topics, subjects, and insights cover clinical matters, issues, and topics that relate and support directly or indirectly our clinical scope of practice.*
Our office has made a reasonable attempt to provide supportive citations and has identified the relevant research study or studies supporting our posts. We also make copies of supporting research studies available to the board and or the public upon request. We understand that we cover matters that require an additional explanation as to how it may assist in a particular care plan or treatment protocol; therefore, to further discuss the subject matter above, please feel free to ask Dr. Alex Jimenez or contact us at 915-850-0900. The provider(s) Licensed in Texas& New Mexico*
References
American College of Rheumatology. Fibromyalgia. 2013. http://www.rheumatology.org/Practice/Clinical/Patients/Diseases_And_Conditions/Fibromyalgia/. Accessed December 5, 2014.
Wolfe F, Clauw DJ, Fitzcharles M, et al. The American College of Rheumatology Preliminary Diagnostic Criteria for Fibromyalgia and Measurement of Symptom Severity. Arthrit Care Res. 2010;62(5):600-610.
Professional Scope of Practice *
The information herein on "Fibromyalgia Pain Causes And Chiropractic Treatment" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Wellness and Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multi-state Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Colorado License #: C-APN.0105610-C-NP, Verified: C-APN.0105610-C-NP
New York License #: N25929, Verified N25929
License Verification Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card
Licenses and Board Certifications:
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
My Digital Business Card